Each year on average in the BEACH (Bettering the Evaluation and Care of Health) program, GH has been managed at 6.7 per 100 000 recorded general practice encounters (about 670 times a year nationally). Although rarely managed, 92 GH encounters were recorded from April 1998 to March 2012.
GH was significantly more likely to be managed at female (8.3 per 100 000) than at male patient encounters (3.9 per 100 000). The lowest age-specific rates were among the young and the elderly.
As expected, the most common patient reasons for encounter (RFEs) were ‘throat symptom/complaint’ (40.2% of GH encounters) and ‘swallowing problem’ (17.4%). Conversely, GH was an unlikely diagnosis arising at 0.1% of encounters with an RFE of ‘throat symptom/complaint’ and at 1.2% of encounters with an RFE of ‘swallowing problem’. GH was managed as a new problem at 37 of the 92 GH encounters. Other problems commonly managed with GH were anxiety and GORD.
Management of GH included significantly higher rates of specialist referrals (23.9 per 100 GH problems) and imaging (14.1 per 100 GH problems) (presumably to exclude organic pathology), but significantly lower rates of medication (25.0 per 100 GH problems) than the BEACH averages for 2011–12 (5.6, 6.6 and 69.6 per 100 problems respectively, n = 152 286). Of the 22 referrals, 17 were to ear, nose and throat specialists, and four to gastroenterologists. Of the 23 medications recorded, 11 were anxiolytics or antidepressants. Of the 13 imaging requests, five were for barium swallow and four were for ultrasound of the neck or thyroid. There were no significant differences in the rates of clinical treatments (counselling, advice) or of pathology tests ordered, compared with the averages for all problems managed in the 2011–12 BEACH year.
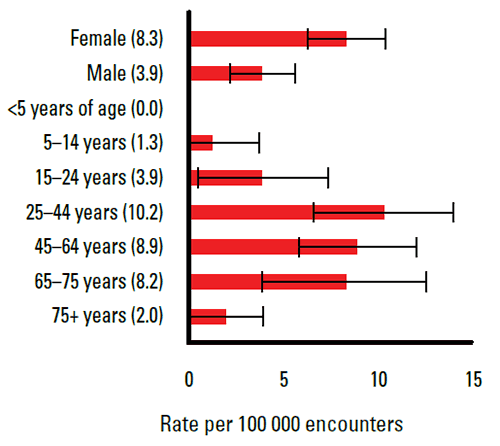
Figure 1. Sex and age-specific management rates of globus hystericus (error bars indicate 95% confidence interval)
Competing interests: None.
Provenance and peer review: Commissioned; not peer reviewed.
Acknowledgements
The authors thank the GP participants in the BEACH program and all members of the BEACH team. Financial contributors to BEACH between 1998 and 2012: Abbott Australasia; AstraZeneca Pty Ltd (Australia); Australian Government Department of Health and Ageing; Australian Government Department of Veterans’ Affairs; Australian Institute of Health and Welfare; Aventis Pharma Pty Ltd; Bayer Australia Ltd; CSL Biotherapies Australia Pty Ltd; GlaxoSmithKline Australia Pty Ltd; Janssen-Cilag Pty Ltd; Merck, Sharpe and Dohme (Australia) Pty Ltd; National Occupational Health and Safety Commission; National Prescribing Service; Novartis Pharmaceuticals Australia Pty Ltd; Pfizer Australia; Roche Products Pty Ltd; Sanofi-Aventis Australia Pty Ltd; Wyeth Australia Pty Ltd.