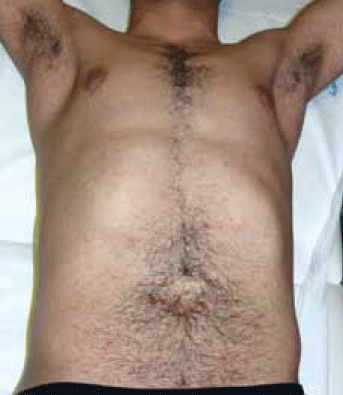
Figure 1. Scattered excoriated papules over the trunk and axillary folds
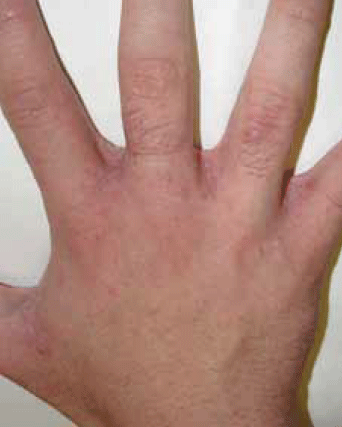
Figure 2. Scabby plaques in the interdigital web spaces of the hands
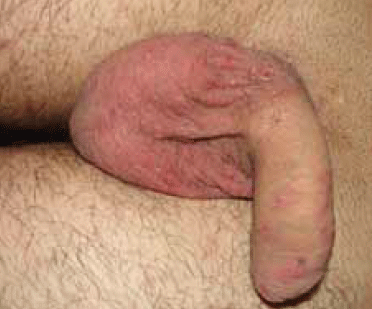
Figure 3. Erythematous nodules and scratching lesions located on the scrotum and penile shaft
Question 1
Based on the history and physical examination, what is the most likely diagnosis?
Question 2
What diagnostic tests are useful to confirm the clinical diagnosis?
Question 3
What is the differential diagnosis?
Question 4
What are the treatment options for this disease?
Question 5
What are the possible reasons for persistent symptoms, despite treatment?
Answer 1
Scabies is the most likely diagnosis. The possibility of scabies should be suspected in patients with one or more of the following:1
- widespread itching that worsens at night, spares the head (except in infants and young children), and seems to be out of proportion to visible changes in the skin
- a pruritic eruption with characteristic lesions distributed primarily in the following areas:
- between the fingers, on the elbows, wrists and in the armpits
- around the nipples, waist and buttocks
- genital areas, particularly the penis and scrotum
- close contacts with similar symptoms.
Answer 2
Diagnostic tests, such as the adhesive tape test, skin scrapings and dermoscopy can provide confirmation of the diagnosis.
- Adhesive tape test: The adhesive tape test involves the use of transparent tape with a strong adhesive (eg. clear packing tape).2 The tape is firmly applied directly to a skin lesion and then rapidly removed. After applying the tape to a glass slide, the clinician utilises a microscope to examine the tape for mites and eggs. An advantage of the adhesive tape test is the lack of need for specialised equipment (other than a microscope). The procedure may also be useful in children who cannot tolerate skin scrapings
- Skin scrapings: The following procedure allows identification of mites or eggs in scrapings from burrows or papules:3
- equipment: alcohol preparation, number 15 or 18 blade, glass slide and coverslip, microscope
- look for a nonexcoriated papule with a fine white-to-grey line across the top
- scrape the area with a number 15 blade or pinch the area between the thumb and index finger and superficially shave the top layer of skin; anaesthesia is not necessary
- place the specimen on a glass slide, apply the coverslip and examine it under the microscope at 10x magnification to identify the female adult mite (0.4 mm long), the male (0.2 mm long), the eggs or faeces (Figure 4)
- mite eggs are all the same size, while air bubbles are different sizes and change with compression of the slide
- Dermoscopy: Examination of the skin surface with a handheld dermatoscope may be useful. The test can be used to directly visualise mites and eggs for diagnosis or as a guide in choosing the site for skin scrapings.2 The characteristic finding on dermoscopic examination is a dark, triangular shape that represents the head of the mite within a burrow ('delta wing' sign). Eggs may also be visible. These features are frequently difficult or impossible to detect in patients who have dark skin.4
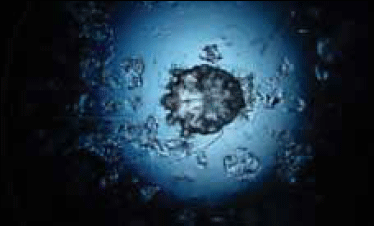
Figure 4. Microscopic features of Sarcoptes scabiae
Answer 3
The lesions of scabies are often excoriated, obscuring their appearance. The differential diagnosis is broad and scabies can appear similar to eczema, tinea, atopic dermatitis, papular urticaria, seborrheic dermatitis and acropustulosis of infancy.5 The diagnosis of scabies usually rests on the typical distribution of lesions and a history of affected family members. It is recommended to perform a complete clinical examination including the genitalia. In males, the presence of itching erythematous nodules on the scrotum is highly suggestive of infection by Sarcoptes scabiei.
Answer 4
Treatment for scabies includes administration of a scabicidal agent, an antipruritic agent such as a sedating antihistamine and an appropriate antimicrobial agent if secondarily infected.
- Permethrin 5% cream appears to be safe and effective even when applied to infants less than 1 month of age, although Australian guidelines recommend use only in those aged 6 months or over.6 Patients should massage permethrin cream thoroughly into the skin from the neck to the soles of the feet, including areas under the fingernails and toenails; 30 g is usually sufficient for an average sized adult. The hairline, neck, temples and forehead may be infested in infants and geriatric patients. In these populations, permethrin should also be applied to the scalp and face, sparing the eyes and mouth. Permethrin should be applied last thing at night to avoid inadvertent removal (eg. with hand washing). The cream should be removed by washing (shower or bath) after 8–14 hours. Two applications, about a week apart, may be necessary to eliminate all mites (including hatchlings), particularly when treating crusted (Norwegian) scabies5,7
- Ivermectin is an oral antiparasitic agent approved for the treatment of worm infestations. Evidence suggests that oral ivermectin (200 µg/kg) may be a safe and effective treatment for scabies.8–10 However, ivermectin is not Therapeutic Goods Administration or Pharmaceutical Benefits Scheme (PBS) subsidised for this use. Its use should be considered in patients who have failed treatment with, or who cannot tolerate, topical medications for the treatment of scabies and/or for severe forms such as Norwegian scabies. A total of two or more doses at least 7 days apart may be necessary to eliminate a scabies infestation. Ivermectin is not recommended for use in pregnant or lactating women and safety has not been determined in children who weigh less than 15 kg. Outside of these groups, ivermectin can be considered a very safe treatment11,12
- Lindane lotion 1% is not recommended as a first-line therapy. Overuse, misuse or accidental ingestion can be toxic to the brain and other parts of the nervous system; its use should be restricted to patients who have failed treatment with or cannot tolerate other medications.
All family members and close contacts, including sexual contacts, must be evaluated and treated for scabies, even if they do not have symptoms. When a person is infested with the scabies mite for the first time, symptoms may not appear for up to 2 months. Therefore, asymptomatic individuals can still infect others. All persons should be treated at the same time in order to prevent re-infestation. Pets do not require treatment. All carpets and upholstered furniture should be vacuumed and vacuum bags immediately discarded. Instruct patients to launder clothing, bed linen and towels used within the past week in hot water the day after treatment is initiated and again in 1 week.
Answer 5
The most common symptoms of scabies (itching and skin rash) are caused by sensitisation to the proteins and faeces of the parasite. A number of factors may contribute to the persistence of symptoms for more than 2 weeks post-treatment including:11
- incorrect diagnosis of scabies – many drug reactions can mimic the symptoms of scabies and cause a skin rash and itching
- treatment failure due to medication resistance, incorrect application of topical scabicides or failure to complete the second topical application
- treatment failure of crusted scabies because of poor penetration of scabicide into thick, scaly skin containing large numbers of scabies mites; repeated treatment with a combination of both topical and oral medication may be necessary to treat crusted scabies successfully
- re-infestation from a family member or other infested person if the patient and all their close contacts are not treated simultaneously
- re-infestation from items (fomites) such as clothing, bedding or towels that were not appropriately washed or dry-cleaned
- an allergic skin rash (dermatitis) or exposure to household mites that cause symptoms to persist because of cross-reactivity between mite antigens.
Conflict of interest: none declared.