Although the older adult population has been a national focus, there are also demographic changes among the paediatric age group.1 These changes may also affect current and future aspects of the healthcare system and the workforce available to provide care to this segment of the populace.
General practitioners provide the vast majority of primary care services in Australia.4–5 These physicians provide primary care across the age span and are responsible for the care of children and adults.5,6 However, the demographic changes in the population over time may also affect the demography of patients attending general practices. As the overall population ages, it is possible that the patients attending general practices will increasingly comprise adults and seniors. This potential shift in the demography of general practices has the potential to result in diminished exposure of GPs to the care of children and, over time, less comfort and expertise in the care of children.
A similar trend has been experienced in the United States, where research has demonstrated changes in the demography of patients attending family physician practices (the United States equivalent of Australian general practices) consistent with the ageing demographic changes in that country.7 This has resulted in altered care patterns with more children seeking primary care from paediatricians.8
This study uses Medicare claims data and data from the Australian Bureau of Statistics to examine the impact of demographic trends in the Australian population, specifically the ageing of the population, on the demography of patients attending general practices.
Methods
Demographic changes in the population
To assess changes in the age of the Australian population via proportional and absolute numeric domains, we accessed data from the website of the Australian Bureau of Statistics. Data regarding the total number of those living in Australia each year from 1971–2010 were assessed by age. Age groupings of population counts for each year were constructed to match the five Medicare data age groupings: (1) 0–4 years, (2) 5–14 years, (3) 15–19 years, (4) 20–64 years and (5) >65 years.
The proportions of each age group relative to the overall population in each year were calculated. Graphs were constructed to show the numeric and proportional changes in population by age grouping over time. Similar processes were employed to assess population changes only from 1996–2010, corresponding to the time period for which Medicare claims data are available.
Demography of general practice patients
Medicare data were provided by the Medicare Information and Analysis Section of the Department of Health and Ageing. All claims for the most common general practice consultation service delivery codes (3, 23, 36 and 44) were requested. Data were received in an Excel file, with defined categories for visit numbers for each service delivery code grouped into the five age classifications noted above. Data were organised by state/territory and by individual year 1996 through 2010.
For each year of claims data, total visits were calculated by combining the counts for the four service delivery codes for each age classification by state/territory, and for the country as a whole. These counts were then placed in a single data file and graphed on line plots. Next, the proportions of the total claims for each age group relative to the total number of claims in a given year were calculated. Calculations were performed for each state/ territory and for the nation as a whole. These proportions were then placed in a single data file and graphed on line plots.
Results
Demographic changes in the population 1971–2010
There have been marked changes in the population of Australia during the 40 years from 1971–2010. The overall population has increased by 71% from 13.1 million to 22.3 million. However, the increase in population has not been uniform across all age groups, with the largest growth among those aged 20–64 years (92% increase) and >65 years (176% increase), and the smallest increases among those aged 0–4 years (16.9%), 5–14 years (10.9%) and 15–19 years (32%). Figure 1a demonstrates the change in total population among all age groups, while Figure 1b has the age group 20–64 years removed and the scale adjusted to better show the relative changes across the remaining younger age groups.
Although the absolute number of children increased during this same time period, the proportion of children as a percentage of the total population has decreased markedly. For those aged 0–4 years, the decrease was from 9.6% of the population to 6.5%; for those aged 5–14 years, the decrease was from 19.1% to 12.4%; and for those aged 15–19 years, the decrease was from 8.7% to 6.7%. Overall, from 1971–2010, the proportion of children aged 0–19 years in the population fell a combined 11.8%, from 37.4% to 25.6%. Figure 2 demonstrates the change in the proportion of the population among all the paediatric age groups.
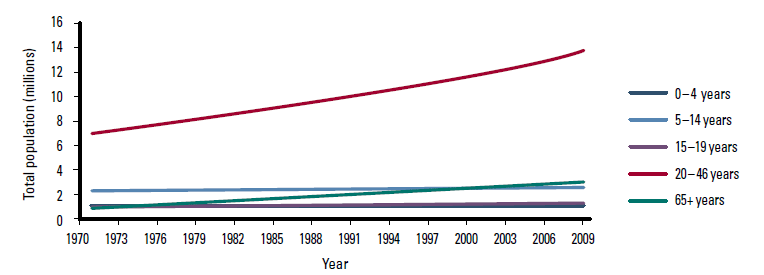
Figure 1a. Australian population: 1971–2010
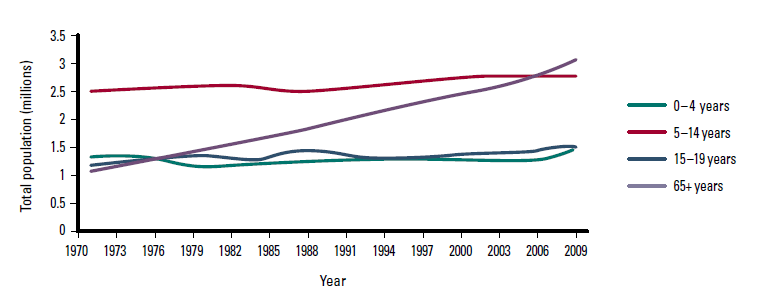
Figure 1b. Australian population: 1971–2010, excepting ages 20–64 years
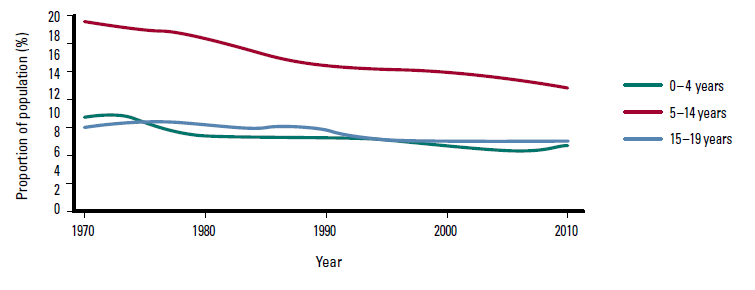
Figure 2. Ages 0–19 years as proportion of the Australian population
Demographic changes in the population 1996–2010
Medicare data to assess changes in the demography of patients attending general practices are only available for the years 1996– 2010. Therefore, assessments of the population changes for this specific time period are necessary to determine their association with changes in the demography of general practices over this more limited time period.
From 1996–2010, the overall population of Australia increased 22% from 18.3 million to 22.3 million. Again, the increase in population was not uniform across all age groups, with the largest growth among those aged 20–64 years (25% increase) and >65 years (36.6%). The smallest increases were seen among those aged 0–4 years (12.6%), 5–14 years (5.9%) and 15–19 years (17.3%).
These data demonstrate that most of the population growth of the younger age groups over the past 40 years actually occurred in the most recent 15 years.
Demography of general practice patient visits 1996–2010
There were changes in the demography of patients presenting for general practice consultations over the 15 years from 1996–2010. The proportion of patient visits in general practices made by those aged >65 years increased from 18.3% to 23.3%, an absolute increase of 5% but a relative increase of 27.3% for this age group.
Opposite trends were seen for those in younger age groups. The proportion of patient visits to general practices made by those aged 0–4 years decreased from 9.9% to 8.5% of total general practice visits, corresponding to a relative decrease of 16.4%. For those aged 5–14 years the decrease was from 8.9% to 6.9% of total general practice visits, corresponding to a relative decrease of 28.9%. For those aged 15–19 years, the decrease was from 4.9% to 4.3% of total general practice visits, corresponding to a relative decrease of 14%. Figure 3 demonstrates the change in proportions of general practice visits among all age groups, except for those aged 20–64 years. As this age group dominates the country demographically, their removal allows for adjustment of the scale.
These trends were consistent across all states and territories. Figure 4 illustrates these trends for the 0–4 years age group. Similar trends were seen for all other age groups of children.
The changes in the absolute number of visits to general practices from those of different age groups also varied widely. From 1996–2010, the number of visits for those aged 20–64 years increased from 49 million to 59 million; for those aged >65 years, the number of visits increased from 15.4 million to 24.4 million. For the paediatric age ranges, the changes were more modest. For those aged 0–4 years, the increase was from 7.9 million to 8.2 million visits; for those aged 5–14 years, there was a decrease from 7.5 million to 7.1 million visits; and for those aged 15–19 years, there was an increase from 4.2 million to 4.5 million visits. Overall, for the paediatric population as a whole, there was an increase of 0.2 million visits from 1996–2010. Figure 5 demonstrates the change in numbers of general practice visits with the age group 20–64 years again removed to better show the relative changes across the remaining smaller age groups.
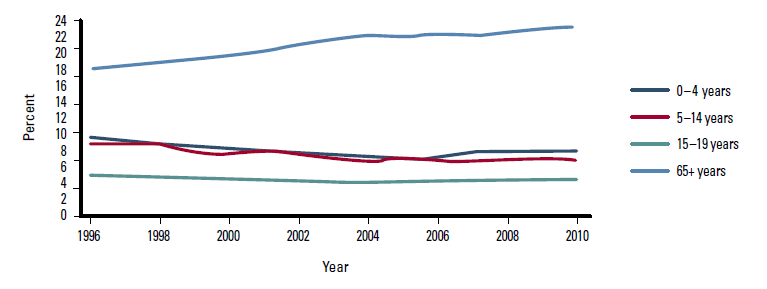
Figure 3. Proportion of general practice visits by age, 1996–2010, excepting ages 20–64 years
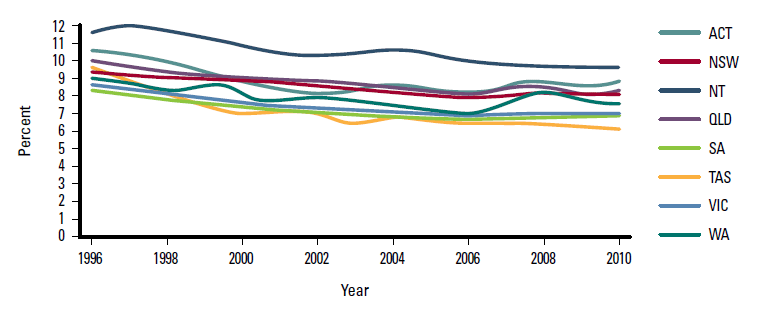
Figure 4. Visits to general practice by those aged 0–4 years, by state/territory, 1996–2010
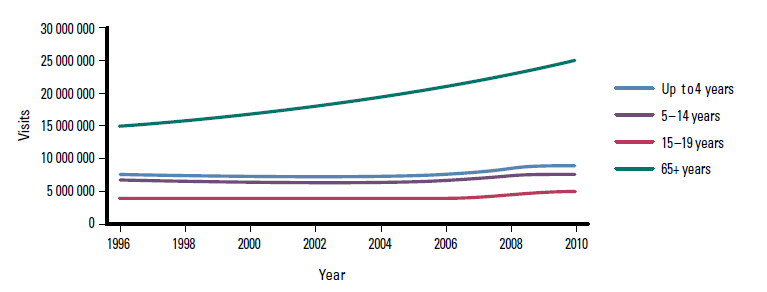
Figure 5. General practice visits by age group 1996–2010, excepting ages 20–64 years
Discussion
Important limitations regarding the datasets used in this study are as follows:
- Only the most common Medicare consultation codes were used in the analysis (ie. 3, 23, 36, 44). The newer 700 series codes used for Health Assessments were not included as they have only been in use for <2 years and their use by GPs is in transition. At this time, they have been used by GPs primarily for consultations with adults and seniors. As such, their inclusion would have skewed the results to further exaggerate the trends in visit proportion increases for adults and decreases for children. Thus, their exclusion may have resulted in a more conservative view of the trends described
- It is possible that some of the Medicare item numbers billed reflect care provided by practice nurses rather than GPs
- We have not included data regarding emergency department (ED) visits. There have been increases in the volume of care provided to children in EDs over the study period9 and it is possible that there may be a substitution effect of ED visits for GP visits. However, we contend that EDs should not function as a replacement for primary care for children and that any increase in ED visits only serves to further diminish exposure of GPs to the care of children
- Another possibility is that Health Direct, the national 24 hour helpline (available in some states for some of the MBS data period) may account for at least some of the decrease in GP visits.
Despite these limitations, the data clearly point to a marked decrease in the proportion of visits to general practices made by children over the time period 1996–2010. This trend is consistent with the concurrent changes in the demography of the population of Australia. Further, at the same time that the actual population of children in the country has increased by >10%, the number of visits to GPs by this segment of the population has remained relatively unchanged (<1% change). By contrast, visits by adults and seniors have risen both proportionally and in absolute numbers. The demographic ageing of the country is set to continue for the foreseeable future, resulting in an even greater decrease in the proportion of patients in the paediatric age range seen by GPs.
The change in proportion of visits to general practices may have several implications for the care of children in Australia, now and in the future. As visits for children become an even smaller fraction of the overall visits for GPs, the continued comfort level and competency to address the primary care of acute and chronic illness in children as well as the recognition and care for normal and abnormal development may be affected. A similar demographic trend in the United States among both the population and family physician practices has resulted in concerns about patient care for children by family physicians. Some family physicians have begun to limit their practices to the care of adults as the proportion of children in their care shrinks to levels that make it difficult to maintain their skills.8
According to our data, the impact of these trends on general practices also differs marginally by state and territory: states and territories with older populations and a smaller proportion of children (eg. Tasmania) have a more pronounced paucity of general practice paediatric patient visits than some others with a higher proportion of children (eg. Northern Territory). However, these data are likely to be confounded by multiple issues (including the proportion of the population that is Indigenous and rural and socioeconomic status) that are beyond the scope of this analysis.
Another potential outcome of the decrease in the proportion of paediatric visits for GPs is increased referrals from GPs to general paediatricians and/or paediatric subspecialists. As general practices become increasingly focused on the care of adults and seniors, GPs may be less able or willing to focus on timeconsuming issues of paediatric care, including developmental and behavioural and issues, obesity and the primary care of chronic illness. A recent study documented that approximately one-third of all visits to general paediatricians in Australia are for behaviour and development issues and the number is growing.10
As the demographic trends described above continue, and the proportion of children in general practices continues to decrease, it is reasonable to assume that ongoing general practice clinical experience and comfort levels in the care of children may further erode over the coming decade. A greater focus for GPs on continuing professional development targeting paediatric issues may be part of the solution. However, workforce issues are also likely to be relevant. To inform future decision making around these issues, additional research may assist, including those described in Table 1.
Table 1. Areas for further research
- Assessment of the current baseline of referral to paediatricians among GPs, and how this will change over the next decade
- Workforce assessments of the adequacy of general and subspecialty paediatricians to handle potential increases in referrals over time
- Investigation into rates of referrals of children, urban/rural differences in referral patterns and wait times for ambulatory care from general paediatricians or paediatric subspecialists
|
Conclusions
It appears that most of the public and political focus on the healthcare system in Australia is on the ageing population.11 This is understandable given the current demographic trends. However, there is a danger if this focus results in a myopia that excludes or diminishes the examination and assessment of the care of other segments of the population. Simply put, there are not fewer children in Australia today than 15 years ago. We must not confuse their decreased proportion of the population with a decrease in absolute numbers. Thus, proportional allocation of time and resources, while simplistic to consider, may not be the most effective strategy for health system resource allocation going forward.
GPs are the fundamental base of the healthcare system, but are stretched in many directions. The increased proportion of their patient population comprised of adults and seniors with multiple chronic diseases and taking multiple medications rightly demands their attention. Over time, continued population trends will require even greater focus of GPs on this population. However, although demographic projections indicate children will become a smaller and smaller proportion of the Australian population in the future, their absolute numbers will continue to rise modestly. As such, the primary care of this population must continue to be a priority of the healthcare system. To ensure the adequate provision of services to this paediatric population, careful ongoing monitoring of general practices, referral patterns and comfort levels in the care of children must be undertaken. The future of the country demands no less.
Conflict of interest: none declared.
References