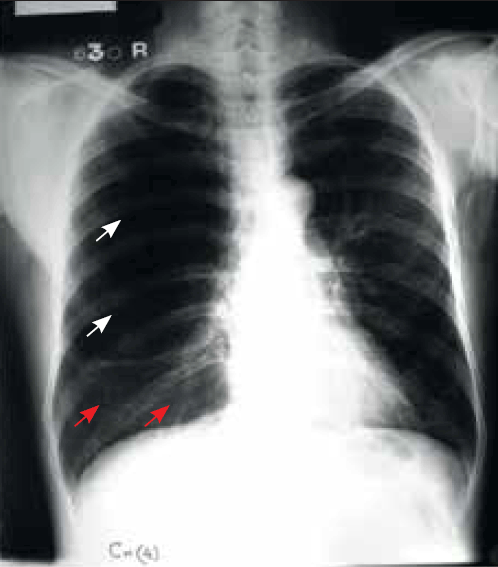
Figure 1. Chest X-ray (PA view) of the patient taken following acute breathlessness and chest pain
Question 1
Based on history and physical examination, what differential diagnoses would you consider in this patient?
Question 2
What does the chest X-ray show?
Answer 1
Based on the history and physical examination, the differential diagnoses include:
- right-sided pneumothorax
- right-sided bronchopleural fistula
- giant bulla in the right lung
- unilateral hyperinflation of the right lung
- right-sided massive pulmonary embolism
- partial airway obstruction
- Swyer-James syndrome.
Answer 2
The chest X-ray shows an area of hyperlucency with complete absence of bronchovascular markings in the upper and mid-zones on the right side. This area of hyperlucency has a convex lower border, suggestive of the presence of a large bulla (>15 cm diameter), occupying nearly two-thirds of the right hemithorax (Figure 1, white arrows). Compressed normal lung parenchyma is seen below it, which appears to be ‘pancaked’ atop the right hemidiaphragm (Figure 1, red arrows). The trachea is significantly shifted to the left side.
Case study continued
On admission to hospital, the clinical signs and chest X-ray were reviewed. While clinical findings were suggestive of a large right-sided pneumothorax, chest X-ray revealed the possibility of a giant bulla in the right hemithorax. A high resolution computed tomography (HRCT) chest scan was done in order to confirm the findings (Figures 2a to 2d).
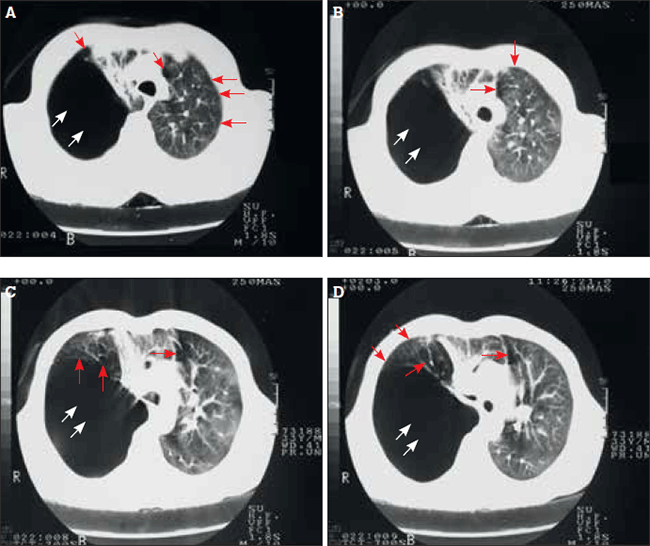
Figures 2a to 2d. High resolution computed tomography chest scan
Question 3
What does the HRCT chest scan show?
Question 4
Based on the above findings, what is the most likely diagnosis?
Answer 3
The HRCT chest scan (Figures 2a to 2d) confirms the presence of a large bulla (approximately 18 cm diameter) in the upper-and-mid zones on the right side (white arrows), which occupies nearly two-thirds of the right hemithorax, along with multiple areas of paraseptal emphysema (red arrows) and subpleural bullae (red arrowheads) in both lungs.
Answer 4
The patient is a chronic smoker and long term marijuana abuser with symptoms of acute breathlessness and right-sided chest pain. Chest X-ray and HRCT chest scans are suggestive of a giant bulla on the right side,1,2 with the underlying normal lung parenchyma compressed below it. Multiple areas of paraseptal emphysema and subpleural bullae are also seen in both lungs. In view of these findings, vanishing lung syndrome (VLS, giant bullous emphysema) is the most likely diagnosis in
this patient.
Question 5
What is the aetiology, and what are characteristic features of this condition?
Question 6
What is the appropriate treatment plan for this patient?
Answer 5
The main causative factors responsible for VLS include chronic tobacco smoking and/or long term marijuana abuse.3,4 Occasionally, alpha-1 antitrypsin deficiency has been shown to be an independent causative factor for this condition.5 Vanishing lung syndrome derives its name from the fact that the ‘lungs appear to be disappearing’, on chest X-ray. It is characterised by the presence of bullae ranging in size from 1–20 cm in diameter, occupying more than one-third of the hemithorax, predominantly involving the upper lobes, with the underlying normal lung parenchyma appearing to be ‘pancaked’ atop the hemidiaphragm. Extensive paraseptal emphysema and subpleural bullae are also characteristic features of VLS.
Answer 6
Bullectomy is the treatment of choice in patients with giant bullous emphysema. Bullectomy may be undertaken via VATS (video-assisted thoracoscopy) or open thoracotomy. However, the extent of centrilobular and paraseptal emphysema are important determinants in the preoperative assessment of bullectomy.6 Bullectomy causes significant improvement in breathlessness, work tolerance, exercise capacity, gas exchange and pulmonary function parameters. Moreover, studies have shown that bullae do not reappear and residual bullae do not become enlarged at the site of bullectomy.7
Before discharge from hospital, the patient should also be counselled against any further tobacco and marijuana abuse.
Case study follow up
Following confirmation of giant bullous emphysema, the patient successfully underwent bullectomy. One year post-surgery, the patient has remained clinically stable and symptom free.
Discussion
Aetiological factors attributed to giant bullous emphysema include chronic tobacco smoking, long term marijuana abuse and alpha-1 antitrypsin deficiency. While each of these aetiological factors may be independently responsible for this condition, it has been observed that marijuana smoking leads to asymmetric bullous disease at a younger age (approximately 20 years earlier) than chronic tobacco smoking.3,4 This is believed to be because marijuana smokers inhale more deeply and hold the smoke four times longer than tobacco users.
While long term marijuana abuse is occasionally known to cause VLS, the more common respiratory effects of prolonged marijuana smoking include increased cough, excess sputum production, chest tightness, pharyngitis, laryngitis, dryness of the throat, hoarseness of voice and persistent wheeze.8,9 Moreover, in patients with a history of bronchial asthma and chronic bronchitis, long term marijuana abuse is known to result in increased frequency of acute exacerbations.8,10
A patient with VLS commonly presents with acute breathlessness and chest pain, and on clinical examination the physical signs closely mimic those of a pneumothorax. However, radiographic features help to distinguish the two conditions. In cases of pneumothorax, the lateral margin of the collapsed lung is clearly seen, with the lung having collapsed medially in the direction of the hilum. In cases of giant bullous emphysema, where a giant bulla is present in the upper two-thirds of the lung, the lateral lung margin is not seen, as air is within the bullous cavity and not in the pleural space. Instead, the lower margin of the bulla is clearly seen with convexity downwards, and the normal lung parenchyma is below it, compressed between the bulla above and the hemidiaphragm below. These radiographic features help to distinguish giant bullous emphysema from a pneumothorax. However, in some cases, it may be radiographically difficult to distinguish the two conditions from each other, especially when a very large bulla occupies nearly the entire hemithorax.
Differentiating VLS from a pneumothorax is vitally important, as the treatment for both conditions is different. Bullectomy is the treatment of choice in patients with VLS. However, if the condition is mistaken for a pneumothorax and an intercostal drainage tube is inadvertently inserted into the bulla, this would result in the formation of an iatrogenic open pneumothorax with persistent air leaks. Insertion of an intercostal drain into a giant bulla could also lead to more serious complications such as haemothorax, haemorrhagic shock or death.
Key points
- Giant bullous emphysema or VLS is a chronic, progressive condition, usually seen in young people, predominantly males, who are chronic tobacco smokers and/or long term marijuana abusers.
- It is defined as a primary bullous disease of the lung in which a large emphysematous bulla occupies at least one-third of a hemithorax.
- Primary causative factors attributed to giant bullous emphysema include chronic tobacco smoking and long term marijuana abuse.
- Diagnosis is confirmed by HRCT chest scans that show giant bullae occupying at least one-third of the hemithorax, with the underlying normal lung parenchyma appearing to be ‘pancaked’ atop the hemidiaphragm.
- A definitive diagnosis of VLS is necessary for successful management, as this condition may be easily mistaken for a pneumothorax.
- Bullectomy is the treatment of choice in patients with giant bullous emphysema.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.