Case study
A man, 31 years of age, with type 1 diabetes, presents with a slightly pruritic plaque located on the lateral aspect of his left elbow. It has developed over 8 weeks, beginning as a 'sting' that has progressively extended. He reports no other symptoms.
On examination there is an erythematous plaque with nodular and pustular lesions on the inside (Figure 1). He has small, mobile axillary adenopathy. He is afebrile. The lesion has been treated with oral amoxicillin clavulanic acid for 10 days and topical mupirocin for several weeks without response. For the 2 days before the consultation, it was treated with topical antifungal (ciclopirox olamine cream) without clinical benefit. Direct microscopic examination and potassium hydroxide examination of skin scrapings, culture on dermatophyte test medium and punch biopsy (Figure 2) are performed.
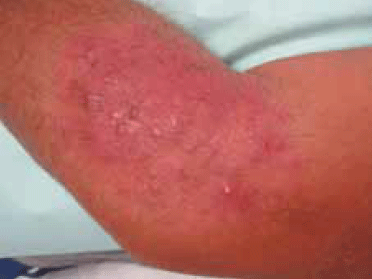
Figure 1. Lateral aspect of left elbow
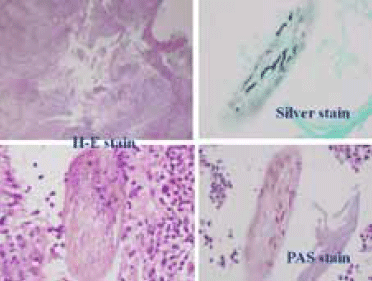
Figure 2. Histology from punch biopsy
Question 1
What is the most likely diagnosis?
Question 2
What is the aetiology of this condition?
Question 3
What factors can contribute to its development?
Question 4
Why suspect Majocchi granuloma? What diagnostic tests would you use?
Question 5
What is the recommended treatment for this condition? Would topical antifungal treatment be sufficient?
Answer 1
The most likely diagnosis is Majocchi granuloma.
Answer 2
Majocchi granuloma is a fungal infection caused by a dermatophyte, in this case Trichophyton rubrum. It is most commonly caused by dermatophytes of the genus Trichophyton, but it may be produced by either of the other two genuses of dermatophytes (Epidermophyton and Microsporum). Dermatophytes are keratinophilic fungi, so they routinely generate infection dependent on stratum corneum. However, Majocchi granuloma is a dermatophytosis that produces a folliculitis and perifolliculitis. The follicle is infected and, when it breaks, keratin is released into the dermis, producing a foreign body reaction that generates granulomas; there is cell destruction and release of acid mucopolysaccharides (amending the alkaline environment of the dermis).1 The most common organism associated with Majocchi granuloma is T. rubrum, both in immunocompromised and immunocompetent groups. Other dermatophytes involved are T. mentagrophytes, T. epilans, T. violaceum and M. gypseum.1
Answer 3
Two important risk factors are a near source of infection, such as tinea unguium or pedis, along with a previous trauma causing injury to a hair follicle. It has been suggested that misdiagnosis of the initial presentation leading to the inappropriate application of topical corticosteroids is a risk factor for tinea corporis manifesting as Majocchi granuloma.2,3 Other conditions associated with Majocchi granuloma are diabetes mellitus and immunocompromised status.4,5 Radentz and Yanase2 distinguish two distinct clinical forms of Majocchi granuloma: perifollicular papular or superficial form, which usually affects women who shave their legs and are immunocompetent, and a deep nodular or subcutaneous form, more common in immunocompromised patients, characterised by groups of firm or fluctuant nodules located in the head or upper limbs.
In the case study, the patient has type 1 diabetes. Majocchi granuloma has been described at the forearm in immunocompromised patients. Moreover, although the patient reports that he has not applied any topical corticosteroid, the lesion shows a pale peripheral erythema suggesting the application of corticosteroid treatment. Diabetes mellitus and the possible use of topical corticosteroid may justify the clinical presentation.
Answer 4
Clinical suspicion is essential. Features that may lead to consideration of the diagnosis in this case are the presence of pruritic and erythematous plaque and nodular lesions (a sign of perifollicular and follicular inflammation) with progressive growth over weeks. If no topical treatment is applied, dermatophytosis lesions show a scaly nature. If treated with antibiotics, antifungals or topical steroids there is no response or only a partial response.
If a fungal infection is suspected, it must be confirmed. Direct examination with potassium hydroxide (KOH) and culture on dermatophyte test medium is useful for confirming the dermatophyte infection. However, the confirmatory test about the deep granulomatous character of the infection is provided by the histopathology. It shows granulomas (foreign body or Langhans type) in middle and deep dermis. Dermatophyte structures are also identified as filaments or spores along with fragments of hair, as found in the case study (Figure 2).
If Majocchi granuloma is suspected, confirmation of the diagnosis is important by, at least, direct examination with KOH and culture. This is important as treatment requires an oral antifungal for several weeks and doctors who suspect a fungal infection may be discouraged by a partial response to topic antifungal that fails to completely heal the lesion. Therefore, in a patient with an indurate plaque with pustules and/or nodules that develops over weeks and with any of the risk factors described, a microbiological study can guide diagnosis and effective treatment. It is a condition that has a high risk of becoming a longstanding clinical problem if initially it is not properly treated.
Punch biopsy is a gold standard test to confirm the granulomatous nature of Majocchi granuloma. Practically, dermatophyte infections can be classified as dermatophytosis affecting the hair follicle (tinea capitis, tinea barbae or Majocchi granuloma), which require systemic treatment, and lesions affecting glabrous skin (tinea corporis, tinea cruris, tinea manuum), which usually only require topical treatment. As reflected in the study of Gómez-Moyano and Crespo-Erchiga,6 'the involvement of the hair follicle is a sign that directs to make systemic treatment'.
As it has been signalled, Majocchi granuloma is a follicular dermatophytosis. In cases where there is a diagnostic confirmation of dermatophytosis, some clinical variables should guide the use of a systemic treatment, such as the lack of response to topical antifungals, nodular lesions, follicular pustules or parasitism endothrix/ectothrix under potassium hydroxide examination.
Answer 5
As it is a dermatophyte infection that affects the hair follicle, systemic treatment is always required. Dose and treatment time is higher than for superficial mycoses. Recommended treatments are: griseofulvin at doses of 0.5–1.0 g/day for at least 8 weeks,7 itraconazole 200 mg/day for 30–90 days,8 or terbinafine until there is a clinical response (usually 15–30 days).9 Thus, the lack of response to a topical antifungal should not mean totally disregarding fungal causes.
In this case, the patient was treated with 1 g/day of griseofulvin for 2 months with a total improvement and without recurrence.
Because systemic treatment is always required, Majocchi granuloma is an entity that needs a high level of clinical suspicion before being treated. A common natural history of Majocchi granuloma is a lesion suspected as bacterial pyoderma treated with antibiotic without resolution, or a suspected fungal infection treated with topical antifungal that only shows a partial response.
Conflict of interest: none declared.