Stress is a state that can be precipitated by a range of factors, including unpleasant circumstances, that, when chronic, cause the signs and symptoms of anxiety in its sufferers, such as poor sleep, impaired concentration and irritability.
Why stress?
The explanation of stress seems to lie in the oft-used medical adage – ‘it varies’. As a society we have an ambivalent attitude to stress, however we define it. On the one hand, we have access to a wide range of techniques, nostrums and medications to help reduce it. On the other hand, we make little genuine effort to prevent or manage it. Indeed, our modern lifestyles seem to encourage it, with increasing work hours, commitments and expectations. Logic demands that for behaviour to be maintained, it must confer some advantage. It appears that if we have too little stress, we act below our peak efficiency. Increasing stress so that we operate at peak efficiency is said to utilise good stress or ‘eustress’.2
In other words, stress can be a useful part of the ‘fight or flight’ response, allowing us to be ready for action when necessary. This concept is embodied in the Yerkes–Dodson law,3 or the anxiety performance curve (Figure 1).
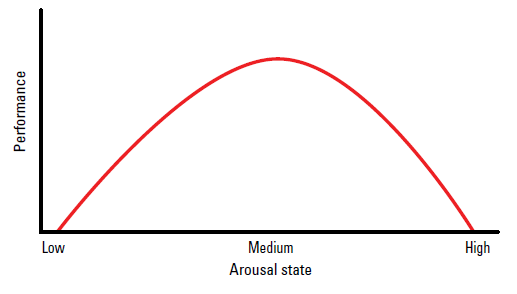
Figure 1. Yerkes–Dodson law, or the anxiety performance curve
The curve indicates that, depending on a person’s initial level of stress or where they are on the curve, performance can be improved by either decreasing or increasing stress. If they are on the left of the curve, increased stress will improve performance; in the middle of the curve, an increase in stress will worsen performance; and on the right of the curve, performance will improve only if arousal/stress is decreased
The Yerkes–Dodson law indicates that performance increases with (cognitive) arousal, but only to a certain point; when levels of arousal become too high, performance decreases.3,4 In this case, cognitive arousal is a synonym for stress. The curve indicates that, depending on a person’s initial level of stress, performance can be improved by either decreasing or increasing stress. This suggests that the aim of intervention should not necessarily be to abolish stress, but to manage it.4
The ‘general adaption syndrome’5 is an alternative analogy proposed by Hans Selye, a Hungarian endocrinologist, widely considered the father of stress. He described three stages of the stress response as:
- alarm
- resistance
- exhaustion.
There is an initial strong response to the stressor, physiological, emotional and/or behavioural. This is maintained until the challenge is met or, if the challenge is overwhelming, the individual reaches a stage where the response can no longer be sustained – exhaustion. This concept can be useful when describing the costs of chronic stress to patients and that this is a process mediated by the neuroendocrine systems and not just ‘all in the mind’.
Stress is subjective and individual
Such is the range of the human condition that very few circumstances are universally stressful. Stress seems to rise from a clash between a person’s perception of events and their expectations.
The age-old argument of nature versus nurture could also be seen to impact on the individual’s response to stress. To paraphrase Shakespeare, ‘Some are born stressed, some achieve stress and some have stress thrust upon them’.6
There are some individuals who seem, by nature, to exhibit more extreme stress reactions, and these behaviours can be present from a very early age – the placid versus the unsettled and highly responsive newborn, for example.
Then there are those who seem to deliberately expose themselves to excessive stress by seeking out increasing commitments in work or personal life, and perhaps achieve a state of heightened responsiveness by repeated exposure. And finally, there is the group who find themselves in unpleasant circumstances for which they bear no responsibility and that they cannot exert control over.
Further, the stress an individual experiences may not be proportional to the quality of their performance. The Dunning–Kruger effect describes a cognitive bias in which unskilled individuals suffer from illusory superiority, mistakenly rating their ability much higher than average.7,8
So, at one extreme, there are perfectionists who perform better than others but who have insufficient confidence in their own abilities, which leads to the experience of stress; at the other extreme, there are those who are relaxed and confident, but are not as capable.
Is stress dangerous?
Historically, doctors have been taught that psychosomatic complaints are unpleasant, but not dangerous. It is now known that stress is a major cause of illness, especially cardiovascular, gastrointestinal and psychiatric disease,9 both directly and indirectly, due to the harmful behaviours through which people seek to relieve their distress (eg. substance abuse).10
Of course, excessive stress is not in itself a diagnosis. Like iron deficiency, it is a symptom and once detected, it should lead us to look deeper into the patient’s circumstances. Chronic stress can certainly predispose to anxiety and depression,9 and whether or not these conditions develop tends to depend on the individual response to the stress. Anxiety may also be the manifestation of other conditions. The Diagnostic and Statistical Manual of Mental Disorders, Version V (DSM-V) criteria states that anxiety may accompany depression and other mood disorders, psychoses and neurodegenerative conditions, including dementia.11
Excessive stress can also aggravate the symptoms of a wide range of conditions, hastening the patient’s decline. This reflects the consequences of the placebo and nocebo effects.12 Perceptions matter. For example, patients may worry about stopping smoking due to the stress it will cause them, because they perceive the effects of stress to be worse than those of smoking. Negative expectations feed into their experience. The experience of stress and its consequences are very real for the patient, and stress has rarely been known to improve a condition.
How can we prevent excessive stress?
Stress may be relieved by following the ancient principle of mens sano in corporo sano – a healthy mind in a healthy body – and aiming to achieve a balance of physical and mental fitness by following accepted principles. The acronym PRAISES can provide a framework for addressing life balance with patients (Table 1).5
Table 1. The PRAISES approach to assessing life balance
| Domain | Activity |
|---|
| Physical |
Health/self care |
| Recreational |
Fun/relaxation |
| Artistic |
Creative pursuits or appreciating creativity of others (eg. listening to music) |
| Intellectual |
Direct or indirect learning |
| Spiritual |
Connection beyond the individual/family (eg. community, religion) |
| Employment |
Pursuit of financial goals |
| Social |
Time spent with important others (eg. family) |
Mental fitness also requires the development of frustration tolerance, namely enhancing the level of a person’s ability to withstand challenges or disappointment without developing inadequate modes of response, such as ‘going to pieces’ emotionally.13 This concept involves practise. Teaching a child to accept being told ‘no’ when appropriate, and to be able to graciously tolerate a loss in a sporting game, is an illustration of the foundations of this concept.
It is also helpful to utilise a wide range of relaxation therapies.
How can we treat those with excessive stress?
If a patient comes into your consulting room exhibiting signs and symptoms of anxiety – are they stressed? Of course, it varies.
Management firstly consists of good communication and diagnosis. Table 2 outlines an approach to the assessment of the stressed patient.
Table 2. Assessing a stressed patient – some points to consider
- Are you aware of any psychiatric history, including that of family members or personal history in both childhood and adulthood?
- What are the stressors in this patient’s life?
- When did the patient first notice their symptoms?
- Are the patient’s stressors excessive compared to what might be considered usual? ‘How would another person cope in your circumstances?’ can be a useful question to ask
- Is the patient as aware of their symptoms and signs as you are?
- Stress is very much influenced by individual perceptions. Explore the patient’s perceptions – you may be the first person to whom they have mentioned their concerns or issues
- Does the patient have underlying perfectionist qualities and is anxious that they have not achieved their goals?
- Is the presentation part of another psychiatric disorder, such as anxiety or mood disorders, psychosis, delirium or dementia?
- How does the patient manage their symptoms? Do they use medication or recreational substances? Take a drug and alcohol history
|
Communication is essential to understand the patient as an individual. They need to trust us, so that we can really learn about them and not just be told what they think we want to know.
It is wrong to think that a patient is ignorant, but dangerous to assume that their understanding of specific terms is the same as yours. One of the meanings of the word ‘doctor’ is ‘teacher’, and this should remind us to apply educative principles and ask a person about their own meaning of the word ‘stress’ rather than tell them about it, providing them with a regurgitated, rehearsed speech, which may be totally irrelevant to their needs. For example, a patient saying they get ‘stressed’ when they exercise, may reveal on close questioning symptoms of angina.
Patients and their carers must be educated, and relaxation and lifestyle changes encouraged. Referral to specialists and allied health professionals may be appropriate, as may the use of medication. Even when it may seem that therapeutic options are exhausted, there are still things that we, as general practitioners, can do to assist our patients who are experiencing excessive stress (Table 3).
Table 3. Four things to do when nothing else can be done
- Education – ensure the patient has as much information as they need about their illness
- Diet – ensure the patient receives information on an appropriate diet
- Exercise – ensure the patient receives information on an appropriate exercise program – even the dying will receive some benefit from activity
- Stress management – internal and external
- External:
- pharmacotherapy
- massage
- aromatherapy
- music therapy
- acupuncture
- Internal:
- relaxation exercises and procedures
- positive imaging and techniques include breathing, muscle contraction and muscle relaxation exercises
- spiritual: reconciliation and forgiveness for those who have wronged them
- relationship counselling
- meditation
- prayer
- sexual counselling – even the ill are entitled to a good sex life
|
|
Courtesy of Professor Mark Cohen, RMIT University Health Innovations Research Institute
|
Key points
- Stress is a word commonly used, but vaguely applied, in the community.
- Signs and symptoms of anxiety can also be part of more serious physical and psychiatric conditions.
- Stress or arousal can have positive effects when appropriate.
- Helping a patient to manage stress relies on understanding the individual in their own circumstances.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.