Although post-traumatic stress disorder is often thought of as the signature disorder in the aftermath of a traumatic event, in fact, a range of mental health disorders can develop, including depression, generalised anxiety, panic, agoraphobia and substance use disorders.2 Initial acute distress is to be expected and, in the early days and weeks, many people will experience difficulties with sleep or concentration, feel anxious, jumpy or irritable, or get very upset when they think about the event. However, a ‘resilient’ trajectory with only transient distress and minimal impact on functioning is the most common outcome.3
Among people with persistent symptoms and impaired functioning, a significant proportion will display a ‘recovery’ trajectory and return to their usual level of functioning in the ensuing months without the need for formal mental health interventions.4 Only relatively few people go on to develop chronic mental health problems following exposure to a traumatic event.2 Risk factors for development of more chronic mental health disorders include pre-existing mental health problems, severity of trauma exposure, lack of social support and life stressors.5,6
Given the high prevalence of trauma exposure among primary care patients,7,8 general practitioners (GPs) are well placed to support and monitor the wellbeing of these individuals, and to deliver simple interventions to those experiencing acute distress. In doing so, GPs can help patients to better cope and return to healthy functioning, and may prevent the development of more persistent mental health problems.
Stepped-care approach
A stepped-care approach is recommended for GPs and other practitioners when providing assistance following trauma. This facilitates the provision of an appropriate level of support to patients (Figure 1). GPs have an important role to play at each level of this stepped-care approach. Given that many people will display a resilient trajectory following trauma, the priority and focus of the first level is on advice and support to promote normal recovery, rather than on mental health diagnosis and treatment.
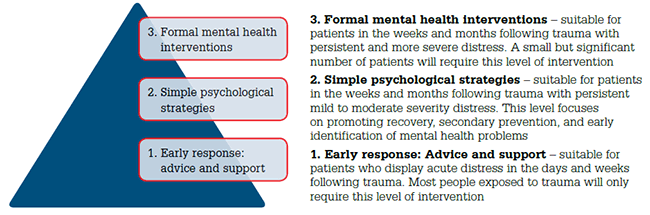
Figure 1. Stepped-care approach to providing assistance following trauma
As a general guide, level 1 support is appropriate and often sufficient for patients with acute symptoms, or mild symptoms that persist in the days and weeks following trauma. Where mild to moderate distress persists despite the provision of level 1 support, patients can be taught simple psychological skills9 (level 2). Patients who display persistent and severe distress in the weeks and months following a traumatic event should be provided with and/or referred for formal mental health interventions (level 3).
Note that there is no replacement for clinical judgement and a stepped-care approach is not always practical or appropriate. Patients presenting in crisis or with extreme distress should be provided more intensive interventions regardless of the time since trauma.
Evidence-informed early response to trauma
International clinical practice guidelines for the management of psychological trauma recommend psychological first aid (PFA)10 as the preferred approach to providing early assistance to people who have experienced a traumatic event.11 PFA seeks to:
- reduce initial distress
- address basic needs (eg. comfort, information, practical and emotional support)
- promote adaptive coping (eg. problem solving)
- encourage engagement with existing social supports.
While this approach has been endorsed by many experts in post-traumatic mental health, it should be noted that the effectiveness of PFA to promote recovery and prevent the development of more serious mental health problems has not been tested empirically. However, the approach can be broken down into a number of separate components, many of which are supported by research.10
What is reasonably clear from the research evidence is that structured psychological interventions, such as psychological debriefing (which encourages individuals to recount the traumatic event and their responses in some detail), should not be offered on a routine basis in the first few weeks following trauma.12 Psychological debriefing as an early intervention after trauma is not effective in preventing post-traumatic mental health problems, and may be counterproductive for some people.13
What should GPs do immediately following a traumatic event?
There is no standard formula for assisting people to better cope with trauma. They should be supported in using strategies and resources that suit them and that are readily available. Consistent with the approach of PFA, GPs can be guided by and promote five empirically derived principles: a sense of safety, calming, self efficacy, connectedness and hope.14 Examples of advice or reassurance GPs can provide in relation to each of these principles can be found in Table 1.
Table 1. Examples of helpful things for GPs to say to patients when providing early response following trauma
| Sense of safety |
That was then, you’re safe now
I’ve been informed by the authorities that the threat of danger has passed
I don’t know the whereabouts of your parents, but let’s see if we can find out some more information |
| Calming |
Those distresssing reactions you describe are quite common; most people will have similar reactions for days if not weeks after a very stressful event
It’s very upsetting at times for you, but that doesn’t mean that you’re weak or going crazy; it’s a normal stress response to a very scary experience
What helps you to feel calm and take your mind off things?
Looking after yourself, and spending some relaxing time with the family, can really be very helpful during this tough time |
| Self efficacy |
I understand that you feel overwhelmed. Let’s see if we can come up with at least three things that you do have some control over at the moment
What has helped in the past when you’ve had to deal with a lot of stress? What hasn’t been so helpful?
You’ve obviously got a lot on your plate at the moment. What’s the priority problem that you think you could tackle first?
I can see that you’re wanting everything to return to normal as soon as possible. But you may want to pace yourself for a period so that you don’t put yourself under any additional stress |
| Connectedness |
We know that having people that we can rely on and enjoy spending time with is a very helpful for recovery
Is there some time over the next week when you could catch up with your friend?
It’s up to you of course, but if you’d like to talk about what happened then I’m a good listener
I understand that you don’t feel comfortable receiving government assistance just now. But it’s there if you change your mind |
| Promoting hope |
I’m confident that you’ll get through this
Let’s monitor how you’re going but I would expect that within a week we’ll see things start to settle down
Well done. I think you’re doing a great job of staying positive |
Sense of safety
Promotion of a sense of safety is particularly relevant to GPs providing assistance as part of emergency or disaster relief efforts. When promoting a sense of safety with a patient, it is important to:
- be realistic and specific, rather than provide vague and potentially inaccurate reassurances
- provide simple and accurate information on how to meet the person’s basic needs (eg. food and shelter)
- repeat information as often as needed
- encourage the person to limit exposure to media coverage of the event, particularly graphic coverage that can lead to increased distress.
Calming
Contact with patients in the days and weeks following trauma provides an opportunity for GPs to promote calming and address heightened arousal, anxiety or other emotions that can undermine confidence and active coping. There are a number of helpful calming strategies that GPs can provide, such as:
- teaching patients to use controlled breathing when anxious (Table 2)
- ‘normalising’ psychological reactions to such events
- encouraging sufficient rest, exercise and a healthy diet
- assisting patients to schedule enjoyable and relaxing activities.
Table 2. Instructions for controlled breathing to promote calming
| Step | Action |
|---|
| 1 |
At the first sign of anxiety, inhale and hold your breath for 4 seconds (don’t take a deep breath) |
| 2 |
Breathe out and say the word ‘relax’ to yourself in a calm, soothing manner |
| 3 |
Breathe in and out slowly, using a 6-second cycle of breath, ie. breathe in for 3 seconds and out for 3 seconds |
| 4 |
Say the world ‘relax’ to yourself every time you breathe out |
| 5 |
At the end of each minute, hold your breath again for 10 seconds and then continue breathing in the 6-second cycle |
| 6 |
Continue breathing in this way until all the symptoms of anxiety have gone. If you commence controlled breathing as soon as you notice the first sign of anxiety, the symptoms should subside within a few minutes. The more you practise this controlled breathing, the better you will become at using it. Sometimes, you will notice that symptoms of anxiety return after a short while. That’s okay; just do your controlled breathing again for as long as it takes to settle |
It is also important to encourage the patient to avoid unhelpful coping strategies such as substance use and social withdrawal.
Cautious and time-limited use of prescribed medications (eg. benzodiazepines) may be required to reduce severe arousal, insomnia and distress. However, if benzodiazepines are prescribed, the course of treatment should be kept as brief as possible due to the risk of tolerance and dependency. There is no evidence to support the practice of routinely offering medication to prevent post-traumatic mental health problems.12
Self efficacy
After experiencing a traumatic event, patients may present to their GP feeling overwhelmed and unable to prioritise or cope with a range of practical and emotional concerns. For example, following a natural disaster, patients are frequently concerned about lost possessions, organising childcare and schooling, completing insurance forms and lack of employment. When promoting a sense of self efficacy with a patient, GPs can:
- highlight those aspects of the situation that the person has some control over
- remind the person about past experiences of successfully coping with stressful situations
- encourage the person to actively address problems and solve one problem at a time
- assist the person to ‘recalibrate’ their expectations of themselves.
Connectedness
Support from family, friends and community services is a strong protective factor and enhances recovery following trauma.5,6 There are many different forms of social support (eg. emotional support, material and physical assistance, a sense of belonging), and people can derive benefit from receiving support and from helping and connecting with others. GPs can help to promote a patient’s connectedness by:
- explaining the known benefits of social support
- encouraging the person to identify opportunities to spend time with family and friends
- telling the person that they may find talking to others helpful, but should do so when they feel ready
- directing and referring the person to appropriate community support services
- anticipating that some people will not feel deserving of assistance.
Promoting hope
Many patients seen by their GP in the days and weeks following disaster or trauma will feel pessimistic and defeated by their recent experiences, and may have difficulties envisaging a future for themselves or their family. A GP has an early opportunity to promote hope about the patient making a successful recovery, by conveying that:
- most people recover with time by using helpful coping strategies and with the support of family and others
- for many people, distressing psychological reactions are transient
- the patient has strengths, such as their ability to cope under stress or their available social supports.
Ongoing monitoring and GP self care
Given the variability in mental health trajectories following trauma, active and ongoing monitoring of patients by GPs is often needed for early detection of stalled recovery and/or persistent mental health difficulties that require more intensive treatment. It is important to be aware that patients experiencing persistent difficulties in recovery may often present to GPs with non-specific physical health complaints.
Providing care in the aftermath of a traumatic event can place significant demands on GPs. For example, GPs may face repeated exposure to traumatic and distressing experiences of others, and in some large scale events, may themselves be members of the affected community. It is therefore important that GPs look after their own mental health, by employing the self-management strategies that they encourage their patients to use.
Key points
- Only a minority of people develop chronic mental health problems following exposure to a traumatic event.
- GPs are well placed to support and monitor primary care patients following trauma exposure.
- Psychological first aid is the preferred approach to providing early assistance to people who have experienced a traumatic event.
- Early advice and support provided by GPs can be guided by the following principles: a sense of safety, calming, self efficacy, connectedness and hope.
- GP self care is an important aspect of providing post-trauma patient care.
Resources
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.