To adequately cover all aspects of palliative care for children, a team of health professionals, including the general practitioner (GP), is required (Figure 1).2 This team is individualised for each patient. Local health resources, including community palliative care teams, the GP and other primary health services, are critical components for achieving appropriately supported palliative and/or terminal care in the community.

Figure 1. Model of care for paediatric palliative care services2,8
Reproduced with permission from NSW Ministry of Health from the Paediatric Palliative Care Planning Framework 2011–20142
Prevalence, diagnostic groups and disease trajectory
It is difficult to quantify the number of paediatric patients in need of palliative care. In Australia, 1503 children aged 15 years or younger died in 2012.3 Formal analysis of these deaths with respect to palliative care needs has not been done. The number of children referred to palliative care is likely to increase with time as awareness of the need and knowledge of what palliative care teams can offer increases in the community and health system. Best clinical practice should aim for palliative care to start at diagnosis of a life-limiting illness rather than when end of life is imminent.4 Although this goal is unlikely to be achieved in every situation, it is probable that early referral for palliative care will mean the GP is exposed to more children who are known to a palliative care team.
Paediatric patients in palliative care fall into two broad diagnostic groups: children with malignancies and children with non-malignant conditions. At Sydney Children’s Hospital, Randwick, non-cancer referrals make up about 60% of patients known to the palliative care team. The patients may have cardiac, respiratory, neuromuscular, renal, metabolic or hepatic conditions.4 Some conditions have a genetic basis and therefore it may be important for the GP to understand the implications for the patient and other family members. Table 1 lists the medical conditions that warrant consideration of palliative care.5,6
Table 1. Referral guide for potential palliative care patients5,6
| Potentially curable conditions for which curative treatment proves unsuccessful (eg. malignancy) |
| Conditions in which intensive therapy prolongs and enhances life before a premature death (eg. cystic fibrosis) |
| Progressive conditions for which no curative or disease-altering therapy is available (eg. neurodegenerative disorders) |
| Non-progressive conditions in which the child is highly likely to die before adulthood as a result of complications such as protracted seizures or respiratory failure (eg. severe cerebral palsy) |
| Adapted with permission from BMJ Publishing Group from Goldman A. BMJ 1998:3166 |
What is the role of the GP?
Specialist PPC services may need to make contact with GPs to assist with care needs of children in the home setting. The child may or may not be known to a GP already. Alternatively, the GP may wish to refer a child and family from their practice to specialist PPC services to assist with needs assessment and access to relevant supports. Over the past 12 years our service has found GPs are willing to be part of the team supporting the child in the community; many have commented on feeling privileged to have been involved in the child’s care.
Acknowledgement of a need for referral to palliative care services need not signify giving up hope. It is not primarily about preparation for death, but rather about improving the quality of life for a child with a life-limiting illness and providing the child and family with optimum support wherever they choose to be. Varied trajectory of disease progression can make it difficult to know when to introduce palliative care. It is important to remember that early referral facilitates building rapport with the family, improves ease of linking in to local services and enhances symptom management.7 These tasks are more difficult if referral is later in the course of an illness. Figure 2 illustrates possible situations when palliative care involvement may be helpful.8
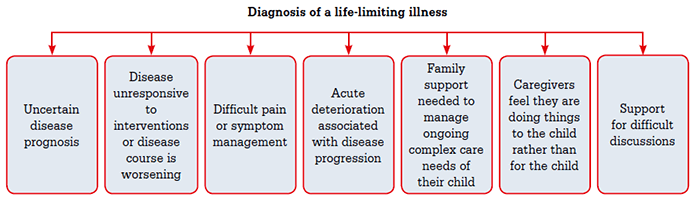
Figure 2. Triggers for considering paediatric palliative care involvement in patients with life-limiting conditions.8
Reproduced with permission from NSW Palliative Care Programme from the Fact Sheet for Health Professionals.8
It can also be difficult to judge when to have discussions about goals and end-of-life care. Although consideration of end of life usually occurs at a point of crisis or deterioration in a patient’s condition, it may be helpful to have these discussions at times of stability. Specifically, the aim is to discuss with the family the concept of hoping for the best while identifying a plan for all possible outcomes. Table 2 lists questions to consider to aid in understanding a family’s goals.9
Table 2. Five important questions for exploring a family’s goals of care9
| Who is your child (as a person)? |
| What is your understanding of your child's illness? What does the illness mean to you and your family? |
| In light of your understanding, what is most important regarding your child’s care? |
| What are your hopes for your child? What are your fears and concerns regarding your child? |
| Where do you find support and strength? |
| Reproduced with permission from Macmillan Publishers Ltd from Waldman E, Wollet. Nat Rev Clin Oncol 2013;109 |
In most cases, children still die in hospital, although it has become increasingly apparent that many families, if given the option, would choose end-of-life care to occur at home.10–12 Some Australian states have purpose-built paediatric hospices, which families may choose as an alternative to home or hospital for terminal care. Hospices can also offer respite for families and patients who need a break from management in home or in hospital. Where possible, it is important that families feel they have a choice over location of end-of-life care. This is more likely to be achieved if patients are linked to PPC services13 and have access to a GP. The GP is essential, particularly if the children are to be successfully managed at home.
As highlighted in the case study below, the role of the GP includes clinical reviews, symptom management, support for community palliative care teams and, if needed, certification after death. The GP also has an invaluable role in assisting with symptom management and review of intercurrent illnesses for the duration of the illness, not just during the terminal phase. The GP’s role can extend to family support, identifying parent and sibling needs, and bereavement support.
Specialist PPC services
Most tertiary paediatric hospitals in Australia have at least some specialist PPC services, but the actual composition at each site is unique. It is generally recognised that a multidisciplinary approach to care is essential and teams may consist of various components including medical, nursing, social work, occupational therapy, physiotherapy, play therapy, psychology, bereavement coordination, volunteer coordination and music/art therapy.14
In Australia, geographical and workforce considerations make it impossible for specialist PPC services to take on direct care aspects for children and families in their local community. They do, however, take on an important role in facilitating communication between specialist/tertiary paediatric services and primary care providers, including GPs, to ensure all relevant medical information and documentation is available for smooth transitions between hospital and community care (Table 3). In Australia, community palliative care teams are based out of adult services. Generally these teams are willing and able to support children and families in the home in conjunction with the GP and paediatric services.
Table 3. PPC information for the GP and local services
| Diagnosis/anticipated problems |
| Medications/allergies |
| Family structure |
| Plan if unwell |
| Details of any resuscitation documentation or discussions |
| Symptom management plan/terminal care medications (if appropriate) |
| Contact details of relevant involved health professionals (and other support agencies) |
| Respite options |
Most services in Australia function in a consultative manner, providing inpatient/outpatient consultations to primary teams, and facilitate primary care links. The services are available to provide education, advice and support to a child’s primary medical team and other involved health practitioners. The aim is to enhance the confidence of any health professional involved in managing the palliative care needs of a child and family. After-hours medical advice for health professionals may also be available. In the future, Telehealth opportunities are also likely to increase.
Care of the dying child at home
This topic warrants an article on its own but it is important to note that while care of a dying child in the home is an uncommon and potentially daunting situation for the GP, it can be an immensely rewarding experience. In most cases terminal care at home can be well managed by the GP, other primary care services and community palliative care teams, with a small selection of medications and ongoing advice from specialist PPC team. Medication detail has not been included in this article; however, it is available from specialist PPC services. The specialist PPC service should provide the GP with an individualised management plan, which includes advice on appropriate terminal care medications.
Bereavement
It has been well established that grief following the loss of a child is profound.15,16 Grief is not limited to parents but can have a marked effect on grandparents and siblings. The GP is in a unique position to be part of bereavement care for families following the death of a child. This care may range from supportive listening and empathy during clinic visits to early recognition of family members in need of referral for bereavement counselling. Specialist PPC services can be contacted at anytime to assist with organising bereavement support.
Conclusion
The GP and other local services are critical components of the team supporting the child, to allow optimal palliative care support to children and families. The GP should feel able to contact specialist PPC services for advice and support to carry out this important role.
Case study
Dave is 14 years of age and has a non-specific neurodegenerative disorder. He has been known to the PPC service for 2 years.
The onset of symptoms was at 15 months of age. Initially, Dave presented with regression of cognitive and motor milestones. Over the next few years he developed dystonia, bulbar dysfunction and poorly controlled complex seizures. There were recurrent hospital admissions for aspiration pneumonias. At the age of 13 years, a gastrostomy tube was inserted to aid nutrition. As the progressive nature of the illness was recognised a referral was made to the PPC team for symptom management, home support and family support.
Dave was reviewed with his mother and father in a PPC multidisciplinary clinic. At the clinic, Dave and his family met the team, comprising a palliative care consultant, palliative care clinical nurse consultant, social worker, physiotherapist, occupational therapist (OT), play therapist and clinical psychologist. A comprehensive review of his clinical and social situation was carried out revealing the significant impact of Dave’s illness on the family. Dave was living at home with his parents and younger sibling, a brother aged 11 years. The family had recently moved to a new house and did not have a GP. Dave could no longer ambulate independently and needed assistance with all activities of daily living. He had limited verbal communication.
Goals of care were identified with the family, including a wish for the family to spend time together and to keep Dave at home as much as possible. At this time, the importance of a GP was discussed. During the clinic visit and subsequent follow-up reviews, the OT was able to help facilitate the family’s access to extra equipment at home. The physiotherapist discussed transfers and positioning at home. The play therapist was able to provide the parents with ideas, including books to support Dave’s brother.
Over the next 6 months Dave continued to have periods of deterioration as well as times of stability. This created significant anxiety for the family, especially as there was no formal diagnosis and, therefore, no clear trajectory of the illness. Dave had constipation, difficulty managing secretions and intermittent respiratory tract infections. Increasingly, the family tried to manage Dave at home and avoid trips to hospital. Dave and his family were supported by a community nurse and referred to the local children’s hospice. However, the family were reluctant to accept respite services and very slow to organise a GP review. Most changes to Dave’s medical management were made by telephone with occasional home visits from the PPC team.
At the age of 13.5 years, Dave and his family had found a local GP who had the capacity to do home visits. The referral was facilitated by the PPC team who discussed Dave with the GP and provided comprehensive information on his current management and contact details of the specialists involved in his care. Initially, the GP saw Dave regularly and was able to manage symptoms with advice from PPC as needed. Dave now has regular bowel actions and reduced respiratory tract infections, which are probably secondary to improved secretion management.
Despite Dave’s complex clinical condition, the involvement of a GP who provided basic symptom management has greatly improved his quality of life and prevented unnecessary visits to hospital. In addition, Dave and his family now have an established relationship with a GP, which will allow them to look after Dave at home if they wish for end-of-life care to be in this location.
While prognosticating remains difficult for Dave’s doctors, he now has the necessary links to hospital, hospice and community providers to allow true choices on well-supported care in any location.
Key points
- PPC is holistic care of children with life-limiting conditions and their families. It is not solely about end-of-life care but care throughout all phases of the illness.
- Children with malignancies make up less than 50% of children known to PPC services.
- The GP and other local community services are critical components of the team around the child, providing support during the illness and into bereavement.
- Many families would like the option of care at home. A good relationship between a patient, their family and the GP can enable this to occur.
- Specialist paediatric services are approachable and available throughout Australia to offer support and advice to GPs and community teams looking after children with life-limiting conditions.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.
Resources for GPs and patients
Handbooks
Journal articles
- Baile WF, Buckman R, Lenzi R, Glober G, Beale EA, Kudelka AP. SPIKES – a six-step protocol for delivering bad news: application to the patient with cancer. The oncologist. 2000;5:302–11 (an excellent tool to facilitate effective communication). Available at theoncologist.alphamedpress.org/ content/5/4/302.full.pdf+html
- Levetown M. Communicating with children and families: from everyday interactions to skill in conveying distressing information. Pediatrics. 2008;121:e1441–e60 (an informative article about effective communication for paediatric patients and their families). Available at pediatrics.aappublications.org/ content/121/5/e1441.full.pdf+html