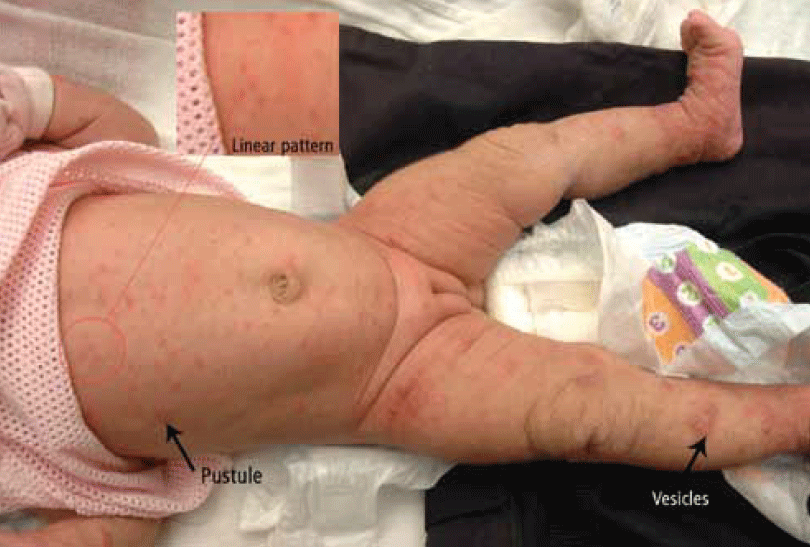
Figure 1. Papules, vesicles, pustules and linear pattern of burrows on the infant’s body
Question 1
What is the most likely diagnosis?
Question 2
What differential diagnoses would you consider for rash in an infant?
Question 3
What clinical features would you look for to support your diagnosis and how would you confirm your diagnosis?
Question 4
What are the available treatment options for this condition?
Question 5
How would you manage this infant?
Answer 1
The generalised, polymorphous appearance of the rash and the family history of pruritic rashes mean the most likely diagnosis is scabies infestation caused by Sarcoptes scabiei mites.
Answer 2
Differential diagnoses for neonatal rashes should include:1,3–7
- eczema – this commonly affects the face, neck, elbow and knee flexures in an infant
- infantile seborrhoeic dermatitis – this is a common neonatal scaly disorder that involves the face and scalp
- papular urticaria – caused by an allergic reaction to insect bites. Skin hypersensitivity created by the scabies infestation
- erythema toxicum – the rash, which is noninfectious and asymptomatic, usually occurs from birth to 2 weeks of age and can affect any area of the body. It comprises red macules, papules, pustules or wheals that disappear within a few days
- insect bites – usually on exposed parts of the body.
Examination of the whole body is essential in making the correct diagnosis.
Answer 3
Classic clinical features of scabies include intense itch and the presence of characteristic skin burrows, which can be linear or ‘S’ shaped, papules, nodules, vesicles and pustules. Lesions are usually seen in the finger webs and flexural regions of the wrists, elbows, axillae and perineal regions in older children and adults. Nodules on the penis and scrotum are pathognomonic. In females, these lesions are also found under the breasts and around the areola. Both the mother and the sibling were treated for scabies and did not exhibit classic features or any signs of infestation under the nail plates.
Clinical presentation in neonates is unlike that of adults and older children, resulting in missed or delayed diagnosis. Neonates do not itch but present with extensive rashes, irritability, poor feeding and failure to thrive. The skin lesions spread rapidly, and involve the face, scalp, palms and soles. Vesicles are common, leading to early pustulation, crusting and scaling.
Diagnosis is usually based on clinical appearance and history of close or familial contact with a pruritic rash. Scabies is highly contagious and spreads mainly through direct skin contact although fomites like bedding can also transmit the infestation. If a definitive diagnosis is required, the condition can be confirmed by skin scrapings and low power magnification to look for the presence of mites, eggs or faeces (scybala). This was not performed in this infant as the diagnosis was clear, based on the history and physical examination.
This case illustrates the importance of taking a detailed history, including family history, and systematic examination in the approach to dermatological problems. 1–8
Answer 4
The available treatment options are as follows:5,6,9–11
- permethrin cream 5%. This is a synthetic pyrethroid that is safe and effective in killing both mites and eggs and hence is advocated as the treatment of choice by Centers for Disease Control11 and the Cochrane review group.9 But it cannot be prescribed to infants less than 2 months of age
- crotamiton cream 10% is less effective but has some antipruritic effect. It has not been approved by the Food and Drug Administration for use in children
- lindane lotion 1% is not recommended as a first line therapy because of its neurotoxicity. It should not be used in children or pregnant or breastfeeding women
- emulsion benzyl benzoate 12.5% (for children >2 years and 25% for adults) is a cheap and effective scabicide in developing countries where cost is an issue. However, it can be very irritating to the skin and cannot be used for young children under 2 years of age12
- ivermectin is an oral preparation that is especially effective for crusted scabies. Its safety profile for children weighing less than 15 kg and in pregnant women has not been established.
Answer 5
This infant was initially treated with sulphur 5% in calamine lotion applied once daily for 3 days over the whole body including the scalp, hairline, neck, side of the face, forehead, palms and soles. Care was taken to avoid the eyes and mucous membranes. Mittens were worn over the hands to prevent the baby from sucking the medication. The calamine lotion is soothing and antipruritic. This baby’s treatment was continued with twice daily crotamition cream for 2 weeks to relieve itchiness and to cover incomplete eradication.
The Therapeutic Guidelines12 recommend sulphur 5% in white soft paraffin, applied once daily for 2–3 days for babies younger than 2 months of age, with crotamiton 10% cream as an alternative. Permethrin 5%, while not approved for use in very young infants, may also be considered if the clinician judges the benefits outweigh the risk of treatment.12
Pruritus begins only 4–6 weeks after a first time infestation due to a type 4 delayed hypersensitivity reaction to the mites and their faeces. This asymptomatic period allows for unchecked spread within families and institutions. In this case, the sibling was infested at his daycare facility and carried it back to his family. The mother’s diagnosis was initially missed as the pruritic rashes were thought to be due to gestational diabetes or pruritic urticarial papules and plaques of pregnancy.6 The neonate was infested while breastfeeding but was misdiagnosed as having erythema toxicum and eczema and so the correct diagnosis was delayed. This case illustrates the public health implications of this highly contagious infestation and the consequence of missed or delayed diagnosis. All family members and prolonged skin-to-skin close contacts, whether symptomatic or not, have to be treated simultaneously to prevent re-infestation.
For the mother and sibling, the treatment of choice is permethrin 5% cream, applied from neck to toes and beneath the nail plates and kept on for 8 hours or overnight before washing off.9–11 It can be prescribed for this lactating mother (ADEC category B2) under Australian guidelines.12 A repeat treatment 1 week later is advised to cover for incomplete eradication.
If the infected child attends childcare, the facility has to be informed and the child should not return until a day after commencing treatment.13 This is to prevent re-infestation at the institution.
The mother was advised to trim all fingernails6 to prevent re-infestation and secondary bacterial infection. Other precautionary measures include washing bed linen and clothing in 60°C hot water7 and drying laundry in the sun or in a hot air dryer. Items like toys that cannot be washed can be dry cleaned or placed in a plastic bag7 and sealed tightly for a week to kill the mites. Mites cannot survive more than 48–72 hours away from the human body.11 Upholstered furnishing and bedding can be vacuumed. There is no need for special fumigation.
Patients have to be advised that even after successful eradication, pruritus can continue for another 2–4 weeks5–7 until all mite proteins have been degraded and removed. Pruritus can be treated with topical steroid cream and antihistamines. However, promethazine is contraindicated for children under 2 years and should not be prescribed for this infant. If itching continues more than a month post-treatment, consider the possibility of re-infestation, allergic dermatitis or incorrect diagnosis.
Conflict of interest: none declared.