Basal cell carcinoma (BCC) is the most common NMSC, but squamous cell carcinoma (SCC) is the more problematic as it is often more aggressive and has a propensity for local nodal and even distant spread. Most NMSCs are small and easily dealt with by surgery, radiotherapy or ablative techniques. Radiotherapy, as used for the case presented here, used to be the most common treatment modality for NMSC (eg. in Queensland); however, for early disease, radiotherapy has largely been replaced by general surgical or plastic surgical techniques. Despite this, the cure rate with radiotherapy is the same as that for surgery. For straightforward cutaneous sites, especially where primary closure is possible, surgery is often favoured as it is fast and simple, whereas radiotherapy usually involves many fractions of treatment over a period of weeks. Several important roles for radiotherapy in this disease remain, including: (1) radiotherapy alone (definitive radiotherapy) with curative intent, (2) radiotherapy alone with palliative intent (as described here) and (3) adjuvant radiotherapy after surgery. Definitive radiotherapy is often used for lesions in sites where the functional or cosmetic result is particularly important, including cancers of the lower lip, nose and periocular regions. Here, radiotherapy often achieves excellent function and cosmesis. Definitive radiotherapy can also be used for larger or more advanced lesions, often with a substantial chance of local cure. The indications for adjuvant radiotherapy include close or positive margins, large size, difficult sites (including lower lip, nose, ears and periocular regions) and perineural invasion.2
Case study
A man aged 75 years presented with a large, neglected, neoplastic-like ulcer on his left lateral posterior chest wall. The patient had difficult-to-control pain from the local lesion, despite narcotic analgesia. The lesion was highly malodourous and there was low-volume subcutaneous disease extending around onto the anterior chest wall (Figure 1A). The lesion was associated with ipsilateral arm lymphoedema and axillary lymphadenopathy (hard, matted lymph nodes were clinically tippable in the patient’s left axilla, but a full axillary examination was not possible, as the patient could not abduct his arm), but there was no clinical evidence of metastatic disease.
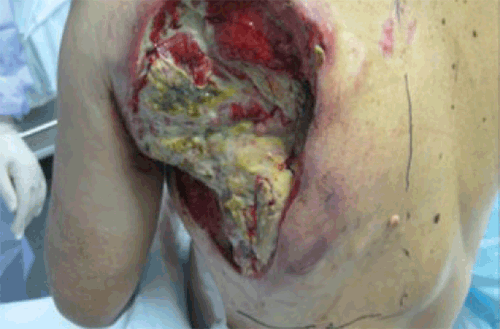
Figure 1A. Neoplastic-like ulcer
A biopsy from a non-necrotic edge of the mass showed moderately differentiated squamous cell carcinoma (SCC) consistent with origin in the skin. Given that it had been developing over many months, its pathology and the likelihood that it was locally advanced rather than metastatic disease, no further investigations were performed. The patient was referred for consideration of radiotherapy in an attempt to palliate his pain and improve the malodour.
Figure 1B shows radiotherapy treatment simulation (ie. computed tomography (CT) scanning in the treatment position). The patient was unable to lie on his back because of pain from the tumour, so he was simulated for radiotherapy in the less reproducible (compared with supine or prone) left lateral position. A CT planning axial slice through the lesion, in the mid-thorax, is shown in Figure 1C. The lines show the doses of radiation to be delivered in this position. The radiotherapy was a balance between not exceeding radiation tolerance of normal tissues (mainly the left lung) and tumour coverage: treating the entire lesion was not possible with a simple approach within the radiation tolerance of the lungs. Hence, the great bulk of the tumour, part of the axilla and the large ulcerated component were covered with the full radiation dose (straight line through the lungs is the medial edge, Figure 1C). If the treatment was with radical intent, intensity-moduated radiotherapy (IMRT) could potentially be used to cover the entire tumour, but given its complexity and need for excellent immobilisation IMRT was contraindicated here. Keeping the treatment simple was important as the patient’s positioning was not highly reproducible and the aim of therapy was symptom palliation. The thickness of the lesion can also be appreciated from Figure 1C (see asterisk). The radiotherapy dose comprised five treatments (fractions) of 6 Gy given once weekly over 5 weeks (30 Gy total).
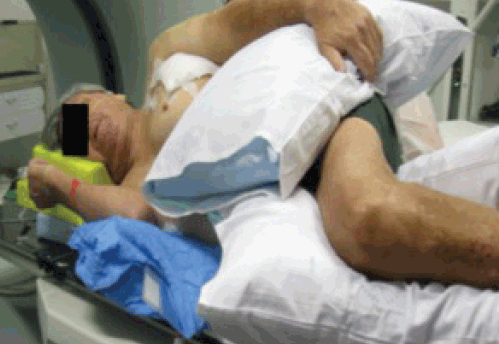
Figure 1B. Radiotherapy treatment simulation
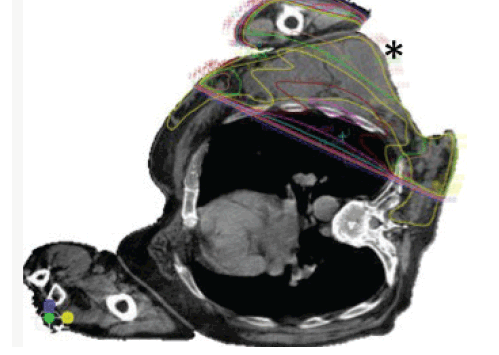
Figure 1C. CT planning axial slice
Figure 1D shows the appearance of the lesion 6 weeks after the last dose of irradiation. There was significant regression of the lesion, with complete relief of pain and a large reduction in malodour; the base of the ulcer appeared mainly to comprise granulation tissue. Pleasingly, there was also a complete response of the patient’s left arm lymphoedema, presumably due to radiation-induced regression of the treated left axillary nodes. It was conceivable that further regression may have occurred with time. This was the last time the patient was followed up and at this last review he now appeared cachectic, with many kilograms of weight loss. This is common when a patient has a significant total body tumour burden. Since this lesion had largely regressed, the cachexia was possibly but not certainly associated with metastatic disease from the lesion. No further investigations were performed.
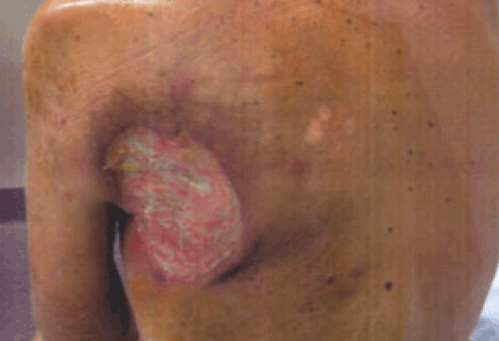
Figure 1D. Post-irradiation appearance of lesionFigure
These findings illustrate that, at times, tumour regression after radiotherapy can be quite slow. It also shows that radiotherapy can give excellent palliation of advanced SCCs, using simple treatment approaches that do not interfere substantially with the patient’s quality of life.
Discussion
An advanced case such as the one presented here is, fortunately, a very uncommon situation. However, it shows that radiotherapy can be a useful modality to consider in the palliation of advanced tumour masses. Large cancers of different histology and locations can also respond gratifyingly to radiotherapy.
Following oncological principles (viz, candidate lesions may be benign or malignant, primary or secondary), it was possible that this lesion was secondary to an SCC originating at an internal site. This was felt unlikely because the patient had no symptoms or signs other than those related to this tumour, skin metastases are typically multiple and the tumour grew over many months from a small skin lesion. The distinction here was largely academic as the lesion itself required attention because it was causing significant symptoms. For these reasons, a screen for other secondary or primary cancers was not performed.
At presentation, hard, matted lymph nodes were clinically tippable in the patient’s left axilla, but a full axillary examination was not possible as the patient could not abduct his arm. However, he had almost a full range of movement and no lymphoedema after tumour regression, presumably because tumour obstruction of the nodes had been relieved.
Regarding the role for other anticancer modalities in this situation, the tumour was clearly inoperable given its large size and invasion of adjacent tissues. However, surgery could be considered for debridement of slough to reduce malodour. Similarly, broad-spectrum antibiotic powders or creams, especially those active against anaerobic bacteria (eg. metronidazole) may be helpful.
Anticancer drugs are rarely indicated for NMSC as the vast majority are small and usually dealt with easily by surgery, radiotherapy or ablative techniques. For advanced lesions such as that described here, chemotherapy regimens are usually platinum-based and hence the patient needs to be relatively fit to tolerate them. Alternatively, oral methotrexate can be considered as it has lower toxicity, although response rates are lower.
A role for the newer targeted drugs in NMSC is yet to be defined. However, drugs such as cetuximab show excellent efficacy when delivered with other modalities for internal SCCs, such as advanced head and neck cancer, where they improve both local control and survival when combined with radical radiotherapy.3
It is concluded that radiotherapy can be a useful modality for advanced NMSC.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.