Fortunately, skin cancer is amenable to early detection and potential cure. About 86% of the Australian population present to a GP each year.2 Hence, GPs are well placed to facilitate the detection of skin cancer by using opportunistic examination, a high index of suspicion and good observation skills. The article by Sinclair in this issue of Australian Family Physician provides further details on providing skin checks in the general practice setting.
Nonmelanoma skin cancers are a lot more common than melanoma and their detection and treatment mainly occurs in general practice.3 This article outlines the presentation of common NMSCs and the treatment options currently available. It also highlights which lesions may be best referred for specialist review.
Basal cell carcinoma
Basal cell carcinoma (BCC) is the most common skin cancer, accounting for about 68% of all skin cancers.1 Squamous cell carcinoma (SCC) accounts for 28%, melanoma 3%, and rarer tumours such as merkel cell carcinoma, 1%.1 The three main clinical presentations of BCC are:
- nodular
- superficial
- morphoeic.
Nodular BCC
A nodular BCC classically presents with a pearly raised edge with surface telangiectasia. It may develop a central ulcer (rodent ulcer). These cancers tend to be slow growing and bleed occasionally when towelled or when the central scab comes off. Nodular BCCs present commonly on the face (Figure 1).
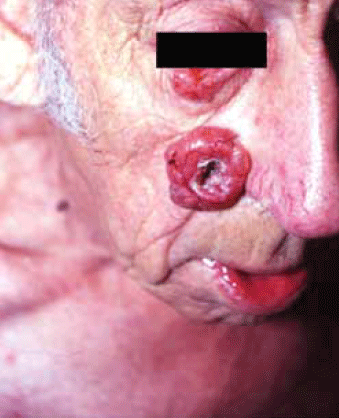
Figure 1. Very large nodular BCC with classic features of a pearly rolled edge, telangiectases and central ulcer. Note also the tumour on the lower eyelid
Superficial BCC
A superficial BCC usually presents as a well defined red patch, typically on the body or limbs (Figure 2). It may have the appearance of psoriasis, eczema or tinea and is sometimes treated as one of these conditions before a correct diagnosis is made. Psoriasis and eczema typically have symmetry and patches tend to come and go with treatment. Be suspicious of a single lesion that does not respond to treatment. Inspect the lesion in good light and with a small amount of magnification (eg. a binocular loupe). Stretching the lesion may reveal a small pearly edge (Figure 3). Biopsy can confirm the diagnosis.
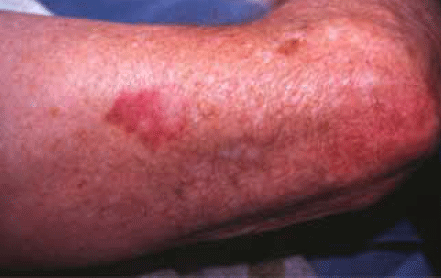
Figure 2. Superficial BCC on the arm
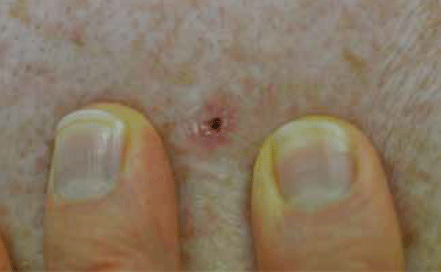
Figure 3. Good light and stretching the skin to better visualise a BCC
Morphoeic BCC
Morphoeic BCCs are the least common of the carcinomas and the most difficult to diagnose. They typically present as a poorly defined scar in a sun damaged area, usually on the face. It is easier to appreciate these lesions if the skin is palpated and stretched. Any unexplained scar should be biopsied. Dermatoscopy, with appropriate training and skill development, may be useful in enhancing the diagnosis of BCC, including pigmented BCC.4
Squamous cell carcinoma
Squamous cell carcinoma is the second most common skin cancer, appearing commonly on chronically sun exposed areas such as the face, ears and hands. The three main clinical presentations are:
- classic
- keratoacanthoma
- Bowen disease (in situ SCC).
Classic SCC
Classic SCCs are a relatively quickly growing keratotic lesion (Figure 4). A very important finding is tenderness of the lesion. Other important findings are induration and failure to clear with treatment (eg. after liquid nitrogen).
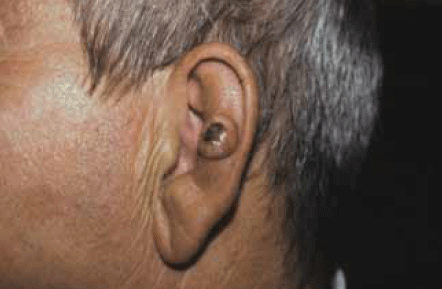
Figure 4. Well defined and well differentiated SCC of the ear
Keratoacanthoma
Keratoacanthoma are rapidly growing lesions, often with a smooth outer dome and a central keratin core (Figure 5). They are often misdiagnosed as a furuncle, however, in keratoacanthoma pus cannot be released.
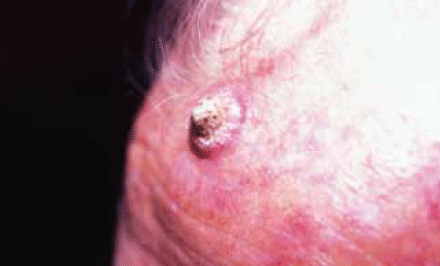
Figure 5. Rapidly growing keratoacanthoma with a central keratin core
Bowen disease
The typical presentation of Bowen disease is a slowly expanding red patch on the body (Figure 6) or limbs, classically appearing on the legs of older women. As with superficial BCC, it may be mistaken for psoriasis or eczema. A biopsy should be taken to confirm the diagnosis.
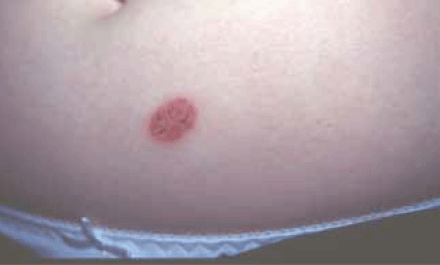
Figure 6. Bowen disease. This slowly enlarging solitary lesion was treated as psoriasis for 4 years
Treatment options for NMSCs
The first step in treatment is diagnosis. Experienced GPs can diagnose most skin cancers on clinical grounds. If a specific benign lesion can be confidently diagnosed it may be left alone. However, if a patient returns for a second time concerned about a particular lesion, it should be biopsied or referred for specialist review.
The gold standard for treatment is excision biopsy.3 Most NMSCs can be removed with a simple ellipse. If a lesion is suspicious of NMSC but is too large or too difficult for simple elliptical excision, it should also be biopsied or referred for specialist review.
The choice of biopsy technique will be determined by the site, size and shape of the lesion. For thin lesions (eg. Bowen disease or superficial BCC), a partial shave biopsy is ideal as it provides a larger surface area of malignant cells (Figure 7–10). Occasionally a small punch biopsy will miss the malignant cells in these lesions (a false negative). For thicker lesions, a punch biopsy is more appropriate so that deeper cells are included in the histology. Punch biopsy tools are very sharp and can penetrate quickly to several millimetres in depth. Be very mindful of this in danger areas such as over the facial nerve or over a major vessel.
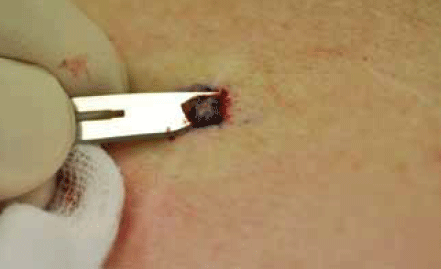
Figure 7. Shave biopsy of a superficial BCC
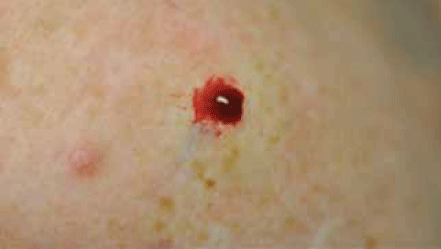
Figure 8. Bleeding after shave biopsy
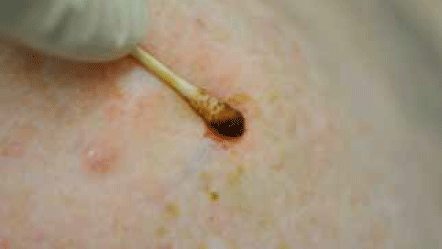
Figure 9. Applying 20% aluminium chloride (eg. 'driclor') to produce haemostasis
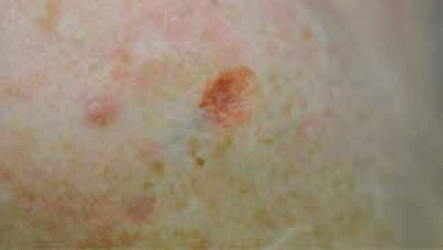
Figure 10. Haemostasis after applying aluminium chloride
For NMSCs not easily treated with elliptical excision, treatment options include curettage and diathermy, liquid nitrogen, imiquimod or fluorouracil, radiotherapy or excision and flap repair/graft. Generally, the only treatments that should be used on the face are excision or radiotherapy.
- Curettage and diathermy may be useful for superficial BCCs and Bowen disease on the body and limbs.
- Liquid nitrogen is useful for superficial lesions on the body and limbs. Treatment requires a 30 second freeze followed by thawing and another 30 second freeze (not a short freeze as used for solar keratoses).
- Imiquimod or fluorouracil: fluorouracil is approved for the treatment of Bowen disease. Imiquimod is approved for the treatment of biopsy proven superficial BCCs where surgery and other treatments cannot be used. Both of these topical agents can produce an intense local inflammatory reaction, which may require a change in the dosing schedule.
- Radiotherapy is usually reserved for patients over 70 years of age. It can have a very high cure rate and is particularly useful for margin control or for treating very large or awkwardly placed lesions. Radiotherapy usually requires 6 weeks of treatment over 5 days per week.
- Excision and flap repair/graft: where possible, lesions should be removed by elliptical excision, even if the ellipse is quite long. By following tension lines, an ellipse usually produces minimal scarring. It is much easier to remove a positive margin following elliptical excision compared to a flap repair. If a skin cancer is poorly defined, it is advisable to have a clear histological margin before flap repair or grafting, even if this means delaying the repair by a day or so. Some areas such as the ala nasi will often require a flap repair or graft.
- Moh's micrographic surgery: a specialised excision technique aimed at improving margin control by viewing microscopically the entire excision margin. Availability is limited, but it is appropriate for use on difficult tumours such as poorly defined, recurrent or anatomically difficult tumours.
- Photodynamic therapy: is used for superficial BCCs and involves the application of a photosensitising cream (eg. methyl aminolevulinate) followed by exposure to an intense light source. Photodynamic therapy requires specific equipment and training.
Areas requiring special consideration
The ears, eyes, nose and lips are potential danger areas. Skin cancers in these areas are often more aggressive and infiltrating and have a higher risk of recurrence and metastasising.3 Skin cancers in these areas need to be excised or referred on for specialist intervention. It is vital to check the patient's histology report. Positive margins, or within 0.5 mm for an SCC, require re-excision (or referral) until clear margins are achieved. Perineural or perivascular invasion conveys a considerably higher risk of recurrent or metastatic disease. These patients should be referred to a specialist for consideration of further surgery or radiotherapy. If the histology report is difficult to interpret, contact the pathologist for clarification.
The leg area has a significant risk of ulceration, regardless of treatment method. Patients at particularly high risk of ulceration are those with previous ulcers, vascular disease or diabetes. The risk of ulceration and infection is increased if there is any tension in the sutures. Compression bandaging, rest and elevation may reduce the risk of complications. Secondary intention healing may be a reasonable option. Radiotherapy should be avoided due to the high risk of ulceration.
Follow up
Excision with clear margins on histology gives about a 96% cure rate.3 Other treatments including liquid nitrogen, curettage and diathermy, imiquimod, fluorouracil and photodynamic therapy have lower cure rates.3 In addition to treatment method, recurrence rates are influenced by doctor proficiency, and the size, type and position of the tumour. No matter what treatment is used, there is always the possibility of tumour recurrence or metastatic disease. For most patients who have had a skin cancer removed, a yearly skin check is reasonable to check the cancer site and the draining nodes, and to assess for new skin cancers. For patients with a high risk SCC, follow up should be every 3 months.
Excision of NMSCs
A simple ellipse is preferred for most skin cancers. A well defined cancer 10 mm or less in size (Figure 11) may be excised with a 2–3 mm margin.3
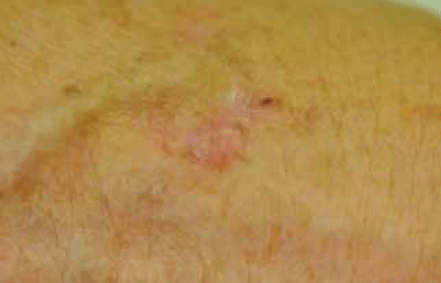
Figure 11. Nodular BCC of the hand
Suggested routine
- Mark out the lesion boundary with a marker pen (Figure 12).
- Measure the lesion diameter and the excision margin (Figure 13).
- Mark out the excision lines along tension lines (Figure 13).
- Consider any underlying structures to be avoided (eg. facial nerve).
- Inject with local anaesthetic and adrenaline (eg. lignocaine 1% with adrenaline) (Figure 14).
- Excise the lesion: depth will depend on the size, type and position of the tumour but most excisions will be to subcutaneous fat.
- Tie off any significant bleeding vessels.
- Suture the wound. If there is significant tension, then subcutaneous sutures are advised. This reduces the risk of wound infection and wound dehiscence, and reduces scarring.
With larger and more poorly defined lesions, include a larger excision margin of 4–5 mm, particularly for micronodular and morphoeic BCCs and poorly differentiated SCCs.3
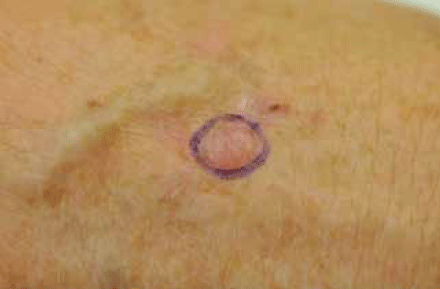
Figure 12. Marking the boundary of the BCC
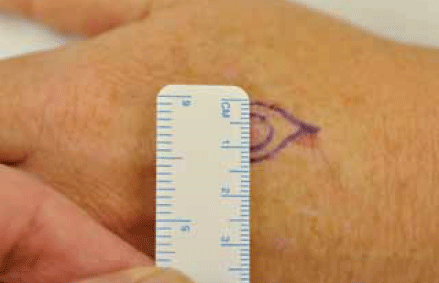
Figure 13. Measuring the lesion and margins
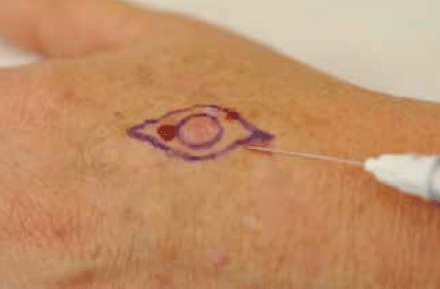
Figure 14. Infiltrating local anaesthetic into the area
Wound infection
Most sutured wounds have uncomplicated healing and routine antibiotics are not recommended. However, situations that significantly increase the risk of wound infection may warrant prophylactic antibiotics. This includes ulcerated lesions, wounds under significant tension, lesions below the knee, flap or graft repairs and wounds in immunocompromised patients.
Prevention of skin cancer
All parents of young children should be made aware of the need for sun protection early in life to significantly reduce the risk of skin cancer. Skin cancer patients can significantly reduce their risk of further skin cancers by minimising sun exposure and by covering up and applying sunscreen daily to the face. Some high risk patients may be offered chemoprevention measures such as acitretin capsules (a vitamin A derivative).
Key important points
- GPs play a pivotal role in the early detection and management of NMSCs.
- Excision is still the gold standard treatment for NMSCs.
- Uncomplicated small tumours are best removed by an elliptical excision with a 3–4 mm margin.
- Other treatment options include liquid nitrogen, radiotherapy, imiquimod and photodynamic therapy.
- Consider referring difficult skin cancers or cancers in danger areas such as the nose, lips, eyes and ears.
- Prophylactic antibiotics are not required except in certain settings such as ulcerated lesions, lesions below the knee, wounds under tension and for immunocompromised patients.
- Opportunistic screening for skin cancer should be a routine part of general practice. Young patients with sun damaged skin require ongoing review.
Conflict of interest: none declared.