This article will explore RCA as a powerful tool for teaching, supervision and formative assessment. As well, we propose a new framework for conducting this activity in the Australian general practice setting.
Chart audit and chart stimulated recall
Chart audit is the review and assessment of patient medical records against predetermined criteria.2 It has been used for a range of educational applications, including identification of learning needs and assessment of professional competence.3
Chart stimulated recall (CSR) is a case-based teaching and assessment tool originally developed for assessing clinical decision making in the emergency department setting.4 It uses probing questions to elicit information about the process of care. As a teaching method, CSR is time efficient; allows provision of timely feedback; and encourages reflective practice.
Random case analysis
Random case analysis is a specific method of CSR where records are selected at random, not directed by learner selection.5 It allows identification and exploration of areas where the registrar either does not recognise a clinical knowledge gap (‘unconscious incompetence’), or those they wish to avoid (‘conscious incompetence’). As a result, RCA has educational utility for all stages of learner, and across all levels of competence. A number of templates for medical record review have been devised.6–8
We identified the need for a new framework for RCA for a number of reasons. Our anecdotal experience was that RCA was not commonly used as a teaching method in the local practice setting. This may be, in part, due to the absence of a framework for analysis that reflects the Australian general practice training context. We also wished to better emphasise the potential learning opportunities from the non-clinical aspects of the consultation. As well, we wanted to explicitly incorporate the practice of proposing hypothetical scenarios as a core component of the RCA method.
We developed a new framework of content analysis based on the five domains of general practice from The Royal Australian College of General Practitioners (RACGP) curriculum.9 The framework encourages further exploration and development of clinical reasoning through consideration of four contextual influences: the doctor, the patient, the problem and the system (Figure 1).
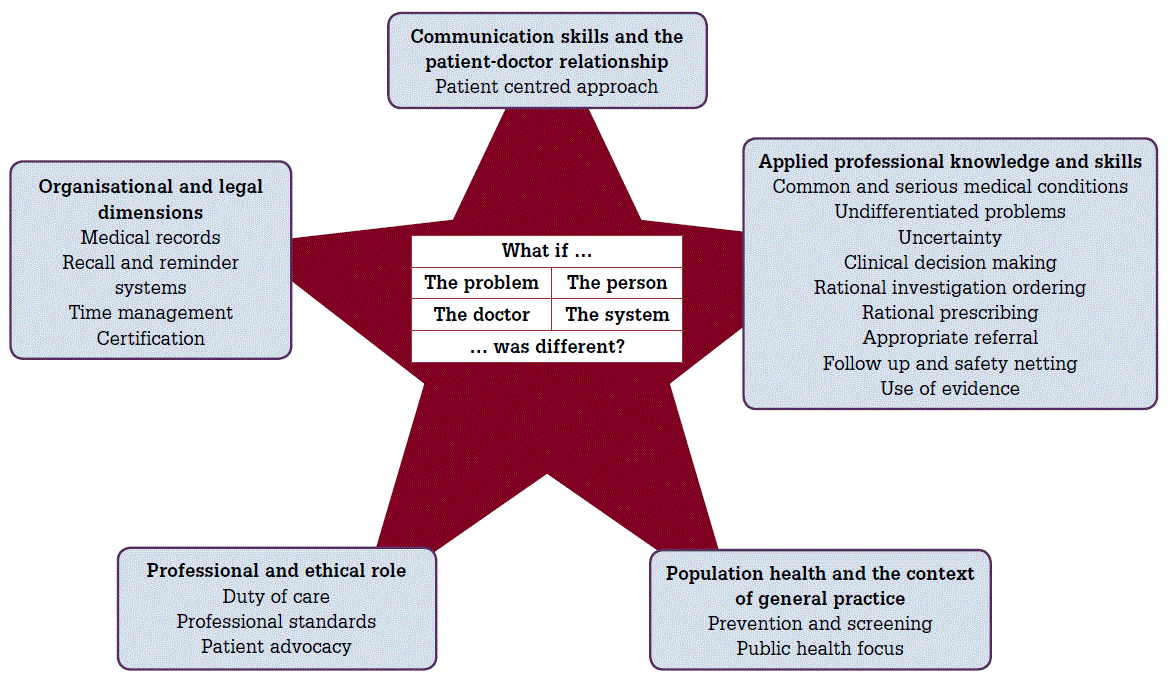
Figure 1. Framework for random case analysis using the RACGP domains of general practice
The RACGP domains of general practice
Communication skills and the patient-doctor relationship
Patient-centred communication is positively associated with patient satisfaction, adherence and better health outcomes.10 Communication skills are ideally assessed and taught by direct observation,11 but review of patient records can also give valuable insight into the registrar-patient relationship. Patient centred communication can be explored though targeted questions, for example, ‘Did the patient have any particular concerns?’ or ‘Do you feel you reached common ground with the patient?’ This is particularly relevant in more challenging consultations, such as when breaking bad news.
Applied professional knowledge and skills
Assessment of the registrar’s applied knowledge and skills is perhaps the most tangible educational application of RCA. The medical record can provide information on focused information gathering (history taking and physical examination), problem definition (differential diagnosis and probabilities) and development of management plans. Rational pathology testing and prescribing have been found to be particularly challenging areas for general practice registrars.12,13 Random case analysis gives an insight into these skills, as well as use of sources of evidence for patient care. Other important areas in this domain include the registrar’s approach to referral, follow up and safety netting.
Undifferentiated presentations are common in general practice and are associated with clinical uncertainty. Random case analysis is an ideal method to explore tolerance of uncertainty and the approach to undifferentiated problems.14
Population health and the context of general practice
Practising with a population health perspective is an essential component of quality primary healthcare. Random case analysis is a useful tool to help explore this domain in the individual consultation.
Questions can be used to explore the registrar’s understanding of epidemiology of disease (‘What is the most likely cause of this particular presentation in this particular patient population?’), public health, including notifiable diseases (‘What are the potential implications for the patient’s family and the wider community?’) and prevention (‘Which, if any, opportunistic preventive interventions did you discuss?’).
Professional and ethical role
Role modelling is arguably the most potent means of instilling professional values in learners.15 However, professionalism must also be explicitly taught,16 with the GP supervisor playing a key role. Random case analysis can contribute to fostering professional practice, especially in the areas of duty of care, patient advocacy and maintenance of professional standards. In appropriate cases, registrars may be asked questions such as, ‘Were there any issues related to consent or confidentiality?’ or ‘Were there concerns about patient-doctor boundaries?’
Random case analysis is a true reflective learning exercise and during the process the supervisor can assess the registrar’s capacity for self-reflection, another aspect of the professional role.
Organisational and legal dimensions
The Medical Board of Australia’s Code of Conduct states that good medical practice involves ‘keeping accurate, up-to-date and legible records that report relevant details of clinical history, clinical findings, investigations, information given to patients, medication and other management’; and are ‘sufficient to facilitate continuity of patient care’.17 Through exploration of the consultation, RCA will reveal the accuracy and clarity of the registrar’s medical records. It can also be used to assess documentation of arrangements for follow up (including use of recall and reminder systems), billing practice and certification.
It has been demonstrated that information contained in referral letters often does not meet the needs of recipients.18 As well as the appropriateness of referral (clinical indication and urgency), RCA can be used to review the quality and comprehensiveness of referral letters.
Clinical reasoning and decision-making
Clinical teachers play a key role in the development of clinical reasoning skills in their learners,19 with GP supervisors integral in the process of helping registrars learn how to ‘think like a general practitioner’.20 Although less immediate than through direct observation, RCA can be used to explore and assess registrar clinical reasoning and decision-making skills. This is particularly effective through the use of so-called ‘Why?’ questions. For example, ‘Why did you come to that diagnosis over any other?’
Deeper exploration of clinical reasoning and decision making can be undertaken by introduction of alternative scenarios, so called ‘What if?’ questions.21 As part of our new framework, we propose a quadrant of four contextual factors on which to base such hypotheticals (Figure1). These may relate to different clinical (patient and presentation) factors such as demographics (‘What if the patient were 75?’) or presence or absence of key symptoms (‘What if the headache was waking the patient from sleep?’). However, by using a framework as we suggest, other (less apparent) contextual influences can be explored. These include factors relating to the registrar (attitudes, skills) and system issues (individual practice and healthcare system). Use of such a contextual framework is therefore likely to broaden the scope of exploration of clinical reasoning.
Use in practice
The basic process and requirements for conducting RCA have previously been described.21 We have adapted this established model to incorporate the new framework for analysis (Table 1).
We suggest the supervisor takes notes as the registrar presents the case, using Figure 1 as a template. Suggested exploratory questions are listed in Table 2. It is clearly unrealistic to try to address all domains and potential contextual influences with each consultation review. Learning areas should be negotiated and prioritised between supervisor and registrar, with the scope for some to be deferred to a subsequent teaching session.22 The stage of training of the registrar may help determine which areas are prioritised – for example, clinical management and note keeping may be more appropriate for a junior registrar, while management of complexity, and care coordination, might be more suitable for more experienced registrars. Specific and constructive feedback remains a critical element of the process.
Figure 2 shows an example of how the new framework of RCA could be used in practice.
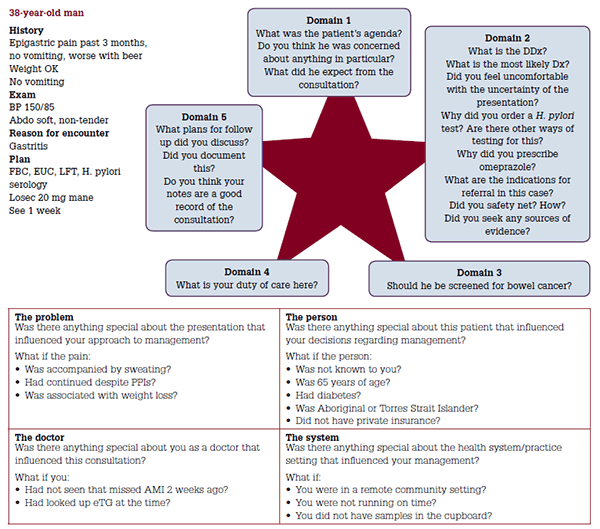
Figure 2. Example scenario: Medical record entry
Table 1. Process for random case analysis
Set
- Ensure an appropriate environment – ideally quarantined teaching time
|
Clarify
- Supervisor to clarify the purpose of RCA – identify particular learning needs
- Supervisor to select a record for review – needs to be both random and recent, enabling better recall of the consultation and clinical reasoning
- Supervisor and registrar to read through the case notes together, as well as other relevant components of the record (eg. past history, medications)
- Registrar to provide further recollections of the case, and clarify what they knew of the patient prior to the consultation
|
Explore
- Supervisor to explore issues in greater detail (using the five domains of general practice – ‘the star’)*
- Supervisor to pose alternative scenarios (using the quadrant of contextual factors – ‘the square’)*
|
Assess
- Supervisor to provide assessment and feedback with reference to the RACGP domains of general practice
- Supervisor and registrar to both identify learning needs and opportunities, and how they will be addressed
- Supervisor to discuss expectations and follow up
- For more senior registrars, the process can be reversed where the supervisor’s notes are reviewed
|
* The supervisor and the registrar should negotiate priority areas for discussion rather than attempting to cover the breadth of learning opportunities available
Adapted from Hays R. Practice based teaching: a guide for general practitioners. Melbourne: Eruditions Publishing, 1999 |
Table 2. Suggested exploratory questions by domain area
| Communication skills and the patient-doctor relationship |
- What do you think was the patient’s agenda?
- Do you feel you reached ‘common ground’ with the patient?
- Did the patient have any particular concerns?
- What did the patient expect from the consultation?
|
| Applied professional knowledge and skills |
- In retrospect, would you have taken further history/conducted further examination?
- What is the most likely diagnosis? How did you reach that conclusion?
- What was the differential diagnosis?
- Were there any conditions you ruled out? How?
- Why did you order the tests you did?
- What was the rationale for prescribing the medication you did?
- Did you feel uncomfortable with the uncertainty of the presentation?
- What are the indications for referral in such a presentation?
- Did you arrange follow up? What exactly did you say?
- Did you safety net? How?
- Did you seek any sources of evidence?
|
| Population health and the context of general practice |
- What is the most likely cause of this particular presentation in this particular patient population?
- What are the potential implications for the patient’s family and the wider community?
- Which, if any, opportunistic preventive interventions or screening tests did you discuss?
|
| Professional and ethical role |
- Were there any issues related to consent or confidentiality?
- Were there concerns about patient-doctor boundaries?
- How might the patient’s culture or values impacted on the consultation?
- Were there any ethical issues in the case?
|
| Organisational and legal dimensions |
- Do you think your notes are a good record of the consultation?
- Did anything special about our particular practice setting influence your management?
|
Assessment
Random case analysis has been identified as a useful in-training formative assessment method for general practice training.8,23 There is evidence supporting the validity24 and reliability25 of (non-random) chart stimulated recall. The mapping of our framework of RCA to the RACGP curriculum domains suggests high validity. Training of supervisors in the use of RCA improves skills26 and may increase standardisation and reliability.
The effectiveness of any assessment tool depends on its level of acceptance. It is therefore vital that a safe learning environment is established and the supervisor clarify the purpose of the exercise at the beginning.
One of the great strengths of RCA as an assessment tool is the immediacy of feedback. Timely, specific and relevant feedback will enhance deeper learning and reflection.
Conclusion
Random case analysis has been described as ‘the most powerful teaching and assessment tool at our disposal’.27 Along with other supervision techniques, it can help the supervisor identify whether their registrar is ‘safe in there’.1 We believe that our new model of analysis will allow a more comprehensive assessment of the registrar’s performance. The use of this framework as a teaching and formative assessment tool merits formal evaluation.
Competing interests: None. Provenance and peer review: Not commissioned; externally peer reviewed.