Patients’ attitudes to their asthma and perception of their asthma control are suggested reasons for dissonance between recommended and actual medication use.8,9 How clinicians perceive their patients’ asthma control, and the concordance between the two perspectives, may also influence asthma management and the patient’s disease.10 The few international studies conducted have found concordance between patients and physicians perceptions of asthma control to be low,11,12 but this has not been investigated in Australia.
The aims of this study were to determine the prevalence of asthma in adult patients (18 years and older) attending general practice, the (measured) level of asthma control in these patients, the general practitioners’ (GP’s) perception of the patients’ asthma control and the patients’ perceptions of the impact of asthma on their lives. Any correlations between the perceptions of asthma control and measured asthma control score were also investigated.
Method
This study was conducted through a Supplementary Analysis of Nominated Data (SAND) sub-study of the Bettering the Evaluation and Care of Health (BEACH) program. BEACH is a continuous, national, cross-sectional survey of Australian general practice activity. The BEACH methods are described in detail elsewhere,13 but in brief, each year approximately 1000 randomly sampled, currently active recognised GPs are recruited. The GPs record details for 100 consecutive encounters with consenting, unidentified patients, on structured paper forms. Information is collected about what is managed for each patient at each visit on the days the GP is participating. Throughout the program, a series of SAND sub-studies are carried out. These utilise the GP as an ‘expert interviewer’ to record, in discussion with the patient, aspects of patient health additional to the content of the encounter. For this sub-study, 125 GPs were posted recording kits containing the asthma control SAND questions. Each GP was asked to survey 30 patients from their sample of 100 over a 5-week period from 10 July to 13 August, 2012.
For each of the sampled adult patients, the GP was asked to record: whether the patient had diagnosed asthma, how the GP rated the patient’s asthma control (poor, partial, well controlled), what impact asthma has on the patient’s life (patient’s perspective), what medications the patient has taken for asthma in the past month, how often the patient has used these medications in the past week, and each of the questions contained in the Asthma Control Questionnaire (5-item version (ACQ-5)).14,15 The five ACQ-5 questions (shown in Table 1), are scored on a 7-point scale (0 = good control, 7 = poor control), and the overall score (‘raw score’) is the mean of the five responses.16 Patients’ scores were then classified into three prescribed groups (‘grouped scores’) as having well-controlled asthma (ACQ-5 score < 0.75); not well-controlled asthma (ACQ-5 score 0.75–1.5), or uncontrolled asthma (ACQ-5 score >1.5).17 For comparability with the GP perception scale and the ACQ-5 which have three asthma-control levels, the patient perception scale categories of ‘not at all’ and ‘a little’ were collapsed to compare with ‘well-controlled’, the ‘moderate’ category was compared with ‘partial control’ and the ‘quite a lot’ and ‘a great deal’ were combined to compare with ‘uncontrolled’.
Table 1. Asthma Control Questionnaire, 5-item version (ACQ 5)14,15
| Circle the number of the response that best describes how you have been during the past week |
| 1. On average, during the past week, how often were you woken by your asthma during the night? |
|---|
0. Never
1. Hardly ever
2. A few times
3. Several times
4. Many times
5. A great many times
6. Unable to sleep because of asthma |
| 2. On average, during the past week, how bad were your asthma symptoms when you woke up in the morning? |
|---|
0. No symptoms
1. Very mild symptoms
2. Mild symptoms
3. Moderate symptoms
4. Quite severe symptoms
5. Severe symptoms
6. Very severe symptoms |
| 3. In general, during the past week, how limited were you in your activities because of your asthma? |
|---|
0. Not limited at all
1. Very slightly limited
2. Slightly limited
3. Moderately limited
4. Very limited
5. Extremely limited
6. Totally limited |
| 4. In general, during the past week, how much shortness of breath did you experience because of your asthma? |
|---|
0. None
1. Very little
2. A little
3. A moderate amount
4. Quite a lot
5. A great deal
6. A very great deal |
| 5. In general, during the past week, how much of the time did you wheeze? |
|---|
0. Not at all
1. Hardly any of the time
2. A little of the time
3. A moderate amount of the time
4. A lot of the time
5. Most of the time
6. All the time |
We calculated proportions and robust 95% confidence intervals using survey procedures in SAS software (version 9.3; SAS Institute, Cary, NC)18 that adjust for the study’s cluster design. Statistical significance of differences was judged by non-overlapping 95% confidence intervals (CI), which improve the interpretation of data because they provide robust upper and lower boundaries for the probable size of the true effect. A sample prevalence estimate was calculated which can be interpreted as the prevalence of asthma among patients who present to GPs at any given time.
Pearson’s correlation statistics were used to measure any correlation between GP’s opinion of patient asthma control and the patient’s perception of the impact of asthma on their life, GP’s opinion of patient asthma control and actual ACQ-5 scores, and patient’s perception of the impact of asthma on their life with actual ACQ-5 scores.
Results
Recording pads were returned by 103 of 125 GPs (82.4%). The age distribution of the patients in this SAND sample (Figure 1) did not significantly differ from that of patients at the 122.5 million general practice encounters claimed across Australia through Medicare in 2011–2012 (personal communication, Department of Health Australia, May, 2012). Completed asthma forms were received for 2563 patients aged 18 years or older.
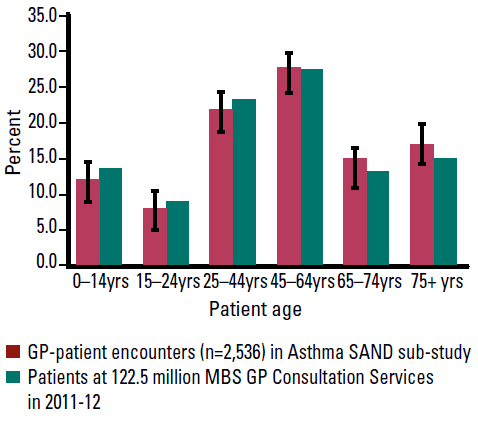
Figure 1: Age distribution of patients in SAND sub-study sample
The prevalence of diagnosed asthma in adult patients was 12.7% (95% CI: 10.9–14.5) (n = 325). Age-specific prevalence did not differ between age groups, but the asthma prevalence was significantly higher among females (14.4, 95% CI: 12.31–16.54) than males (10.0, 95% CI: 7.72–12.28).
General practitioners believed asthma to be well controlled in three-quarters of patients (Table 2). A similar proportion of patients felt that asthma had little or no impact on their lives. However, the grouped ACQ-5 scores showed only half of patients to be classified as ‘well controlled’ and 31.8% uncontrolled.
Table 2. GP and patient perceptions of asthma control and grouped ACQ-5 scores
GP opinion
(n = 318) | %
(95% CI) | Patient-perceived impact
(n = 319) | Percentage
(95% CI) | ACQ-5 scores*
(n = 318) | Percentage
(95% CI) |
|---|
Well controlled
(n = 237) |
74.5
(70.0–79.1) |
Not at all
(n = 113) |
35.4
(29.2–41.6) |
Well controlled
(n = 166) |
52.2
(46.6–57.8) |
Partial control
(n = 62) |
19.5
(15.5–23.5) |
A little
(n = 134) |
42.0
(36.3–47.7) |
Not well controlled
(n = 51) |
16.0
(11.7–20.4) |
Poor control
(n = 19) |
6.0
(3.4–8.5) |
Moderately
(n = 47) |
14.7
(10.6–18.9) |
Uncontrolled
(n = 101) |
31.8
(26.5–37.0) |
|
|
Quite a lot
(n = 17) |
5.3
(2.9–7.8) |
|
|
|
|
A great deal
(n = 8) |
2.5
(0.7–4.3) |
|
|
| * Scores of <0.75 = well controlled; 0.75–1.5 = not well controlled; >1.5 = uncontrolled |
When comparing the ACQ-5 raw scores with GP and patient perceptions of asthma control, there was good correlation between GP perception of asthma control and individual patient ACQ-5 raw scores, and between GP perception and patient perceived impact of asthma. The highest correlation occurred between the patients’ perception of the impact of their asthma and their raw ACQ-5 score (Table 3).
Table 3. Correlation between GP and patient perceptions of asthma control and actual ACQ-5 scores
| Variables | Pearson’s correlation |
|---|
| GP perception of asthma control |
Actual ACQ – scores (ungrouped raw scores) |
0.6545 |
| Patient-perceived impact |
Actual ACQ – scores (ungrouped raw scores) |
0.7435 |
| GP perception of asthma control |
Patient-perceived impact |
0.6671 |
Of the 325 patients with diagnosed asthma, 24.4% took no medication in the previous month. In the remaining 245 patients, short-acting â2 agonist (SABA) and inhaled corticosteroids (ICS)/long-acting â2 agonist (LABA) accounted for 43% and 39% of medications, respectively. The frequency of use in the previous week was high for both medications (Table 4). Only 8.2% took ICS alone.
Table 4. Medication taken for asthma management
| Asthma medications in last month (n = 414) | Taken how often in the past week? Percentage* (95% CI) (n) |
|---|
| Not at all | 1–2 times | 3–10 times | 11+ times |
|---|
SABA (± other medication)
(n = 178) |
22.2
(16.4–28.1)
(n = 38) |
24.0
(17.8–30.2)
(n = 41) |
24.6
(18.4–30.2)
(n = 42) |
29.2
(22.3–36.2)
(n = 50) |
SABA only
(n = 43) |
41.9
(27.4–56.3)
(n = 18) |
25.6
(12.4–38.7)
(n = 11) |
18.6
(4.9–32.3)
(n = 8) |
14.0
(3.6–24.3)
(n = 6) |
LABA & ICS
(n = 162) |
7.2
(2.9–11.5)
(n = 11) |
11.1
(5.7–16.5)
(n = 17) |
24.2
(16.4–32.0)
(n = 37) |
57.5
(47.9–67.1)
(n = 88) |
LAMA
(n = 17)† |
5.9
(0.0–42.1)
(n = 1) |
17.6
(0.0–42.1)
(n = 3) |
76.5
(50.0–100.0)
(n = 13) |
0.0
(n = 0) |
ICS without LABA
(n = 18)† |
0.0
(n = 0) |
22.2
(2.0–42.4)
(n = 4) |
33.3
(10.4–56.2)
(n = 6) |
44.4
(17.7–71.2)
(n = 8) |
OCS
(n = 14)† |
23.1
(0.0–57.5)
(n = 3) |
23.1
(0.0–51.4)
(n = 3) |
30.8
(0.0–69.8)
(n = 4) |
23.1
(0.0–59.8)
(n = 3) |
Asthma medications recorded as taken in the previous month by 245 patients. Frequency of use was reported for 391 of the 414 asthma medications. SABA = short-acting beta agonist; ICS = inhaled corticosteroid; LABA = long-acting beta agonist; LAMA = long acting muscarinic agonist
*Missing data removed
† result should be interpreted with caution due to small numbers |
Discussion
Nationally, one in eight adult general practice patients has diagnosed asthma, a finding consistent with other national prevalence estimates.19,20 There was a high level of agreement about the perceived control/impact of the patient’s asthma between GPs and patients, while the grouped ACQ-5 suggested the patients’ asthma to be less well controlled than either perceived. Medication use for asthma patients was sub-optimal.
There is evidence from the literature that patients with well-controlled asthma may still experience exacerbations, particularly during respiratory infections.21 These data were recorded in July and August, which are winter months when patients are most likely to suffer a respiratory infection that may trigger their asthma. This increases the likelihood that they experienced respiratory symptoms in the previous week, even when their asthma was reasonably well controlled previously. This may explain why the ACQ-5 grouped scores for asthma symptoms experienced during the previous week indicated a greater proportion of patients with poorly controlled asthma than either GPs or patients perceived, given their ‘opinion’ is based on a year-round perspective.
It is also possible that patients have become used to the impact of asthma on their lives, and, having not communicated the existence and/or recurrence of symptoms, lead the GP to believe that their asthma is better controlled than it is in reality. The correlation coefficients show a moderate-to-high level of agreement between the GP and patients’ perceptions of asthma control, and on each of these with the individual ACQ-5 scores. However, agreeing on the level of control does not mean that control could not be significantly improved, and the ACQ-5 has highlighted this group.
This study also highlights issues with asthma medication. No medication use was recorded in the preceding month for one quarter of patients. Only 18 (5.5%) patients were taking ICS without LABA, which is the recommended first-line treatment. Given the recommended ICS/LABA regimen is twice-daily (i.e., 14 times per week),22 it is a concern that only 57.5% of patients were compliant with guidelines. SABA use was high, with 53.8% taking it three or more times in the previous week; more than half of these took SABA more than 10 times and 13.2% of patients were medicating solely with SABA. Both are indicators of loss of asthma control.22 We do not know whether these patients had not been prescribed long-term preventive therapy, or were not adhering to their GP’s recommendations. Investigating asthma control related to medication use would have been informative, but numbers were too small for reliable conclusions.
Implications for general practice
The ACQ-5 is a useful tool to opportunistically assess asthma control during consultations. A sizeable proportion of patients with asthma presenting to general practice have indicators of a loss of asthma control. The ACQ-5 questions may prompt medication reviews, reinforcing the benefits of compliance and enhancing self-management skills, which will improve long-term asthma control.
Competing interests: None.
Ethics approval: The BEACH program and all SAND sub-studies are approved by the Human Research Ethics Committee of the University of Sydney (Ethics protocol Ref. No. 11428).
Provenance and peer review: Not commissioned; externally peer reviewed.