Case study
A man, 34 years of age, presented with a 4 day history of painless ulcerative lesions on his penis. He was human immunodeficiency virus (HIV) negative and had previously been well. He had received unprotected oral sex from a male partner about 3 weeks before the onset of the ulcers. There was no urethral discharge or dysuria.
Examination revealed discrete, nontender, superficial ulcers on the penis; 1–2 cm in diameter with rolled, indurated borders (Figure 1a, b). Bilateral inguinal lymphadenopathy was present. The remainder of the physical examination was unremarkable. A serologic test for syphilis showed a negative rapid plasma reagin test result.
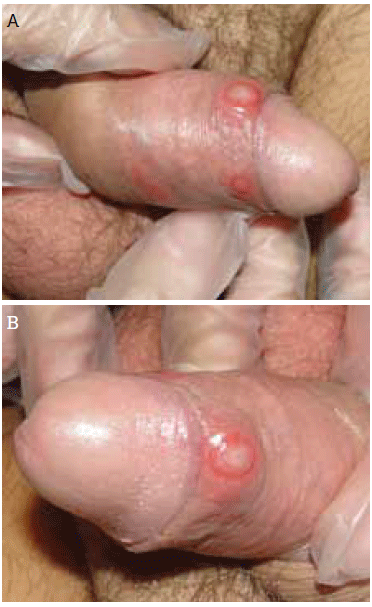
Figure 1a, b. Multiple ulcers on the patient's penis
Question 1
Based on the history and physical examination, what is the most likely diagnosis?
Question 2
What is the differential diagnosis?
Question 3
Why does the patient have a negative rapid plasma reagin test result and what other tests can be used to aid the diagnosis?
Question 4
What are the treatment options for early syphilis?
Answer 1
Primary syphilis is the most likely diagnosis. Syphilis is caused by the spirochete Treponema pallidum. It is mainly sexually transmitted, but transmission through blood transfusion or the placenta is also possible.1 The rate of syphilis has increased since 2001, with a high incidence in men who have sex with men. Many patients diagnosed with syphilis also have HIV.2 A primary syphilis lesion is an ulcer known as a chancre. It is typically indurated, with a clean base and rolled edges, and develops around 3 weeks after infection (10–90 days). The lesion may occur anywhere on the skin or the mucous membranes but usually appears on or near the genitals. Uncommon presentations of primary syphilis can also occur. Chancres may vary in size, number, shape, morphology and colour. This patient had several simultaneous syphilitic chancres on his penis, possibly due to traumatic injuries from oral sex.
Answer 2
The differential diagnosis for genital ulcers includes genital herpes, genital chancroid, drug eruptions, traumatic ulcers and Behçet disease. Typical presentation of these conditions include:3
- genital herpes is characterised by multiple, shallow, painful ulcers that may be vesicular; a history of recurrent disease may be elicited
- genital chancroid typically presents with a deep, undermined, purulent ulcer that may be associated with painful inguinal lymphadenitis
- Behçet disease is characterised by recurrent oral aphthae plus two of the following: recurrent genital ulceration, eye lesions, skin lesions or a positive pathergy test result.4
Chancroid and Behçet disease are very uncommon. If the patient acquired syphilis by performing oral sex, a syphilitic chancre may be noted in the oral cavity, buccal mucosa, tongue or lips.5 These syphilitic lesions can be misdiagnosed initially as herpetic or aphthous ulcers. Oral lesions may also be present in secondary syphilis, known as ‘snail tract’ ulcers.6
Answer 3
T. pallidum cannot be cultured in a laboratory. Therefore, syphilis must be identified by either direct visualisation of the organism in clinical specimens, or by serology. Serologic testing traditionally involves a nonspecific nontreponemal antibody test followed by a more specific treponemal test for diagnostic confirmation.7 Serologic tests for syphilis are divided into two types. One type, the reaginic nontreponemal tests (RPR) and venereal disease research laboratory (VDRL) are used for screening and to follow therapeutic response. The more elaborate T. pallidum based fluorescent treponemal antibody absorption test (FTA-ABS) is used for diagnostic confirmation. Although treponemal tests have higher specifity and sensitivity, they are not used for screening due to high cost. They are used to corroborate the accuracy of a positive reactive nontreponemal test.
The sensitivity of nontreponemal testing increases with the duration of infection.8 False negatives can be seen with very early infection (before serum antibodies have developed) or in a patient with a ‘prozone reaction’. Approximately 20–30% of patients presenting with a chancre will not yet have a reactive serologic test for syphilis.9 In this setting, testing for treponemal antibodies is usually also nonreactive. If clinical suspicion is high, repeated serologic testing is indicated 1–2 weeks later. Dark field microscopy from primary chancres or mucous membrane lesions of secondary syphilis is often diagnostic if available. A drop of expressed exudate or a scraping is needed in a wet prep on a microscope slide. This is the quickest and most direct method for diagnosing primary and secondary syphilis but access may be difficult. Polymerase chain reaction (PCR) testing for T. pallidum (using sequences of the DNA polymerase I gene) is also useful and has a sensitivity of 96% and a specificity of 96%. It does not cross-react with nonpathogenic treponemal species or other spirochetes.10
A second cause of a false negative test result is the ‘prozone reaction’. This phenomenon occurs in less than 2% of samples from patients with syphilis. The prozone reaction refers to nonvisualisation of agglutination, which normally occurs when antigen and antibody bind together to form a complex. When antibody titers are high (as in secondary syphilis), an overabundance of antibodies interferes with clumping of antigen-antibody complexes.
Finally, true positive results usually become nonreactive over time, even without treatment.
Answer 4
The efficacy of penicillin for the treatment of all stages of syphilis has been established over approximately 50 years of clinical use11,12 and there has been no reported resistance. The following treatment recommendations are consistent with current guidelines:
- a single dose of benzathine penicillin G (1.4 g IM) provides low but persistent serum levels of penicillin and is standard therapy for primary, secondary or early latent syphilis
- late latent syphilis or latent syphilis of unknown duration requires three doses of benzathine penicillin G (1.4 g IM) at 1 week intervals
- patients with penicillin allergy: Options for the treatment of early syphilis include tetracyclines, macrolides or ceftriaxone, although data is limited.13 Although macrolides have the advantage of single dose administration (2 g oral dose), there are reports of macrolide resistance. Therefore doxycycline 100 mg twice daily for 10 days for primary, secondary or early latent syphilis unless adherence is a significant concern when azithromycin may be used; 28 days of treatment are required for late latent syphilis. When alternative agents to penicillin are used, close follow up is essential. The effectiveness of alternatives to penicillin in the treatment of latent syphilis has not been well documented. In pregnancy, penicillin is preferred even in the penicillin allergic patient and penicillin desensitisation needs to be considered.
Contact tracing is essential and partners should be offered testing and empirical treatment. After treatment, patients should be monitored clinically and assessed serologically at 3, 6 and 12 month intervals. Declining nontreponemal antibody titers are reflective of successful therapy. A fourfold decline in titre, equivalent to a change of two dilutions (eg. from 1:16 to 1:4 or from 1:32 to 1:8) is considered a significant change reflective of a response to treatment.14 A confirmed fourfold increase in the nontreponemal titre signifies treatment failure requiring retreatment. Specific treponemal tests often remain reactive for extended periods in the majority of patients and should not be used to interpret treatment response.
Conflict of interest: none declared.