Case
A woman, aged 29 years, presented to her general practitioner (GP) with a 12-month history of multiple skin-coloured nodules on the palmar aspect of her fingers bilaterally. The nodules were painless, but frequently interfered with her work as a florist. On examination, the nodules were 1–2 cm in diameter, firm, mobile and non-tender to palpation (Figure 1).
A full blood count and angiotensin converting enzyme level were normal. Serology for rheumatoid factor and anti-cyclic citrullinated peptide (anti-CCP) were negative. A chest radiograph performed six weeks earlier for an unrelated complaint was reported as normal. Excisional skin biopsy showed lymphohistiocytic palisades surrounding degenerated collagen and mucin within the subcutis.
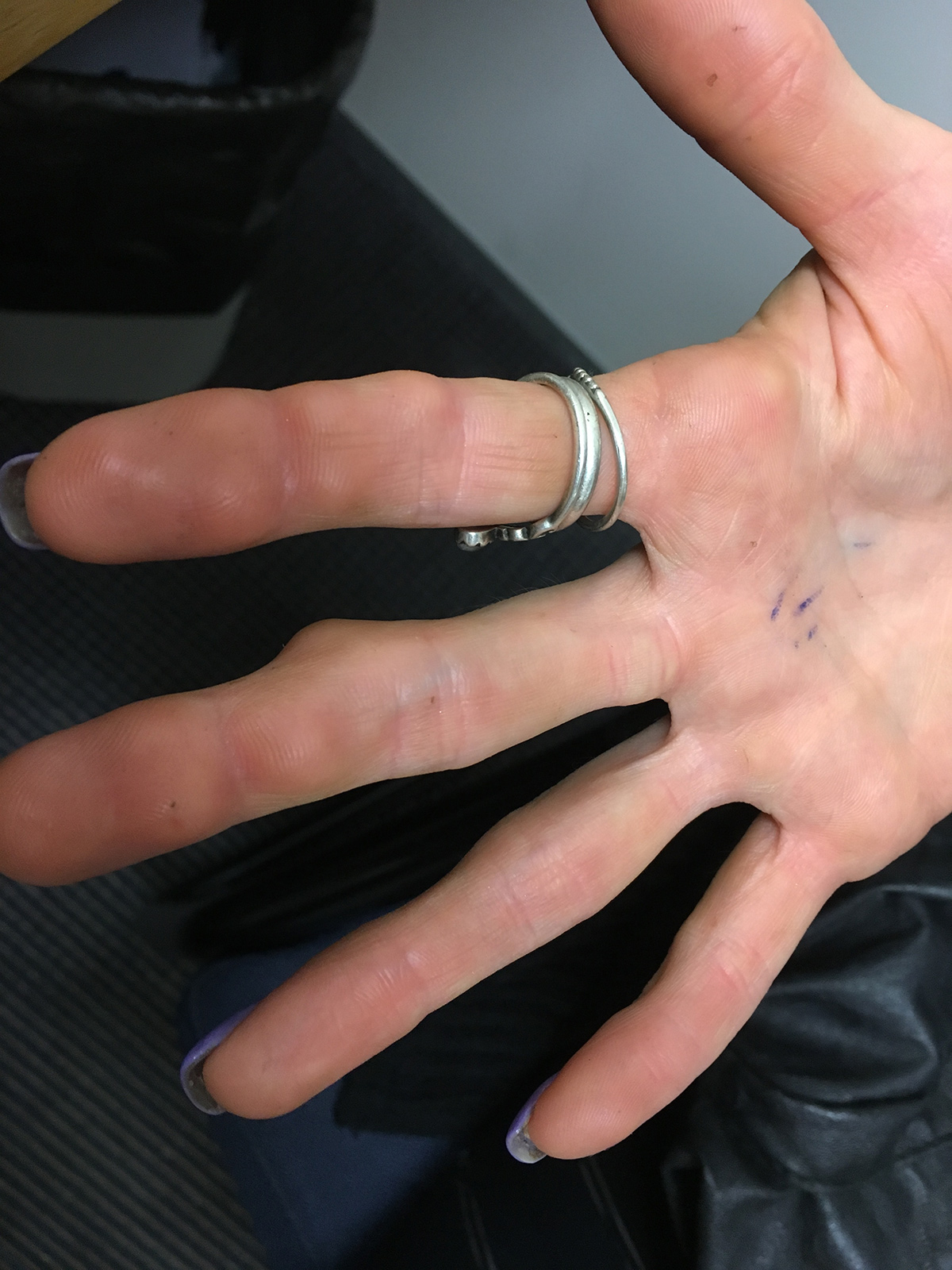
Figure 1. Multiple subcutaneous nodules on palmar hand
Question 1
What are your differential diagnoses for this case? What is the most likely diagnosis?
Question 2
How does the diagnosed condition usually present?
Question 3
How is this condition diagnosed?
Question 4
What are the other variants of this condition?
Question 5
What disease associations should be considered?
Question 6
How is this condition managed?
Answer 1
Possible differential diagnoses include:
- rheumatoid nodules
- sarcoidosis
- deep fungal or bacterial infections
- subcutaneous granuloma annulare (SGA)
- necrobiosis lipoidica.
SGA was considered the most likely diagnosis for this patient. Rheumatoid nodules and cutaneous sarcoidosis were excluded on the basis of negative laboratory findings and imaging. The presence of mucin deposition on histology made necrobiosis lipoidica unlikely.1,2
Although the exact cause of SGA is unclear, it is known to be a type IV hypersensitivity reaction to dermal components, in which inflammation is mediated by tumour necrosis factor alpha.3
Answer 2
SGA usually presents as single or multiple deep dermal or subcutaneous skin-coloured nodules on the hands, anterior lower legs, scalp or buttocks. Lesions are typically painless and <4 cm in diameter. SGA is most commonly seen in children, but can also affect patients of other ages, as seen in this case.4
Answer 3
The absence of overlying skin changes in SGA often makes clinical diagnosis challenging. Excisional skin biopsies are usually required to distinguish SGA from skin disorders with similar clinical features (eg rheumatoid nodules). Blood tests are generally only useful for excluding other diagnoses. Clinical examination is often sufficient for the diagnosis of SGA.
Answer 4
Other variants of granuloma annulare are presented in Table 1.
Table 1. Other subtypes of granuloma annulare13
|
Localised
(most common)
|
Asymptomatic skin-coloured or erythematous annular or arciform plaque(s) with rope-like border and central clearing on distal extremities14
|
|
Generalised
|
Widespread skin-coloured to erythematous papules and plaques. Trunk and extremities most commonly affected. Pruritus may accompany generalised GA15
|
|
Perforating
|
Asymptomatic erythematous papules that evolve into yellowish umbilicated papule that discharge white/yellow fluid. Most commonly seen in children and young adults16
|
|
Patch
|
Annular or non-annular non-scaly patches. Most often on the proximal extremities17
|
Answer 5
SGA may be associated with diabetes mellitus,5 and patients should be probed for suggestive signs and symptoms. Routine serum testing is not required unless otherwise indicated. SGA may also be associated with lymphoma and this possibility should be explored, particularly in older adults with atypical presentations.6 Dyslipidaemia,7 thyroid disease8 and human immunodeficiency virus infection9 have also been implicated in SGA.10
Answer 6
Intervention is not usually required as SGA is self-limiting and reassurance is sufficient. Half of patients achieve spontaneous resolution within two years.11 As such, it is appropriate to offer reassurance. However, those who strongly desire treatment may be referred to a specialist for consideration of intralesional corticosteroids, cryotherapy and/or phototherapy. Treatment options for generalised granuloma annulare include topical calcineurin inhibitors and phototherapy.12 Recurrence is common after surgical excision. Persistent or troublesome cases of SGA could be referred to a dermatologist for consideration of treatment.
Key points
- SGA is most commonly seen on the hands of children.
- Granuloma annulare has a number of subtypes of which subcutaneous variant is one of the rarer forms.
- Diagnosis is often challenging clinically and may require skin biopsy for confirmation.
- Treatment is usually not required as SGA is self-limiting and resolves in months to years.
Authors
Olivia A Charlton BAS, MBBS, RMO, St George Hospital, Sydney; UNSW, Kensington, Sydney, NSW. oacharlton@gmail.com
Thomas J Stewart BBioMedSc (Hons), MBBS, Southderm Research Fellow, Southderm, Kogarah, NSW; UNSW, Kensington, Sydney, NSW
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.