Pathophysiology
Floaters refer to the sensation of dark spots that are caused either by opacities in the vitreous, which cast shadows on the retina, or by light bending at the junction between fluid pockets and the vitreous.4 Floaters may be caused by vitreous debris from infection, inflammation and haemorrhage, but are typically due to the age-related degeneration of the vitreous, forming condensations of collagen fibres. Patients may describe floaters as ‘flies’, ‘cobwebs’ or ‘worms’ that are more pronounced against light backgrounds. Floaters may also result from haemorrhage of retinal vessels into the vitreous and may be described as minute black or red spots. The most common cause of vitreous haemorrhage is proliferative diabetic retinopathy.5
Flashes are visual phenomena known as photopsias and refer to the perception of light in the absence of external light stimuli. Photopsias can be generated anywhere along the visual pathway, but in the eye they result from mechanical stimulation of the retina by vitreoretinal traction. Flashes are typically described as a momentary arc of white light, similar to a bolt of lightning or a camera flash. They are more noticeable in dim lighting, may be triggered by eye movement and are usually in the temporal visual field.
Posterior vitreous detachment
Posterior vitreous detachment (PVD) is the most common cause of acute onset of flashes and floaters, present in nearly 66% of patients over 70 years.4,6 It is an age-related change in which the vitreous degenerates, shrinks and separates from the retina. During separation, the vitreous may tug and cause mechanical stimulation of the retina, resulting in flashes. Clinically, the patient has normal vision, no visual field defects and no relative afferent pupillary defect.4,7
A patient with posterior vitreous detachment is deemed to be at higher risk of retinal detachment if it is associated with vitreous haemorrhage; about 70% of these patients have been found to have at least one retinal tear8 (Figure 1).
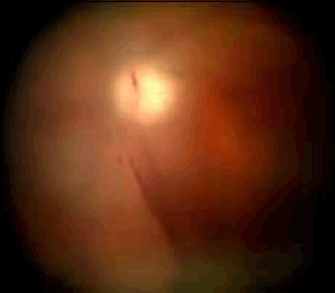
Figure 1. Vitreous haemorrhage associated with posterior vitreous detachment
Retinal tear
Of PVD, 14% cause a tear in the retina during separation.4 Clinically, the patient has no visual field defect and no relative afferent pupillary defect. The patient may complain of black or red spots and impaired vision if the tear has disrupted a blood vessel, resulting in vitreous haemorrhage or release of retinal pigment epithelium.4,9
Retinal detachment
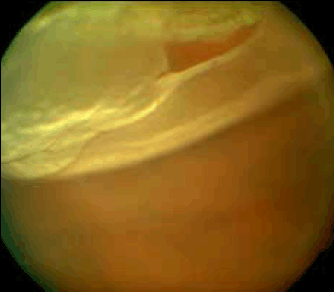
Figure 2. Retinal tear associated with rhegmatogenous retinal detachment
Approximately 33–46% of patients with a retinal tear or hole will develop a rhegmatogenous retinal detachment.10 Fluid from the vitreous is able to pass through the tear underneath the retina, separating it from the retinal pigment epithelium (Figure 2). Detachment can progress as more fluid enters through the retinal break. Detachment results in visual field loss as the photoreceptors become severely damaged by separation from their underlying choroidal vascular supply. For example, a superior retinal detachment will result in an inferior visual field defect. Patients may describe a ‘shadow’ or a ‘curtain coming down’ over their vision. If the macula is detached, central visual acuity is lost and this is typically permanent6 (Figure 3).
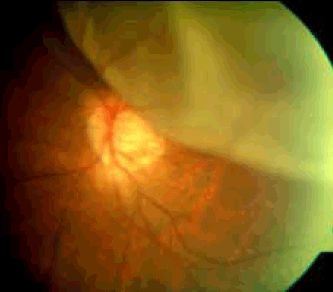
Figure 3. Retinal detachment superiorly (optic disc visible in the background)
The most common location for a retinal tear is in the superotemporal quadrant (60%) and because of the effects of gravity results in a greater incidence of macula-off retinal detachment, compared with inferior or nasal retinal tears.11,12
Other types of retinal detachment include tractional and exudative and these can also present with flashes and floaters. Tractional retinal detachment is caused by mechanical forces on the retina, usually as a result of previous haemorrhage, infection, inflammation, trauma or surgery. Exudative retinal detachment results from accumulation of fluid in the potential sub-retinal space due to disruption of hydrostatic forces (severe acute hypertension), inflammation or neoplasm.13
Assessment
- History: to help differentiate ocular from non-ocular causes of flashes and floaters (Table 1)
- Examine the eye:
- visual acuity of each eye separately and with glasses or pinhole
- visual fields to confrontation
- pupil response for relative afferent pupillary defect (RAPD)
Direct ophthalmoscopy alone is not enough as most retinal tears or detachment are in the periphery; the patient should be referred to an ophthalmologist at this point. Dilating eye drops take 10–15 minutes to take effect and as there is a small risk of triggering acute-angle closure glaucoma, pupil dilation is not ideal in a general practice setting.14,15
General practitioners in rural areas may have limited access to an ophthalmologist; hence those with experience in ultrasonography may be able to determine the presence or absence of ocular pathology. A study assessing the accuracy of bedside ocular ultrasonography in 61 patients in an emergency department showed a sensitivity of 100% and a specificity of 83–97.2%.16,17
Table 1. Differential diagnoses
Flashes
- Ophthalmic
- Posterior vitreous detachment
- Retinal tear/hole
- Retinal detachment
- Optic neuritis – photopsia on eye movement, retrobulbar pain
- Non-ophthalmic
- Migraine – scintillating scotomas, coloured lights, bilateral, evolves over 5 to 30 minutes before resolving with onset of a headache, normal visual acuity
- Postural hypotension – bilateral temporary dimming of vision and
light-headedness
- Occipital tumours
- Vertebrobasilar transient ischaemic attacks
|
Floaters
- Ophthalmic
- Vitreous syneresis
- Vitreous haemorrhage
- Posterior vitreous detachment
- Retinal detachment
- Vitritis
- Tear film debris
|
Referral guidelines
- Patients with symptoms of acute onset flashes or floaters and visual field loss need same day referral to an ophthalmologist for a dilated fundus examination, to rule out retinal tears and retinal detachment.6,9
- Longstanding flashes or floaters require non-urgent ophthalmology review.10
Table 2. Risk factors for retinal detachment1
- Myopia (near sightedness) – the length of the eye and vitreoretinal forces are greater than normal and also the retina is thinner and more prone to breaks
|
- Trauma – compression and decompression forces may generate sufficient vitreoretinal traction to produce retinal tears
|
- Cataract surgery – detachment of the vitreous is accelerated
|
- Previous retinal detachment surgery
|
- Advancing age – degeneration of the vitreous increases with time
|
Treatment by an ophthalmologist
PVD in itself does not require treatment. Depending on the clinical scenario, patients may be re-examined by the ophthalmologist at 6 weeks, as 3.4% will have a new retinal tear. If the patient complains of a new shower of flashes and floaters, or reduction in vision, they should be reviewed sooner.3,4
If the PVD is associated with retinal tears, they need prompt treatment to prevent progression to retinal detachment. Usually, breaks are surrounded with laser or cryo burns to create a chorioretinal scar that prevents fluid seeping into the sub-retinal space.6
PVD associated with retinal detachment needs vitreoretinal management. These include vitrectomy, pneumatic retinopexy and scleral buckling with endolaser or cryopexy.6 A vitrectomy aims to relieve vitreoretinal traction on the retinal tear by removing the vitreous. Pneumatic retinopexy is a procedure where an intravitreal gas bubble is used to seal a retinal break and reattach the retina. For scleral buckling, a band is placed on the exterior surface of the globe, indenting the sclera so that vitreoretinal traction is reduced.13
If the macula was not detached before surgery, visual acuity will be maintained. If the macula was detached before surgery, final visual recovery depends on the duration and degree of elevation of macular detachment and the patient’s age. Surgery, therefore, is more urgently indicated in patients with preserved visual acuity. Surgery is routinely done in patients whose macula detached within a week.13
Key points
- Flashes and floaters are usually signs of benign disease; however, a small percentage will have sight-threatening disease and hence all patients require a dilated fundus examination.
- If symptoms of acute onset flashes and floaters are present urgent same day referral is required.3,4
- Acute-onset flashes and floaters with visual field defect are suggestive of retinal detachment.
Competing interests: Jolly Gilhotra is a paid board member of Alcon and has received payment for consultancy, expert testimony, lectures, manuscript preparation, travel expenses, accommodation and has grants pending from Bayer Pharmaceuticals and Novartis Pharmaceuticals.
Provenance and peer review: Not commissioned; externally peer reviewed.
Acknowledgements
The authors would like to thank Anton Drew, ophthalmic photographer at the Queen Elizabeth Hospital, for the retinal photographs.