The authors believe that teaching surgical skills to general practice registrars using SBE is a priority because:
- while recent reports indicate an increasing number of conditions requiring surgical intervention in general practice,2 there is simultaneous deskilling of general practitioners in performing minor surgical procedures3
- an increase in procedural work has the potential to attract more junior doctors to the specialty of general practice4 by improving job satisfaction, range of work and patient satisfaction.5
General practitioner supervisors – who play an important role in training general practice registrars to undertake and master practice-based surgical procedures6 – need to ensure that registrars are technically and clinically competent and safe. In order to maintain procedural skills, and to increase enthusiasm for such procedures, simulated models are useful as they allow the opportunity for 'deliberate practise'7 in a stress free environment. It has been observed that medical skills laboratories do lead to improvement in procedural skills compared with standard or no training when assessed by simulator performance and immediately post-training.8,9
There are a range of simulation models available for teaching surgical skills and their advantages and disadvantages have been well described.10 When choosing a teaching model, the 'functional similarity' of the model to its real-life counterpart is crucial.11 In recent years, many simulation models have become available commercially, but most of these are expensive, difficult to access, or are poor replicas of the conditions seen in human patients. Sushruta – the father of plastic surgery – has been stated to use simple simulation models such as fruits and animal hides to teach common surgical procedures.12 In this article we describe three simulation models for teaching surgical skills in general practice following the examples described by Sushruta to teach:12
- the excision of a sebaceous cyst (also known as an epidermal cyst)
- debridement
- escharectomy of chronic wounds.
All of these skills are included in the recommended core list of procedural skills in general practice vocational training.13
The authors have used the model described here for the excision of a sebaceous cyst since 2004 as part of a course run for General Practice Training in Tasmania. The wound debridement models have been used to teach junior doctors at the clinical school in Hobart, Tasmania, and in wound care workshops for other health professionals. We believe these models have the potential to be useful to others involved in such courses, for in-practice teaching and for teaching junior doctors in the hospital setting.
Model 1. Simulated sebaceous/epidermal cyst
The simulated sebaceous/epidermal cyst model proceeded through a series of prototypes before the authors arrived at the final version. The first prototype was created by cutting the tip of a finger from a glove, filling it with toothpaste and tying it with suture material. This was then inserted into the subcutaneous space created in a pig's trotter using the needle attached to the suture material, which was then cut off leaving the finger tip in the subcutaneous space (Figure 1 and 2). In this model, we found that the cyst was too mobile compared to a real-case scenario where the cyst wall is relatively fixed to the overlying skin at the punctum. To address this issue, after the needle was brought through the skin it was then brought back into the subcutaneous space and a knot was tied beneath the surface of the skin before the suture material was cut. This not only stabilised the cyst but also created what looked like a punctum of the cyst when 3/0 black silk was used to make the knot (Figure 3 and 4). We observed that this still did not resemble a real sebaceous cyst, which often remains adhered to its surrounding tissue and requires careful dissection to avoid rupturing the cyst. So a further modification was made by applying a drop of synthetic glue ('Super Glue') between the simulated cyst wall and the surrounding tissue. We found this to be a very effective model for teaching the technique (Figure 5) and a close replica of a real sebaceous cyst (Figure 6).
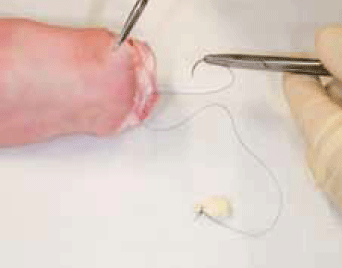
Figure 1. Preparation of cyst
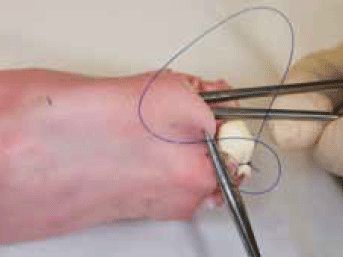
Figure 2. Placement of cyst
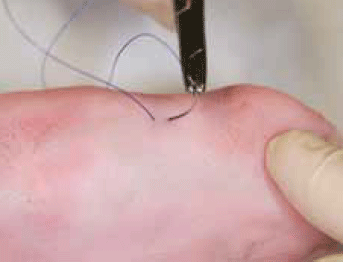
Figure 3. Creation of punctum
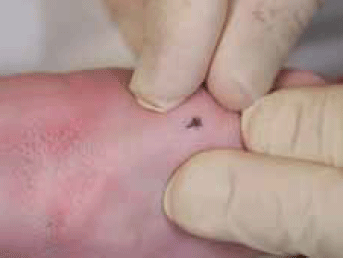
Figure 4. Completed sebaceous cyst model
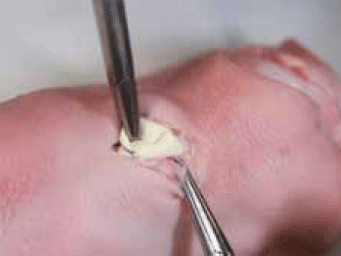
Figure 5. Sebaceous cyst excision on model
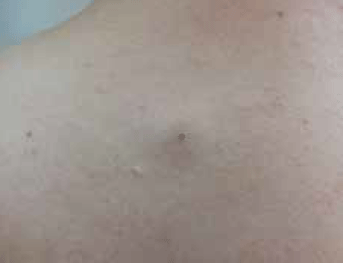
Figure 6. Sebaceous cyst on patient
Preparing the simulation model
- Obtain a fresh (not frozen) pig's trotter from a local butcher
- Cut off a finger tip from a small disposable glove
- Insert about 2–3 mL of toothpaste into the cut-off glove tip
- Tie the glove tip with a 3/0 black silk suture or Prolene™ with curved cutting needle to form a cyst, keeping the needle attached (Figure 1)
- Dissect a tunnel under the skin of the pig's trotter
- Place two drops of Super Glue on the wall of the cyst
- Advance the needle, suture and cyst through the tunnel and bring the needle through the skin (Figure 2)
- Take a small bite of skin with the needle and advance the needle back under the skin and tie it off to form a punctum (or use a black marker-pen dot if using Prolene™, to highlight the punctum) (Figure 3 and 4).
Model 2. Simulated chronic wound for debridement
A simulated chronic wound covered with thick slough, as described by Sinha in 2007,14 can be created on a pig's trotter by excising an area of skin and applying a layer of hydrocolloid paste (eg. ADAPT™, Hollister) to the denuded area (Figure 7). A layer of toothpaste to simulate eutectic mixture local anaesthetic (EMLA) cream can then be applied. This is then covered with a piece of GladWrap™. A small curette is then used to debride the area (Figure 8) after removing the GladWrap™ and wiping away the layer of toothpaste.
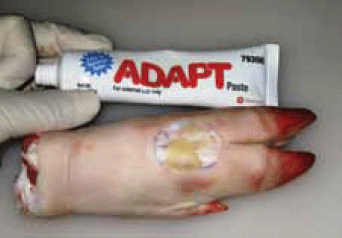
Figure 7. Completed chronic wound model
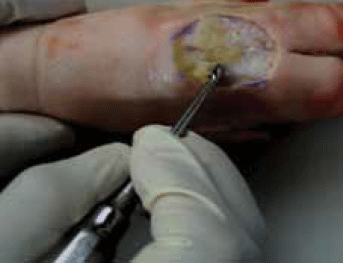
Figure 8. Curettage of sloughy wound
This model simulates the conditions of a chronic wound in a real patient (Figure 9).
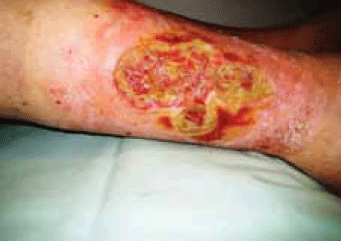
Figure 9. Chronic sloughy wound on patient
Model 3. Simulated wound debridement for escharectomy
An eschar resembling that seen in patients can be created on a on pig's trotter skin by marking out an area of skin then coagulating this skin with a diathermy (Figure 10). If diathermy is not available, the area can be painted with black ink to simulate an eschar. Escharectomy is then performed (Figure 11)15 in a manner similar to that performed on a real patient (Figure 12).
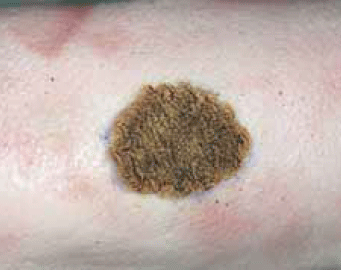
Figure 10. Completed eschar model
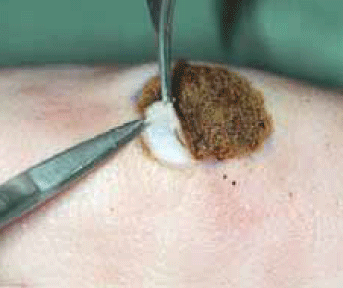
Figure 11. Escharectomy on model
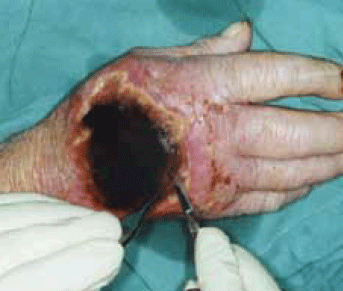
Figure 12. Escarectomy on patient
Discussion
Contemporary teaching methods for procedural skills acquisition in general practice and surgical training programs have been well described.16,17 Important components of these methods include learning in phases or steps, effective feedback,18 transitioning from theory to simulation to clinical settings and combining mechanical skills with communication, professional and ethical skills.19 In order to teach basic surgical skills to junior doctors within the hospital setting, and to trainees in general practice, there is a need to develop inexpensive, safe and authentic simulation models.
Registrars vary in their confidence and competence around surgical procedures and some may benefit from repeated practise with easily available, authentic simulation models. Maran and Glavin9 have emphasised the concept of simulator fidelity and the distinction between engineering fidelity and psychological fidelity, of which the latter is of greater importance.
The three simulation models described here encourage the reproduction of the motor skills or 'engineering fidelity', required in the real patient situation. The models described here replicate the physical characteristics of the respective clinical conditions, as well as the psychological or functional fidelity, ie. the simulated task capturing the skills required in the real task.9
A model of sebaceous cyst made with synthetic material is available commercially (Limbs &Things20). However, it has drawbacks in regards to cost ($69 per item) and fidelity (the model has no punctum and no adherence to surrounding tissue). The sebaceous cyst model described here is easy to prepare, is more life-like and is inexpensive. Written evaluation collected by the authors from general practice registrars using the sebaceous cyst model at skin surgery workshops held by General Practice Training in Tasmania, indicated that the model highly resembled the clinical situation and increased their confidence in the cyst excision. However, the simulation models described here do not exactly replicate the actual clinical situation, especially when complications arise such as with a challenging patient or difficult pathology (eg. a very adherent or multilobulated sebaceous/epidermal cyst). This underlies the importance of providing registrars with adequate supervision (onsite, visiting or at a specialised centre), especially when initially applying these surgical skills to patients.
Conflict of interest: none declared.
Acknowledgement
Thanks to Jo Hanuszewicz from the University of Tasmania for taking many of the clinical photographs, and staff at GPTT for assistance with the development of these models.