Overweight and obesity in children increases the likelihood of premature mortality and physical morbidity in later life, including diabetes, hypertension, ischaemic heart disease, stroke, asthma and polycystic ovarian syndrome,9 with Aboriginal and Torres Strait Islander children at higher risk.10–12 These problems are compounded by a lack of parental concern about obesity in the general Australian population,13 and desirability of weight gain among Indigenous parents.14,15
This study investigated the prevalence of overweight and obese Indigenous kindergarten children in the Australian Capital Territory and the frequency of self reported parental concern about weight and eating habits.
Methods
A retrospective analysis was performed on data collected as part of the Kindergarten Health Check, a cross sectional population based survey conducted in the ACT from 2004 to 2008.
Participants
All children enrolled in kindergarten, ie. the first year of full time school in the ACT during the years 2004–08, were invited to participate in the Kindergarten Health Check, part of the ACT Health Child, Youth and Women’s Health program. Parents provided written consent for their child to participate, and completed a questionnaire covering demographic data, self reported Indigenous status, health history, and a number of questions. Those related to this study were a tick box option for each of weight and eating in response to the question: ‘Do you have areas of concern about your child’s health?’ There was also space for parents to write comments as they wished.
Data collection
Once consent was received, the Academic Unit of General Practice collated the questionnaire data, and school health nurses performed the health checks, according to a pre-defined ACT Health Directorate protocol. This included height being measured to the nearest 0.1 cm using a stadiometer with shoes off, and weight to the nearest 0.1 kg using calibrated digital scales with jumper off. The International Obesity Task Force body mass index (BMI) cut-off points were used to classify overweight and obesity.16 As these are extrapolated graphically in a continuous curve, age at the date of the health check was calculated for each subject, and age categories were then determined as close as possible to half years of age (Table 1). A BMI equal to or less than 13.8 was used to identify underweight children.
Table 1. Age and body mass index categories
| Subject’s age calculated to two decimal places | Age for purposes of BMI | Body mass index 25 kg/mm2 equivalent (overweight) | Body mass index 30 kg/m2 equivalent (obese) |
|---|
| | Males | Females | Males | Females |
|---|
| 4.25–4.74 |
4.5 |
17.47 |
17.19 |
19.26 |
19.12 |
| 4.75–5.24 |
5.0 |
17.42 |
17.15 |
19.30 |
19.17 |
| 5.35–5.74 |
5.5 |
17.45 |
17.20 |
19.47 |
19.34 |
| 5.75–6.24 |
6.0 |
17.55 |
17.34 |
19.78 |
19.65 |
| 6.25–6.74 |
6.5 |
17.71 |
17.53 |
20.23 |
20.08 |
Where subjects were found to be over or underweight, according to the Centers for Disease Control and Prevention growth charts,17 nurses recommended that either their family doctor or an ACT health dietician review them. Parents who expressed concern about their child’s weight or eating habits on the health questionnaire, were given a leaflet with information about nutrition.
Statistical analysis
All data was entered onto an Access database and then analysed using Predictive Analytics Software to calculate the p value (using c2 test), unadjusted odds ratio (OR) and 95% confidence intervals (CI).
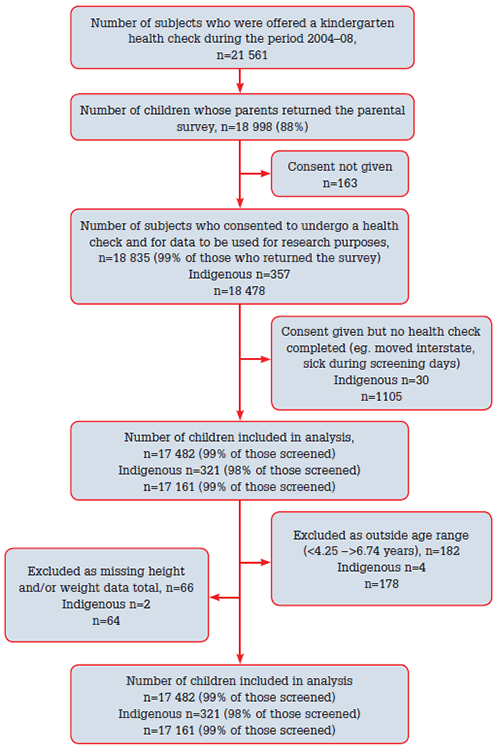
Figure 1. Selection of subjects for the study
Results
During the study period, of the 21 561 children enrolled in kindergarten in the ACT, 18 998 (88%) completed and returned the questionnaire;18 482 (81%) were eligible for this study (Figure 1). Rates of overweight and obesity between the two groups fluctuated over the study period, with higher prevalence in the Indigenous subjects in 2004, 2005 and 2008; and higher prevalence in the non-Indigenous children in 2006 and 2007 (Figure 2). Across the study period, the prevalence of overweight and obesity was statistically significantly higher among Indigenous (18%) compared to non-Indigenous kindergarten children (14%) (p=0.020, OR=1.40, 95% CI=1.051–1.862) (Table 2). Ten percent of parents of normal weight children, and 16% of parents of overweight or obese children, reported concerns about weight and eating habits, with no significant difference between Indigenous and non-Indigenous parents (Table 3, Table 4).
Table 2. Overweight and obesity in Indigenous and non-Indigenous kindergarten children
| Outcome – overweight and obesity | p value | Odds ratio | 95% confidence interval |
|---|
Overweight or obese
(%) | Healthy weight or underweight
(%) |
|---|
| Exposure – indigeneity |
Indigenous
(n=321) |
59 (18) |
262 (82) |
0.020 |
1.401 |
1.051–1.862 |
Non- Indigenous
(n=17 161) |
2378 (14) |
14 783 (86) |
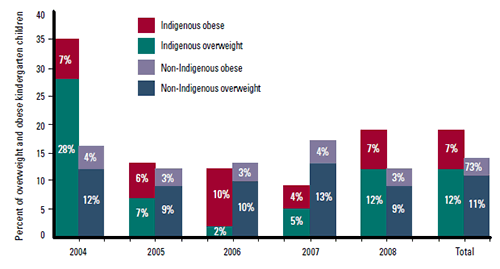
Figure 2. Overweight and obesity in kindergarten children, 2004–08
Table 3. Parental concern about obesity in overweight and non-overweight kindergarten children
| Outcome – parental concern | p value | Odds ratio | 95% confidence interval |
|---|
Parental concern
(%) | No parental concern
(%) |
|---|
| Exposure – weight |
Overweight or obese (n=2437) |
380 (16) |
2,057 (84) |
0.000 |
1.612 |
1.428–1.820 |
Healthy or underweight
(n=15 045) |
1547 (10) |
13 498 (90) |
Table 4. Parental concern about obesity in Indigenous and non-Indigenous kindergarten children
| Outcome – parental concern | p value | Odds ratio | 95% confidence interval |
|---|
Parental concern
(%) | No parental concern
(%) |
|---|
| Exposure – indigeneity |
Indigenous
(n=321) |
42 (13) |
279 (87) |
0.234 |
0.820 |
0.591–1.138 |
Non-Indigenous
(n=17 161) |
1885 (11) |
15 276 (89) |
Discussion
This study demonstrated a statistically significantly higher prevalence of overweight and obesity in Indigenous kindergarten children than their non-Indigenous counterparts. This cannot be explained by a lack of parental concern or positive parental attitudes toward weight gain. In the absence of national data on overweight and obesity in Aboriginal and Torres Strait Islander children, this study provides further insight into the nature and extent of the problem. The reliability of the data is assisted by the high response rate and that the proportion of Indigenous subjects in this study (1.8%) is similar to that of the Australian population (2.5%).17 The higher prevalence of overweight and obese children found in this study is consistent with previous research,4–6 and mirrors a broader national trend of increased burden of disease among Indigenous Australian children.19–21
Several government campaigns specifically targeted at childhood overweight and obesity coincided with the study period (2004–08). The ‘Go for 2&5’ campaign began in the ACT in 2005 and continued throughout the entire study period. Aimed at children aged 5–12 years and their parents, it encouraged daily consumption of fruit and vegetables.22 The ‘Get Moving’ campaign of 2006, targeted children aged 5 years and over, and promoted regular physical activity.23 The ‘Get Set 4 Life – Habits for Healthy Kids’ campaign began in the final year of the study period (2008), and involved the distribution of an information booklet to parents regarding healthy eating, regular exercise and other children’s health issues.24 Despite these numerous public health campaigns, only 16% of parents of overweight or obese children expressed any concern about their child’s weight and/or eating habits on the questionnaire.
One of the limitations of this research is its focus on kindergarten children. The greatest burden of childhood obesity may arise later, in early adolescence, when eating and exercise behaviours are more strongly linked to peer group influence and hormonal changes.25 In addition, the age at which childhood obesity is an accurate predictor of obesity in adulthood remains uncertain.26 In light of this, obesity during the kindergarten year may not be a reliable indicator of adult obesity and disease.
Implications for general practice
- Advertising campaigns may not be successful at raising parental awareness about weight and eating habits in children.
- Childhood obesity among kindergarten children remains a significant problem, particularly for Aboriginal and Torres Strait Islander children.
- The low level of parental concern for obesity suggests that GPs should persist with screening for, and managing, overweight and obesity in kindergarten aged children in similar jurisdictions on a proactive basis.
- Ongoing research will help to better define and manage the complex dynamics around childhood obesity.
Competing interests: None.
Ethics approval: ACT Human Research Ethics Committee and the ANU Human Research Ethics Committee.
Provenance and peer review: Not commissioned; externally peer reviewed.
Acknowledgement
The authors acknowledge the diversity of Indigenous peoples in Australia and the problematic nature of attempting to adequately reflect that diversity with suitable terminology. In this article, the use of the term ‘Indigenous’, unless otherwise evident by the context of its use, should be taken to include Aboriginal and Torres Strait Islander peoples.