Management of skin infections
Direct management of skin infections needs to take into consideration the likely causative agent, degree of severity of the infection, the natural progression of the disease, treatment risks and side effects, as well as the acceptability, likelihood of compliance and follow-up requirements.
Common causes of skin infections
Generally, skin infections can be considered on the basis of the causative factors – bacterial, viral, fungal and parasitic – and managed accordingly.
Bacterial infections
The most common bacterial skin infections are caused by Staphylococcus aureus or Streptococcus pyogenes.3 Infections may present as boils, impetigo, folliculitis or cellulitis.
Viral infections
Whilst many viral infections have skin manifestations, such as exanthems associated with diseases including measles, parvovirus and roseola, there are also infections that can specifically cause skin disease. The highly infectious Molluscum contagiosum can lead to outbreaks among school-aged children. Other common viral infections include Herpes simplex virus, which causes vesicles, and papilloma virus, which causes cutaneous warts.
Fungal infections
Fungal infections tend to thrive in tropical regions. Tinea infections, in the form of ringworm or tinea pedis, are common. Seborrhoeic dermatitis may occur as a result of a fungal infection such as malassezia.
Parasitic infections
Of the parasites, scabies and lice are the most frequently seen causes of infection for children in remote communities. Cutaneous larva migrans from animal hookworms is less common but can also occur.
Table 1. Common causes of skin infections and their treatment
| Organism | Treatment | Frequency | Duration |
|---|
| Bacterial |
Staphylococcus aureus |
Flucloxacillin/dicloxacillin 12.5 mg/kg oral |
6 hourly |
5–10 days |
| Cephalexin 25 mg/kg oral |
12 hourly |
5–10 days |
| Streptococcus pyogenes |
Benzathine benzylpenicillin (by weight) intramuscular |
Stat |
|
| Phenoxymethylpenicillin 7.5–15 mg/kg oral |
6 hourly |
10 days |
| Viral |
Herpes simplex |
Chlorhexidine mouth wash 0.2% |
tds |
As required |
| Acyclovir 5% cream |
5x/day |
4 days |
| Acyclovir 10 mg/kg oral |
5x/day |
7 days |
| Fungal |
Tinea |
Terbinafine 1% cream |
Daily |
1 week |
| Miconazole 2% cream |
bd |
4 weeks |
| Terbinafine (by weight) oral |
Daily |
4 weeks |
Malassezia
(seborrhoeic dermatitis) |
Hydrocortisone 1% + clotrimazole 1% topical |
Daily or bd |
7 days |
| Parasite |
Scabies |
Permethrin 5% topical |
For 8 hours |
Repeat after 1 week |
| Lice |
Permethrin 1% topical |
For 20 minutes |
Repeat after 1 week |
| Treatment failure |
Ivermectin 200 µg/kg oral |
Stat |
Repeat as per guidelines |
Management of infections
Bacterial skin infections may be more severe than other types of infection, and more difficult to clear in remote Aboriginal and Torres Strait Islander communities. Typically, they require antibiotic treatment. The first-line treatment is often flucloxacillin on the presumption that the likely cause is S. aureus. However, this varies from region to region and it is worthwhile to have some feedback about laboratory samples to understand local prevalence. For example, a review of our laboratory samples in far north Queensland have shown a combination of streptococcal and staphylococcal organisms on swabs4 (unpublished laboratory data). Therefore, treatment targeting just one type of bacteria may not result in clearance of the infection.
Topical antibiotics, such as mupirocin 2% for mild bacterial infections, have a risk for development of resistance so should be used with caution.5 When prescribed, it is important that they are used as a complete course. Usually, the recommended course is 8 hourly for 7 days. It should not be dabbed on in either a single use or ad hoc approach as part of a dressing. In far north Queensland about 16% of staphylococcal infections are attributed to community-acquired methicillin-resistant S. aureus (MRSA), which may be another reason for failure to clear an infection.4 Furthermore, a child with multiple skin sores in numerous locations should receive oral or intramuscular antibiotics, not just topical treatment.3
Bacterial infections can also have a risk of significant complications so should be treated more aggressively to try to clear them. In communities with high rates of post-streptococcal glomerulonephritis (PSGN) it is important that any potential streptococcal skin infection is actively treated using penicillin (or an antibiotic such as cephalexin that will treat both streptococcal and staphylococcal skin infections). There is also increasing support for the hypothesis that skin disease is linked to the pathogenesis of rheumatic heart disease.6 Therefore, in children with bacterial skin sores in these settings, a complete assessment, including cardiac examination, blood pressure and urinalysis for proteinuria, should be considered. Antibiotics are generally well tolerated but do have a small risk of anaphylaxis, gastrointestinal side effects and rare side effects such as liver toxicity.
In remote settings, management of a boil using incision and drainage can be complex in young children. Medical practitioners may need to be comfortable and able to provide safe procedural sedation to give adequate treatment. Magnesium sulphate paste may be useful for bringing boils to the surface before formal intervention.
As always, treatment options should be discussed with the parent or guardian to help with acceptability and compliance with treatment. This will go a long way to determining the ability of the child and carer to comply with treatment. As a general rule it is very difficult to complete 6-hourly treatment for children, so twice daily cephalexin is a useful alternative to flucloxacillin.3 It is also more palatable. In the author’s experience, carers will often request benzathine benzylpenicillin as a single injection in preference to completing 6-hourly oral penicillin for 10 days.
Viral infections generally only need symptomatic treatment, although acyclovir may be used if commenced immediately for H. simplex infections. M. contagiosum will usually resolve spontaneously, or parents can be shown how to extract the core with squeezing.
Fungal infections may resolve with topical anti-fungal creams. These creams should be applied after drying the area thoroughly and typically must be continued for a period of 1–2 weeks after resolution of the infection. The choice of anti-fungal agent will depend on the local options available. If there is widespread infection affecting hair-bearing areas or unresponsive or recurrent, it is more appropriate to use oral medication instead of topical treatment.
Parasitic infections, such as scabies and lice, should be similarly managed, initially with topical treatment, but where there is extensive infection (for the patient or community) and compliance is considered difficult or there is recurrence or lack of response, oral ivermectin may be considered as an alternative.
Recurrence/persistence
After commencement of treatment patients should be requested to return if the condition is not improving within an expected time frame. It may be appropriate to have home visits and follow-up by the Aboriginal and Torres Strait Islander health workers, to review whether the infection has cleared. Recurrence or persistence can be a sign of non-compliance, treatment failure, incorrect diagnosis or re-infection.
Non-compliance
The degree of compliance with interventions should be investigated and, if necessary, improved by use of an alternative medication with a better profile. If appropriate, other supportive measures may be considered, such as provision of antibacterial soap to facilitate cleansing of the sores.
Treatment failure/incorrect diagnosis
For persistent infections it is essential to take swabs or scrapings as appropriate to confirm the diagnosis. A longer course of treatment may be required or, if a resistant strain is identified, treatment should be altered accordingly.
Re-infection
Where re-infection is a possibility it is important that all sources of infection are treated concomitantly. Consider perianal and nasal swabs to look for MRSA carriers They should receive a clearance regime with intranasal mupirocin ointment twice daily for 5 days followed by re-swabbing to confirm the infection has cleared.3
Isolation/risk of spread
Contacts should be considered, particularly for highly transmissible infections such as scabies or impetigo. All family and household contacts should be treated for scabies at the same time. Linen should be washed and dried or put away for a week to give a chance for mites to die.3 Any infected contacts should receive retreatment after 1 week to target any hatching eggs. Children should remain at home, away from play groups and school, until completion of the second course of treatment. Note that children with lice do not need to be kept away from school once the initial treatment has been given, but the school should be notified.
Weeping or open impetigo should be covered with a waterproof dressing as this should protect against spread; however, families are usually advised that children should remain at home until treatment has been implemented (at least 24 hours). Some guidelines will further recommend that the child remain at home until all weeping areas have dried up.7 Note that for M. contagiosum, it is generally considered impractical to isolate children to avoid spread. Some guidelines do recommend avoiding sharing towels or baths between siblings to reduce their risk of being infected.8
General interventions
Patient specific
Topical management can include clearing the crusts with soap and water. Careful personal hygiene and hand washing for all medical staff, patients and their relatives should be emphasised to minimise the risk of transmitting infections.
Community based
Overall standards of housing and accommodation contribute to spread of infections. Overcrowding increases the risk of exposure and makes clearance of the disease more difficult where re-infection is more likely to occur. Access to functioning washing machines can facilitate the availability of clean linen.
Community swimming pools have been linked to a decrease in skin infections,9 although they require construction, maintenance and supervision, which can limit their implementation in remote communities.10 Use of showering for children instead of shared bath facilities can reduce spread, especially in those too young to swim.
Efforts to try to reduce the significant social and economic impact of these highly prevalent conditions include specific single-disease targeting, such as the One Disease at a Time project tackling scabies in the Northern Territory. Community education and involvement are essential components in dealing with skin disease in the long term. Whilst it is possible to manage on a case-by-case basis, ultimately if the socioeconomic determinants of skin infection and spread are not dealt with, eradication is extremely difficult, whether in a rural or urban setting. These diseases are viewed as relatively benign and common but they place a significant burden on communities already stressed through socioeconomic disadvantage and, as such, deserve complete management at both a patient and community level.
Case study
A child presents with a spreading rash, low-grade fever and increasing irritability. The rash is extremely pruritic with marked excoriation noted. Otherwise the child seems generally well and cardiac examination, blood pressure and urinalysis are normal.
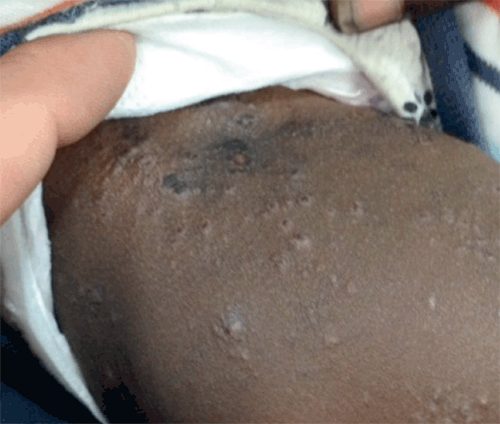
Figure 1. Rash in a child from a remote community
This child has scabies with a secondary bacterial component.
Management would include the following:
- Treat the impetigo
- As the disease is extensive disease, administer cephalexin, 25 mg/kg orally every 12 hours for 10 days.
- Topical care: advise the carer to soften the crusts with soap and water.
- Treat the scabies
- First wash, then dry off and ensure the skin is cool. Then apply permethrin 5% to the whole body from the neck down and wash off after 12–24 hours. Be careful to include body creases, fingernails and areas of impetigo but avoid direct application to open wounds.
- Supply sufficient quantity for a repeat dose after 1 week for any household members who are symptomatic.
- Manage contacts
- Minimise exposure of the patient to other children (eg. in school or play group) until 2 doses of treatment have been given.
- Treat all family and household contacts with a dose of permethrin even if they are asymptomatic. Ensure you supply sufficient quantity for all members of the household aged over 6 months, to be applied at the same time.
- Advise to hot wash or else put away all linen, clothes and towels for 1 week.
- Follow-up
- See the child again in 24–48 hours to ensure that the impetigo is improving. If not, consider a dose of benzathine benzlpenicillin injection.
- Advise the carer to return if symptoms have not resolved 2 weeks after completion of scabies treatment. Warn them that the itch can persist for up to 3 weeks and is not necessarily a sign of infection. There is no advantage in repeating doses of topical treatments. If the child is old enough and symptoms persist beyond 3 weeks consider treating the entire household with ivermectin.
- Advocate
- Use public health messages to promote personal hygiene, and early detection and treatment of skin infections.
- Take public health measures to improve housing, reduce overcrowding, provide access to safe public swimming pools and good water, and availability of sanitation measures.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.