What is familial hypercholesterolaemia?
Familial hypercholesterolaemia is an autosomally dominant inherited lipid disorder, which causes premature heart disease and death in affected individuals. Untreated, men have a 50% chance of coronary heart disease (CHD) before the age of 50 years and women a 30% risk by the age of 60 years.2 Atherosclerosis caused by FH starts in childhood and adolescence, highlighting the need to identify cases early and commence preventive measures.3 The frequency of causative mutations in the low density lipoprotein (LDL) receptor gene is estimated to be one in 500 in the general population, and up to one in 100 in certain ethnic groups such as Ashkenazi Jews from South Africa, Christian Lebanese and Dutch Afrikaaners, due to a genetic founder effect.4
In Australia, it is estimated that there are over 45 000 cases of FH, with less than 10% of cases formally diagnosed.5
International data show that of those diagnosed, many are inadequately treated.6 For a general practice of 12 000 patients there may be up to 25 cases.7 Of these cases, the rate of diagnosis and treatment could be as low as 15–25%, and this is particularly so in children.8–10 Familial hypercholesterolaemia can be diagnosed with phenotypic criteria (Table 1) or a DNA test.1
Table 1. Dutch Lipid Clinic Network criteria for making a phenotypic diagnosis of familial hypercholesterolaemia in adults17
| Criteria | Score |
|---|
| Family history |
|---|
First degree relative with known premature coronary and/or vascular disease (men aged <55 years, women aged <60 years)
OR
First degree relative with known LDL-cholesterol above the 95th percentile for age and gender |
1 |
First degree relative with tendinous xanthomata and/or arcus cornealis
OR
Children aged <18 years with LDL-cholesterol above the 95th percentile for age and gender |
2 |
| Clinical history |
|---|
| Patients with premature coronary artery disease (men aged <55 years, women aged <60 years) |
2 |
| Patients with premature cerebral or peripheral vascular disease (men aged <55 years, women aged <60 years) |
1 |
| Physical examination |
|---|
| Tendinous xanthomata |
6 |
| Arcus cornealis before 45 years of age |
4 |
| Investigation |
|---|
| LDL-cholesterol (mmol/L) |
LDL-C ≥8.5 |
8 |
| |
LDL-C 6.5–8.4 |
5 |
| |
LDL-C 5.0–6.4 |
3 |
| |
LDL-C 4.0–4.9 |
1 |
| Diagnosis | Total score |
|---|
| Definite FH |
>8 |
| Probable FH |
6–8 |
| Possible FH |
3–5 |
| Unlikely FH |
<3 |
Screening for familial hypercholesterolaemia
Familial hypercholesterolaemia meets all of the World Health Organization screening criteria as defined by Wilson and Jungner11 (Table 2). Familial hypercholesterolaemia confers a life long risk of CHD and is hence most appropriately screened for in a primary prevention setting in the community.
Table 2. WHO screening criteria and familial hypercholesterolaemia
| Criteria11 | Familial hypercholesterolaemia |
|---|
| The disorder should be an important health issue |
FH affects at least 1:500 individuals and leads to premature CHD. The prevalence may be twofold higher |
| The natural history should be well understood |
Untreated men have 50% chance of coronary heart disease before the age of 50 years, and women 30% before the age 60 years |
| The disorder should be detectable at an early age |
Can be detected in children of affected families before onset of cardiovascular complications |
| Early treatment improves outcome |
Cohort studies and clinical trials show that cholesterol lowering with statins lowers risk of CHD |
| A suitable and accepted test should be available |
Can be readily diagnosed with good clinical history, lipid profile and/or DNA testing |
| The risks of screening should not outweigh the benefits |
The health benefits (eg. prevention of CHD and complications) significantly outweigh the risks (psychosocial and side effects of medication) of screening |
| Screening must be cost effective |
Several international studies demonstrate that cascade screening and treatment of FH is cost effective |
The most cost effective method of screening for FH is cascade screening family members of known 'index cases' of FH12 but at a population level this requires that an efficient method be adopted to detect index cases. Other approaches are therefore required for screening the general population to identify index cases, whose relatives can then be screened. One of the challenges, particularly in today's environment with an epidemic of obesity, is differentiating cases of borderline FH from acquired hypercholesterolaemia due to poor diet and lack of exercise, and this is particularly relevant in children and adolescents.
It is in this context that general practice has a potential advantage in identifying cases of FH. In Australia, 83% of people attend a GP at least once a year,13 and as for other chronic disease and health prevention, this is a great opportunity for screening. Four possible approaches to screening for FH in the general practice setting are outlined in Table 3.
Table 3. Four possible models of screening for familial hypercholesterolaemia in general practice
| Opportunistic screening for family history |
Patients with a positive family history should have their lipid profile measured and be examined for clinical features of FH (I) |
| Opportunistic screening of lipids |
As recommended in the RACGP 'red book,14 those with LDL-C >4.0 or total cholesterol >7.5 should be reviewed for family history and clinical features of FH |
| Systematic searching of general practice electronic records |
Use of search engines to systematically search general practice electronic records and extract patients at higher risk of FH for further review. A possible model has been trialled in the UK15 |
| Universal screening of children |
More controversial but recommended in the US, all children age 9–11 years should have their lipid levels measured.19 Alternatively, screening of all those aged 16 years12 |
Opportunistic screening is very much within the realm of everyday general practice activities.14 Raising the profile of FH means that the GP is more likely to consider the diagnosis when screening for undiagnosed disease.
Systematic searching of general practice electronic records is a more recent approach, which is increasingly being used, notably in managing chronic disease such as diabetes and asthma. Use of data extraction software within the electronic general practice record allows identification of a subset within the total patient population at higher risk of the target disease. Data from the United Kingdom suggests that this may be an effective method of discovering new cases of FH.15
Universal screening of children aged 9–11 years and young people aged 19–21 years is the position taken by expert guidelines in the United States,16 but this is not recommended in The Royal Australian College of General Practitioners Guidelines for preventive activities in general practice ('red book').14 Introduction of universal screening for hypercholesterolaemia recognises the shortfall in systematic detection of index cases of FH in primary and secondary care settings, particularly where diagnosis relies on obtaining an accurate family history of CHD and/or hypercholesterolaemia as a condition of testing for FH. Alternatively, screening of all people aged 16 years is another approach that has been advocated as being cost effective.12
The probability of a person having FH can be determined using the Dutch Lipid Clinic Network Criteria17 (DLNC) which scores people for their clinical history, physical features (eg. tendon xanthomata and corneal arcus), and the plasma level of LDL-cholesterol. General practitioners, or a trained nurse, can therefore apply this scoring system to identify those patients most likely to have FH. Patients with a DLNC score of greater than five have 'probable FH' and may benefit from referral to a specialist lipid clinic. The DLNC should not be used in children, who should be identified as having FH according to LDL-cholesterol thresholds. At a practical level, children should be initially screened using a nonfasting lipid profile, with a repeat fasting test if FH is still suspected. One interesting but untested approach to augmenting the detection of children with FH, is to recommend that all couples planning a pregnancy be tested for hypercholesterolaemia before conception.
It is important to note that before making a phenotypic diagnosis of FH in adults and children, secondary causes of hypercholesterolaemia such as hypothyroidism, nephrosis, cholestasis and use of steroids must be excluded. It should also be noted that if plasma triglycerides are >4 mmol/L, LDL-cholesterol cannot be calculated and must be measured by a direct laboratory method.
The role of specialist lipid clinics in familial hypercholesterolaemia
There are several important reasons for referring patients with probable FH to a specialist lipid clinic:
- Confirmation of the diagnosis. The DLNC score will be confirmed by more extensive clinical and laboratory assessment, including DNA testing for causative mutations in the LDL receptor and other genes. Some patients with classic phenotypic features of FH may still not have a mutation identified (eg. 10% children with definite phenotypic FH),18 reflecting limitations of the current DNA test and multiple mutations causing the disease. However, identification of a specific mutation is important in confirming the diagnosis and in cascade screening
- Cascade screening of family members, either through an identified genetic mutation or phenotypic assessment using the DLNC criteria. The process of cascade screening can be complex (Figure 1), and while general practice may have a role, a centralised service coordinated via a lipid clinic is probably best placed to undertake extended cascade screening of second and third degree relatives. Cascade screening may be a feasible option for parents and children under the care of the same GP
- Cardiovascular disease assessment and disease prevention. A lipid clinic can determine appropriate investigations to detect existing cardiovascular disease, determine the best pharmacological regimen to manage the abnormal lipid profile, and reinforce the importance of a healthy lifestyle
- If there is no specialised lipid clinic available, referral to a cardiologist or endocrinologist with special interest in lipid disorders would be alternative referral pathways.
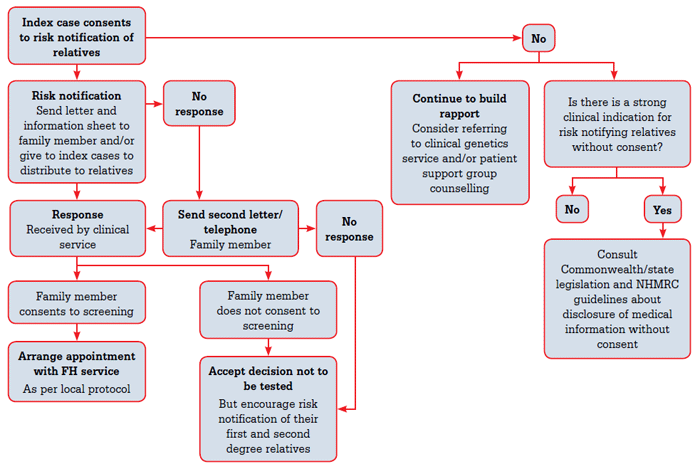
Figure 1. Process of cascade screening family members of index case of familial hypercholesterolaemia
Reprinted with permission from Watts GF, Sullivan DR, Poplawski N, et al. Familial hypercholesterolaemia: A model care for Australasia. Atherosclerosis Supplements 2011;2:221–63
Summary
Familial hypercholesterolaemia is an important but underdiagnosed cause of premature coronary artery disease. General practice could play an important role in identifying families with this condition and, in collaboration with specialist lipid clinics, instituting effective disease prevention. Screening programs in primary care aim to identify index cases and encompass universal, targeted and opportunistic approaches. Index cases should also be vigorously identified in secondary prevention settings (such as cardiac rehabilitation) and once identified, these cases can be integrated into a coordinated, centralised cascade screening program.
Conflict of interest: ICMJE forms have been completed by all authors. Gerard Watts has received funding for consultancy and lectures from Amgen, Genzyme-Sanofi and Roche.