Fatigue as a presenting symptom
Fatigue is ‘that state … characterised by a lessened capacity or motivation for work ... usually accompanied by a feeling of weariness, sleepiness, irritability or loss of ambition’.1 It is derived from the Latin fatigare, to tire. For the purposes of this review article, we regard fatigue as synonymous with tiredness and malaise.
Fatigue is a common reason for presentation in primary care. In the Australian general practice setting, fatigue presents at a rate of 1.4 per 100 encounters.2 This is similar to the findings from a large UK study (1.5%)3 but lower than rates of 5–7% reported in other international studies.4–6 Fatigue is the most common unexplained complaint presenting to general practitioners (GPs).7 Adult presentations of fatigue are positively associated with the patient being female4,8–14 and younger (mean age 34–39 years)8,9,11 and the GP being female.4
Causes of fatigue
Murtagh provides a helpful framework for understanding the aetiology by categorising the causes of fatigue into probability diagnoses, serious disorders not to be missed and pitfalls.15 Probability diagnoses include stress and anxiety, depression, viral/post-viral infection and sleep-related disorders. Serious disorders include malignancy, cardiac arrhythmias, cardiomyopathy, anaemia, bacterial infection, haemochromatosis, human immunodeficiency virus (HIV) infection and hepatitis C. Common pitfalls include coeliac disease, pregnancy, renal failure and metabolic disturbances. Medication-related side effects are another key consideration. There is a strong relationship between fatigue (especially if prolonged) and psychological disorders.11,16–18 Psychosocial causes of fatigue (eg. depression and anxiety) have been shown to be the most common non-somatic diagnoses made.8–10,19
The prevalence of formal diagnoses made in patients presenting with fatigue in primary care is not clearly established. Studies vary widely in methodology (definitions and inclusion criteria), making comparison difficult. In a recent Dutch cohort study of patients with fatigue, more than half had not received a diagnosis after 12 months follow up and only 8.2% were diagnosed with somatic pathology (eg. anaemia, thyroid disease, diabetes).19 Other studies have demonstrated significantly higher rates of organic disease of 25–50% of all patients.9,10,13 These discrepant findings are probably due to differing methods of classifying fatigue and somatic diagnoses. Thus, although fatigue may be related to a variety of medical and psychological causes, it often remains unexplained. It has been shown that for close to half (43%) of patients presenting to their GP with fatigue, the final diagnosis will be ‘tiredness’.5
Test ordering behaviour
There have been a number of described influences on the test ordering behaviour of doctors.20,21 These comprise doctor factors (eg. demographics, knowledge, prior experience, personality and fear of litigation), patient factors (eg. trust and anxiety), practice factors (eg. billing) and systems factors (eg. the rise of technology).
A Dutch study from 2002 investigated the test-ordering practices of GPs when faced with an ‘unexplained complaint’.22 They found that in the context of fatigue, the most common reasons for ‘superfluous’ testing was for patient reassurance and diagnostic uncertainty. However, a recent systematic review has shown that ordering tests for symptoms with a low pre-test probability of serious illness (as is the case with fatigue) does little to reassure patients or decrease their anxiety.23
Frequency of test ordering
A combination of potentially serious underlying diagnosis, a non-specific unexplained symptom and a previous lack of guidelines has led to high rates of test ordering in the investigation of fatigue. In 2011–12, pathology tests were ordered in 64.2% of patients with fatigue presenting to Australian GPs.2 This rate has increased considerably over the past decade.12 Similar rates have been found in other Australian studies14 and internationally.5,13 Moreover, tests for patients with fatigue were ordered at a rate higher than for any other problem managed. On average, 3.63 pathology tests were ordered per encounter (when tests were requested) by GPs.12 Associations of ordering tests at the first visit were older patient age and absence of comorbidity.14
Type of tests ordered
In Australian general practice, the most commonly ordered tests were full blood evaluation (FBE, 45.7%), thyroid function tests (TFT, 32.3%), ferritin (21.0%), liver function tests (LFT, 17.4%), electrolytes, urea and creatinine (EUC,15.5%) and blood sugar levels (BSL, 11.5%).24 This is broadly similar to findings from international studies.8,13
Yield of test ordering
In most cases, investigating patients with fatigue in the general practice setting does not result in a formal clinical diagnosis. An Australian study from 2003 found that only 16% of tests ordered returned abnormal results, leading to a ‘significant clinical diagnosis’ in only 4% of patients.14 Other studies have shown similar rates (5–9%) of identification of clinically significant disease by ordering tests.8,11,13,25
It has been shown that a limited set of blood tests (haemoglobin, erythrocyte sedimentation rate [ESR], BSL and thyroid stimulating hormone [TSH]) is almost as useful in diagnosing serious pathology as a more extensive set of investigations.7 Clearly, some of the potential causes of fatigue are serious and life-threatening conditions with potential for early diagnosis and treatment. However, excessive test ordering comes with significant potential costs, both financial and to patient safety.26 This is particularly the case with investigation momentum, or the cascade of unnecessary tests created by the further investigation of false-positive or clinically non-significant results.27
Existing international guidelines
A number of guidelines for the assessment and investigation of fatigue have been developed.28–32 Primarily, they emphasise the vital importance of a thorough clinical assessment, including a comprehensive history and examination, identification of red flags (Table 1) and a clear understanding of the epidemiology of disease in the practice population.
Table 1. Red flags that raise suspicion of serious underlying disease34
| Red flags | Examples of potential serious underlying disease |
|---|
| Recent onset of fatigue in a previously well older patient |
Malignancy
Anaemia
Cardiac arrhythmia
Renal failure
Diabetes mellitus |
| Unintentional weight loss |
Malignancy
HIV infection
Diabetes mellitus
Hyperthyroidism |
| Abnormal bleeding |
Anaemia
Gastrointestinal malignancy |
| Shortness of breath |
Anaemia
Heart failure
Cardiac arrhythmia
Chronic obstructive pulmonary disease |
| Unexplained lymphadenopathy |
Malignancy |
| Fever |
Serious infection
Hidden abscess
HIV infection |
| Recent onset or progression of cardiovascular, gastroenterological, neurological or rheumatological symptoms |
Autoimmune disease (eg. rheumatoid arthritis, systemic lupus erythematosus)
Malignancy
Arrhythmia
Coeliac disease
Parkinson’s disease
Multiple sclerosis
Haemochromatosis |
Many of these guidelines recommend an initial 4-week postponement of test ordering and subsequent restricted investigation. Delaying investigation has been shown not to affect patient satisfaction or anxiety levels.33 Recommended tests vary considerably from guideline to guideline and take into account duration of fatigue, patient age and presence of risk factors. UK guidelines recommend testing for coeliac disease in all patients in the initial battery of tests.28 A second line of testing is generally suggested if tiredness persists for 3 months.
Australian guidelines
In 2011, Australian guidelines for the investigation of fatigue were published (Figure 1).34 These guidelines cover conditions associated with fatigue, the demographics of their presentations and a diagnostic approach. As in previous international guidelines, the Australian guidelines recommend balancing the risks and benefits of testing, especially when the pre-test probability of disease is low. They also advocate a watchful-waiting approach in the absence of red flags. In particular, they recommend postponement of ordering any investigations when psychosocial causes seem to explain complaints of fatigue and when patients have an expectation of further investigation that is deemed inappropriate on the basis of the history and examination.
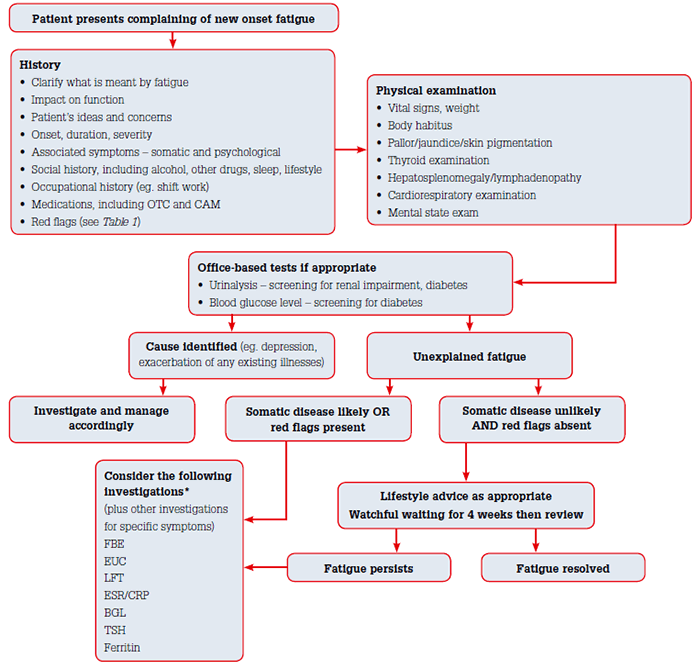
Figure 1. Australian guidelines for investigation of fatigue34
CAM, complementary and alternative medicines; FBE, full blood evaluation; BGL, blood glucose level; ESR/CRP, erythrocyte sedimentation rate/c-reactive protein; EUC, electrolytes, urea, creatinine; LFT, liver function tests; OTC, over-the-counter, TSH, thyroid stimulating hormone
In patients with unexplained or persisting fatigue, the guidelines recommend the judicious use of investigations with high sensitivity, including urine dipstick and finger-prick blood tests (eg. proteinuria, BSL) before more formal tests. If proceeding to formal investigations, they recommend FBE, venous fasting BSL, TSH, EUC, LFT and ESR or C-reactive protein (CRP). The critical importance of follow-up is also highlighted.
Conclusion
On the basis of the international literature on this challenging subject and consistent with the new Australian guidelines, we recommend the following practical approach to the patient presenting with fatigue: a comprehensive history and examination, consideration of a period of watchful waiting in the absence of red flags and the judicious use of tests once the decision to investigate is made.
Case 1
Milla is a previously well woman aged 29 years who presents with a 3-week history of being ‘tired all the time’. She is married with no children and works as a full-time registered nurse. She has no other symptoms to report and there are no red flags. She is not taking any regular medications or other drugs. There have not been any significant changes in her life that she can recall and she cannot explain why she feels so fatigued. Physical examination is unremarkable. Her mental state examination is essentially normal – she reports her mood as ‘tired’.
Given the low pre-test probability of serious illness and because there are no red flags on history, you do not order any investigations on this occasion. You discuss lifestyle changes with Milla and arrange for her to return for follow-up in 3–4 weeks.
Milla returns to see you, as recommended, with persisting fatigue, although with some improvement. On further discussion, Milla felt that her fatigue was probably related to her work schedule and she was going to try to arrange a change in the roster. She was happy not to have any investigations done. You advised her to return if her fatigue did not resolve.
Case 2
Greg, an accountant aged 63 years, presents complaining of reduced energy levels over the past few weeks. Greg has no significant past history and is not on any regular medications. He drinks 1–2 standard drinks 5 days a week and is a non-smoker. Further questioning is unremarkable. Physical examination demonstrates normal vital signs, normal cardiovascular examination and no organomegaly, but you think that Greg’s conjunctivae are a bit pale.
As Greg is suffering from a new onset of fatigue and is a previously well older patient (a red flag), you arrange for the following investigations: FBC, EUC, LFT, ferritin, TSH, CRP and fasting BGL. Greg’s blood tests showed iron deficiency anaemia but no other abnormalities were detected. Greg was referred for gastroscopy/colonoscopy. Multiple dysplastic bowel polyps were found and removed.
Competing Interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.