There is some confusion and poor consensus surrounding the classification and naming of many shoulder conditions,3 compounded by evidence indicating that clinical examination and investigations have limited utility.3–6 However, providing practical training to general practitioners about shoulder problems has significant benefit and cost effectiveness.7 Anatomical and medical knowledge combined with clinical acumen and pattern recognition are essential when formulating a diagnosis and management plan for the patient with an injured shoulder. This article provides the clinician with an outline of common acute shoulder injuries, typical presentations, the most valid and reliable clinical tests and basic management and referral considerations.
Classification and natural history
Shoulder injuries may be classified in two ways. The first categorises injuries as either intra- or extra-articular (Table 1), the second classification revolves around the static and the dynamic stabilisers of the shoulder (Table 2). In practice, either classification or a combination may be used. Both classifications include referred and red flag conditions. The clinician must screen for red flag conditions in every patient presenting with shoulder pain or with any shoulder injury (see the article 'Initial assessment of the injured shoulder' in this issue of Australian Family Physician).
Shoulder injuries may present as acute, chronic or acute-onchronic conditions. If the patient is examined very soon after an acute event, movements and palpation anywhere in the region of injury may elicit tenderness and discomfort, making assessment difficult. Progressive biomechanical changes occur after any shoulder injury to compensate for pain or dysfunction. These events alter the natural symmetry and synergy of shoulder movement, compounding the injury and dysfunction. Early intervention, restoration of normal function and appropriate analgesia are therefore important. Around 23% of all new episodes of shoulder pain completely resolve within 1 month and 44% within 3 months of initial onset.8 Approximately 50% of people with acute shoulder pain who are treated conservatively recover within 6 months and approximately 60% recover within 12 months.8,9 The patient's personality traits, coping style and occupational factors may determine if the shoulder pain becomes chronic.2 With the exception of red flag conditions, there is no need of urgent referral for most acute shoulder injuries. The acute phase priority is maintaining near-normal function and biomechanics by providing appropriate analgesia and early physiotherapy involvement.
Table 1. Articular classification of shoulder injuries
- Extra-articular
- rotator cuff lesions
- impingement:
- adhesive capsulitis (stiffness)
- Intra-articular
- instability/labral tears
- osteoarthritis
- Referred pain
- Red flags
|
Table 2. Stabiliser classification of shoulder injuries
- Joint stability (revolves around static stabilisers)
- adhesive capsulitis (stiffness)
- joint instability/labral tear
- Joint control/anatomy (revolves around dynamic stabilisers)
- rotator cuff lesions
- scapulothoracic joint stabilisers
- impingement
- Referred pain
- Red flags
|
Investigations
It is likely that shoulder injuries and shoulder pain presentations are over-investigated. Imaging or further investigation is indicated if there is suspicion of a red flag condition, fracture, dislocation or inflammatory arthropathy. Following the reduction of a shoulder dislocation, imaging is indicated to exclude possible bone or labral damage. In the absence of the above features, the diagnostic utility of imaging is minimal and the results are unlikely to improve management,10–13 and therefore imaging is not discussed in this article.
Special tests
There are multiple special tests for the shoulder, although there is no conclusive evidence for their reliability14 and no clinical test is both reliable and valid for any specific diagnosis.4–6,15 Special tests are often used if the diagnosis remains uncertain or equivocal. The clinician must perform tests with the same method to ensure reliability.
Common presentations to general practice
Refer to the article 'Initial assessment of the injured shoulder' in this issue of Australian Family Physician for a refresher on key history and examination features. This article refers to soft tissue injuries of the shoulder. Red flag conditions, fractures, dislocations, referred conditions and inflammatory arthropathies are beyond the scope of this article. For all shoulder injuries, consider the need for appropriate, regular analgesia to improve comfort and to maintain reasonably normal function and biomechanics.
Impingement syndrome
In impingement syndrome, the subacromial bursa and supraspinatus tendon become compressed between the humeral head, the acromion and the coraco-acromial ligament. This results in pain with forward elevation of the arm and narrowing of the subacromial space (Figure 1). Causes are functional, anatomical or a combination of both. Functional impingement occurs when there is poor control of the shoulder stabilisers and this allows cephalad slippage of the humoral head compressing the subacromial space. It may also result from overuse of the shoulder or an injury to the shoulder resulting in altered biomechanics and poor stabiliser control. Anatomical impingement occurs secondary to arthritis or hypertrophic changes of the acromion, resulting in a narrowed subacromial space. Either cause may result in subacromial bursitis and/or rotator cuff lesions,16,17although these terms are often used interchangeably to mean the same thing.3
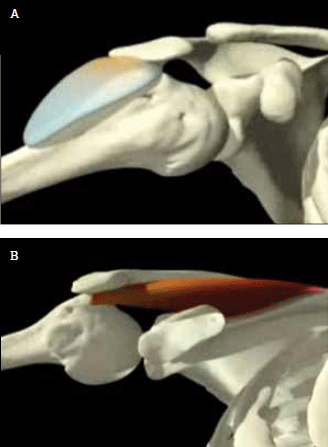
Figure 1. A) Impingement of the subacromial bursa between the humeral head and acromion; B) and supraspinatus between the humeral head, acromion and coraco-acromial ligament (not shown) Reproduced with permission Primal Pictures. Available at www.primalpictures.com
Presentation
The main reason for presentation is pain, especially with overhead movements of the arm. Sometimes lying on the affected shoulder at night may cause pain due to cephalad slippage of the humeral head with lateral compression.
Clinical assessment
The most reliable special test for subacromial impingement is the Hawkins test (Figure 2). To ensure standardisation of this test the humerus is elevated to 90 degrees and positioned 30 degrees anteriorly, this ensures the humerus is in the line of the scapula. The elbow is flexed to 90 degrees and the glenohumeral joint internally rotated. In the figure, the clinician's right arm acts as a fulcrum for internal rotation only: this is a minor variation on the original description by Hawkins and Schutte.18 This test has a sensitivity of 91–92% and specificity of 25–43%.5,15 Therefore a negative test suggests that impingement is unlikely (although still possible) and a positive test is meaningless. Pain constitutes a positive test.

Figure 2. The Hawkins test
Referral and management
The initial management for impingement is to address the underlying cause. Physiotherapy assessment and intervention is indicated in most cases. Surgical management is controversial and is unlikely to be of benefit, especially if the cause is secondary to a functional problem. Arthroscopic acromioplasty provides no additional benefit over a structured and supervised exercise program for subjective pain outcome or cost effectiveness when measured after 2 years.19
Anterior shoulder instability
Anterior shoulder instability occurs secondary to acute or chronic stretching of the anterior shoulder capsule, resulting in instability and decreased support over the anterior aspect of the glenohumeral joint. It is seen following anterior shoulder dislocation and subluxation. A more common cause is repetitive and progressive stress on the anterior shoulder capsule from loading and stretching beyond functional range, as performed by swimmers and baseball/softball pitchers. It is also frequently seen in resistance trainers, using an incorrect technique and/or attempting to lift too heavy weights especially in the supine or semi-recumbent position. Dropping the elbow below shoulder height while controlling a load places unnecessarily large forces on the anterior shoulder capsule.
Presentation
Anterior shoulder instability can be difficult to diagnose as nonspecific signs and symptoms are common, including shoulder ache and occasional clicking or clunking. Pain may wake the patient at night when lying on the affected shoulder due to anterior slippage of the humoral head. If the condition has been longstanding or the laxity is pronounced, the patient may complain of hand or arm weakness, tingling or numbness from proximal nerve traction.
Clinical assessment
A focused history will provide the clinician with the most valuable information as the examination is often unremarkable and imaging usually is unhelpful.4 The Anterior release test (Figure 3) has a sensitivity of 91.9%, specificity of 88.9%, positive predictive value of 87.1% and negative predictive value of 93%.20
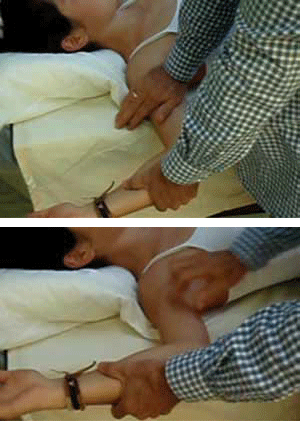
Figure 3. The Anterior release test for anterior shoulder instability. The patient is supine, the arm is abducted and externally rotated, the examiner's hand closest to the patient applies a downward force over or close to the humeral head in an attempt to relocate and secure it within the glenoid. Once a firm pressure is applied the patient's arm is externally rotated further at which stage the humeral head is suddenly released. The patient may experience pain, apprehension or a combination during the release phase of the test. Extreme caution is required because if the shoulder is very unstable, dislocation may occur during the release phase
Referral and management
Imaging is indicated for all traumatic shoulder dislocations; ideally this should be performed pre- and post-reduction of the dislocation, initially plain X-rays are sufficient, although magnetic resonance imaging (MRI) and/or ultrasound may be indicated. There is a 93% chance of re-dislocation following a first time dislocation, especially in the younger age group, with the risk increasing with higher levels of physical activity or contact sport.21,22 All first time dislocators should therefore be referred for physiotherapy and orthopaedic assessment. There is no data to guide management of instability from chronic overuse. Logically identifying and correcting the predisposing factors is a reasonable approach. Referral to a physiotherapist may aid identification of provoking factors, correction of the underlying cause and prescription of an appropriate rehabilitation program. If severe instability does not improve an orthopaedic opinion may be indicated.
Rotator cuff tears
Rotator cuff tears are common and increase proportionally with age. More than 50% of those aged over 50 years have either symptomatic or asymptomatic tears.11,23,24 Tears of the rotator cuff muscles may occur as a result of direct trauma or progressive wear and tear. The tear may be partial or full thickness. Pain and dysfunction does not appear to correlate with the degree of tear. There is often progression from tendinopathy to tear, especially if the tendinopathy is not addressed early.
Presentation
Tears present as a spectrum. The patient may be asymptomatic and the tear found incidentally following imaging. The patient may present with features similar to anterior shoulder instability, given that a tear of the dynamic stabilisers of the shoulder may result in loss of congruency of the humeral head within the glenoid. The patient may complain of pain and/or weakness when attempting to elevate the arm. There may be night pain when lying on the affected shoulder and if longstanding there may also be features of numbness and tingling in the affected arm or hand. Patients with a rotator cuff tear may recruit other muscles to perform the task of the torn muscle, thereby having normal or near-normal shoulder function.
Clinical assessment
Although it is possible to activate any one of the rotator cuff muscles, it is extremely difficult to isolate any one for testing.25 There are two clinical tests that are useful in helping to diagnose an acute rotator cuff tear. These are less useful if the tear is chronic because compensatory recruitment of other muscles is likely to occur.
The first test is the Empty can test (Figure 4). For detecting a supraspinatus tear the test has a sensitivity of 18.7% and a specificity of 100%,4 this means if the test is positive it is highly likely that the patient has a tear.
The second test is the Drop arm test. In this test the patient's arm is abducted to at least 90 degrees, they are then asked to lower the arm slowly and control the decent. Inability to perform this task slowly and with control constitutes a positive test and has a positive predictive value of 100% and a sensitivity of 10%.26 Therefore inability to perform the test is highly suggestive of a tear, although with a negative test the patient may still have a tear.

Figure 4. The Empty can test for supraspinatus tear. The arm is elevated to 90 degrees and angled forward 30 degrees to place the humerus into the line of the scapula. The shoulder is internally rotated by pointing the thumb down to the ground. The clinician then applies a downward force as the patient attempts to resist. Pain and/or weakness are deemed a positive test
Referral and management
In all cases early referral to a physiotherapist is appropriate. If the tear is acute, in the younger age group and affecting comfort and/ or function, imaging may be of benefit.10–13 If the tear is the result of sudden trauma, occurs in the younger age group and is impacting on comfort and/or function, orthopaedic opinion may be indicated. In other settings imaging and surgical management are of debatable benefit.
Acromioclavicular joint sprain and osteoarthritis
There are varying degrees of severity of acromioclavicular joint (ACJ) sprain.27 In the more common, less severe types there is no gross displacement of the joint. Complete joint disruption is less common and needs orthopaedic assessment. Acromioclavicular joint sprain typically results from a fall or impact onto the shoulder tip, resulting in stretching or tearing of the ACJ capsule and ligaments. A prior ACJ sprain will eventually result in osteoarthritis and chronic pain or discomfort.
Presentation
If the presentation is acute, the patient will remember the mechanism of injury. Often the painful region is poorly localised and they may present with diffuse shoulder pain. Sleeping on the affected side often disturbs sleep and across body movements with the arm of the affected shoulder may cause pain. The patient presenting with the osteoarthritic joint may not recall the injury and describe increasing pain over time of a diffuse nature. When the ACJ is placed under repetitive stress (eg. bodybuilders and weightlifters), damage to the joint may occur resulting in pain and instability.
Clinical assessment
Point tenderness over the ACJ is very typical with either an ACJ sprain or osteoarthritis. Performing the Active compression (O'Brien) test (Figure 5) is helpful in localising the source of pain. This test has a sensitivity of 16–100% and specificity of 90–96.6%,28–30 meaning a positive test is highly suggestive of localised ACJ pathology, most often a sprain or osteoarthritis.

Figure 5. The Active compression (O'Brien) test for ACJ pathology. Testing in internal and external rotation. The clinician stands behind or to the affected side of the patient. The affected arm is flexed to 90 degrees with the elbow fully extended, the arm is then adducted about 15 degrees medial to the sagittal plane. The arm is internally rotated so that the thumb points to the floor, the patient then resists the downward force applied by the clinician. Maintaining the arm in the same position, the patient then supinates the arm so as the palm is facing upward and resisting another downward force. The test is positive and diagnostic of ACJ pathology if pain is elicited over the ACJ or on top of the shoulder in the thumb down position and reduced or eliminated in the palm up position
Referral and management
Most cases of ACJ pathology presenting to the clinician are easily diagnosed and managed. Involving a physiotherapist ensures that significant biomechanical changes are minimised as a result of inappropriate use of the affected shoulder. Simple acute sprains often settle well with conservative management. Supportive shoulder strapping provides ACJ stability, reduces pain and is easy to apply (Figure 6a, b). Tape may stretch by up to 40% after application, therefore it needs to be applied with significant tension. Hypoallergenic tape under the strapping tape (Figure 6a), allows the strapping to be left in place for up to 4–5 days. (Strapping may become wet, provided it is dried well afterward.)
Acromioclavicular joint sprains not responding to appropriate conservative management may benefit from a corticosteroid injected into the ACJ using an aseptic technique.9 This is a relatively safe procedure with minimal side effects.3,8
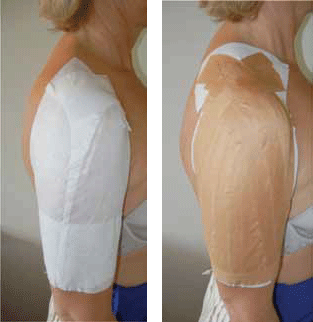
Figure 6. A) Application of hypoallergenic tape before application of strapping tape; B) For support of ACJ sprain. The strapping tape must be applied distal to proximal with significant traction to support and elevate the arm and therefore offload the ACJ
Key points
- Shoulder injury presentations are common in the general practice setting and most can be effectively managed at this level.
- A systematic focused approach to history and examination are important to determine a diagnosis and formulate an appropriate management plan.
- With the exception of red flag conditions, fractures, dislocations and inflammatory arthropathies investigations are not indicated and will not alter management.
- Maintaining near-normal function and biomechanics is essential following shoulder injuries and the prescription of appropriate analgesia and early physiotherapy involvement will substantially contribute to achieving these goals.
Conflict of interest: none declared.