There is a high level of (mis)information about cannabis, its medicinal applications and addiction liability, which add to confusion in providing good patient care. Increasing prevalence, particularly daily use, among those reporting that they use cannabis for medical conditions1 means that screening and intervention are increasingly important.
Prevalence of cannabis use and its associated disorder
Cannabis is the most commonly used illicit drug of dependence in the Western world.2 The Diagnostic and statistical manual of mental disorders, 5th edition (DSM-5) has amended the nomenclature to a cannabis use disorder severity continuum;3 however, the term cannabis dependence will be used as that was correct at the time of publication.
The 2013 National Drug Strategy Household Survey reported that around one in 10 Australians (10.2%) aged >13 years used cannabis in the previous year, and more than one-third (35%) had tried it.4 Among recent cannabis users, 12.8% are daily users. The age group with the highest prevalence of recent cannabis use are those aged 20–29 years, with 24.7% of males reporting use.
While cannabis is mostly used experimentally and occasionally, approximately 6% of all Australians will meet the criteria for cannabis dependence in their lifetime, and 1% in the past 12 months. The rates of meeting the criteria for cannabis dependence among those who used it at least five times in the previous year has increased to 14.3%.5 Current cannabis use disorders are more common among males and younger users. Those who used cannabis before 17 years of age were found to be 18 times more likely to develop cannabis dependence by 30 years of age than their peers who did not use cannabis.6
Harms
Although cannabis has a very low acute toxicity, its related morbidities are a major public health burden. A recent study of mortality and morbidity attributable to cannabis reported a relative risk of >2 based on at least 50 occasions of cannabis use.7 Cannabis dependence is the most common harm. Those who are dependent on cannabis are at a higher risk of experiencing the negative consequences of using the drug, such as short-term memory impairment, mental health problems and respiratory diseases (if cannabis is smoked).2 Regular use and dependence can also lead to problems with finances, conflict in relationships with family and friends, and employment problems.8
As cannabis is almost always smoked, and most often mixed with tobacco in blunts or smoking mixtures, there is a risk of adverse respiratory effects. These include chronic cough, sputum production, wheezing and bronchitis, even after controlling for tobacco use.9 Cardiovascular events, such as stroke and heart attack, are also potential health risks.10 Certain groups may be at a higher risk of developing adverse acute and chronic effects of cannabis. These groups include adolescents, pregnant women, those with underlying or pre-existing respiratory or cardiovascular disease or vulnerability, and those with comorbid disorders.11 The onset of cannabis use in early adolescence poses particularly high risks of serious adverse physical and mental health, and social/academic consequences. These include increased risks of cardiovascular disease, depression and anxiety, and poorer academic achievement – again potentially persisting into adulthood. There is also evidence to suggest that cannabis use increases the risk of suicide attempts, particularly among the young.6
The issue of comorbidity of cannabis and other substance use disorders (eg alcohol) with mental health disorders (eg anxiety, depression, schizophrenia) is a clinical concern that occurs relatively frequently. For patients who are vulnerable to psychotic disorders, cannabis use precipitates the disorder three years earlier on average, increases the rate of non-compliance with medication, and increases hospitalisations.11
As well as the direct effects of cannabis on the psychological and physical health of the user, its use increases the risks of injury or death while driving or operating equipment at work.12
Presentations and screening
Despite the availability of efficacious treatments for cannabis use disorders, only a minority will identify their cannabis use as problematic.6 Various barriers can inhibit treatment seeking, including not being aware of treatment options, thinking treatment is unnecessary, wanting to avoid the stigma associated with accessing treatment, concerns about confidentiality, lack of accessibility, and costs of treatment.13 When adults do present for cannabis treatment, they have typically used cannabis for more than 10 years, with multiple failed attempts to quit.15 Adolescents who use cannabis are usually coerced into presenting for treatment; families, schools or the legal system typically initiate efforts to access assistance for them.16
Those who use cannabis may seek assistance for problems such as poor sleep, anger, depression, anxiety, psychosis, relationship issues, or respiratory problems,15 but not mention their cannabis use to the general practitioner (GP). Several valid and reliable screening tools are available for the detection of current and longer term (12 months) problems related to cannabis use. These screening tools can be found on the National Cannabis Prevention and Information Centre’s (NCPIC) website (refer to ‘Resources’).
Assessment and intervention flowchart
The flowchart shown in Figure 1 sets out the steps in the assessment and brief management of cannabis use and cannabis-related problems. This flowchart is available at the NCPIC website (refer to ‘Resources’). For example, the Severity of Dependence Scale is a short, five-item measure of the degree of cannabis dependence.17,18 The importance of simple screening and very brief advice, with provision of psychoeducational materials, cannot be overemphasised. Even very brief interventions of around 20 minutes have been found to positively influence levels of cannabis use among users of cannabis who are not seeking treatment.19
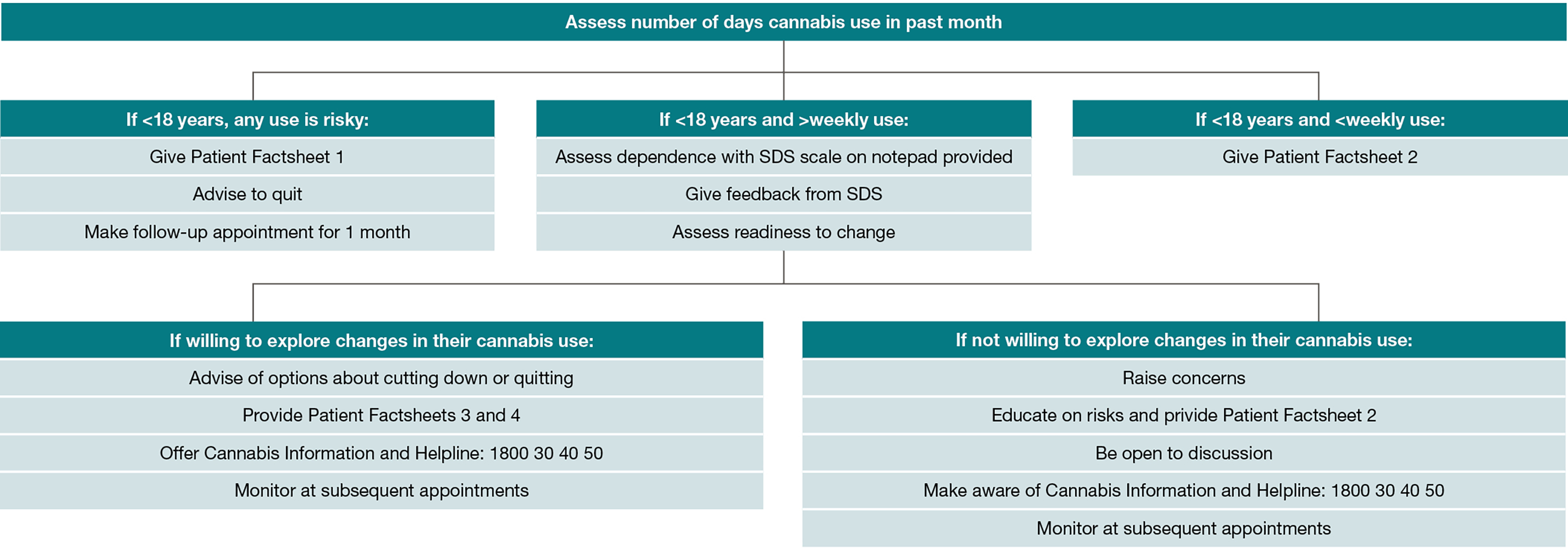
Figure 1. Algorithm to assess and manage cannabis use
Reproduced with permission from the National Cannabis Prevention and Information Centre. Management of cannabis use disorder and related issues – A clinician’s guide. Sydney: University of New South Wales, 2009. Available at https://ncpic.org.au/media/3069/gp-kit_resource-pack.pdf [Accessed 27 September 2016].
SDS; Severity of Dependence Scale
The demand for the treatment of cannabis use disorder is increasing internationally. Almost one in four (24%) people in specialist alcohol and other drug treatment services in Australia are presenting for a cannabis use concern.20 Adults who use cannabis and seek professional help typically report numerous problems related to their cannabis use, some clearly related to core dependence criteria (eg inability to stop or cut down, withdrawal symptoms).15 Other issues prompting treatment include relationship, family and financial difficulties, health concerns, and poor life satisfaction.
Management
For patients who are interested in further discussion of their cannabis use, psychoeducation (refer to ‘Resources’) and one to six sessions of cognitive behavioural therapy (CBT) within a motivational interviewing framework has the strongest evidence base.21
Cannabis withdrawal
Barriers to abstinence that patients may experience are cannabis withdrawal symptoms. The most troubling withdrawal symptoms reported by clinical populations include irritability or restlessness, low mood, sleep disturbance and gastrointestinal discomfort.22 Cannabis withdrawal symptoms significantly affect attempts to quit, and are associated with functional impairment to daily activities, substance use to alleviate cannabis withdrawal symptoms, and increased frequency of cannabis use.23 The duration is typically five to seven days with symptoms peaking on day one or two. Efects on sleep may persist for longer (weeks or even months).24 Cannabis withdrawal symptoms are also strongly associated with relapse, highlighting the importance of ongoing assessment and monitoring of withdrawal symptoms as part of treatment.
Psychosocial interventions
The majority of those with cannabis use disorders go on to manage their disorder and/or abstain from use without formal treatment.25 The strongest evidence base is for individualised psychosocial interventions.21 Primary approaches to the planning, cessation or reduction of cannabis use, and maintenance of abstinence, have included motivational enhancement therapy (MET), CBT and contingency management. Supportive psychotherapy and family system approaches have also proved effective. Support groups, such as 12-step and SMART (self-management and recovery training) programs, can also be of assistance for some patients and families.
Motivational enhancement therapy
MET aims to resolve ambivalence around changing cannabis use behaviours, thereby increasing the patient’s motivation to change. The tenets of the therapy rest on empathy and non-judgemental interactions, using open-ended questions and validation, increasing cognitive discrepancy between actual and desired behavioural states, avoiding confrontation, and supporting clients’ own self-efficacy.26 Studies have found that two brief MET sessions with adolescents who use cannabis are promising for increasing motivation for change and reducing cannabis use.16
Cognitive behavioural therapy
CBT focuses on altering the learned behaviours of cannabis users in order to change their current behaviour patterns with cannabis use, so as to increase the opportunity to use adaptive behaviours instead. It focuses on recognising and limiting the ‘cues-and-use’ circumstances, and moderating the precipitators of drug use. CBT has proved to be beneficial in the treatment of cannabis dependence and can be combined with MET.21
Pharmacotherapy
Currently, there is no evidence-based pharmacotherapies for the management of cannabis withdrawal or craving. Early-stage studies of pharmacotherapies have largely focused on cannabis withdrawal. Agonist therapies have shown the most promise. The most innovative and encouraging results have been seen with nabiximols (not listed on the Pharmaceutical Benefits Scheme), which has demonstrated efficacy for reducing the severity and time course of cannabis withdrawal. It also appeared to increase retention of participants in withdrawal treatment.23
Conclusion
Cannabis use and cannabis use disorders are common. They frequently co-occur with other substance use disorders and mental health conditions, and should be assessed and treated concurrently.
There is no evidence-based pharmacotherapy for cannabis dependence, but recent studies with agonist therapies have shown promising early results. The strongest evidence for treatment efficacy is for one to six sessions of CBT, with predictors of successful treatment including active coping strategies and distress tolerance. The evidence base for technological platforms such as computers, telephones and smart phone applications as prevention and intervention tools is also being established.
Resources
Author
Jan Copeland PhD, Director, National Cannabis Prevention and Information Centre, Medicine UNSW, Sydney NSW. J.Copeland@unsw.edu.au
Competing interests: Jan Copeland is the founding Director of the National Cannabis Prevention and Information Centre at UNSW Medicine, which is funded by the Australian Government. She led the National Health and Medical Research Council (NHMRC) study into nabiximols and was provided the drug by GW Pharmaceuticals at no cost and with no other consideration. She does not consult for, own shares in, or receive funding from any company or organisation that would benefit from this article, and has no relevant affiliations.
Provenance and peer review: Commissioned, externally peer reviewed.