The reasons behind the sobering disparity are varied and complex. It is imperative that a person’s health be considered in the context of their social, emotional, spiritual and cultural wellbeing, and that of their community. Having at least a rudimentary understanding of the history and politics that have shaped the lives and health of Aboriginal and Torres Strait Islander people helps to place some health behaviours into context. For example, the policy of forcibly removing children from Aboriginal families until the 1960s known as the Stolen Generations5 may still engender distrust of the ‘system’ in Aboriginal mothers.
It is also important to realise that Aboriginal communities across Australia are not a homogenous group. They vary in their cultural beliefs and practices, language, historical events and geography from the urban setting to remote communities. Most Aboriginal and Torres Strait Islander peoples live in inner regional or urban areas and 33% live in capital cities.6 Healthcare for Aboriginal and Torres Strait Islander people is delivered mainly through mainstream services and not through dedicated Aboriginal community-controlled organisations, and is therefore a concern for healthcare providers across all settings.
Many Aboriginal and Torres Strait Islander women experience healthy pregnancies. The women having babies are generally younger and, on average, have more children during their reproductive life than non-Indigenous women.1 Aboriginal culture has many strengths that can provide a positive influence, such as a supportive extended family network and kinship, connection to country, and active cultural practices in language, art and music. It informs a more holistic view of wellbeing.7 For women who experience adverse events in their pregnancies, the reasons are diverse and occur throughout the life course (Figure 1).
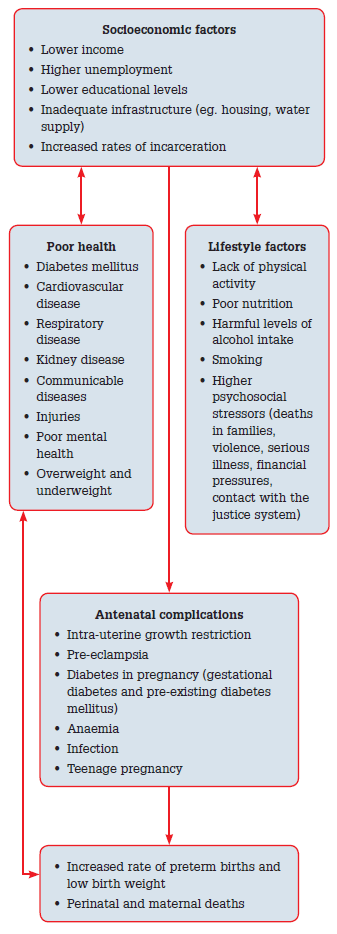
Figure 1. Factors that influence pregnancy outcomes in Aboriginal and Torres Strait Islander women
This article aims to give an update on pregnancy care and the steps general practitioners (GPs) can take to provide best practice care in a culturally appropriate manner. Some aspects of culturally competent care presented here are not new but given the persisting disparity in pregnancy outcomes between Aboriginal and Torres Strait Islander and non-Indigenous women and the continual addition of overseas-trained doctors to the primary care workforce it is important this topic be addressed on a regular basis. It is timely this occurs now with the release of Module 1 of the National Guidelines for Antenatal Care,8 which are discussed in this article.
Improving uptake of antenatal care
Significant improvements in health will be made by tackling the underlying social determinants. Many frontline clinicians feel it is beyond their scope to deal with these issues, but having an understanding of some of these concepts will lead to greater empathy in the interactions with Aboriginal and Torres Strait Islander women. Clinicians also have the opportunity, by being leaders in their communities, to support and even advocate for policy changes at local, state and national levels.
The Department of Health recently published Clinical Practice Guidelines in Antenatal Care.8 Chapter 3 deals with antenatal care for Aboriginal and Torres Strait Islander women and the following discussion draws on elements from this guideline.
Fundamental to improving outcomes for Aboriginal and Torres Strait Islander pregnant women is to engage them in antenatal care. This allows the opportunity to screen for and manage a number of conditions and complications, as well as undertake health promotion activities and risk reduction strategies. Without engagement, opportunities to make a difference are limited. Improving uptake of antenatal care may be achieved through consideration or implementation of the point described below.
Individual cultural competence
Cultural competence is essential for effective communication and cultural security for Aboriginal and Torres Strait Islander women. It involves reflecting on one’s own cultural practices, attitudes and beliefs, and acknowledging differences between one’s own cultural experience and that of patients from other cultures. A number of tools and training programs have been developed and can be accessed to aid in this (Appendix A).
Improve service delivery
A number of programs have been implemented around the country to improve the delivery of antenatal services to Aboriginal and Torres Strait Islander women. Evaluations have shown their success in improving uptake of care earlier in the pregnancies, for the duration of the pregnancy and often post-natally, which allows other opportunistic healthcare interventions, such as family planning, cervical screening and improving breastfeeding rates.9 This shows that if services cater for their needs, women will utilise them. However, not all Aboriginal and Torres Strait Islander women have access to these programs and many still rely on mainstream services such as GPs and public hospital clinics. Hence, it is important that mainstream services embed cultural competence into their quality improvement cycle (Appendix B).
Take an individualised approach
Improve the woman’s experience of antenatal care by taking time to establish rapport and trust (eg. continuity of carer), ensuring her privacy and confidentiality, having some knowledge about the community she is from and endeavouring to have flexible scheduling of appointments. Ideally a nominated person within a practice should be able to ensure the woman is receiving appropriate care from other healthcare team members and to assist to coordinate services if required.
Involve women in decision-making about their healthcare
This means providing information to women in a culturally appropriate way, as well as giving them strategies to help them achieve positive change. There is indirect evidence that in some settings, Aboriginal and Torres Strait Islander women have fewer opportunities to be involved in decision-making than other women.10
Assistance from Aboriginal community workers
Where available, assistance from Aboriginal health workers, community workers or Aboriginal liaison officers should be sought as they can facilitate understanding between the woman and her healthcare provider and provide assistance for attending appointments and coordinating care. This may be particularly important where English is not the woman’s first language.
Special considerations
For the most part, Aboriginal and Torres Strait Islander women have the same requirements in antenatal care as other women. However, there are some specific clinical issues that require special consideration. These issues are covered in the following section.
Psychosocial factors
- Rates of teenage pregnancies are higher in Aboriginal and Torres Strait Islander communities than other communities.1 However, these pregnancies, as with non-Indigenous teenage pregnancies, have higher rates of complication, such as preterm births.11 They also often require higher levels of social support and parenting preparation. It is also important to address contraception and family planning post-natally.
- Aboriginal and Torres Strait Islander women experience high rates of anxiety and depression.12 It is important to screen and refer as appropriate. Note that when using the Edinburgh Postnatal Depression Scale, the score may be influenced by the woman’s understanding of the language used, mistrust of mainstream services or fear of consequences of depression being identified.13
- Aboriginal and Torres Strait Islander women experience higher rates of domestic violence.14 It is important, therefore, to be aware of culturally appropriate services available in the local area and refer patients to these services as required.
Chronic disease
- Rates of pre-existing medical conditions, such as ischaemic heart disease, diabetes mellitus and renal disease, are higher among Aboriginal and Torres Strait Islander women of reproductive age, compared with other women.15 The prevalence of rheumatic heart disease (RHD) is also higher in certain communities, particularly across Northern Australia, which is not usually seen in the non-Indigenous pregnant population.16 Women with RHD may need echocardiograms and cardiology review.
- The safety of current medications in pregnancy should be confirmed.
Physical activity and nutrition
- There are lower rates of folate supplementation in pre-conception and early pregnancy17 and, as access to fresh fruits and vegetables is often limited in many communities, folate deficiency may be more pronounced. Other micronutrient deficiencies include iron and iodine. Cost of supplementation may be an issue in some areas, but supplementation may be freely available in others.
- A high proportion of Aboriginal and Torres Strait Islander women are either underweight or overweight during pregnancy.18 Assessing weight, height and BMI at the booking visit will enable discussion of appropriate weight gain in pregnancy. Weight should be assessed regularly throughout the pregnancy.
- Safe exercise during pregnancy should be discussed.
Infection
- Syphilis is diagnosed more in the Aboriginal and Torres Strait Islander population,19 but as it is a universal screening test in antenatal care, it should be detected and treated in most cases (if the woman is engaged in antenatal care). In areas of high prevalence, consideration should be given to repeat screening in the third trimester.
- Chlamydia screening is recommended for all pregnant women under the age of 25 years, regardless of Indigenous status. For women over the age of 25 years it should be performed as a screening test only if there are high community prevalence rates.8 It is important, therefore, for clinicians to be aware of prevalence rates in their local areas of work.
- Gonorrhoea screening should be performed only if the woman comes from a community with high prevalence.
- Hepatitis C prevalence is higher in the incarcerated population.20 Screening should be offered if the woman or her partner has ever been incarcerated.
- Screening for trichomoniasis in asymptomatic pregnant women is not recommended (including Aboriginal and Torres Strait Islander women) as treatment does not improve outcomes and may cause harm.21
- Screening for bacterial vaginosis in asymptomatic pregnant women is not recommended (including Aboriginal and Torres Strait Islander women).21 However, there is emerging evidence that detection and treatment in early pregnancy may be beneficial in women with a history of previous pre-term birth.22
Smoking and alcohol
- There are higher rates of smoking in Aboriginal and Torres Strait Islander women.3 Reducing this has the potential to make a significant impact on some of the adverse pregnancy outcomes seen in this population. There is currently no evidence of effectiveness for any particular interventions to assist Aboriginal and Torres Strait Islander women to quit smoking in pregnancy.23 Clinicians may be reticent to ask women about smoking in pregnancy and women’s knowledge of the risks of smoking in pregnancy may be limited.23 During pregnancy women should be asked about smoking and the barriers they may encounter when trying to quit. The benefits of quitting should be discussed and cessation advice provided. It is also important that the healthcare team provides support and discusses ways in which the family may support the woman in quitting. There is significant work occurring in this area nationally (Appendix C).
- Aboriginal and Torres Strait Island peoples are less likely to drink alcohol than other Australians but more likely than other Australians to drink at levels above the NHMRC 2001 guidelines if they do drink. A national survey, found that alcohol consumption during pregnancy in non-Indigenous women was 47% and in a survey of Aboriginal and Torres Strait Islander women in Western Australia, the reported rate was 19–44%.24
- It is important for clinicians to be aware that rates of intrauterine growth restriction,3 low birth weight and pre-term births are higher in Aboriginal and Torres Strait Island women than in other women.
Conclusion
As healthcare professionals providing care to Aboriginal and Torres Strait Islander women in pregnancy, we have the potential to improve not only the experience and outcomes of the mothers and their babies but, in the longer term, perhaps also improve the adult health of the babies. Fundamental improvements are needed in the social determinants of health, but as clinicians we can make changes to improve engagement of Aboriginal and Torres Strait Islander women into antenatal care, which is essential for providing ongoing optimal clinical care.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.
Appendix A
- RACGP (2011) Cultural Awareness Education and Cultural Safety Training. The RACGP National Faculty of Aboriginal and Torres Strait Islander Health. Available at www.racgp.org.au/yourracgp/ faculties/aboriginal/education/ cultural-awareness/ [Accessed 27 November 2013]
- Queensland Health Cultural Safety Module. Available at www.health.qld.gov.au/ atsihealth/documents/cultural_ capability.pdf [Accessed 27 November 2013].
Appendix B
- Cultural Respect Framework for Aboriginal and Torres Strait Islander Health 2004-2009. Australian Health Minister’s Advisory Council, March 2004. Available at www.health.gov.au/ internet/main/publishing.nsf/Content/health-oatsih- pubs-crf.htm/$FILE/Cultural_Respect_Framework.pdf [Accessed 11 December 2013].
Appendix C
- www.smokecheck.com.au
- www.ceitc.org.au
- www.aascp.org.au
- Bittoun R, Femia G. Smoking cessation in pregnancy. Obstet Med 2010;3:90–93. Abstract available at www.obmed.rsmjournals.com/cgi/ content/abstract/3/3/90 [Accessed 27 November 2013].