Although it is important to note that generalist medical practitioners also work in urban areas across a variety of disciplines,6 rural and regional medical practice has long been an area where generalism thrives and leads by example, supported by innovation bred through necessity and the pioneering spirit of many rural and regional practitioners. A rural generalist practitioner is often required to perform procedural tasks and work within a broader scope of practice than their urban general practitioner (GP) counterparts, and is also likely to work in more diverse settings (including hospitals, community and/or private practice).7 Such generalist practitioners provide essential, and sometimes the only, medical services for rural and remote communities. Yet the medical workforce remains poorly distributed, both geographically and vocationally (Figure 1).8 The rural medical workforce is ageing,9 and for medical graduates the trend has been towards subspecialty practice and training (Figure 2).8,10 So it is understandable that the decline in generalism is particularly worrying for rural and remote Australia where a shrinking generalist workforce will surely have negative consequences for access to high-quality healthcare.11
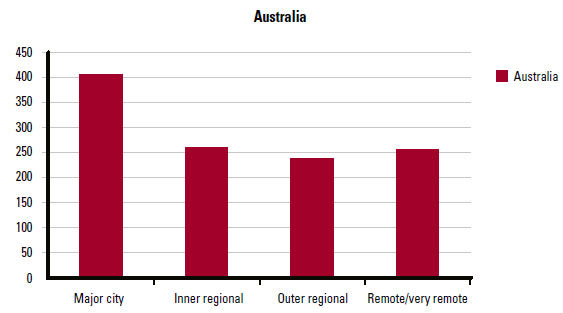
Figure 1. Full-time equivalent clinician medical practitioners per 100,000 population: remoteness area of main job 2011 (Based on Australian Institute of Health and Welfare material)8
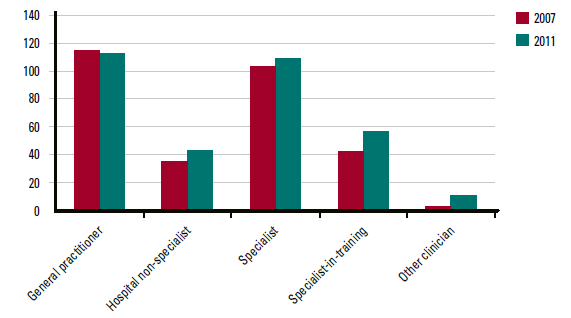
Figure 2. Full time equivalent employed medical practitioners per 100,000 population by field of practice (Based on Australian Institute of Health and Welfare material)8
In recognising the challenges facing generalism in medicine, government priorities and training programs have been slowly changing to ensure a sustainable generalist workforce can thrive once again, especially in rural and regional Australia. For example, there is widespread recognition of rural and regional practitioners as exemplar medical generalists and now a recognised training and career pathway in rural generalist medicine.12,13 Given the vital role of medical generalists in rural and remote areas, there is much more that could be done to support generalism, both in our medical education system and through broader health sector policy and health workforce initiatives.
What are the support needs for rural and regional medical generalist practitioners?
The following sections outline some support needs for rural and regional generalist medical practitioners under six headings, synthesised from current Australian and international academic literature and policy documents (Table 1).4,13–16 The issues will be presented, followed by some existing and proposed strategies for further supporting generalists in these same areas. A number of strategies, such as broader policy initiatives to increase the rural health workforce through bonded scholarships, restricted provider numbers and selection strategies, are beyond the scope of this article. Other articles in this series address other challenges and endeavours that will help to overcome some of the challenges associated with reinvigorating generalism.
Table 1. Support needs for rural and regional generalist practitioners
| Support needed | Description |
|---|
|
Workforce support
|
Locum relief and flexible support from regional specialist practitioners.
Consideration of innovative rural workforce models involving various health care providers.
|
|
Rural and regional training pipelines
|
Flexible rural and regional training pathways including flexible (including remote) supervision options to obviate need to leave rural community
|
|
Access to CPD (procedural)
|
All forms of CPD can be difficult to obtain in rural areas – procedural upskilling is particularly important for generalist practitioners.
|
|
Flexibility in practice ownership
|
Many young rural generalists plan to stay for 5–10 years in rural practice – still a significant contribution. Flexible walk-in, walk-out practice arrangements are vital.
|
|
Family support
|
Employment for spouse and senior schooling for children are two important areas in retention in rural areas
|
|
Recognition and remuneration
|
Increasing the status of generalist medicine in all its forms through undergraduate and postgraduate training is important in attracting doctors to generalist careers. Health financing reform to remove the perverse incentives for subspecialty practice is vital.
|
Workforce support
Workforce shortages in rural and regional areas mean that doctors in these areas tend to work long hours, frequently in solo or small practices, and at the extremes of their scope of practice. These stressors necessitate adequate holidays and support, yet one of the most commonly noted issues for rural doctors is the difficulty in getting locum support in a timely or affordable fashion to provide care for their patients while they are on leave.17 Throughout Australia, doctors are fortunate to have a number of rural and state-based medical workforce agencies that take a very active role in addressing these issues, through employing regular locums and encouraging city doctors to consider a regular arrangement of providing relief in a rural or regional area (eg. Queensland Country Relieving Doctors Program; Docs for the Bush; D4B, a range of others are summarised at www.rhwa.org.au/). In addition, Health Workforce Australia (HWA) and other agencies are undertaking considerable work exploring the potential of innovative alternative rural workforce models involving task substitution and/or delegated practice to alleviate workloads on rural medical practitioners.14
Professional isolation can also be a significant barrier to considering or maintaining a rural generalist role. Here, access to advice from specialist colleagues is a vital source of professional support for rural practitioners. Most urban-based doctors recognise this need and do their best to respond to requests in a timely fashion and some are proactive in setting up support networks (Telederm, www.acrrm.org.au, is a good example). The advent and increased popularity of telemedicine options are making it increasingly feasible for rural practitioners to receive a timely opinion on a worrying ECG, fracture or emergency presentation.18,19 Innovative applications of new communication technologies offer great potential for overcoming professional isolation for rural generalists; there is an unmet need for rigorous evaluation and wider implementation of these initiatives.
Rural and regional training pathways
The success of the so-called ‘rural-pipeline’ (spanning secondary school to undergraduate medical study through to vocational training) in increasing the number of medical students who pursue rural careers is now well established and will help to address imminent challenges that await an ageing generalist workforce.14–16,20 However, there are still many potential gaps in the pipeline that can cause problems for the workforce in rural and regional areas. For example, doctors working in remote or rural towns who want to undertake vocational training are often forced to leave their hometown for at least part of the training. Although this may be desirable in terms of developing a broad range of skills in different environments, it causes disruption for doctors and their family and leaves a rural community without their resident practitioner. Creative solutions to these issues involve flexible, often remote, models of supervision for some or all of the period of training. An example of this is the Remote Vocational Training Scheme (RVTS, www.rvts.org.au). Rural and regional areas are also extremely short of generalist physicians and surgeons. Initiatives such as the Northern Clinical Training Network (NCTN, www.nctn.net.au) link undergraduate training with junior doctor hospital training and specialist training in regional areas, thus avoiding the need for rural and regional junior doctors to move to cities for training programs at a time when they are likely to form relationships and not return.
Access to continuing professional development
All doctors are required to participate in continuing professional development (CPD), which is recognised as a vital component of good clinical governance and high-quality care. In metropolitan areas, such training is often provided through evening and weekend workshops but it is often impractical for rural doctors to attend these activities. Rural doctors have long requested more flexible and accessible CPD options, and many CPD offerings are now available in flexible online formats. The maintenance of high standards and quality knowledge and skill acquisition using these online formats is an ongoing challenge.21
Furthermore, for generalist practitioners, CPD in their procedural discipline of choice often remains problematic. Hands-on experience and refresher training is required to maintain skills; however, the progressive closure of rural operating theatres and delivery suites is severely limiting options for upskilling or skill maintenance.22 Closure of vital infrastructure can have a devastating effect on retaining desirable procedural skills in a rural community where regular practice/application is important for skill maintenance (eg. attending deliveries on a regular basis). Additionally, medical schools are increasingly relying on rural generalist practitioners as teachers in their teaching programs. A World Health Organization review of faculty support has highlighted the need for rural preceptors to receive adequate training and support in their teaching roles as well as clinical roles.23
Flexibility in practice ownership
There is increasing recognition that rural and remote professional practice is not always a lifetime vocation and that, in fact, many younger doctors can make a great contribution for 5 or 10 years in rural areas, before moving to a regional centre or similar (often for family reasons).24 The need to own or buy into a medical practice can be a considerable disincentive for such doctors, as the prospects of selling when moving on can be low. Rural councils and health services are demonstrating success through models whereby practice infrastructure is owned by the council and community, facilitating a walk-in, walk-out model for practitioners providing health services in particular communities. An example of this kind of support is the NSW Rural and Remote Medical Services (www.rarms.com.au/).
Family support
There can be a number of family-related challenges associated with working in a rural or remote area. Spouses can have difficulty finding satisfying work or interests in the community; long work hours can make work–life balance unachievable; families may feel isolated from friends and/or family; and appealing schooling options for children (especially secondary) may not be available locally.25 Family-related challenges to rural and remote practice are not new17 but we might consider novel strategies to address them. Many of the other strategies listed in this paper will certainly help with issues such as work-life balance, including greater availability of locum support and walk-in/walk-out practices. The Royal Australian College of Physicians (RACP) suggests that sensible, safe and family-friendly work hours and on-call duties will be helpful in attracting and retaining practitioners to rural areas, as would assistance with finding housing and spousal employment.26
Arrival housing and spousal employment are issues that may be addressed by, or in partnership with, local organisations such as local councils and Medicare Locals/Primary Health Networks, as Divisions of General Practice had done previously.27 In addition, local support networks such as the state-based Rural Medical Family Network (www.rmfn.org.au) provide much-appreciated support to rural families.
Recognition and remuneration of generalist work
Increasing the status of generalism at all stages of medical education and training is a priority for increasing its attractiveness as a career choice for junior doctors. Often, even in medical schools that pride themselves on a generalist-focused curriculum and extensive community and rural placements, this work is undermined by derogatory comments from a minority of vocal specialist practitioners.10 Persistent bias promoting specialist and subspecialist care throughout the media and other community forums, and within the medical professions, can have the same negative effects.28 A ‘culture change’ is required to ensure that generalism is afforded the recognition within the wider medical profession that it is due.4 Achieving this culture change is linked to greater recognition that will come through high-quality, accepted training pathways, and appropriate remuneration is likely to also be important.29 Generalist careers need to be promoted by and within the medical profession to junior doctors as careers of first choice for the best and brightest, supported by their exposure to inspirational and committed generalist preceptors.
The effects of government policies and programs must also be considered here. Persistent views of generalist careers as inferior choices, or as a ‘back-up’ option, are reinforced by the Medicare Benefits Schedule (MBS). The current MBS undervalues the vital work of generalist practitioners and offers perverse financial incentives for procedural specialty practice, encouraging over-servicing and workforce drift away from generalism. This ultimately has negative outcomes for accessibility and appropriateness of care for non-metropolitan Australians. In marked contrast to changes proposed in the 2014–15 budget, policy initiatives that reform relative MBS funding rebates towards generalism and develop additional funding streams for primary care are likely to be helpful, particularly in rural and regional areas where patients are more likely to attend just one practice.29
Conclusion
A generalist approach to healthcare can have many important benefits to the health of Australians through improving continuity and integration of healthcare, facilitating equitable access to services and encouraging a whole-person approach to care. Considerable progress has been made in Australia over the past decade in terms of recognising the importance of generalism in the medical workforce and initiatives to bolster and support the health workforce in rural and remote Australia. Despite this, the generalist medical workforce in rural and regional Australia still has a number of ongoing support needs. Federal and state governments, professional bodies, local organisations and educators must work together to address the policies, health system design, remuneration and training pathways that will support a vibrant and sustainable rural and regional medical workforce that is responsive to community needs.
Competing interests: None.
Provenance and peer review: Commissioned, externally peer reviewed.