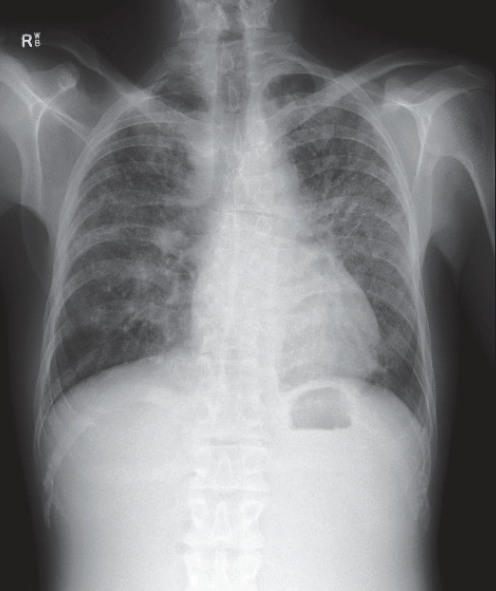
Figure 1. Chest X-ray demonstrating bilateral symmetrical hilar lymphadenopathy and reticular opacities
Question 1
What are the differential diagnoses?
Question 2
Which investigation would you consider initially?
Question 3
What further investigations may result in a diagnosis?
Question 4
What is the management and prognosis of this condition?
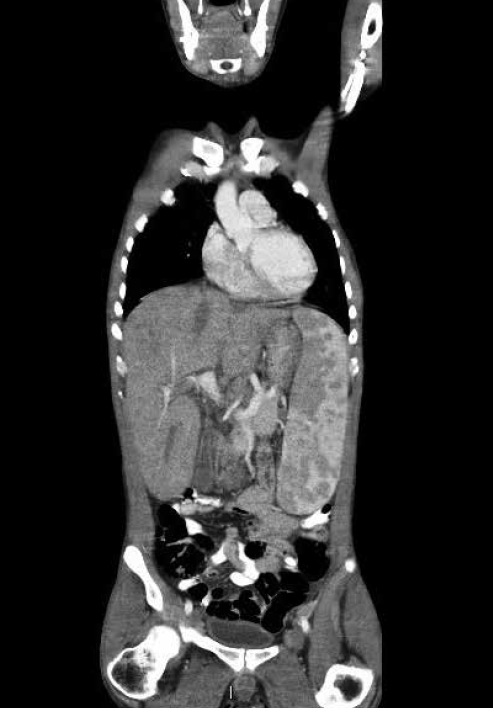
Figure 2. Coronal CT abdomen demonstrating marked hepatosplenomegaly
Answer 1
The list of diagnoses causing elevated calcium is extensive.1 A simple mnemonic to assist in remembering most aetiologies of hypercalcaemia is VITAMINS TRAP (Table 1). Primary hyperparathyroidism is the most common cause of hypercalcaemia in subjects presenting to primary care, while malignancy is often the most common cause in hospitalised patients. Milk–alkali syndrome due to the ingestion of absorbable antacids (calcium/magnesium carbonate) should be considered in any patient presenting with the triad of hypercalcaemia, renal dysfunction and alkalosis. Systemic disorders such as lymphoma, sarcoidosis, tuberculosis and berylliosis should be considered in a subject with hypercalcaemia, lymphadenopathy and hepatosplenomegaly.
Table 1. Causes of hypercalcaemia – VITAMINS TRAP
- Vitamin D and A excess
- Immobilisation
- Thyrotoxicosis
- Adrenal insufficiency
- Milk alkali syndrome
- Inflammatory/granulomatous – tuberculosis, berylliosis, coccidiodomycosis
- Neoplastic-related disease (PTH-r peptide), myeloma, lymphoma
- Sarcoidosis
- Thiazide diuretics, other medications (lithium, heparin)
- Rhabdomyolysis, chronic renal failure, renal transplant
- AIDS
- Paget’s disease, parenteral nutrition, phaeochromocytoma, parathyroid disease, familial hypocalciuric hypercalcaemia
|
Answer 2
A parathyroid hormone (PTH) assay will differentiate between PTH-mediated hypercalcaemia (primary and tertiary hyperparathyroidism, familial hypocalciuric hypercalcaemia) in which the PTH will be elevated or inappropriately normal and other causes in which the PTH will be suppressed. In this patient the serum PTH was 0.8 pmol/L (normal 2–9.5), consistent with a non-PTH mediated cause.
Answer 3
The chest X-ray demonstrates bilateral symmetrical hilar lymphadenopathy and reticular opacities. The abdominal computed tomography (CT) scan confirmed marked hepatosplenomegaly and moderate ascites. The most likely diagnosis was sarcoidosis, with the major differential diagnoses being lymphoma and tuberculosis. Histology from a transbronchial lung biopsy demonstrated bronchial and interstitial non-necrotising granulomas, with negative stains for fungal elements and acid-fast bacilli consistent with sarcoidosis (Figure 3). Serum angiotensin-converting enzyme was elevated at 460 U/L (normal 20–130).
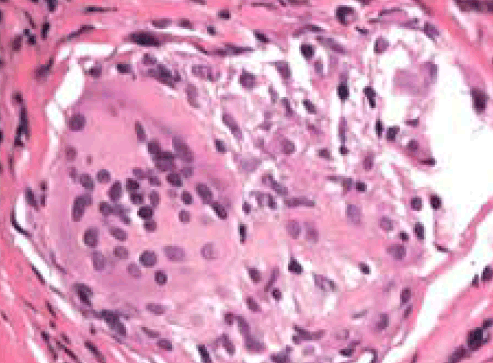
Figure 3. Haematoxylin & eosin stain of transbronchial lung biopsy showing a bronchial wall granuloma
Answer 4
Sarcoidosis manifests as some combination of intrathoracic lymphadenopathy, pulmonary involvement, ocular or skin involvement in more than 90% of patients, though any organ system can be affected.2 Hepatic and splenic lesions are seen on CT scan in 5% and 15% of patients respectively, and clinical neurologic involvement is seen in 10%, cardiac in 5%. Hypercalciuria occurs in 40% of subjects and hypercalcaemia in 11%.
Sarcoidosis is often a self-limiting disease. Two-thirds of patients enter remission within 10 years of diagnosis with few or no consequences of their illness, while one-third suffer progressive disease leading to significant organ impairment. Less than 5% of patients die as a result of sarcoidosis, usually due to respiratory failure secondary to progressive lung fibrosis, or neurologic or cardiac involvement.
Most patients with sarcoidosis do not require treatment as they are not disabled by the illness.3 Treatment is usually instituted when organ function is threatened; the risks of glucocorticoid therapy need to be weighed against the potential benefits. In the subject presented here, treatment was indicated for severe hypercalcaemia, renal dysfunction and respiratory and gastrointestinal involvement. The initial management of hypercalcaemia and renal dysfunction is rehydration and calciuresis with intravenous saline. Hypercalcaemia in subjects with sarcoidosis usually improves with glucocorticoid therapy (typically prednisolone 20–40 mg/day initially) though it may take 7–10 days to see an adequate response. Provided renal function is adequate (eGFR >30 mL/min), a single dose of intravenous zoledronic acid (5 mg) may be used for rapid resolution of hypercalcaemia while awaiting the effect of glucocorticoid therapy.
Additional medications may be used to treat sarcoidosis when glucocorticoids are ineffective, poorly tolerated or when a maintenance dose of >10 mg per day of prednisolone is required. These medications include methotrexate, hydroxychloroquine, azathioprine, leflunomide, mycophenolate, cyclophosphamide and tumour necrosis alpha antagonists.
Patient outcome
The subject’s respiratory function tests demonstrated a reduction in lung volumes and diffusing capacity consistent with moderate restrictive lung disease. There was no evidence of cardiac involvement on magnetic resonance imaging. He was commenced on methotrexate orally with the dose gradually titrated to 20 mg once a week. Prednisolone was gradually weaned to 7.5 mg per day, with serum calcium remaining normal. Progress chest X-ray demonstrated some resolution of pulmonary infiltrates, and repeat lung function testing showed improvement in his restrictive lung disease.
The subject gave written informed consent for publication of this case report.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.