The potential consequences of undernutrition and risk factors contributing to its development have been reviewed elsewhere (summarised in Figure 1).1,5–7 This article focuses on:
- introducing routine screening for undernutrition into general practice
- interventions to prevent undernutrition in general practice patients.
Prevention and early intervention are key because it is difficult to reverse the effects of undernutrition and weight loss.8,9 Ageing is associated with significant impairment in the regulation of food intake, which means older people are less likely to want to eat and more likely to feel full, and do not automatically compensate with increased intake following periods of decrease in energy intake (eg. following acute illness).10 Moreover, weight loss in the elderly is associated with loss of muscle mass. If weight is regained, there is a disproportionate regain of fat rather than lean body mass (ie. often there is a net loss of muscle mass).11,12 The ensuing sarcopaenia is associated with a risk of adverse outcomes such as physical disability, reduced mobility, institutionalisation, poor quality of life and even death.13
If an older patient presents with any of the many contributing factors for undernutrition or clinical consequences associated with undernutrition (Figure 1), it is important to consider how undernutrition might affect their clinical outcome and to intervene with appropriate management.
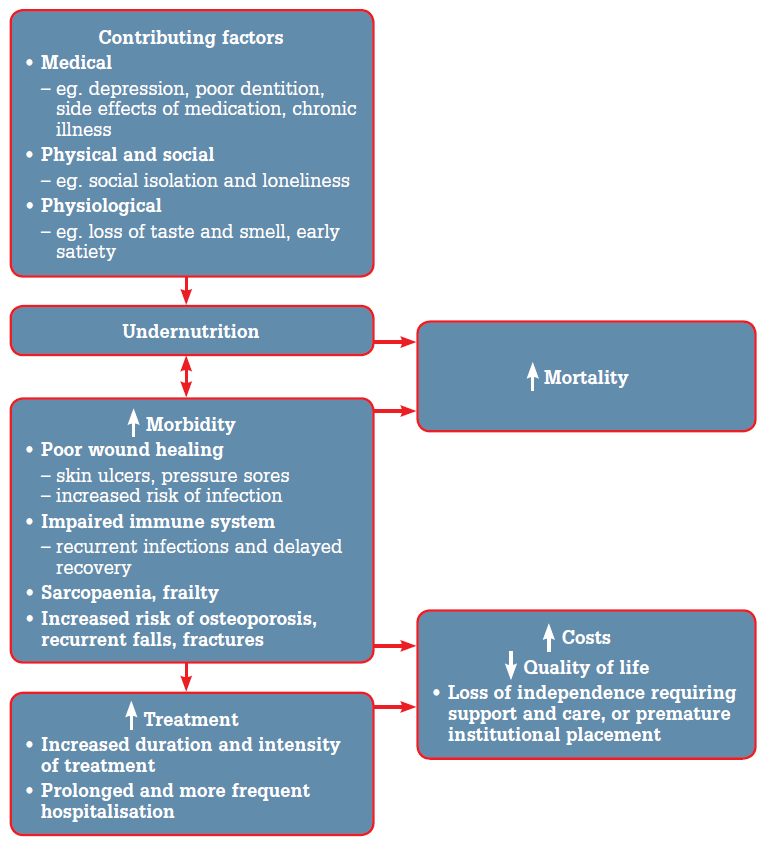
Figure 1. Contributing factors and health outcomes associated with undernutrition1,3,5,7,22
Definitions
Malnutrition: A deficiency or excess (or imbalance) of energy, protein and other nutrients, which causes measurable adverse effects on tissue/body form (shape, size, composition), function and clinical outcome. Can encompass both overnutrition and undernutrition, but often used to refer to undernutrition only.2
Undernutrition: A clinical syndrome characterised by weight loss associated with significant depletion of fat stores and muscle mass. Also known as protein energy undernutrition.3
Frailty: Age related cumulative declines across multiple physiologic systems, with impaired homeostatic reserves and reduced capability to withstand stress, resulting in increased vulnerability to adverse health outcomes such as falls, hospitalisation, institutionalisation and mortality.13
Sarcopaenia: Progressive and generalised loss of skeletal muscle mass and strength, with a risk of adverse outcomes such as physical disability, frailty, poor quality of life and death.13
Identifying undernutrition in the elderly
Who is at risk?
All elderly people are at potential risk of undernutrition. Obese as well as underweight elderly people can experience unintentional weight loss due to undernutrition (masked undernutrition). The risks associated with rapid loss of muscle mass remain in both groups of patients.1,14
It is not possible to identify undernourished patients simply by their physical appearance, body mass index (BMI) or weight at a single time point, therefore systematic screening within general practice is a useful means of identifying those most at risk.
Incorporating screening into general practice
Screening for undernutrition among elderly patients in general practice should be incorporated into routine practice wherever possible, to help focus time and resources on intervention for those identified as at greatest risk.2,15 A systematic approach is best, such as:
- weigh elderly patients at every visit or twice yearly if a patient is seen frequently, with any recorded weight loss triggering nutritional screening (in the elderly, weight loss over time is a better indicator of undernutrition than BMI)
- for patients aged ≥75 years, incorporate a simple nutritional status screening tool (discussed below) into the 75+ annual health assessment.
Screening tools
Validated nutritional screening tools provide an easy and reliable way to identify clinical characteristics associated with undernutrition.3,16 A more comprehensive nutrition assessment can be considered (eg. by an accredited practising dietician) for people identified as malnourished/high risk or with complex nutritional needs.3 Two screening tools that can be easily incorporated into Australian general practice are described in Table 1, with suggested interventions outlined in Table 2.
Table 1. Screening tools for undernutrition
| Screening tool | Criteria assessed | Outcome categories | Validation |
|---|
| Mini Nutritional Assessment Short Form (MNA®-SF)* |
- Weight loss (of 1–3 kg or >3 kg over the past 3 months)
- Appetite
- Mobility
- Psychological stress or acute illness
- Dementia/psychological problems
- BMI (or calf circumference if BMI not available)
|
- Malnourished
- At risk of malnutrition
- Normal nutritional status
|
Validated in international studies for the early detection of undernutrition and frailty in community dwelling individuals aged ≥65 years15,25,26 |
| Malnutrition Screening Tool (MST)† |
- Weight loss (of 1–5 kg, 6–10 kg, 11–15 kg or >15 kg over the past 6 months)
- Appetite
|
- High risk
- Medium risk
- Low risk
|
Developed and validated for acute hospital, oncology and residential care patients27 |
* Downloadable in various formats from www.mna-elderly.com23
† Downloadable from www.health.qld.gov.au/nutrition/resources/hphe_mst_pstr.pdf24 |
Table 2. Suggested interventions according to outcome category23
| Category | Action |
|---|
| Malnourished |
- Commence nutritional intervention:
- oral nutritional supplementation (400–600 kcal/day)
- diet enhancement (Table 5)
- Monitor weight closely
- Carry out further in depth nutritional assessment refer to a dietician)
|
| At risk of malnutrition |
With weight loss
- Commence nutritional intervention:
- diet enhancement
- oral nutritional supplementation (400 kcal/day)
- Monitor weight closely
- Carry out further in depth nutritional assessment
|
No weight loss
- Monitor weight closely
- Rescreen every 3 months
|
Identifying and addressing contributing factors
A variety of common contributing factors can lead to an increased risk of undernutrition in the elderly. Addressing these factors early and in the community allows for improved nutritional health – giving older people the nutritional reserves that can be counted on during periods of acute illness.
Some contributing factors benefit from a multidisciplinary approach involving dieticians, dentists, pharmacists, psychologists and other allied health professionals while for some elderly patients, specialist advice from geriatricians may also be of benefit.
The challenge for general practitioners is to identify contributing factors for undernutrition and address them effectively.
Management strategies
Key factors to address, and management strategies to consider, are reviewed below. It is important to address all of these factors concurrently: addressing social factors without managing contributing medical factors and vice versa may not be fully effective.
A multidisciplinary approach may assist in managing these patients.
Identify ‘red flag’ conditions
If a patient presents with undernutrition, the first objective in general practice is to assess for any potentially life-threatening or serious medical conditions (‘red flags’) that may have led to unintentional weight loss, such as cancer or cardiac, hepatic or renal failure.
Manage chronic or reversible medical conditions
Once ‘red flags’ have been eliminated, many other medical conditions or their treatments that may contribute to undernutrition can be addressed within general practice (Table 3). It is also important to review patient attitudes toward weight; elderly patients may be confused by media coverage of obesity and consider any weight loss to be beneficial.
If geriatric syndromes (eg. falls, dementia, polypharmacy) or functional decline (eg. reduced mobility or ability to perform activities of daily living) are identified, consider referral to a geriatrician.
Table 3. Management of medical conditions that may contribute to undernutrition1,2
- Screen for dementia, anxiety and depression (depression is one of the commonest causes of undernutrition in the elderly)
- Review polypharmacy and long term medications that may influence appetite or nutrition (eg. those causing side effects such as nausea, constipation, anorexia); switch to an alternative medication or eliminate if possible
- Review dietary restrictions – refer to a dietician for advice and support as required
- Identify and manage dyspepsia, nausea or constipation
- Review oral health and encourage regular reviews with the dentist
- Optimise management of chronic conditions that may affect nutrition, such as:
- dysphagia
- gastrointestinal diseases causing malabsorption or maldigestion
- infection or inflammation
- pain
- hypermetabolism (eg. hyperthyroidism)
|
Address social and functional issues
Low socioeconomic status, limited functional ability and social isolation are often major driving factors for undernutrition in the community. Financial constraints will affect access to basic necessities such as nutritious food. Living or eating alone often results in lower food intake for older people and increases their risk of undernutrition.1
It is also important to consider patients’ ability to shop for and prepare food, and awareness of what constitutes healthy eating.
Management of these issues requires an individualised approach for each patient. Where possible, enlist the help of family and friends; some potential interventions are listed in Table 4.
Table 4. Social and functional interventions for undernutrition in the elderly28,29
- Community care services:
- centre based day care
- domestic assistance
- home delivered meals (eg. ‘Meals on Wheels’ or similar)
- Extended Aged Care at Home, Community Aged Care Package Program, Home and Community Care Program
- Allied healthcare:
- consider referral (eg. occupational therapist, dietician)
- Home visit (with nutritional prompts):
- family and friends
- community nurse
- service providers
- general practitioner or practice nurse
- Case management and/or care coordination/planning
- Dietary and social support:
- dietitian
- cooking lessons
- men’s sheds
- community meal programs
|
Recommend nutritional support
Nutritional therapy is an important component in the management of undernourished patients, and should be provided alongside medical and social/functional interventions.
Dietary requirements change in elderly people. In particular, protein requirements for older people are approximately 25% higher than for younger adults.17 Based on the limited data available, the recommended dietary intake for people aged ≥70 years is 81 g per day for men and 57 g for women, or approximately 1 g protein per kg body weight.18
Tailor nutritional advice to the individual. Refer to Table 5 for tips on increasing protein in the diet and other general recommendations.
Consider referral to a dietician for patients with complex needs.
Table 5. Nutritional support and advice for the elderly at risk of undernutrition3,18,28–30
- Liberalise the patient’s diet (review dietary restrictions)
- Encourage use of flavour enhancers
- Recommend frequent small meals and snacks:
- cheese and crackers
- scrambled, poached or boiled eggs
- baked beans
- fortified soups
- milk based puddings and drinks
- sandwiches with high protein fillings (eg. cheese, tuna, ham, chicken)
- Ensure ready availability of nourishing snacks (eg. nuts, yoghurt, cheese and crackers)
- Ensure food texture suits chewing and swallowing ability
- Suggest ways to increase protein and energy intake by fortifying foods:
- incorporate milk, butter or cheese in foods such as soups, sandwiches
or mashed potato
- add milk based sauces (eg. custard, cheese sauce) to fruit and vegetables
- add powdered nutritional supplements to foods such as soups, cereals, custard, mashed potato
- Consider high energy/protein nutritional supplements (nutritional drinks are a convenient and effective way to meet requirements when appetite and/or mood are low. They allow an individual to remain well nourished while the causal factors can be addressed)
- Ensure sufficient fluid intake
- Where a specific nutrient deficiency has been identified, use of a micronutrient supplement may be indicated (eg. iron, folate, vitamin D)
|
Encourage exercise
While not an intervention for undernutrition, resistance training is essential to maximise muscle mass and strength in the elderly. Physical activity provides an opportunity for linking to social activities as well, which can improve general wellbeing and contribute to better energy intake. Encourage physical activity and mobility in addition to an adequate high protein diet.19
Reinforcement and monitoring
It can be difficult for elderly patients to change eating habits, particularly when eating is not triggered by hunger. Regular follow up and reinforcement of nutritional messages is needed. This may include:
- providing written advice (eg. sticky notes to place around the kitchen, or a doctor’s prescription of dietary advice)
- involving family members
- telephone prompting/reminders.
It is important to monitor nutritional intervention regularly. Examples of how this can be achieved include:
- multidisciplinary team management review
- monitoring patients’ weight at each visit
- recording changes in food intake.
As weight gain is achieved, review meal plans and dietary supplements. It is important to remember that weight is also influenced by fluid, so some patients, such as those with cardiac failure, will need their weight assessed in the context of fluid retention.
Intentional weight loss in the elderly
Elderly people who are underweight are at greater risk of mortality than those who are overweight,18,20,21 and the optimal BMI range for older people is suggested to be about 22–27 kg/m2.1 Intentional weight loss is considered inappropriate unless excess weight is associated with functional problems.8,18 If a weight loss program is considered necessary, attention to adequate protein and micronutrient intake, as well as exercise, is required to preserve muscle mass.8 Close monitoring of the weight loss program is important to ensure preservation of muscle mass.
Summary
Undernutrition can present a significant clinical and public health problem among older Australians living in the community. Patients with undernutrition are at increased risk of morbidity, hospitalisation and mortality and therefore early detection and intervention is important. Identifying patients at risk via screening is the first step to providing effective intervention, followed by appropriate management strategies that are implemented once undernutrition or the risk of undernutrition has been identified.
Assessment and treatment of nutritional risk should be part of routine care for the elderly, just as assessment and management of cardiovascular risk factors are standard practice in adults. General practice is an ideal setting to identify and manage patients at risk of undernutrition.
Key points
- Early identification of patients who are at risk of undernutrition is important.
- Monitor weight and incorporate nutritional screening of elderly patients into routine clinical practice.
- Many of the contributing factors for undernutrition in the elderly are amenable to medical intervention by GPs.
- A subset of patients with more complex needs would benefit from referral to a dietician or geriatrician.
Conflict of interest: All authors are members of the Malnutrition in the Elderly Advisory Board, supported by Nestlé Pty Ltd. Karen Charlton and Renuka Visvanathan were members of the international working group to revise and validate the Mini Nutritional Assessment (funded by Nestlé Nutrition Institute, Switzerland). Renuka Visvanathan participated in the 2012 International Consensus Meeting for Protein Intake In Older People, which also received support from the Nestle Nutrition Institute.
Acknowledgements
The authors would like to thank Ms Jane Winters and Dr Sue Cripps for their assistance in preparing this review. Preparation of the manuscript was supported by an independent educational grant from Nestlé Pty Ltd.