Professional bodies have advocated for change to support and enhance generalist practice.2,3 The Australian Medical Association has called for ‘further work to quantify and predict generalist workforce requirements and distribution as a matter of urgency’.3 A review of Australian Government health workforce programs4 also stated ‘…increasing the number of GPs and generalists needs to be a key priority in workforce planning and future funding for vocational medical training’. A recent Health Workforce Australia (HWA) analysis of demand for doctors and scenario modelling predicted an overall shortage of 2700 by 2025.5 However, existing definitions related to generalism, pragmatic issues with workforce planning approaches and transformational issues in the generalist practice setting have limited the usefulness of generalism workforce planning.
Generalism definitional issues
Throughout the literature and policy documents, various terms, including generalism, medical generalism, generalist practice, general practice, general practitioners, are used synonymously. However, the terms are not synonymous and require definitional clarity for workforce planners. Generalism has been defined in different ways (Table 1). A literature review of ‘what is the place of generalism in the 2020 primary care team?’ led to the development of a conceptual model of generalism comprising three essential dimensions (ways of being; ways of knowing and ways of doing). When combined, these dimensions form a philosophy of practice.6 The UK independent commission into medical generalism by the Royal College of General Practitioners stated that generalism was an approach to the delivery of healthcare – a way of thinking, acting and looking at the world.2 The UK commission further emphasised that it was possible to be a generalist in any specialty or profession and equally possible to work as a GP without being a ‘true generalist’. Definitions of generalist practice are based on professional expert opinion or consensus statements that describe the breadth of general practice and not the distinct expertise that distinguishes generalist care from other models of care.7 An evidence-based model of generalist care has been advocated for use by policy makers and planners to support service redesign.7 The distinct and defining expertise of the generalist was defined by the principle of person-centred decision making and is underpinned by the practice of interpretative medicine in a dynamic exploration and interpretation of individual experience.7 Any attempt to quantify and predict generalist workforce requirements needs to be based on the distinct expertise that generalist approaches offer.
Table 1. Definitions of generalism and generalist practice
| Generalism | Generalist practice |
|---|
- A philosophy of practice – a way of being, of knowing and a way of doing6
- An approach to the delivery of healthcare – a way of thinking, acting and way of looking at the world2
|
- The principle of person-centred decision making, underpinned by the practice of interpretative medicine in a dynamic exploration and interpretation of individual experience7
|
Workforce planning pragmatic issues
Workforce planning is conducted in a formulaic, mantra-type manner – predicting the right people with the right skills in the right place at the right time for the right cost. International reviews of approaches to workforce planning have concluded that no one was doing this well and that successful planning required accurate data, modelling, continuous and iterative planning, workforce planning skills, scenario building and input from stakeholders.8 The UK Centre for Workforce Intelligence is focusing on integrating workforce planning, education, training and development, and has developed a workforce planning framework that incorporates horizon scanning with big picture challenges that will impact on the health and social care system.9 In Australia, it is recognised that workforce planners face considerable challenges, including demand and supply factors, lead time for education, and gaps and inconsistent data and terminology.10 Workforce planning approaches are seen as too simplistic – typically they use accepted ratios of health workforce to populations, expert opinion or expressed demand service use and waiting lists.10 Alternative workforce planning approaches have been suggested, such as evidence-driven, needs-based, community-based health workforce models.11 A recent Australian research collaboration review12 of workforce planning approaches also provided the following suggestions:
- use forecasts of government healthcare expenditures to model national demand for healthcare
- examine drivers of demand and supply to assist with predictions of the effects of changes in key drivers
- modelling of the determinants of healthcare demand and utilisation
- modelling of the determinants of recruitment, retention, mobility, hours worked, productivity and quality of care provided by the health workforce.
Health Workforce Australia (HWA), Australia’s first health workforce planning agency, provided the opportunity for evidence-based and appropriate workforce planning. HWA’s analysis of demand for doctors and scenario modelling predicted a shortage of 2700 by 2005.5 However, the HWA report stated a key limitation in the projected demand, namely, ‘limitations arise in projecting demand due to the unknown impacts of external factors such as changes in technology, new skills, roles or service delivery models.5 These limitations are of concern and the HWA predictions do not recognise the following:
- conceptually, generalism is an approach – more doctors does not equate to more generalists
- the big picture challenges that may impact on the health system
- the substantial transformational changes occurring within and beyond generalist practice settings.
Transformational issues within generalist practice setting
Substantial changes are occurring within the primary care generalist practice setting. GPs are responding to older patients who present with chronic complex conditions and multimorbidity.13 GPs are working fewer hours and are more focused on a work–life balance.14 There is a decrease in the number of GPs choosing to work in general practice organisations, undertaking teaching, research14 and choosing to be non-principals. They are working more in expanded team-based models of care with role delegation and substitution arrangements with practice nurses, nurse practitioners, allied health assistants, pharmacist and paramedics.15 There is also a decrease in the number of medical students choosing general practice as a career.14
Outside the clinical setting, new organisational networks (eg. Medicare Locals) are taking action to support workforce planning, retention and development activities matched to the population health needs.16 The Commonwealth and state governments also continue to fund multiple transformational initiatives within generalist practice settings. General primary care medical practitioners are being recruited to adopt, implement and sustain new models of care, which require new skills and role re-design. These transformative changes reinforce the notion of general practice as a complex adaptive system17 because of diversity (complex), uncertainty, unpredictability (adaptive) and interdependencies (system) that exist. All of these issues need to be considered in any attempt to quantify and predict generalist workforce requirements.
Generalist workforce capability-based model
Educators have argued to go beyond building individual skills, knowledge, competencies, and to focus on building capabilities – the ability to apply knowledge, adapt to change and implement competencies within and across sectors, settings, organisations and systems – given the uncertainty and unfamiliarity in which healthcare workers work.18 However, in workforce planning, there continues to be an emphasis on aligning competencies with job role requirements and allocating the appropriate skill mix to meet the models of care and service delivery requirements.19 We argue that current workforce planning number and competency-based approaches are limited, given that generalist primary care medical practice is underpinned by a philosophy defined by distinct principles and practices within diverse settings with uncertainty, unpredictability and interdependencies. Furthermore, a generalist workforce approach is not just a challenge for workforce planners, but has implications for how we prepare (workforce educators) and support and sustain (workforce regulators, managers, funders) our generalist workforce. It is not possible to build generalist workforce capability by simply incorporating a generalist ‘philosophy of practice’ into a practical workforce planning approach in isolation from workforce educators; regulators, funders and employers of generalists.
Workforce capability frameworks20 and resources21 exist that provide a structure for supporting the workforce. However, we need to go beyond structural plans, to develop a capability-based model to ensure that the capabilities required of a generalist workforce are implemented within diverse contexts (ie. sectors, settings, targeted populations groups and organisations), within multiples levels of care (ie. individual/micro, organisational/meso, systems/macro), and has appropriate supporting mechanisms (ie. workforce planning, service planning, financial planning, workforce development, human resource management, governance arrangements). Figure 1 illustrates the proposed model, highlighting the interdependencies between the contexts, mechanisms and level of care. The model provides a framework to move beyond focusing only on identifying, predicting and modelling workforce supply and demand. Table 2 provides rationales for the mechanisms to support generalist practices.
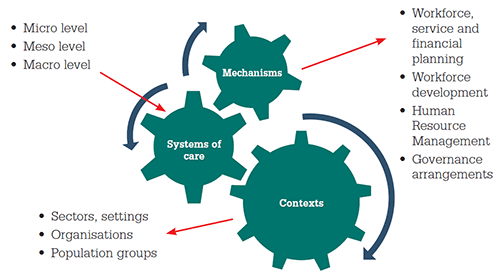
Figure 1. Generalist workforce capability-based model
Table 2. Mechanisms to support generalist practices
- Integrated workforce, service and financial planning – due to the recognition that more GPs does not equate to more generalist practices, and that generalist practice requires service and funding redesign
- Governance arrangements – due to the recognition that a supportive governance and authorising environment is required to apply and implement generalist capabilities
- Workforce development, education and training – due to the need to build more emphasis on generalist capabilities into training programs (ie., how to ensure primary care practitioners are trained in generalist principles and practices, and able to apply and deal with increasing complexity and uncertainty)
- Human resource management (recruitment, selection, retention) – due to the need to increase medical students choosing and continuing a generalist career pathway
|
The model could serve as way to bring together academics, policy makers and practitioners to reach consensus as to how to incorporate a generalist workforce approach into practical workforce planning, education, regulation, funding and governance arrangements (mechanisms), within differing contexts and levels of care. More pragmatically, the model could also inform the assessment of the content of current medical and nursing education curricula or regulations or funding arrangements in relation to the recognised principles, dimensions, and expertise of a generalist workforce, within differing contexts and level of care.
Key points
- With increasing demands on the health system from both the demand side and workforce side there is a resurgence in interest in strengthening generalist primary care medical practice.
- Current workforce planning approaches that focus on identifying, predicting and modelling workforce supply and demand are limited due to definitional, pragmatic and transformational issues.
- A generalist workforce capability-based model is proposed to ensure that the capabilities required of a generalist workforce are implemented within diverse contexts and levels of care, and supported with appropriate mechanisms (workforce planning, education, regulation, funding and governance arrangements).
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.