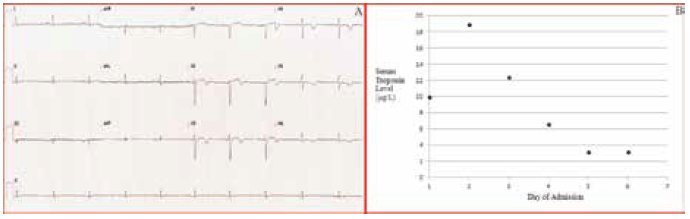
Figure 1. Case study 1: ECG demonstrated T wave inversion in leads V2 to V6 (A). Serum troponin levels demonstrated a rise and fall over the days of admission (B)
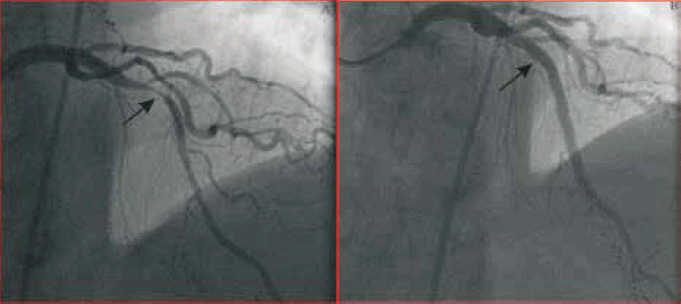
Figure 2. Case study 1: coronary angiogram in right anterior oblique cranial projection demonstrated the severe proximal LAD lesion (arrow) pre (A) and post (B) DES insertion
Case commentary
This patient had an ischaemic myocardial infarction (MI). His history of chest pain was typical for myocardial ischaemia. There were ischaemic changes on ECG and a rise and fall of serum troponin levels. On coronary angiography, a lesion was identified in the proximal LAD, which corresponded to the anterior ECG changes. He was successfully managed with DES insertion to the LAD lesion, along with medical therapy for acute coronary syndromes, including dual anti-platelet therapy, a beta-blocker, an angiotensin converting enzyme inhibitor and a statin.
Case study 2
A man, 51 years of age, presented to a regional hospital with chest heaviness on exertion. He was an ex-smoker with a
5 pack year history, and a family history of ischaemic heart disease, with his father having had CABG aged in his 60s. He had no other medical history, and led an active lifestyle as a fisherman. While hiking, he experienced a single episode of prolonged chest heaviness associated with shortness of breath. He did not have any previous history of chest pain, and usually had an excellent exercise tolerance.
His ECG demonstrated minor (<1 mm) ST-segment elevation in leads II, III and aVF. His serum troponin I was elevated at
3.98 µg/L (normal <0.03 µg/L) and then fell rapidly (Figure 3). He was transferred to our institution for further management as a presumed case of acute coronary syndrome. Coronary angiogram was performed and demonstrated normal coronary arteries without obstructive coronary artery lesions. Transthoracic echocardiography demonstrated normal left and right ventricular systolic function (Figure 4). Is this a case of MI?
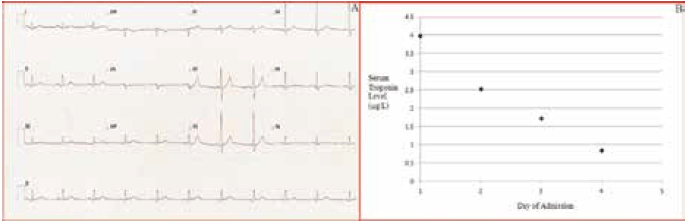
Figure 3. Case study 2: ECG demonstrated minor ST-segment elevation in leads II, III, aVF (A). Serum troponin levels fell rapidly from the day of admission (B)
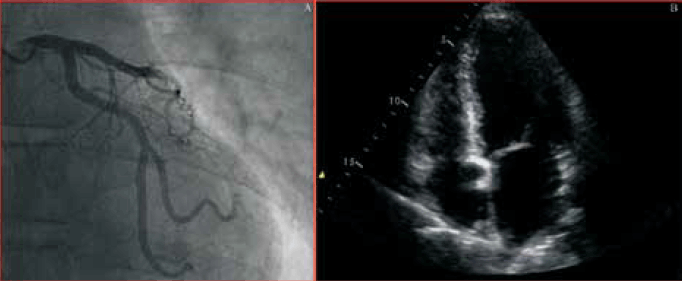
Figure 4. Case study 2: coronary angiogram in left anterior oblique cranial projection demonstrated smooth coronary arteries (A). Apical four-chamber view of transthoracic ECG demonstrated normal left and right ventricular size and systolic function (B)
Case commentary
This patient’s history is not typical for myocardial ischaemia. He had a single episode of chest heaviness. Although many patients with MI present with atypical symptoms, the patient’s coronary angiogram did not demonstrate obstructive coronary artery disease and there was no evidence of a regional wall motion abnormality on echocardiography. The diagnosis of MI was not confirmed. Therefore, other diagnoses must be considered.
In retrospect, the patient remembered trauma to his right knee associated with swelling 1 week before presentation. A computed tomography pulmonary angiogram demonstrated a right middle lobe pulmonary artery embolus (Figure 5). The patient was managed with therapeutic anticoagulation. Although the elevated troponins indicated a significant clinical event had occurred, this turned out to be a pulmonary embolus rather than MI.
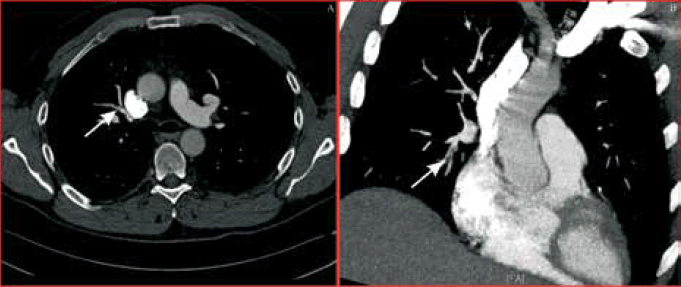
Figure 5. Case study 2: Computed tomography pulmonary angiogram demonstrated right middle lobe pulmonary artery embolus (arrow) in coronal (A) and sagittal (B) sections
Case study 3
A woman, 53 years of age, presented to hospital with an episode of severe chest pain associated with shortness of breath. Her cardiac risk factors included hypertension and a family history of premature coronary artery disease. Recently she had been experiencing significant stress at work.
Her ECG demonstrated sinus rhythm with widespread T wave inversion. Her serum troponin I peaked at 1.61 µg/L (normal <0.03 µg/L) (Figure 6). Coronary angiogram was performed, which demonstrated smooth coronary arteries without obstructive lesions. Left ventriculogram demonstrated apical ballooning, consistent with Takotsubo or stress cardiomyopathy (Figure7). Transthoracic echocardiogram confirmed mild-to-moderate segmental left ventricular dysfunction consistent with stress cardiomyopathy. The patient was managed conservatively with an angiotensin converting enzyme inhibitor and optimisation of hypertension management. Repeat echocardiography at 7 weeks demonstrated her left ventricular function had returned to normal.
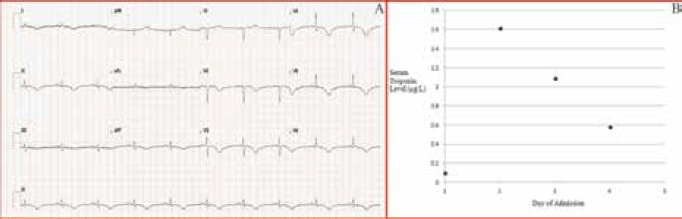
Figure 6. Case study 3: ECG demonstrated widespread T wave inversion in leads II, III, aVF, V2 to V6 (A). Serum troponin levels peaked early, before rapidly falling (B)
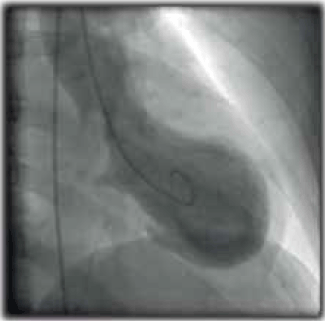
Figure 7. Case study 3: left ventriculogram demonstrated apical ballooning which is characteristic of Takotsubo or stress cardiomyopathy
Case commentary
This patient’s history mimicked myocardial ischaemia. However, an important factor was the recent significant emotional stress. There were some ECG changes, however, there was no typical rise and fall in serum troponin levels. Smooth coronary arteries on coronary angiography made ischaemic MI unlikely. Apical ballooning on left ventriculogram was diagnostic of stress cardiomyopathy.
What is MI?
The third universal definition of MI was released in 2012 by the Third Global Myocardial Infarction Task Force and endorsed by the European Society of Cardiology, the American College of Cardiology Foundation, the American Heart Association and the World Heart Foundation.1
MI occurs when there is myocardial necrosis due to prolonged myocardial ischaemia, and has a high rate of morbidity and mortality.2,3 Half the mortality from MI occurs pre-hospitalisation. A recent large study of ST-elevation and non-ST-elevation MIs reported in-hospital mortalities of 4.5% and 1.9%, respectively.4 There are also major social, psychological and legal implications attached to a diagnosis of MI for the individual.5
Since the advent of cardiac biomarkers, most importantly troponin, an increasing emphasis has been placed on serum troponin elevation in the diagnosis of MI.6 A premise of the first universal definition of MI (released in 2000), was that elevated troponin confirmed myocardial necrosis and therefore MI.7 These guidelines were updated in 20078 to recommend the use of highly sensitive troponin assays.9 The third universal definition of MI provides an integrated approach to diagnosis (Table 1), and acknowledges that troponin elevations can occur in the absence of MI. A large number of conditions are now recognised to cause troponin elevation (Table 2).
Table 1. Definition of acute myocardial infarction
| Acute myocardial infarction is diagnosed when there is evidence of myocardial necrosis in a clinical setting consistent with acute myocardial ischaemia |
Detection of a rise and/or fall of cardiac biomarker with one value >99th percentile upper reference limit, and with at least one of the following:
- Symptoms of ischaemia
- New or presumed new significant ST-segment/T wave changes or new left bundle branch block
- Development of pathological Q waves in ECG (any Q wave in leads V2-V3≥0.02 sec or QS complex in leads V2 and V3; Q wave ≥0.03 sec and ≥0.1 mV deep or QS complex in leads I, II, aVL, aVF or V4-V6 in any two leads of a contiguous lead grouping)
- Imaging evidence of new loss of viable myocardium or new regional wall motion abnormality
- Identification of an intracoronary thrombus by angiography or autopsy
|
| Adapted from Thygesen K, Alpert JS, Jaffe AS, et al. Third universal definition of myocardial infarction. Eur Heart J 2012;33:2551–67. with permission from Oxford University Press. |
Mechanisms and causes of serum troponin elevation
Cardiac troponins (I and T), predominantly myofibril bound, are components of the contractile apparatus of myocytes.1,10 Myocardial necrosis leads to the release of this myofibril bound pool of troponin. Additionally, 5–8% of cardiac troponins are unbound in cytosol.11 Myocardial injury without necrosis can lead to the release of troponin.10 Mechanisms of serum troponin elevation include myocardial apoptosis, normal myocyte turnover, proteolytic troponin degradation, increased cellular permeability and the formation of membranous blebs, in addition to myocardial necrosis.12,13
Table 2. Clinical conditions that can lead to serum troponin elevation without myocardial necrosis1,6,18
| Conditions associated with serum troponin elevation without myocardial necrosis |
|---|
- Arrhythmias
- Aortic dissection
- Hypo- and hypertension
- Acute and chronic heart failure without significant coronary artery disease
- Hypertrophic cardiomyopathy
- Coronary vasculitis
- Coronary spasm
- Myocarditis
- Takotsubo cardiomyopathy
- Pulmonary embolus
- Sepsis
- Renal failure
- Extreme exertion
- Severe acute neurological conditions, eg. subarachnoid haemorrhage
|
| Adapted from Thygesen K, Alpert JS, Jaffe AS, et al. Third universal definition of myocardial infarction. Eur Heart J 2012;33:2551–67. with permission from Oxford University Press. |
Value of point-of-care troponin testing
Point-of-care troponin testing achieves faster turnaround times compared to conventional central laboratory assays. It has been recommended that testing be implemented when central laboratory troponin results cannot consistently provide test results within 60 minutes.14,15 Point-of-care troponin assays are helpful when the results are positive. Point-of-care troponin testing is less sensitive than central laboratory troponin testing,16 therefore, if the point-of-care troponin tests are negative, and there is ongoing clinical suspicion for an acute coronary syndrome, negative point-of-care results should be repeated later, and confirmed by central laboratory testing. Point-of-care troponin testing may be incorporated into patient management in the emergency department setting. A recent study of 858 patients with undifferentiated chest pain presenting to an emergency department within 8 hours of symptom onset, showed that serial testing over 3 hours with a point-of-care troponin I assay produced good diagnostic accuracy.17
A practical approach to diagnosis of MI
Each patient needs to be assessed carefully (Figure 8). On history, pay close attention to the nature of the chest pain (eg. onset with exertion and relief with rest is typical for angina). Note the presence of cardiac risk factors and known coronary artery disease. Remember that the presenting features of MI are often atypical. In the patient with significant cardiovascular risk factors with/without known coronary artery disease, the probability of chest pain being due to myocardial ischaemia is higher. Examination should be focused to detect signs of cardiovascular abnormalities (eg. arrhythmia and heart failure), and signs suggesting alternative diagnoses (eg. fever and bronchial breathing in a patient with pneumonia).
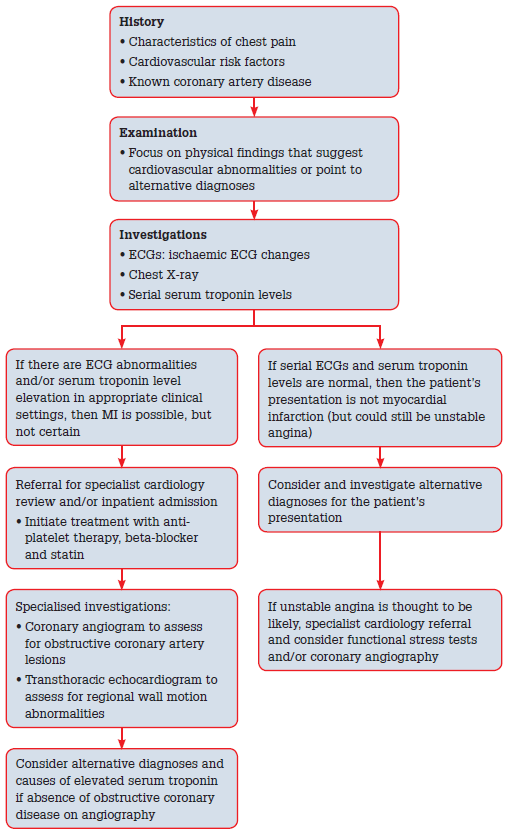
Figure 8. A clinical pathway for the diagnosis of acute MI
Investigations should begin with an ECG. Ischaemic ECG changes, especially ST-segment elevation/depression and T wave inversion, are of particular relevance. The ECG can point to the potential area of myocardium implicated in MI. If initial ECGs are negative, they should be repeated if there is ongoing chest pain or suspicion. Serum troponin levels should be assayed at the time of initial assessment and then at 3–6 hours. A rise and then fall of troponins with at least one elevated reading is highly suggestive of MI, but careful clinical evaluation is required before the diagnosis can be established. In the absence of other evidence of myocardial ischaemia, alternative diagnoses should be considered. A chest X-ray may provide additional diagnostic information and should be considered in patients being evaluated for possible MI. A widened mediastinum could suggest an aortic dissection, but obtaining a chest X-ray should not delay the urgent treatment of a patient presenting with a ST-elevation MI.
If the investigation findings, including serial ECGs and troponin measurements, are negative, then MI is excluded, although unstable angina is still possible. If investigation findings demonstrate ECG changes or serum troponin elevation, then MI is possible, but not certain. In cases where the diagnosis of MI is possible or highly likely, the patient should be referred for inpatient specialist cardiology review, with a view to early coronary angiography in appropriate patients. A transthoracic echocardiogram may supply valuable additional information in patients not thought to warrant immediate coronary angiography. Initial treatment should consist of anti-platelet therapy, a beta-blocker and a statin. If coronary angiography does not reveal evidence of obstructive coronary artery disease, then alternative diagnoses should be considered.
The patients in case studies 2 and 3 all went through this diagnostic regimen, and had significant coronary artery disease excluded by investigations, before arriving at the diagnoses of pulmonary embolus and Takotsubo cardiomyopathy, respectively. If the initial assessment and investigations indicate that MI is unlikely, then alternative causes for the patient’s presentation should be considered. It is important to note that serum troponin elevation is an important clinical prognostic factor, even if the elevated troponin is not due to MI. It is always important to carefully assess and diagnose the underlying clinical conditions.
Key points
- Diagnosis of MI requires evidence of myocardial ischaemia by either:
- history (most typically chest pain) and/or
- ischaemic ECG changes (ST-segment elevation or depression and/or T wave inversion) and/or
- imaging evidence of myocardial ischaemia, such as a regional wall motion abnormality or scarring on ECG
- evidence of myocardial necrosis
- troponin rise/fall with one value >99th percentile upper reference limit.
- Possible cases of MI should be referred for inpatient specialist cardiology review with consideration given to early coronary angiography in appropriate settings.
- There are many causes of serum troponin elevation other than myocardial necrosis.
- The underlying clinical conditions causing serum troponin elevation should be carefully assessed and diagnosed.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.