The menisci of the knee have several important roles:
- shock absorption and distributing load throughout the joint
- increasing stability
- providing nutrition for articular cartilage
- limiting extreme flexion and extension
- controlling the movements of the knee joint.1,2
The medial meniscus is 'C' shaped whereas the lateral is a shorter incomplete circle with closer spaced 'horns'. The medial meniscus is more frequently torn, partly because of this different shape but also because of its attachment to the medial collateral ligament, whereas the lateral is pulled out of the way of compression between femur and tibia by politeus. Superior and inferior branches of the medial and lateral geniculate arteries supply the peripheral third of the menisci via the perimeniscal capillary plexus.3,4
Epidemiology, aetiology and pathophysiology
Meniscal tears occur due to a shear force between the femur and tibia. In younger patients, this is typically a twisting force on a weightloaded flexed knee. These are often 'bucket-handle tears', in which there is a vertical or oblique tear in the posterior horn running toward the anterior horn,5 forming a loose section which remains attached anteriorly and posteriorly.1 In older patients, tears are generally due to degeneration associated with ageing and tend to be horizontal tears. The difference in tear type between these populations is explained by the three-dimensional fibrous structure of the meniscus: horizontal delamination occurs in degenerative injuries, while the fibrous structure is ruptured in a vertical fashion in younger patients. Meniscal tear incidence may be as high as six per 1000 population6 with a 2.5 to 4 times male predominance. Age of injury peaks at 20–29 years.7 Partial meniscectomy (removal of the torn section) is one of the most commonly performed orthopaedic surgical procedures.8
History and examination
Meniscal tears often occur in young patients who have suffered a twisting injury to the knee. Tears present as severe pain, swelling, and possibly catching, clicking, difficulty on deep knee bending and locking of the knee in partial flexion.
The typical meniscal pain profile comprises well localised joint-line pain (with medial pain generally being indicative of a medial tear and vice-versa). Meniscal pain occurs during torsional, weight bearing knee movements (classically pivoting on the knee while walking) as a sharp stab lasting several seconds, often followed by a dull ache for several hours. Pain may wake the patient from sleep as the tender medial aspect of the knee strikes the other side as the patient rolls over in bed. There is no resting pain.
Locking presents in two ways. Most commonly it is impossible to fully extend the knee; more accurately described as stiffness (termed 'pseudo locking') due either to a small effusion (requiring increased force to bend the tense joint capsule) or to pain inhibition as the femoral condyle compresses the torn meniscus. True locking is less common, and suggests a bucket-handle tear, with the torn fragment preventing full extension. There is a history of sudden inability to fully extend the knee, with a rotational flexion/extension 'trick' required to regain full extension. Weakness, grinding, instability or giving way rarely result from meniscal pathology.
On examination, there may be joint effusion, joint line tenderness, and the joint is held in a flexed position.1 in late presentations, there may be significant quadriceps wasting. McMurray (Figure 1) and Apley tests (Figure 2) are often positive, although these are specific but not sensitive – specificity being 57–98% and 80–99%, and sensitivity being 10–66% and 16–58% respectively.2,9 The most useful clinical test for meniscal injury is the Thessaly test, which is demonstrated in Figure 3. Although rarely taught and poorly utilised, recent validation demonstrated a sensitivity of 90%, and specificity of 98% in detecting meniscal injury.10
Diagnosis
If clinically suspicious of meniscal injury, a trial of conservative measures may be considered or confirmation with magnetic resonance imaging (MRI). Unfortunately, general practitioners cannot currently order Medicare funded MRI, although this may change with The Royal Australian College of General Practitioners recent submission to the Australian Government Department of Health and Ageing. 11 Plain radiography is only useful to exclude differentials and computed tomography (CT) is markedly inferior to MRI for meniscal imaging.12 Magnetic resonance imaging is the gold standard, first choice for investigation of suspected meniscal tears.2,13–16
Sagittal peripheral meniscal images demonstrate the normal anatomical 'bow-tie configuration' (the central meniscal body with the anterior and posterior horns as well circumscribed triangles. On MRI, meniscal tears are evident as a linear signal intensity that extends through the meniscal substance to a free edge17 (Figure 4). Tears are typically vertical in young patients and horizontal in the elderly (Figure 5). Magnetic resonance imaging can also be effectively used to estimate the vascular zone classification (see Treatment) of tears.18 This is useful for the orthopaedic surgeon to predict meniscal repairability, assisting informed discussion with patients and scheduling appropriate operating theatre time.18 It is essential to remember that just because a tear can be seen on MRI, this does not mandate surgery.
Indications for specialist referral
The absolute indication for specialist referral is the locked knee – loss of joint function necessitates surgical intervention. Referral is also indicated if the diagnosis is uncertain for review and to access MRI. In older patients, referral is appropriate if conservative management fails to improve symptoms. As the risk of osteoarthritis is increased if meniscal structures are not optimally functional,7 it may also be appropriate to refer all young patients for opinion if symptoms do not rapidly improve.
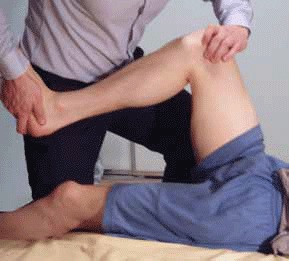
Figure 1. McMurray test: The patient lies supine on the bed with the hip and knee both flexed. With the foot as close to the hip as possible, the clinician holds the knee joint (with fingers along the joint line) with one hand, and the other hand rotates the tibia internally and externally while extending and flexing the knee. If the test is positive (suggesting a meniscal tear), the patient will feel pain and the clinician will feel and/or hear meniscal movement when the meniscus is compressed between the tibia and femur 32

Figure 2. Apley test (grinding) test: The patient lies prone, with their knee flexed to 90 degrees and their hip extended. The clinician applies axial pressure to the foot and rotates the tibia internally and externally. Pain and/or clicking on compression suggest a meniscal lesion 1,32

Figure 3. Thessaly test: The clinician holds the patient's outstretched hands for support, while the patient stands flat-footed with their knee flexed to 20 degrees and rotates their body and knee three times, internally and externally. The test is positive if symptoms are reproduced on rotation 10
Treatment
Nonoperative treatments are an important part of the management of all patients, regardless of whether surgery is being considered. Immediate conservative measures include the RICE regimen:
- Rest (with weight bearing as tolerated or with crutches)
- Ice
- Compression bandaging
- Elevation of the affected limb to minimise acute swelling and inflammation.
Longer term measures include activity modification, nonsteroidal antiinflammatory drugs (NSAIDs) and physiotherapy.4,19–21 Nonsteroidal anti-inflammatory drugs are often recommended for 8–12 weeks,20 although paracetamol can be considered if NSAIDs are contraindicated or poorly tolerated.22 Where available, intensive physiotherapy is very useful and should include range of motion, proprioceptive work and muscle strengthening exercises. Physiotherapy at two visits per week for at least 8 weeks is recommended.20 There is little evidence for strapping of meniscal injuries and this is not currently recommended.
Nonoperative treatments are often successful in patients with certain types of tear – patients who have no loss of joint function, suffer minimal pain or swelling and are willing to reduce their activities – temporarily or in the long term. A recent study demonstrated 46% of patients with degenerative meniscal tears elected not to have surgery after 4 weeks of nonoperative treatment, and their functional improvement matched patients in the operative group.21 Another study of degenerative tears demonstrated that supervised exercise caused the same reduction in knee pain and the same increase in function and satisfaction as partial meniscectomy plus exercise.23 As degenerative tears are more common in elderly patients, this group is more likely to respond to conservative treatment. The degenerative aetiology and reduced vascularisation secondary to ageing also means that meniscal tears in the elderly population are less likely to be amenable to surgical management;7 only about 6% of patients over 40 years of age have operable lesions.24 To prevent re-injury of the meniscus, activity modification is important – for example, ceasing sports such as soccer or netball. Patients are often aware of movements that aggravate mensical pain, but should also be educated to avoid twisting on a weight bearing, flexed knee.
Surgical treatment is usually reserved for younger patients with a vertical longitudinal tear within the vascularised outer third of the meniscus. This is termed the 'red-red zone' (denoting area of vascularity).2,4 repair of the 'red-white zone' (watershed area between vascular and avascular meniscus) is controversial25 with many different surgical techniques.26 tears in the 'white-white zone' (avascular zone) are rarely repaired – rather the damaged segment is resected (meniscectomy). Damaged avascular meniscus must be removed.27 However, meniscectomy causes long term osteoarthritis,28 so is only performed when the patient suffers joint locking or mensical pain that is refractory to conservative management. For patients requiring meniscectomy, meniscal autograft has been utilised with good outcomes,29–31 but is only performed in specialist centres. Research is currently investigating the possibility of implantation of collagen, allogenic and xenogenic cells, embryonic and adult stem cells, or scaffolds derived from polymers, hydrogels, tissues and extracellular matrix,7 and action of biological stimuli (eg. growth factors) on meniscus tissue is being investigated.2 These are currently only being trialled in younger patients7 and the routine use of most of these technologies is some time away.
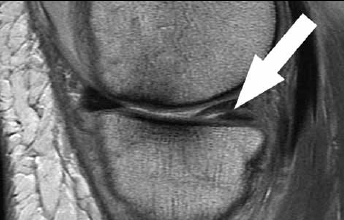
Figure 4. Proton weighted sagittal image demonstrates an example of a posterior horn medial meniscal horizontal tear (white arrow). The anterior horn of the medial meniscus demonstrates half of the normal anatomic 'bow-tie configuration'. Note: the cartilage deficit more anteriorly on the medial femoral condyle and altered subchondral cortical bone interface
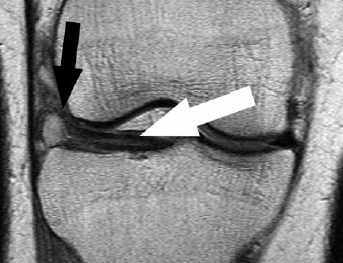
Figure 5. Coronal proton weighted MRI of horizontal tear of lateral meniscus (white arrow) with complicating ganglion (black arrow) at the lateral margin of the meniscus
Key points
- Meniscal injury is common, and the medial meniscus is more frequently injured.
- Younger and elderly patients typically sustain different types of tears.
- Optimal diagnosis and management is essential to prevent long term sequelae.
- The Thessaly test is the most sensitive and specific clinical test to diagnose meniscal injury.
- Magnetic resonance imaging is first line for investigating potential meniscal lesions, but should not replace thorough clinical history and examination.
- Conservative management is important in all patients with acute rest, intensive rehabilitation with physiotherapy and modification of activity. Referral to an orthopaedic surgeon is important if the diagnosis is uncertain or there is minimal improvement at clinical review.
Conflict of interest: none declared.