Case 1
Ray Peterson
Ray, 49 years of age, is a builder's labourer. He presents with a few skin lesions he wants checked.
Question 1
In terms of the approach to skin cancer diagnosis which of the following is true:
- GPs are not qualified in this area and the patient should be referred to a specialist clinic
- use of a magnifying device worn on the head is just as reliable for diagnosing pigmented skin lesions as dermatoscopy
- the dermatoscope allows better visualisation of the patterns formed by pigment and blood vessels by eliminating reflection from the skin surface
- lesions look the same through all types of dermatoscope
- the 'chaos and clues' algorithm can be applied to both pigmented and nonpigmented skin lesions.
Question 2
You are pleased to have this opportunity to practise using the chaos and clues algorithm with your dermatoscope. Careful full body skin examination reveals a couple of pigmented lesions that you feel warrant closer examination. In the chaos and clues method, all of the following are terms used to describe pigmented structures EXCEPT:
- line
- clod
- pseudopod
- clot
- circle.
Question 3
You examine a pigmented lesion on Ray's left forearm. You observe it to be asymmetrical in structure. An additional feature that would lead you to consider biopsy of this lesion is:
- increased vascularity in a symmetrical pattern
- central black clods
- thick reticular lines
- circumferential radial lines
- yellow colour within the lesion.
Question 4
A lesion behind Ray's right ear appears symmetrical in structure and has a uniform blue-grey colour under the dermatoscope. The next most appropriate step in management is:
- move on to examine the next lesion of interest
- arrange an appointment for biopsy next week
- make a note to re-examine the lesion in 6 months
- apply liquid nitrogen
- refer Ray for dermatology review.
Case 2
Patient skin checks
At your monthly practice meeting, it has been suggested that a more structured approach to skin checks within your patient population might be worthwhile.
Question 5
Which of the following is true regarding skin cancer screening:
- general population screening is currently recommended in Australia by the Cancer Council
- recent results from the SCREEN study showed over 70% reduction in melanoma mortality 5 years after the intervention
- patients who self select for skin checks are mostly those at lower risk of skin cancer
- the current Australian standard is patient self skin check and opportunistic screening
- an essential part of a thorough skin check is medical photography of suspicious lesions.
Question 6
Patient features that would lead you to include them in the 'high risk' category for yearly skin checks include all EXCEPT:
- type 1 skin and age >45 years
- more than 100 naevi
- blue eyes
- past history of melanoma
- red hair.
Question 7
At the meeting, the importance of being able to definitively diagnose benign skin lesions as part of your skin check is recognised. The lesion pictured below is:
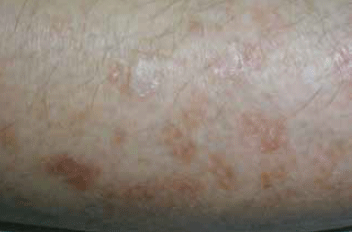
- solar keratosis
- diffuse superficial actinic porokeratosis
- seborrhoeic keratosis
- sebaceous hyperplasia
- benign fibrous papule.
Question 8
When devising your practice approach to suspicious lesions, you need to consider all of the following EXCEPT:
- the limitations of your own surgical skills
- that approximately 20 lesions need to be excised for every one melanoma
- the wait for specialist review of lesions can be long and worrying for patients
- most traumatic lesions that are going to heal will have done so within 1 month
- 50% of skin cancers are squamous cell carcinomas.
Case 3
Alberto Costa
Alberto, 68 years of age, is a long term patient. He attends today for repeat prescriptions. He mentions in passing a skin lesion that has been present for about 4 months and has not resolved, despite a trial of topical corticosteroid suggested by your colleague at his last review. The area is a 7 mm, well defined, solitary red patch on his left forearm.
Question 9
The most appropriate next step in the diagnosis and management of this lesion is:
- to perform a shave or excisional biopsy
- a trial treatment with an antifungal agent
- to advise review of the lesion in 6 months
- to apply liquid nitrogen to the area
- to refer for dermatology assessment.
Question 10
You decide to perform a biopsy of the lesion. In regards to this diagnostic technique, which of the following is true:
- punch biopsy is always the most accurate technique for diagnosis of malignant skin lesions
- 20% aluminium chloride can assist in achieving haemostasis following a shave biopsy
- elliptical excision with 4 mm margins is appropriate for most well defined, nonmelanoma skin cancers
- punch biopsy tools will not penetrate deeply enough to risk damage to surrounding nerves or vessels
- shave biopsy is the most appropriate technique for thickened skin lesions.
Question 11
Alberto's shave biopsy result confirms a superficial BCC and you agree to go on to perform an excision the following week. All of the following steps are appropriate for this procedure EXCEPT:
- mark the boundary of the lesion
- measure the diameter of the lesion and the excision margin
- inject the area with local anaesthetic with adrenaline
- suture the wound, attempting to minimise tension
- prescribe prophylactic antibiotics to avoid complicating infection.
Question 12
If the lesion had been larger, or in a more awkward position, other appropriate options for treatment would have included:
- short freeze liquid nitrogen therapy
- topical fluorouracil
- 3 weeks of radiotherapy for 2 days per week
- curettage and diathermy
- excision and immediate flap repair.
Case 4
Rose Higgs
Rose, 55 years of age, presents with a 4 mm, darkly pigmented lesion on her right forearm. She feels it has been enlarging over the past 6 months. Your dermatoscopic examination reveals a chaotic lesion with blue-grey pigment and you are concerned that it is a melanoma.
Question 13
The next most appropriate step in diagnosis would be to:
- take a punch biopsy from the most suspicious area of the lesion
- perform a wide local excision with margins based on the estimated Breslow thickness
- perform an excisional biopsy with 2 mm margins
- refer for dermatology assessment
- refer for removal by Moh's micrographic surgery.
Question 14
Histopathology indicates an invasive melanoma, Breslow thickness 2 mm. The next most appropriate management step would be:
- early complete lymph node dissection
- wide local excision with margins of 1–2 cm
- referral for specialist assessment and sentinel lymph node biopsy
- arrange staging CT scans and blood tests
- regular monitoring to clinically detect any regional lymph node spread.
Question 15
Rose returns to see you after undergoing complete right axillary node dissection for metastatic disease. In terms of discussing her prognosis, the LEAST important factor would be:
- Breslow thickness
- Clark level
- gender
- tumour mitotic rate
- presence of ulceration.
Question 16
Unfortunately, Rose develops multiple systemic metastases. Her melanoma carries an activating mutation in the BRAF oncogene. The most effective currently known treatment for this type of disease is:
- oral dabrafenib
- surgical excision of metastases
- immunotherapy with ipilimumab
- radiotherapy
- intravenous vemurafenib.