For the success of community placements, it is important to understand the factors involved in students’ perspectives of placements. It may be that immersion in a longitudinal integrated clerkship (LIC) overcomes the problem of unfamiliarity and allows stronger interpersonal relationships to develop with patients and members of healthcare teams.4 Australian authors report that a high proportion of students who spent a year working in rural and remote communities demonstrated positive attitudes to returning to work in similar locations after graduation.6 These students were closely involved in their preceptors’ management of patients and developed a deep understanding of the demands of the communities in which they were placed. Thus, it is possible that a sense of integration into the healthcare team, and the community the team serves, may be pivotal to the success or otherwise of community clinical placements.
Students of the Graduate School of Medicine (GSM) at the University of Wollongong (UOW) undertake an immersive experience of community-based care during a one-year Phase 3 LIC as part of the four-year graduate-entry medical (MBBS) course.7 This component of the course is pivotal to the school’s mission of training doctors prepared to practise in regional and rural Australia. Developing an understanding of factors influencing the success or otherwise of the LIC is therefore very important to the core purpose of the GSM, and of significance to efforts to increase rural workforce participation by other medical schools nationally and internationally. This qualitative project sought to gain an understanding of GSM students’ experience and learning during their LIC, from the perspective of integration or belonging in the general practice healthcare team in which they worked and in the community in which they were placed (regional or rural/remote). Adult Learning Theory (ALT) has played an important part in the development of the GSM curriculum. ALT assumes that adults are independent and self-directed learners, more interested in immediate, problem-centred approaches than subject-centred ones, and more motivated by internal than external drives.8 Thus, the findings were compared with the assumptions of ALT with a view to identifying areas for improvement in the LIC.
Methods
A semi-structured interview guide was developed by consensus of the research team. The guide was designed to provide prompts to cover aspects of the students’ experience across their medical placement, community contexts and their relationships with preceptors, staff, patients, community members, other students and the GSM. Ethics approval was obtained from the Human Research Ethics Committee of UOW (HE11/005). Phase 3 students in two successive cohorts were then invited by email for interview. The first wave of invitations occurred during March 2011 (9 months into their clerkship) and the second wave during November 2011 (5 months into their clerkship). The students were offered either face-to-face or telephone semi-structured interviews. The interviews lasted for 20–40 minutes each, were recorded and transcribed verbatim. The students were offered the opportunity to review their transcripts, but only one did so. The interviewer was a research team member (PJK-B) who, whilst employed by the GSM, did not have any direct connection with the students. The identity of the students was not revealed to team members who had academic roles that might influence students’ responses.
A template approach to analysis9 was undertaken by the principal researchers (GA and AB), with the LIC general practice environment as the context of interest,7 using ALT as an underlying theoretical framework.10–12 NVivo 9 was used to organise data by one researcher (AB) and manual coding used by the other (GA). By repeated readings and analysis of the text, codes were independently developed. These codes were compared at regular meetings and consensus reached on a coding template in an iterative process. Coded text was grouped into categories and abstracted into themes. Conceptual links between the themes were hypothesised. Other team members (PJK-B and JNH) reviewed the data, codes and interpretations. The principal researchers (GA and AB) determined that data saturation was reached after the ninth interview.
Results
A total of 13 students agreed to participate, nine from the initial round of invitations and four from the second round. The gender of the participants and the geographical designation of their practice placements are shown in Table 1. Three themes were derived as a result of the analyses: academic leadership; external (general practice) environment; and intrinsic (student) factors. Each theme was constructed from a number of sub-themes, described below.
Table 1. Gender of participants and LIC remoteness area classification
| Student | Gender | LIC remoteness area |
|---|
| 1 |
M |
RA2 |
| 2 |
F |
RA2 |
| 3 |
M |
RA1 |
| 4 |
F |
RA1 |
| 5 |
F |
RA3 |
| 6 |
M |
RA3 |
| 7 |
F |
RA3 |
| 8 |
F |
RA3 |
| 9 |
F |
RA2 |
| 10 |
M |
RA1 |
| 11 |
F |
RA1 |
| 12 |
F |
RA1 |
| 13 |
M |
RA3 |
| RA1: major cities of Australia; RA2: inner regional Australia; RA3: outer regional Australia |
Theme 1: academic leadership
Students were hosted in a general practice for 2 days and a local hospital for 2 days every week over the academic year of their clerkship. Curriculum content was chiefly covered by the weekly case-based learning (CBL) tutorials, supported by locally developed teaching. These learning materials provided a background to the students' experiential learning in their practices and hospital placements. The structure of the practice-based learning experiences was driven by each practice, preceptor and individual student. In this context, the students’ perceptions of academic leadership played a significant part in their experience of the clerkship.
The medical school
The students’ sense of ongoing leadership by the medical school whilst at a distant learning site was important, having a considerable impact, both positive and negative, on students’ experiences.
‘It’s been great having the rural Academic Coordinator to facilitate stuff from the mother ship, from back at the (medical school)… having all this stuff online is really, really handy and helpful’ (Student 9).
‘…lack of actually structured teaching from the university … I think that’s been really the only negative of the whole time out here’ (Student 8).
‘We don’t end up having that much contact with the university except for doing the CBLs… you kind of lose the university identity a bit’ (Student 6).
The general practitioner preceptor
The extent to which general practitioner (GP) preceptors actively engaged in the learning plans of the students was found to be a pivotal aspect of the students’ perception of their placement. The primary role of the GP preceptors was to facilitate parallel consulting with the student, to provide them with clinical exposure.7 However, over and above this, the students appreciated the GPs providing educational direction and expressed a sense of disorientation if their expectations of academic leadership were not met.
‘I’ve had a really good preceptor and GP and she’s a very, very keen and committed teacher and that’s been fantastic’ (Student 4).
‘But they, in phase three, I’ve found they make a really concerted effort…to say you know, “What is it that you think you’re missing”, and then they plan things and they come up with resources and … structured tutes to sort of fill that’ (Student 2).
‘But I mean I have my own room and stuff …so I guess I felt welcomed but there wasn’t a set structure or an expectation and that’s never ever been really clearly set up, it’s only been, “What do you feel you need to know”, or, “What can we do to help you’ (Student 3).
‘I think you just sort of feel your way through it for a long time; because there’s a lack of time they (the GPs) don’t necessarily have time to just sit down and say, “Oh these are things you could have done better”, or whatever. You just sort of work it out yourself in some ways’ (Student 1).
Theme 2: external (general practice) environment
Several features of the general practice learning environment were found to rank highly in students’ associations with the effectiveness and enjoyment of the placement. These included the geographical location of the practice, the organisational processes that provided structure for their activities and the team environment.
Practice location
Generally, the responses reflected a difference between students’ experiences in remote and rural placements, compared with regional locations. More close-knit communities seemed to promote a greater sense of belonging and a more rewarding experience for students.
‘I think the nicest thing probably about the community is that I do have to see some of my patients down the street… I like the continuity. I’ve seen a number of patients now in ED (Emergency Department) that have been from my practice and I’ll be doing a rotation in ED and then I’ll be able to follow them…’ (Student 11).
‘I’ve just been so grateful that I can study something that I’m really passionate about and have a great life experience at the same time; that’s awesome. I’m very grateful for that’ (Student 8).
‘…being a regional student rather than rural … I think that because we’ve been a little bit less necessary or relied on we haven’t had the opportunity to get as much exposure or to be as involved as perhaps students in rural areas who would have been really integral to the team because they needed more hands and more people’ (Student 4).
Practice organisation
The sense of organisation in the GP practice made an important difference, signalling a sense of welcoming and belonging.
‘…they had little signs on the front counter and even had like – they’ve got a little TV screen … had a little thing welcoming us on there … from day one they had all that arranged’ (Student 1).
Alternatively:
‘I was unhappy in there because I was paralleling with four different doctors, it was disorganised’ (Student 13).
General practice team environment
Feeling part of the practice team was a central theme of responses, frequently central to whether students felt they gained an integrated educational experience. Students wanted to feel they were making a difference in a practice.
‘…by about a third to a half of the way through I knew what she (the GP preceptor) wanted and I knew how to get things done and I was able to be much, much more organised and prepared for her …. I think that I then enabled her to speed up rather than slowing her down’ (Student 4).
‘How do you fit in with the dynamics…?’
‘Oh really well, particularly being a long-term student. I felt like one of the team – definitely’ (Student 8 ).
‘…they’ve really included me in everything. They’ve tried to get me in for meetings and teach me a little bit about the running of the practice, given me exposure to the people in the practice who do allied health and nursing and had me following them for a day or a half day or whatever so that I would understand more about what they do and how that all fits’ (Student 4).
However, not all of the comments reflected these positive themes:
‘…they haven’t kind of brought me in and I haven’t really felt like a working member at the practice’ (Student 13).
Theme 3: intrinsic (student) factors
A large component of the perceived success of the placement arose from factors intrinsic to the student: their learning style, degree of community engagement and future career plans.
Learning style
The students’ learning style, in particular their degree of comfort with self-directed learning, was associated with quite marked differences in their responses.
‘Like I’ve learnt a lot more from that than I do from sitting at home and studying and now all these opportunities where they’re all just happy to have you. If you say … “Can I come and do something” they’re all really willing to do that’ (Student 2).
‘… I think you’ve got to be prepared to self-direct your learning a little bit and I prefer it that way as opposed to someone saying “Read this chapter in a text book” so yeah, I think it’s good. I think we already had the couple of years of lecturing and stuff like that – I didn’t think it was necessary to really have more; you do have to be prepared to look stuff up yourself and direct your own learning and you just have to go “Look, what do I need to know next year when I’m doing my internship and what’s the level of stuff I need to know”’ (Student 6).
‘I appreciate the concept of self-directed learning but if you don’t, if the parameters haven’t been laid … I have no idea if what I’ve been exposed to has adequately prepared me for that’ (Student 3).
Community engagement
An increased level of engagement in the community by the students was generally associated with a more positive response overall to the clerkship.
‘I played soccer back home so I joined the soccer club and met a bunch of people through that, I joined the local gym and have met various people through that and play squash and tennis, I’ve been out to the archery club as well and met some people there. I’m currently playing on one of the local cricket teams and met various people through that. I’ve been to local ‘trivias’, I’ve been to a local ball – a dance that’s been held…’ (Student 13).
‘It’s tight-knit; I feel I have a lot more integration with the community here than in (regional centre) … which I think is just because we’re outsiders here – we’re new here – so we’ve been pushed or we’ve pushed ourselves to become part of the community’ (Student 7).
‘I commute to and from my practice; I commute to and from my university day; you basically it’s in and out. Whereas I feel like if I was in one of those smaller communities they’re just, they’re small so you’re going to run into everyone...’ (Student 3).
Future career plans
For some students, the clerkship reaffirmed previous career decisions. For others, it provided a stimulus for reassessing their goals, influenced by strengths (or their absence) across facilitating factors.
‘…if anything, it’s kind of reinforced my interest in rural health – it hasn’t at all turned me off rural health. I’d say it’s just cemented my desire to work in a regional area’ (Student 7).
‘I wasn’t that interested in GP – actually I didn’t really know what I wanted to do, I was kind of a little bit undecided, but now I know that I definitely like primary care so it’s got to be ED, GP or I actually really want to work for the RFDS’ (Student 6 ).
Interviewer ‘Has the community placement had any impact on that future career plan or not?’
‘…Yes it has. It’s made me realise that I probably don’t want to be a GP’.
Interviewer: ‘And how soon did that realisation hit you?’
‘Pretty soon....’ (Student 12)
Discussion
From the perspective of the general practice placement, the findings suggest that there is a complex interaction of factors resulting in a positive or negative experience of the LIC. Optimally, a synergistic relationship between factors resulted in a sense of belonging, which created a rich learning environment for students and motivation to return to a non-metropolitan community for clinical practice. No single factor or player stood alone; rather the quality of the interactions between the GSM, the practice, the community, GP preceptor and student were involved in the individual response. Figure 1 presents a conceptual model of the interactions resulting in a sense of belonging for students.
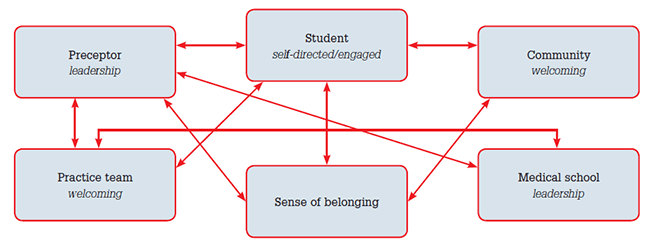
Figure1. Interactions between identified factors resulting in a sense of belonging
Our findings are supported by previous discussion in the literature of the potential strengths3, 4,7,13–15 and challenges4, 5,13,15 of community, particularly rural, LICs. This study provides a number of insights that to our knowledge are unique. First, it has allowed the experience of students undertaking LICs in major Australian regional and rural areas to be compared. Second, analysis from the perspective of ‘belonging’ offers a lens by which students’ experiences can be interpreted, and provides a useful conceptual model. In addition, our findings illustrate some of the tensions regarding the application of ALT in medical education.16,17 Most of the students in this study expressed features of the adult learner as described by Knowles,11 such as self-direction and a readiness to learn driven by changing social roles. However, as Knowles conceded, adult learners come with different life trajectories and learning preferences.11 As not all adult-aged learners will respond similarly,11,16 external motivators, such as the need to pass exams, are also valid and necessary.17 In response to this recognition, a number of authors recommend involving the learner and clinical supervisor in individualised contextualising of the learner’s needs to the clinical tasks at hand.8,12 The conceptual model arising from this study provides a map for strengthening the academic leadership provided at all levels (GSM, Regional Academic Hub and preceptor) to facilitate such student-centred, outcome-oriented learning to complement the ALT foundations of the curriculum.
GSM strategies, applicable to other schools, include facilitation of formal educational training and qualifications for preceptors and delivery of interactive live educational web-casts for students in regional and rural hubs.
These findings should be interpreted in light of the limitations and context of the study. Three of the authors (AB, GA and JNH) are generalist academic clinicians; JNH was actively involved in the development of the GSM curriculum. PJK-B is an academic with a health promotion background. Their professional perspectives need to be borne in mind when considering the analyses. The sample size in this study was comparable to other similar published qualitative studies.18,19 However, the sample size was modest and, when coupled with the nature of the recruitment, the potential for responder bias should be considered. Analysis from the perspective of the hospital component of the LIC was outside of the scope of this study and its possible influence on students’ perceptions should also be borne in mind.
Our findings support the concept of a dynamic interaction among factors determining the experience of students in the general practice component of the GSM LIC. It is hoped the findings will also be of value to other medical schools and their GP preceptors involved in similar community-based programs. The role of academic leadership in facilitating geographically distributed medical curricula warrants further research.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.
Acknowledgements
The authors would like to thank the students who gave their time to participate in this study