Case
A man, 28 years of age, presented to an emergency department with a seven-day history of lethargy, which he attributed to the recent stress of working on a university thesis. The day before, he developed what he described as mouth ulcers, which progressively became more painful, causing some dysphagia.
He had previously been prescribed modafinil for narcolepsy, although he took this intermittently while studying. His last dose of modafinil was four days before he developed the mouth ulcers. He had no other significant past history and was on no other medications. On examination, there were white sloughy blisters in the labial mucosa and raised ulcerative areas in the hard palate. There were also four well-circumscribed, firm blisters in the buccal mucosa. Systemically, he was well and there were no adverse findings on thorough examination.
Blood profiles were taken for haematology, biochemistry and inflammatory markers, which returned within acceptable parameters. A blister was aspirated for virology, and for microscopy, culture and sensitivity (MC&S). He was discharged at the time, instructed to stop taking the modafinil and requested to return to the dermatology clinic the next morning.
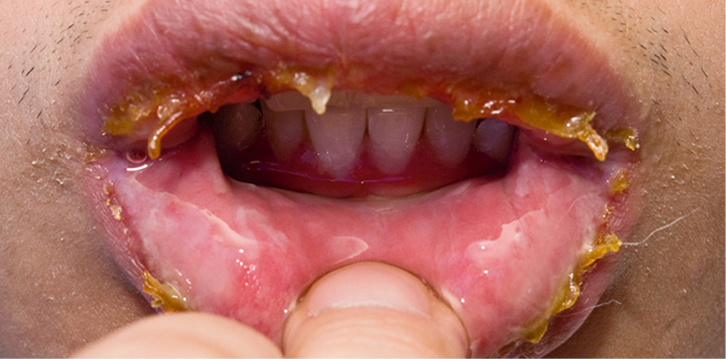
Due to university stressors, he did not return until two days later when he developed odynophagia, sloughing of the labial mucosa, crusty haemorrhagic lesions over the upper and lower lips (Figure 1) and target lesions over the abdomen, genital region and upper limbs (Figure 2).
 |
 |
| Figure 1. Sloughing of the labial mucosa |
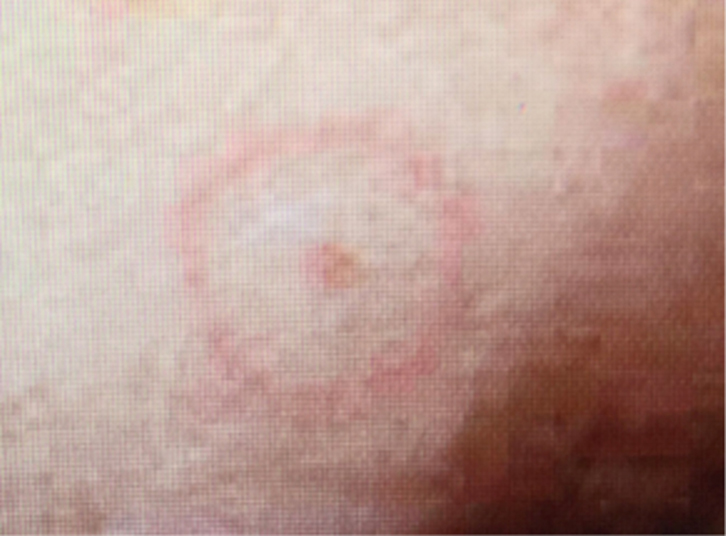
Figure 2. Target lesion on finger |
Question 1
What are the possible diagnoses?
Question 2
What is the pathophysiology of the diagnoses?
Question 3
What is the most likely cause of this condition?
Answer 1
The possible diagnoses for this patient are:
- autoimmune disorder (eg pemphigoid vulgaris)
- herpetic gingivostomatitis
- Stevens–Johnson syndrome (SJS).
Answer 2
Autoimmune disorders (eg pemphigus vulgaris) occur when the body’s immune system attacks and destroys healthy body tissue. Causes of autoimmune disorder can include drug therapy and recent viral infections, and it is commonly associated with malaise, fever and joint pains. Pemphigus vulgaris is a rare autoimmune disease that is characterised by blisters on the skin and mucous membranes, usually starting in the mouth. Pemphigus vulgaris always has a positive Nikolsky sign, which is the dislodgement of intact superficial epidermis by a shearing force, resulting in exfoliation of the outermost layer forming a blister within minutes.1–3
Herpetic gingivostomatitis is an inflammation of the oral mucosa and gingiva, predominantly caused by the Herpes simplex virus, that mainly affects children. Herpangina is another oral ulcerative condition caused by the coxsackie A virus.4,5
Stevens–Johnson Syndrome (SJS) is an immune complex-mediated hypersensitivity disorder that may be caused by drugs, viral infections or malignancies, or it can be idiopathic. SJS is characterised by confluent epidermal necrosis with minimal associated inflammation caused by cell death, forcing the epidermis to separate from the dermis. SJS is considered a milder form of toxic epidermal necrosis (TEN).
SJS and TEN are differentiated by using Bastuj’s classification, which is based on the type of lesions, extent of blisters and erosions on the total body surface. Blisters and erosions cover 3–10% of the body in SJS, 10–30% in overlapping SJS/TEN and more than 30% in TEN.6–8
SJS generally starts with an insidious onset of non-specific, upper respiratory tract infection, then a 1–14-day prodrome of fever, sore throat, diarrhoea, headache and fatigue, with mucosal membrane lesions developing, followed by lesions over the torso and genital area. Conjunctivitis occurs in approximately 30% of children and 3–10% of adults
with SJS.6
The rash resembles a target, which is considered pathognomonic. Mortality is determined primarily by the extent of skin sloughing. When total body surface area sloughing is less than 10%, the mortality rate is approximately 1–5%. However, when more than 30% is present, the mortality rate is 25–35%.6–9 It has a positive Nikolsky sign.7,8
Answer 3
The most likely cause is modafinil, which has been documented as a catalyst in SJS.6,9 It is a psychostimulant, wakefulness medication that is available on the Pharmaceutical Benefits Scheme (PBS), although authority is required by a qualified sleep medicine practitioner or neurologist. The direct action of the drug is unclear, but it is thought that it alters the neurotransmitters in the brain.10,11
Case continued
A tissue biopsy was taken from a target lesion and sent for histology. It confirmed a diagnosis of SJS. The method used direct immunofluorescence to exclude pemphigus.
Question 4
What is the management for this patient?
Answer 4
Treatment is usually symptomatic, with careful attention paid to airway management and haemodynamic stability. Therapy for a patient with SJS would include, but is not limited to:
- withdrawal of the offending drug – certain medications have been linked to SJS and should be avoided (eg modafinil, nonsteroidal anti-inflammatory drugs and sulphur-based medication).6–8,12 The patient should be strongly advised to stop using the offending drug and consider wearing a MedicAlert bracelet
- admission to hospital considering the vulnerability of the patient’s airway and possibility of compromise
- analgesia – a topical local anaesthetic such as mouth irrigation with viscous lignocaine gel can give relief to allow oral analgesia to be taken; however, care must be taken to avoid local anaesthetic toxicity11,12
- mouth care – mouth lesions have been known to erupt for as long as 14–21 days and can extend into the oesophagus, with mucosal shedding in the tracheobronchial tree, leading to respiratory failure6–8
- urgent dermatology review
- chest X-ray to exclude pneumonitis4
- fluid intake – fluid resuscitation with correction of electrolyte imbalance
- tetanus prophylaxis
- treatment as per the burns protocols if there are any external skin eruptions
- use of corticosteroids – this is controversial and some authors report that use of corticosteroids can increase the length of hospital stay, increase the rates of infection and lead to more complications3,6,7,9,13–16
- ophthalmology review – ocular sequelae can include corneal ulceration and anterior uveitis.6 Blindness, secondary to severe keratitis or panophthalmitis, may develop in 3–10% of affected patients. The use of lubricating eye ointments is advocated.
Author
Karen Broadbent DipAsthma (NARTC), DipDiabetes, PGradDipClinNsg, MN,RN, Emergency Nurse Practitioner, Fiona Stanley Hospital, Perth, WA. rusty07@iinet.net.au
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.