Current interventions to increase performance of preventive services fail to combine the necessary elements of educating patients about health risks and how to maintain health; these elements include informing patients about their current preventive health status and providing a means for them to act readily on the information and advice given.22,23 This failure results in only small increases in the uptake of preventive services.24,25
In earlier work, we developed a patient prevention summary and reminder sheet (PPSRS), which was given to patients when they arrived for consultations. The sheet was generated by the practice computer system comparing data in the patient’s electronic clinical record with recommendations in the Royal Australian College of General Practitioners (RACGP) Guidelines for preventive activities in general practice,26 for a range of preventive activities indicated by the patient’s age, gender and recorded medical history. The sheet informed, educated and advised patients about their status for indicated preventive activities and encouraged them to discuss outstanding activities with the GP in the imminent consultation. An example sheet has been published.27 The positive response from patients in our pilot study encouraged us to conduct a preliminary study to assess whether ongoing generation and printing of PPSRSs is acceptable to patients and feasible in busy routine general practice.
Methods
Setting
Three general practices with a total of 14 GPs serving areas of differing socioeconomic status were purposively recruited to the study.
Inclusion and exclusion criteria for patients
The inclusion criterion was that patients had to be 18 years or older. The exclusion criterion was if the receptionist judged that the patient seemed too unwell to be given a PPSRS.
Intervention
We enhanced the Doctors’ Control Panel (DCP) software28 to automatically generate PPSRSs on patients’ arrival for consultations at their general practice. The enhanced DCP software was installed on the computer systems of the participating practices, and GPs, practice nurses and practice staff were instructed in its use. The first 5 weeks of the 13-week intervention period was a ‘run in’ phase. In the first week, a PPSRS was printed for only every tenth eligible patient. In each subsequent week, the number of eligible patients for whom sheets were printed was increased so that by the beginning of the sixth week a sheet was being printed for every eligible patient who had not yet received one. Only one sheet was printed for each patient during the trial. Patient were advised to discuss the contents of the PPSRS with their GP and to keep the sheet for reference. In the ninth week, in response to feedback from the practices, we introduced user controls (Figure 1) that allowed the practices to suppress printing of PPSRSs in situations that they could specify. The controls also allowed them to restrict the overall number of sheets being printed.
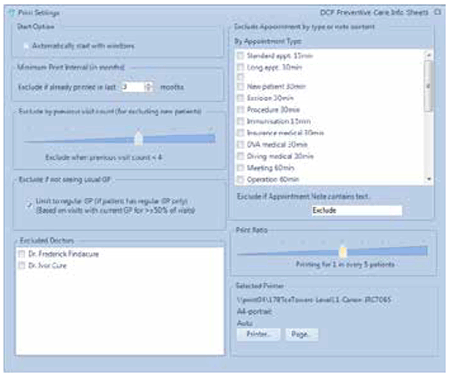
Figure 1. User controls developed during the trial
Every thirtieth eligible patient who arrived for an appointment during the 13-week intervention period and who received a PPSRS also received information about the trial and an anonymous self-completion questionnaire. They were asked to complete the questionnaire after their consultation and post it in a box at the reception desk.
Outcome measures
The acceptability of the intervention to patients was assessed through the questionnaire completed by the sub-sample of all patients who received a PPSRS. The acceptability to practices of the intervention and its sustainability were assessed by the number of PPSRSs printed during and after the intervention period, and the number of practices that continued printing PPSRSs after the end of the intervention period.
Analysis of data
Data were analysed by descriptive statistics and by Fisher’s exact test to examine independent associations between patient characteristics and responses to the patient survey.
Ethics approval
Ethics approval (reference number H-300-2011) was granted by the Human Research Ethics Committee of the University of Adelaide.
Results
Acceptability of the intervention to patients
A total of 130 patient survey forms were printed during the intervention period; 121 (93%) forms were returned. Characteristics of respondents were:
- 62% female
- interquartile age range 30–52 years
- highest level of education: year 10: 28%, year 11 or 12: 31%, tertiary: 41%
- main source of income: wages or salary: 62%, government pension, benefit or allowance: 27%, ‘other’: 11%.
Sixty-two percent of respondents reported that the sheet had made their visit more useful, and 89% reported that they would like to continue receiving the sheets at least occasionally in the future (Table 1).
Table 1. Responses to patient survey
| How easy was it for you to understand the purpose of the prevention summary sheet? n = 117 |
Very easy
85 (73%) |
Easy
29 (25%) |
Neither easy nor difficult
3 (2%) |
Difficult
0 (0%) |
Very difficult
0 (0%) |
Don’t know
0 (0%) |
| How clear were the instructions about what to do with the sheet? n = 118 |
Very unclear 0 (0%) |
Unclear
1 (1%) |
Neither clear nor unclear
2 (2%) |
Clear
37 (31%) |
Very clear
78 (66%) |
|
| Did you discuss the information on the prevention summary and reminder sheet with your doctor in your consultation? n = 104 |
Yes
75 (72%) |
No
29 (28%) |
Don’t know
0 (0%) |
|
|
|
| How did receiving the sheet affect the usefulness to you of your visit here today? n = 114 |
Made my visit much more useful
28 (27%) |
Made my visit a little more useful
36 (35%) |
Made no difference
38 (36%) |
Made my visit a little less useful
0 (0%) |
Made my visit much less useful
0 (0%) |
Don’t know
2 (2%) |
| How often would you like to receive prevention summary sheets like this in the future? n = 106 |
Every time
15 (14%) |
Most times
15 (14%) |
Occasionally 65 (61%) |
Never
9 (9%) |
Don’t know
2 (2%) |
|
Responses to the survey questions varied little with the characteristics of the respondents. Age and main source of income were the only patient characteristics associated with differences greater than 20% absolute (Table 2). The sheets enhanced the usefulness of the consultation for younger and older patients; nearly 9 in 10 of those aged over 68 years reported that the PPSRS had made their consultation more useful. Those in the 32–39 years age bracket were the least likely to indicate they had discussed the sheets in the consultation (50%) or report that the sheet had made their GP visit more useful (41%). Respondents whose main source of income was government or ‘other’ were more likely to report that they had found the sheets useful than were those whose income was from wages or salary. None of the associations between the characteristics of patients and their responses to the survey reached an independent statistical level of significance (P = 0.05).
Table 2. Patient survey questions in which responses varied by more than 20% for various characteristics of patients
| Patient age (years) |
|---|
| <31 | 32–39 | 40–52 | 53–67 | >67 |
|---|
| Discussed PPSRS in consultation |
13/21 (62%) |
9/18 (50%) |
10/13 (77%) |
16/18 (89%) |
19/19 (100%) |
| PPSRS made visit more useful |
14/22 (64%) |
7/17 (41%) |
10/15 (67%) |
12/19 (63%) |
14/16 (88%) |
| Main source of income |
|---|
| | Wages or salary (n) | Government benefit, pension or allowance (n) | Other (n) |
|---|
| PPSRS made visit more useful |
36/67 (54%) |
22/29 (76%) |
5/6 (83%) |
Acceptability to practices and sustainability
At the end of the 13-week intervention period, 2237 sheets had been printed and all participating practices chose voluntarily to continue printing them thereafter (Figure 2). During the subsequent 39 weeks, another 6645 sheets were printed, so that 52 weeks from the start of the trial, a total of 8882 PPSRSs had been printed. The rate of printing of the PPSRSs fell from the ninth week to the twenty-third week as the practices implemented the new user controls to suppress printing of sheets in circumstances that they could specify, such as new patient, patient not seeing his or her usual GP in the practice, or special purpose appointments, including wound dressing, immunisation only, prescription only or test results only. From the twenty-third week, the rate of printing of the sheets became relatively stable for the remainder of the follow-up period.
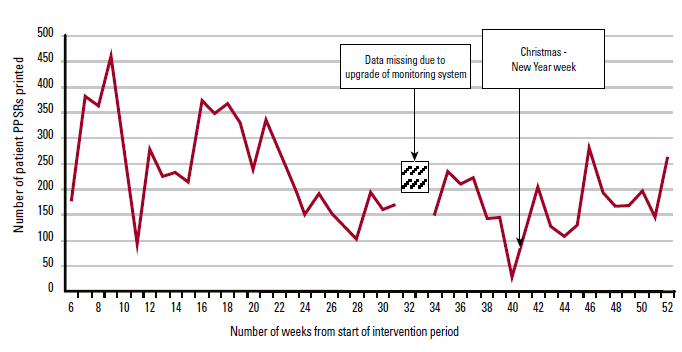
Figure 2. Numbers of PPSRS printed during each week of the trial
Discussion
Our study found that automated generation and printing of PPSRs is feasible: patients valued the intervention and practices have readily adopted it, continuing to print the PPSRSs at a steady rate 1 year after the start of the trial.
Speaking a language other than English at home was not a barrier to understanding the purpose of the sheet or the instructions for what to do with it. It is not surprising that older people were most likely to report that they had discussed the sheet in the consultation and that the sheet had made their visit more useful; however, we do not know why patients aged 32–39 years were less likely than younger patients to report doing so. We speculate that people younger than 32 years may feel less experienced, more dependent and more receptive to medical advice than people aged 32–39 years. Similarly, dependence and a self-perceived lack of mastery or competence may explain why people whose main income was from government benefits, pensions, allowances or ‘other’ non-salary or wage income were more likely to report that the sheet had made their visit more useful, and were much more likely to want to receive the sheets in the future.
The large number of PPSRSs printed since the end of the intervention period across all participating practices testifies to the sustainability of the intervention and to its acceptability to practices. The introduction of the user controls has allowed practices to customise the DCP software to their specific contexts – we believe this has enhanced sustainability.
Our intervention is the first to present personalised, targeted, current preventive education, information and advice to patients when they were about to see their GP. This intervention encouraged and enabled patients to address any outstanding preventive services immediately, with minimal time, effort and cost. It is an improvement on previous strategies such as waiting room posters and leaflets, which do not present information or advice specific to the patient, and on sending letters or other messages to patients when they are not physically at the practice.24,25
Limitations of this preliminary study include a possible lack of generalisability of our findings, given the non-random selection of practices and the small number of practices involved. However, there is no evidence that the patients who received the PPSRSs were substantially different from other Australians.
This preliminary proof-of-concept study did not seek to measure the performance of preventive activities. However, it is likely that the 72% of the patients surveyed in our study who reported that they discussed the contents of their PPSRS in the consultation with their GP did receive or perform some or all of the preventive activities that were listed as due on their PPSRS. These activities were likely to have been performed either during the consultation or subsequently, as a result of a request or referral generated in the consultation.
Because our intervention is new and unique, and a work in progress, we are reporting the findings of this preliminary study as a necessary step before conducting a larger trial that will measure changes in the performance of preventive activities and that will also seek to answer important questions about effects on the process of care, including on the relationship between the patient and the practice, consultation time, numbers of consultations, costs and cost-effectiveness of the intervention.
The technology that we have developed can be adapted to allow general practices to provide other types of information before consultations to specific types of patients. It could be used to improve the care of patients with chronic disease, by reminding them of scheduled care that is due for them, or to recruit patients who may be eligible for research trials. In the future, the information that is provided currently on paper could be sent to or made available to patients electronically.
Implications for general practice
The principle of providing targeted, specific personalised education, information and advice to patients immediately before they consult with their GP seems to have a large potential to help to improve the quality, effectiveness and efficiency of care.
Acknowledgements
We thank the general practices and their patients who participated in the trial, Dr Anton Knieriemen for providing the research software, Daniel Blakeley for entry of survey data and Michelle Lorimer for data analysis. The study was funded by the 2011 RACGP Foundation Grant for a Pilot Study.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.