Extensive lip ulcers
Thank you for the illustrated case of oral erythema multiforme by Kooi-Yau Chean1 (AFP July 2014). This dangerous drug reaction is an important consideration prior to the commencement of carbamazepine and related drugs. However, in Australia it is not easy to implement this in practice.
Firstly, while Asians of Han Chinese ethnic background have HLA B*15:02 as the predictor of Stevens-Johnson syndrome and related severe drug reactions, Caucasians of European background have a different predictive marker, HLA A*31:01.2 In certain domains, recommendations have been made to test HLA B*15:02 where ethnically indicated, but it has not been widely recommended to test HLA A*31:01 on current evidence. It is further complicated when considering patients of Eurasian, South Asian, Korean and Japanese background.
Secondly, the specific tests for HLA B*15:02 and HLA A*31:01 are not currently reimbursed by Medicare, although they are available through limited private pathology providers and also through the Australian Red Cross blood service. Patients may be asked to pay a private fee of $60–220 in some cases.
Unfortunately, this is a situation where science and ideal practice have moved ahead of practical medicine. Clinicians should bear this in mind when discussing potential carbamazepine treatment and related drugs with their patients.
Associate Professor Stephen Reddel
Department of Neurology, Concord Hospital, NSW
swreddel@sydneyneurology.com.au
Genetics in general practice
It was interesting to read the recent Focus article, ‘Genetics for general practitioners’, by Blashki et al3 (AFP July 2014). Apart from thalassaemia screening, there was no mention of antenatal or prenatal genetic counselling for inherited diseases of childhood. I would have considered this an ideal role for general practitioners (GPs), particularly those undertaking shared care obstetrics, but also any GP helping a couple to plan a pregnancy. Questions about family history are not sufficient to identify patients at risk of recessive conditions, as parents will be healthy carriers. The frequency of cystic fibrosis (CF) carriers is 1 in 25 in our community. The Human Genetics Society of Australasia (HGSA) recommends that all pregnant women, or those planning a pregnancy, be made aware of the availability of carrier screening for CF.4 Spinal muscular atrophy (SMA) is less common – carrier frequency is 1 in 40 – but SMA is a devastating illness and most babies who are affected die before the age of 12 months. It is also possible to screen for Fragile X syndrome, the most common inherited cause of intellectual disability. As screening for these conditions is now available, there is no need for parents to have their first child with these conditions to find out they are carriers. Fee-for-service tests are available (there is no Medicare Benefits Schedule item rebate) through public and private pathology services across Australia, and many in vitro fertilisation services also make screening available. Interested patients do not have to reside in the state offering the test (blood can be sent interstate) and genetic counselling can be offered by the GP or testing service.
Associate Professor Dr John Massie
Department of Respiratory Medicine, Royal Children’s Hospital
Associate Professor David Amor
Director, Victorian Clinical Genetics Services, Murdoch Childrens Research Institute
References
- Blashki G, Metcalfe S, Emery J. Genetics in general practice. Aust Fam Physician 2014;43:428–31.
- Human Genetic Society of Australasia. Position Statement. Population-based carrier screening for cystic fibrosis. 2013PS03. Sydney: Human Genetic Society of Australasia, 2013. Available at www.hgsa.org.au/documents/item/1282 [Accessed 7 October 2014].
Reply
We thank Associate Professors Massie and Amor for their interest in our paper and we are in agreement with them that GPs are ideally placed to discuss antenatal and pre-pregnancy carrier screening with their patients, even in the absence of family history risk factors. We agree it is a common misconception among the community that couples without a family history are not at risk of being carriers for recessive conditions. Given the broad scope of the topic, we did indicate to readers in our introduction that, ‘prenatal testing is also a rapidly developing field and … is not addressed specifically in this paper’. We are pleased this issue has been highlighted and encourage GPs to make patients aware that carrier screening is available for serious conditions such as cystic fibrosis, spinal muscular atrophy and Fragile X syndrome, as well as haemoglobinopathies, so that they can make informed decisions about whether to proceed with these tests.
Associate Professor Grant Blashki,
Nossal Institute for Global Health
Professor Sylvia Metcalfe
Murdoch Childrens Research Institute and The University of Melbourne
Professor Jon Emery
Murdoch Childrens Research Institute
Spirometry screening
The article by Wisnivesky and colleagues,5 entitled ‘Spirometry screening for airway obstruction in asymptomatic smokers’ (AFP, July 2014), concludes that spirometry ‘may help detect a small number of patients with airway obstruction who are at high risk of COPD’. This is almost certainly true but the data in the paper do not actually demonstrate this. Airway obstruction was defined as ‘FEV1/FVC below the lower limit of normal (LLN): ie the fifth percentile of a healthy non-smoking population’.
Using this definition, 2.3% of the studied population had a low FEV1/FVC – rather fewer than the 5% one would expect in a healthy population using this definition of airway obstruction. As smoking exposures were only modest, this may also explain why there were no correlations with smoking history, symptoms etc, as it is likely that the individuals who failed the test were actually simply outliers of the normal population.
It would certainly be interesting to know what the actual values of FEV1/FVC ratio were in the nine allegedly abnormal subjects and whether these fell below the value of 0.7, which is widely accepted as defining airflow limitation, accepting the caveat that it may lead to some overdiagnosis in the elderly and underdiagnosis in younger patients.
Graham Simpson
Respiratory physician
Flecker House, Cairns, QLD
References
- Wisnivesky J, Skloot G, Rundle A, Revenson TA, Neugut A. Spirometry screening for airway obstruction in asymptomatic smokers. Aust Fam Physician 2014;43:463–67.
Anticoagulants
There is an important omission in the article, ‘Anticoagulation: a GP primer on the new oral anticoagulants’, by Brieger and Curnow6 (AFP May 2014). Although mentioned, almost in passing, in the paragraph ‘Management of bleeding’, the authors have not highlighted that as yet there are no direct ways to reverse the anticoagulant effects of these new oral agents.
Most patients on permanent anticoagulation have non-valvular atrial fibrillation. The majority are female, many with osteoporosis and an increased risk of falls. Fracture requiring surgical management is not a rare event, although surgery may not be urgent. What about trauma in a motor vehicle accident, or other acute surgical emergencies? A patient of mine developed acute appendicitis not long after commencing warfarin for paroxysmal atrial fibrillation and rapid emergency surgery revealed a leaking appendix. Of course, in this case the effect of warfarin was reversed with fresh frozen plasma, but things could have been very difficult if one of the new oral agents had been prescribed. Haematologist assistance, as suggested by Brieger and Curnow, is rarely available outside the major teaching hospitals.
Use of oral anticoagulants in atrial fibrillation was highlighted in a recent case study in the professional development program of the National Prescriber Service,7 and non-reversibility featured. Surely the lack of reversal of the newer oral agents must be taken into consideration when weighing up the risks and benefits of anticoagulation therapy in each patient. Patients should also be told of this disadvantage when discussing the options for anticoagulant therapy. Brieger and Curnow also failed to mention the current advice against use of the newer agents in patients over 75 years of age.
Dr Phillipa Gibian
Glenorie District Medical Centre, NSW
References
- Brieger D, Curnow J. Anticoagulation: a GP primer on the new oral anticoagulants. Aust Fam Physician 2014;43:254–59.
- NPS MedicineWise. Case study – Oral anticoagulants – exploring treatment options for stroke prevention. Sydney: NPS MedicineWise, 2014.
Reply
We would like to thank Dr Gibian for her comments on the lack of reversibility of the new oral anticoagulants. This is an important issue that does concern clinicians and we would urge all general practitioners prescribing anticoagulants to be sure they have ready access to services capable of dealing with bleeding events. These services should be capable of standard resuscitative measures, be familiar with strategies to reverse warfarin and accelerate removal of the newer anticoagulant drugs from the circulation, have access to appropriate intervention to contain the bleeding and the use of prohaemostatic agents if required. It is important to have effective communication with a local haematologist or consultant physician to aid in the management of these patients.
We wish to draw readers’ attention to the fact that despite the lack of a reversing agent, the available data suggest that the adverse consequences of bleeding in patients receiving a new orally active anticoagulant (NOAC) are no more frequent than in those receiving warfarin. In the RE-LY study, participants taking dabigatran had lower rates of bleeding if they required urgent or emergency surgery than those taking warfarin.8 Furthermore, in this trial the mortality of intracranial haemorrhage was not significantly different between participants assigned dabigatran or warfarin.9 In an independent evaluation of bleeding events from five phase III trials comparing dabigatran with warfarin, patients randomised to dabigatran who bled required more blood transfusions, but had a shorter stay in intensive care and a trend towards lower mortality than those who bled following randomisation to warfarin.10 This is despite access to vitamin K and clotting factors that could pharmacologically reverse the anticoagulant effect of warfarin and no specific antidote for dabigatran. A similar analysis of patients experiencing major bleeding in the ROCKET AF study showed no difference in transfusion rates or outcomes between patients receiving rivaroxaban or warfarin.11
Dr Gibian points out that oral anticoagulants are commonly indicated in elderly patients with non-valvular atrial fibrillation at increased risk of bleeding. It is certainly important to pay careful attention to appropriate dosing and to monitor for changes in renal function in these patients, and to recognise that few very elderly patients (>85 years) were enrolled in the randomised trials. These caveats notwithstanding, with regards to the factor Xa agents and the lower dose of dabigatran (110 mg bd) the randomised trial data have confirmed an acceptable12,13 or improved14 safety profile in the elderly when compared with warfarin. Patients over the age of 75 years with non-valvular atrial fibrillation should not be prescribed dabigatran 150 mg bd.
There are reassuring observations emerging from international post-marketing surveillance data, which confirm the randomised trial findings of efficacy and safety of these newer agents.15
A number of reversing agents have been developed, some with actions against multiple agents. One is in phase III clinical trial (dabigatran antidote) and two others are in phase II. Until they become available, however, we agree patients should be informed of the lack of an antidote when discussing the NOACs. Our recommendation is to conduct this in the context of a broader discussion that includes the observation that despite this limitation, the available evidence indicates that 1) major bleeding is not increased and 2) major adverse consequences of these bleeds are no more frequent in patients taking the NOACs than they are in patients taking warfarin.
David Brieger and Jennifer Curnow
Concord Hospital, Sydney, NSW
References
- Healey JS, Eikelboom J, Douketis J, et al. Periprocedural bleeding and thromboembolic events with dabigatran compared with warfarin: results from the Randomized Evaluation of Long-Term Anticoagulation Therapy (RE-LY) randomized trial. Circulation 2012;126:343–48.
- Hart RG, Diener HC, Yang S, et al. Intracranial hemorrhage in atrial fibrillation patients during anticoagulation with warfarin or dabigatran: the RE-LY trial. Stroke 2012;43:1511–17.
- Majeed A, Hwang HG, Connolly SJ, et al. Management and outcomes of major bleeding during treatment with dabigatran or warfarin. Circulation 2013;128:2325–32.
- Piccini JP, Garg J, Patel MR, et al. Management of major bleeding events in patients treated with rivaroxaban vs. warfarin: results from the ROCKET AF trial. Eur Heart J 2014;35:1873–80.
- Eikelboom JW, Wallentin L, Connolly SJ, et al. Risk of bleeding with 2 doses of dabigatran compared with warfarin in older and younger patients with atrial fibrillation: an analysis of the randomized evaluation of long-term anticoagulant therapy (RE-LY) trial. Circulation 2011;123:2363–72.
- Halperin JL, Hankey GJ, Wojdyla DM, et al. Efficacy and Safety of Rivaroxaban Compared with Warfarin among Elderly Patients with Nonvalvular Atrial Fibrillation in the ROCKET AF Trial. Circulation 2014;130:138–46.
- Halvorsen S, Atar D, Yang H, et al. Efficacy and safety of apixaban compared with warfarin according to age for stroke prevention in atrial fibrillation: observations from the ARISTOTLE trial. Eur Heart J 2014;35:1864–72.
- US Food and Drug Administration. FDA Drug Safety Communication: FDA study of Medicare patients finds risks lower for stroke and death but higher for gastrointestinal bleeding with Pradaxa (dabigatran) compared to warfarin. 2014. Available at www.fda.gov/Drugs/DrugSafety/ucm396470.htm [Accessed 15 July 2014].
Appropriate prescribing for viral conjunctivitis
Viral conjunctivitis is a common, highly contagious, usually self-limiting disease. Studies have identified adenoviruses as the most common causative organisms in two major classifications: epidemic keratoconjunctivitis (EKC), characterised by severe pain, pseudo-membranes, subconjunctival haemorrhage and corneal involvement causing vision changes and photophobia; and pharyngoconjunctival fever (PCF), characterised by fever, pharyngitis, pre-auricular lymphadenopathy, conjunctivitis and, less commonly, corneal involvement. Other key symptoms and signs for both types include conjunctival injection, follicles on eyelid eversion, watery discharge and lid oedema.16
Our current hospital clinical practice guidelines and the American Academy of Ophthalmology Preferred Practice Pattern Guidelines recommend conservative management with ocular lubricants and cold compresses.17 The concurrent use of antibiotics has little value and, in fact, may lead to allergy or ocular surface toxicity, which can complicate the clinical picture.18,19 Repeated use of topical antibiotics may also change the resistance pattern of normal ocular flora.20
A recent retrospective audit of 400 case notes of presumptive viral conjunctivitis attending the Royal Victorian Eye and Ear Hospital (RVEEH) emergency department between July 2010 and November 2010 found that 35% of cases represented probable PCF. There was a marked difference in prescribed treatments between RVEEH clinicians and community practitioners, with the majority of patients prescribed antibiotics within the community prior to presentation (Figure 1). Among patients who were prescribed antibiotics at RVEEH, almost 25% were a continuation of antibiotic drops commenced previously.
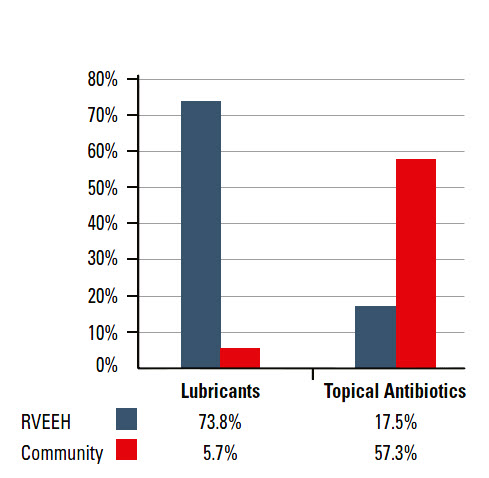 |
| Figure 1. Comparison of RVEEH and community treatments |
|---|
|
It is important for community health providers to recognise that our current recommendation for the management of viral conjunctivitis is the use of ocular lubricants. There is no indication for antibiotics unless there is a suspicion of another condition or a higher risk of bacterial infection (eg contact lens wearers or recent intraocular surgery, which must be referred for specialist care). It is also important to educate patients on the risk of transmission: infection precautions should be practiced for 2 weeks after the onset of symptoms, including meticulous hand hygiene.
However, a patient presenting with any alteration in their vision, photophobia, severe pain or non-resolving symptoms should be referred for specialist care as this may signify corneal involvement or pseudo-membranes, or the incorrect diagnosis (eg chlamydia conjunctivitis). In the case of corneal involvement, topical steroid drops are sometimes required under specialist care. In general, most patients can be treated symptomatically and will recover with no residual effects, but it is vital to be able to distinguish those who require specialist care and to limit the use of topical antibiotics for uncomplicated viral conjunctivitis.
Patricia Usher
Royal Victorian Eye and Ear Hospital
Jill Keefe
Department of Ophthalmology, The University of Melbourne, Centre for Eye Research Australia
Carmel Crock
Royal Victorian Eye and Ear Hospital
Elsie Chan
Royal Victorian Eye and Ear Hospital
References
- Alvarenga L, Scaarpi M, Mannis MJ. Viral Conjunctivitis. In: Krachmer JH, Mannis MJ, Holland EJ, editors. Cornea. 3rd edn. Philadelphia: Elsevier, 2011.
- American Academy of Ophthalmology Corneal/External Disease Panel. Preferred Practice Pattern Guidelines. Conjunctivitis – Limited Revision. San Francisco: AAO, 2011.
- Jefferis J, Perera R, Everitt H, et al. Acute infective conjunctivitis in primary care: who needs antibiotics? An individual patient data meta-analysis. Br J Gen Pract 2011;61:542–48.
- Dart J. Corneal toxicity: the epithelium and stroma in iatrogenic and factitious disease. Eye 2003;17:886–92.
- Milder E, Vander J, Shah C, Garg S. Changes in antibiotic resistance patterns of conjunctival flora due to repeated use of topical antibiotics after intravitreal injection. Ophthalomology 2012;119:1420–24.
Imaging for cardiac disease: a practical guide for general practitioners
I read with interest Dr Storey’s article ‘Imaging for cardiac disease: a practical guide for general practitioners’ (AFP May 2014).21 In the second introductory paragraph, he states that a ‘...myocardial perfusion study (MPS…) is widely used and available for assessing whether reversible or fixed myocardial ischaemic changes are present’. Ischaemia is reversible, by definition, and there is no such diagnosis of ‘fixed’ ischaemia. On MPS, ischaemia is detected as a perfusion defect on a post-stress (exercise or pharmacological) image that reverses (fully or partially) on the rest image. A fixed perfusion defect, on the post-stress and rest images, is a transmural infarction. A partially reversible defect at rest is usually due to a non-transmural infarction with peri-infarctional ischaemia.
A non-invasive MPS is unique, compared with all other cardiac imaging modalities. The imaging agent used, 2-methoxyisobutyl isonitrile labelled with technetium-99m, (sestamibi or MIBI), for MPS is strongly cationic and lipophilic and is largely sequestered in myocyte mitochondria.2 MPS images the myocyte directly, hence its uniqueness. MIBI extraction by the myocardium is directly proportional to myocardial blood flow.22
If there is significant coronary artery stenosis, the stress MPS depicts the lack of coronary flow reserve as a perfusion defect, decreased or absent (if severe), of myocyte uptake, which is not present at rest. Hence, MPS directly images ischaemia, the impairment of coronary artery flow reserve, due to haemodynamically significant stenotic coronary disease. No other cardiac imaging modality has this ability, making it still the best predictor of future cardiac events, compared with extensive other diagnostic studies.23
Electrocardiogram-gated single photon emission computed tomography MPS provides multiple functional cardiac parameters: three-dimensional segmental perfusion (severity and extent of ischaemia and the presence or absence of myocardial infarction), left ventricular ejection fraction, ventricular volumes (end-systolic and end-diastolic), regional wall contraction and thickening (all of these at rest and post-stress) and post-stress transient ischaemic ventricular dilatation (a bad prognostic sign). No other cardiac imaging modality can provide all of these data from a single study.
Computed tomography coronary angiography (CTCA) is relatively non-invasive.24 However, it is anatomical and does not identify which stenoses are haemodynamically significant in causing ischaemia. MPS is the only functional study that directly images ischaemia. CTCA does not obviate the need for invasive cardiac cathertisation, which is essential for determining the suitability of lesions for revascularisation, stenting or bypass graft surgery.
The author’s diagnostic algorithm is misleading for GPs with only one pathway to MPS. There should be a direct one, in patients with risk factors or suspicious symptoms, for GPs to refer for an MPS. It must be borne in mind that GPs cannot refer for CTCA and only cardiologists do stress echography.
Andrew McLaughlin,
Burwood Nuclear Medicine, NSW
References
- Storey P. Imaging for cardiac disease: a practical guide for general practitioners. Aust Fam Pysician 2014;43:260–63.
- Beller GA. Watson DD, Physiological basis of myocardial perfusion imaging with the technetium 99m agents. Semin Nucl Med 1991;21:173–81.
- Gimelli A, Rossi G, Landi P, et al. Stress/rest myocardial perfusion abnormalities by gated SPECT: Still the best predictor of cardiac events in stable ischemic heart disease. J Nucl Med 2009;50:546–53.
- Budoff MJ, Dowe D, Jollis JH, et al. Diagnostic performance of 64 multidetector row CT angiography for evaluation of coronary artery stenosis in individuals without known coronary disease: results from the prospective multicentre ACCURACY trial. J Am Coll Cardiol 2008;52:1724–32.
Reply
Thank you for the interest in this topic. I think there is no disagreement with the assertion that MPS and CTCA are complementary and I have been at pains to point this out.
CTCA is a relatively new imaging tool and its role is still evolving. It is unlikely that it will replace SPECT-MPS but there are newer applications of CTCA and also cardiac MRI, which assess wall perfusion, and these will be interesting technologies to follow.25 However, the real strength of the technology lies in its temporal advantage, in particular, the 12–20 second Triple Rule Out study, which has more of a role in the accident and emergency department.
The algorithm is of course a personal observation and discussion is always welcome.
Dr Peter Storey
Director of Imaging, Queensland X-Ray, St Vincent’s and St Andrew’s Hospitals
Toowoomba, QLD
References
- Wince WB, Suranyi P, Schoepf UJ. Contemporary cardiovascular imaging methods for the assessment of at-risk myocardium. J Am Heart Assoc 2013;3:e000473.
Problem gambling
Professor Thomas has produced an interesting article looking at problem gambling (AFP June 2014)26 but has missed a very important and easily treatable cause thereof, namely iatrogenically induced problem gambling.
It is now well accepted and irrefutable that dopamine agonists have the potential to evoke problem gambling, which is easily treated by suspension of the offending medication. Most recently, there has also been a suggestion that some antiepileptic medications may also provoke problem gambling, the mechanism being less clear but possibly also related to dopamine.
Professor Thomas has tactfully avoided any discussion of the possible pathophysiology of problem gambling but clearly, iatrogenically induced gambling has some connection to dopamine and further research in this area is required. Awareness of the potential for iatrogenically induced problem gambling is an imperative because it is by far the easiest mode of intervention if it is found to be present. It is very important that family physicians are aware of this potential so that it can be addressed if and when discovered.
Roy G Beran
Department of Medicine, University of NSW,
References
- Thomas S. Problem gambling. Aust Fam Physician 2014;43:362–64.
Reply
Thank you for the interesting comments from Dr Beran. The treatment of problem gambling using pharmacological agents is an intriguing possibility that reaches directly into the complex brain behaviour linkages.
The use of various pharmacological agents was systematically reviewed for the National Health and Medical Research Council gambling treatment guideline27 and it was concluded that, currently, there is insufficient research evidence to warrant positive recommendations for such treatments. Some research has been performed but it is very limited. Also, some case studies of the impact of using dopamine agonists for Parkinsonism (where the patients have developed gambling control problems) suggest that there are linkages.
However, at the present level of knowledge, pharmacological treatment of gambling would involve off-label use of agents for gambling treatment, drawing on agents with some demonstrated efficacy for substance and alcohol addictions. While pharmacological agents may manipulate and perhaps lower underlying enabling propensities such as impulsivity, my personal view is that problem gambling is a complex learned behaviour that has to be unlearned. So although some pharmacological agents may prove to facilitate this, their use would be as an adjunct to the primary psychological treatments.
Psychological treatments, including cognitive behaviour therapy and motivational interviewing, do have credible research evidence for their efficacy and thus should be the frontline treatments for problem gambling.
Shane Thomas
Monash University, Clayton, VIC
References
- Monash University Problem Gambling Research and Treatment Centre. NHMRC approved guideline for screening, assessment and treatment in problem and pathological gambling. Clayton: Monash University; 2011. Available at www.nhmrc.gov.au/_files_nhmrc/publications/attachments/ext0005_problem_gambling_guideline.pdf [Accessed 20 May 2014].
Flashes and floaters: a practical approach to assessment and management
We read with interest the recent article by Kawahita et al28 regarding the assessment and management of patients with flashes and floaters (AFP April 2014). This is a well-written piece providing practical guidelines for general practitioners regarding relatively common and important symptoms.
We do have some concerns, however, regarding the comments regarding the use of ultrasound. The authors claim that, especially for those in a rural setting, ultrasonography could be used ‘to determine the presence or absence of ocular pathology’. They seem to imply this can be used to substitute for an ophthalmic examination.
While ophthalmic ultrasound can be used to detect the presence of a retinal detachment, it is often difficult to detect peripheral retinal tears, even in experienced hands. It has been reported that the prevalence of retinal tear is up to 14% of patients with acute onset of flashes and floaters.29 Without prompt and adequate treatment, retinal tears can lead to rhegmatogenous retinal detachment and vision loss. The studies quoted did not assess the sensitivity of ultrasound for detecting retinal tears.
A small study from the United Kingdom showed that even an experienced retinal surgeon would miss more than one in 10 tears with 90D biomicroscopy alone if indented ophthalmoscopy were not done.30 A review of medico-legal litigation cases in the National Health Service showed that the majority of vitreoretinal negligence cases result from a delayed or missed diagnosis of retinal detachments and tears.31
We recommend all patients with acute onset of flashes and floaters, especially those with high-risk characteristics, be promptly referred for a dilated retinal examination to reduce the risk of vision loss.
Dr Neil Sharma
Dr Ju-Lee Ooi
Mr Jong Min Ong
Cambridge University Hospitals NHS Trust, UK
References
- Kahawita S, Simon S, Gilhotra J. Flashes and floaters: a practical approach to assessment and management Aust Fam Phys 2014;43:201–03.
- Hollands H, Johnson D, Brox A, et al. Acute-onset flashes and floaters: is the patient at risk for retinal detachment? JAMA 2009;302:2243–49.
- Natkunarajah M, Goldsmith C, Goble R. Diagnostic effectiveness of noncontact slitlamp examination in the identification of retinal tears. Eye 2003;17:607–09.
- Mathew RG, Ferguson V, Hingorani M. Clinical negligence in ophthalmology: fifteen years of national health service litigation authority data. Ophthalmology 2013;120:859–64.
Reply
We would like to thank Dr Sharma and colleagues for bringing up the issue of ultrasonography of the eye for retinal detachment in a rural setting. We agree that ultrasound is not a substitute for ophthalmic examination. Country general practitioners who are not comfortable with examining the eye may have easier access to a local optometrist, who may be able to help diagnose retinal detachment and facilitate referral. However, in a rural setting, where the nearest ophthalmologist may be several hours away, ultrasonography may be helpful in distinguishing retinal detachment from the other differential diagnoses mentioned in our article.32 Ultrasonography seems to be readily accessible in rural areas and it may aid diagnosis for those practitioners who are experienced in ultrasonography.
Indeed, ophthalmologists themselves use ultrasonography when the retina cannot be viewed (eg vitreous haemorrhage) to aid in assessment of masses or retinal detachment; however, this is not a replacement for an ophthalmic exam.
Shyalle Kahawita
The Royal Adelaide Hospital, SA
References
- Kahawita S, Simon S, Gilhotra J. Flashes and floaters: a practical approach to assessment and management Aust Fam Phys 2014;43:201–03.
Stroke
In the article ‘Stroke’ (AFP March 2014), Pollack et al33 provided some valuable data on encounters of cerebrovascular disease in general practice in Australia. Although the majority of strokes are managed acutely in hospital, general practitioners (GPs) need to be confident in assessing initial symptoms as well as managing the longer-term risk factors. Assessing neurological symptoms in general practice can be challenging, particularly given the time restraints during a busy day. Transient ischaemic attack (TIA) and stroke require urgent medical attention but there are many mimics, making diagnosis difficult.33–35 The clinical history and examination are significant parts of making any diagnosis, but a complete neurological examination may be overwhelming in general practice. There is limited evidence in Australia on how GPs assess and manage acute transient neurological events, but there is some literature to suggest that identification of patients with TIA or stroke could be improved.36–39 Pollack et al33 report that for every 100 cerebrovascular problems managed, 5.1 medical specialist referrals were made. Bekkelund et al40 evaluated referrals from general practice to a neurology department and found only 51% of referrals reported findings of a clinical examination; however, it may be that GPs are conducting neurological clinical examinations but not recording them in referral letters. There are variable referral pathways in Australia for patients with a suspected TIA and differing waiting times for general neurology clinics.41 The triage of patients includes consideration of clinical examination findings and omitting such on a referral letter may have an adverse effect.
A thorough examination assists in localising the area of brain affected and provides clues to the aetiology but such an examination may not be feasible in a standard general practice consultation. We have devised an approach to a cerebrovascular examination that can be performed in 5 minutes, to assist the GP in assessing a patient with a suspected TIA or stroke, in order to reach a diagnosis and determine the need for urgent referral. Some have suggested that general clinicians have a fear of clinical neurology, ‘neurophobia’,42 and our approach is designed to provide GPs with an efficient and structured approach. We propose a stroke prevention examination designated the SP Exam (Table 1).
Our 5-minute examination, which is demonstrated in a video (www.youtube.com/watch?v=BBJJ7-0XE6c), has provided our GP trainees with the confidence to perform an appropriately focused neurological examination.
Table 1. SP Exam – 5 minutes
|
Test
|
Status
|
|---|
| Alert |
Yes/No/Confused |
| Mental state |
Orientation: Time Place Person/ Where?/Why? |
| Speech |
Slurred = dysarthria Wrong words = dysphasia |
| Vitals |
HR bpm /Regular Y or N BP |
Face
Visual fields
Smile
Nystagmus
Extra-ocular movements
Mouth
Tongue extend |
Hemianopia
Y/N – L/R
Symmetrical Y/N
Y/N (Vertebro-basilar artery (VBA) = brainstem)
Horizontal only – diplopia/abnormal (brainstem)
‘Ah’ Y/N (brainstem)
midline/deviated
L/R(brainstem) |
Arms
Observe
Outstretched Arms
Finger to Nose
Tone
Reflexes
Sensation
Inattention |
Y/N (Ataxia = VBA)
Normal or increased
Biceps
Touch L/R
Y/N |
Legs
Observe
Walk into room
Lift up leg
Tone
Reflexes
Plantars
If unsteady walk – heel-to-shin
Sensation
Inattention |
Y/N
Y/N
Normal or increased
Knees
Up or down
Normal/ataxia (Ataxia = VBA)
Touch L/R
Y/N |
Elaine Leung
GP, Pasadena Medical Centre, PhD candidate University of Adelaide, SA
Cate Price
Sturt Fleurieu General Practice Education and Training (SFGPET)
GP, Flagstaff Hill, Adelaide, SA
M Anne Hamilton-Bruce
The Queen Elizabeth Hospital, and School of Medicine, University of Adelaide, SA
Prof Nigel Stocks
Discipline of General Practice, University of Adelaide, SA
Associate Prof Simon A Koblar, University of Adelaide and
The Queen Elizabeth Hospital Stroke Unit, SA
References
- Amort M, Fluri F, Schäfer J, et al. Transient ischemic attack versus transient ischemic attack mimics: frequency, clinical characteristics and outcome. Cerebrovasc Dis 203333;32:57–64.
- Castle J, Mlynash M, Lee K, et al. Agreement regarding diagnosis of transient ischemic attack fairly low among stroke-trained neurologists. Stroke 20330;433:33367–70.
- Kraaijeveld CL, van Gijn J, Schouten HJA, Staal A. Interobserver agreement for the diagnosis of transient ischemic attacks. Stroke 33984;335:723–25.
- Harbison J, Hossain O, Jenkinson D, Davis J, Louw SJ, Ford GA. Diagnostic accuracy of stroke referrals from primary care, emergency room physicians, and ambulance staff using the face arm speech test. Stroke 2003;34:733–76.
- Leung E, Hamilton-Bruce M, Price C, Koblar S. Transient ischaemic attack (TIA) knowledge in general practice: a cross-sectional study of Western Adelaide general practitioners. BMC Res Notes 20332;5:278.
- Middleton S, Sharpe D, Harris J, Corbett A, Lusby R, Ward J. Case scenarios to assess Australian general practitioners’ understanding of stroke diagnosis, management, and prevention. Stroke 2003;34:26833–87.
- Wright J, Harrison S, McGeorge M, et al. Improving the management and referral of patients with transient ischaemic attacks: a change strategy for a health community. Qual Saf Health Care 2006;335:9–332.
- Bekkelund SI, Albretsen C. Evaluation of referrals from general practice to a neurological department. Fam Pract 2002;339:297–99.
- Price CJ, Blacker DJ, Grimley RS, et al. National survey of management of transient ischaemic attack in Australia: take immediate action. Med J Aust 2009;33933:337–20.
- Ridsdale L, Doherty J, McCrone P, Seed P. A new GP with special interest headache service: observational study. Br J Gen Pract 2008;58:478–83.
Letters to the Editor
Letters to the Editor can be submitted via:
Email: afp@racgp.org.au
Mail: The Editor, Australian Family Physician
100 Wellington Parade East Melbourne VIC 3002 Australia