To direct treatment to those most likely to benefit, treatment is increasingly focused on those at high risk based on combined risk factors, the absolute risk approach. This approach was developed because it:
- avoids treating people who have a single elevated risk factor but who are at low overall risk of a cardiovascular disease (CVD) event
- avoids missing people with multiple risk factors, each one of which is only slightly abnormal, but who are at high overall risk.4
Because the absolute risk approach prioritises treatment to those most likely to benefit, it is more likely to be effective and cost effective than treating individual risk factors.5
Most international guidelines now advocate the absolute risk approach. Australian guidelines recommend treatment if the 5 year risk of a CVD event is >15%, with some patients being considered for treatment if their 5 year risk is intermediate (10–15%).6 Studies show a gap between patients who are at high absolute risk and those who are currently treated in Australia.7,8 In this study, we sought to identify how the most recent version of Australian guidelines regarding assessment of absolute risk affects who is treated with BP and lipid lowering therapy in a recent Australian cohort.
Methods
Absolute risk estimation
The National Vascular Disease Prevention Alliance (NVDPA) recommends the calculation of CVD risk using the Framingham risk equation based on the original and offspring Framingham cohort studies.9 This equation predicts the risk of ischaemic heart disease, cerebrovascular disease, peripheral vascular disease and heart failure. Although the equation has been validated in patients aged 30–74 years of age in the Australian population,10 risk calculators available to Australian general practitioners only include the age range from 35–74 years. We therefore included participants in this age range.
In addition, the NVDPA guidelines recommend that patients with the following be classified as high risk:
- systolic blood pressure (SBP) ≥180 mmHg
- diastolic blood pressure (DBP) ≥110 mmHg
- total cholesterol >7.5 mmol/L
- diabetes and >60 years of age
- diabetes and microalbuminuria (>20 µg/min or albumin:creatinine ratio of >2.5 for males and 3.5 for females)
- moderate or severe kidney disease (persistent proteinuria or estimated glomerular filtration rate [eGFR] <45)
- familial hypercholesterolaemia.
Individual risk factor approaches
We defined elevated BP according to the 2010 guidelines (SBP ≥140 mmHg or DBP ≥90 mmHg, or diabetes and SBP ≥130 mmHg, or diabetes and DBP ≥80 mmHg).11 Dyslipidaemia was defined as a total cholesterol:high density lipoprotein (HDL) ratio >4.5; a sensitivity analysis was conducted using total cholesterol >6.5 mmol/L.12
The AusDiab follow up study
The 2004–05 AusDiab follow up study included 6527 participants aged ≥30 years or over from the original 11 247 participants recruited in 1999–2000 from 42 randomly selected census collector districts.13 Cholesterol, eGFR, fasting blood glucose, oral glucose tolerance test and albumin:creatinine ratio were measured once. Three sequential BP measurements were taken; we used the average of the second and third in this analysis. A medication audit was conducted to determine if participants were taking BP or lipid lowering medication. The presence of CVD and smoking status was determined by self report, and diabetes by self report, taking an oral hypoglycaemic agent or insulin, a fasting blood glucose level ≥7.0 mmol/L or a 2 hour postload glucose level ≥11.1 mmol/L. Participants were also asked if they identified themselves as Aboriginal or Torres Strait Islander. Information was not available on family history of CVD or familial hypercholesterolaemia.
Participants included in this study
We removed participants from the dataset who were missing data necessary to calculate absolute risk (excluding electrocardiogram evidence of left ventricular hypertrophy). We next removed participants in whom it is not appropriate to attempt to calculate the risk of CVD, that is, those:
- with a prior history of CVD
- aged <35 or ≥75 years
- currently taking BP or lipid lowering therapy, or
- who identified as Aboriginal and/or Torres Strait Islander.
Pretreatment values are more valid for the assessment of cardiovascular risk than on-treatment values. However, in order to estimate potential undertreatment in participants on a single agent, we also calculated cardiovascular risk for treated participants in a secondary analysis.
Results
A total of 3627 participants were included in the primary analysis (Figure 1). Baseline characteristics are shown in Table 1.
Using the individual risk factor approaches, 429 (12%) participants had elevated BP and 983 (27%) had dyslipidaemia, with 167 (5%) having both risk factors, a total of 1245 (34%). Using the Framingham risk equation, 118 participants (3%) had a risk of a CVD event ≥15% in the next 5 years. Using the additional criteria included in the NVDPA guidelines, a further 163 participants were classified as high risk, a total of 281 (8%).
Figure 2 illustrates the cross-classification of the individual versus the absolute risk approaches. Seventy-seven participants (2%) would be treated using the absolute risk approach but not by the individual risk factor approach, having normal BP and lipid levels. They were slightly older (average 56 years), with 20% being smokers, 20% having diabetes and 32% being male. Most were defined as high risk because of reduced renal function. Conversely, 1041 (29%) of participants would be treated by the individual risk factor approach but not by the absolute risk approach. Of these, 218 (6%) had elevated BP, 722 (20%) had dyslipidaemia and 101 (3%) had both.
Using a cut-off of total cholesterol >6.5 mmol/L, fewer participants (736 participants or 20%) would be defined as having dyslipidaemia. Using this cut-off for dyslipidaemia, 233 participants (6%) with dyslipidaemia would be treated using the individual risk factor approach but not using absolute risk.
For participants on treatment, 208 of 1274 participants (16%) had an absolute risk >15% or equivalent: 19% of those on BP lowering therapy and 12% of those on lipid lowering therapy. These participants are potentially being undertreated using the recently released NVDPA guidelines.14
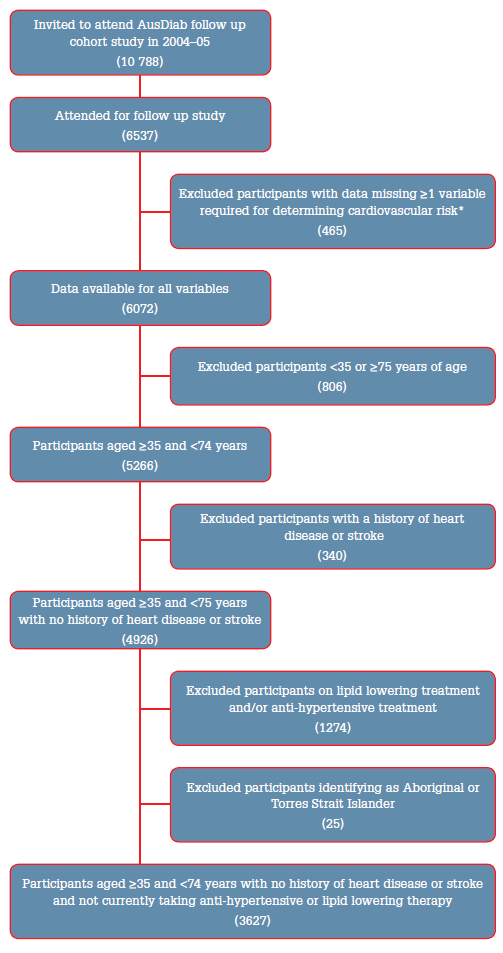
Figure 1. Flow of participants in the analysis
* Excluding ECG evidence of left ventricular hypertrophy
Table 1. Characteristics of participants in the 2004–05 AusDiab dataset aged 35–74 years with no missing data for risk calculation* (n=5266)
| | All patients
(n=5266) | Patients with a history of cardiovascular disease
(n=340) | Patients with no history of cardiovascular disease
(n=4926) |
|---|
BP and lipid lowering treatment
(n=300) | BP treatment only
(n=680) | Lipid lowering treatment only
(n=294) | No treatment
(n=3652†) |
|---|
Age
(SD) |
54.8
(9.9) |
64.0
(7.5) |
62.1
(7.56) |
60.0
(8.36) |
60.7
(8.0) |
52.2
(9.43) |
| Male (%) |
44 |
67 |
49 |
41 |
49 |
43 |
| Smoker (%) |
11 |
11 |
7 |
7 |
8 |
12 |
| Diabetes (%) |
8 |
22 |
32 |
17 |
21 |
4 |
| Total cholesterol mmol/L (SD) |
5.3
(0.96) |
4.7
(1.03) |
4.7
(0.80) |
5.2
(0.94) |
4.8
(0.86) |
5.4
(0.94) |
LDL mmol/L
(SD) |
3.2
(0.88) |
2.6
(1.04) |
2.5
(0.69) |
3.1
(0.85) |
2.6
(0.76) |
3.3
(0.85) |
SBP mmol/L
(SD) |
121
(19) |
128
(20) |
132
(19) |
131
(19) |
128
(18) |
118
(17) |
DBP mmol/L
(SD) |
69
(10) |
70
(10) |
71
(10) |
71
(10) |
70
(10) |
68
(10) |
BP = blood pressure, DBP = diastolic blood pressure, LDL = low density lipoprotein, SBP = systolic blood pressure,
SD = standard deviation
* Excluding ECG evidence of left ventricular hypertrophy
† Includes 25 participants who identified as Aboriginal and/or Torres Strait Islander |
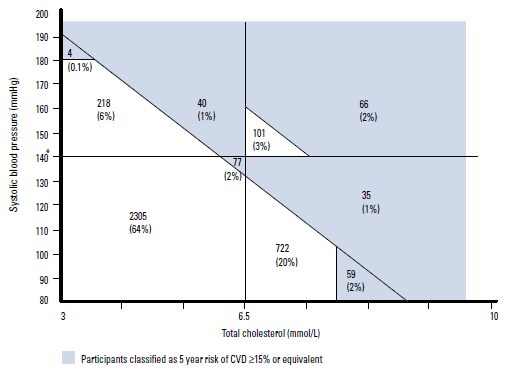
Figure 2. Cross-classification of participants with elevated BP, dyslipidaemia and high absolute risk (n=3627)
* Hypertension defined as SBP ≥140 mmHg or DBP ≥90 mmHg or diabetic and SBP ≥130 mmHg or DBP ≥80 mmHg
Discussion
The estimate of undertreatment in this cohort, 8% (or 10% including those on treatment), is lower than a previous Australian estimate of 22%, albeit that the AusHEART study was conducted in an older cohort (≥55 years of age) and was recruited from patients presenting in a general practice setting.5 The AusDiab cohort is likely to be more representative of the Australian population, but may be limited by volunteer bias. Our study is limited by missing information, such as the family history of CVD and self report on the presence of CVD; both studies are limited by the use of single laboratory measures that may result in misclassification.
Neither study can estimate the potential overtreatment of patients. Patients who have a low risk of CVD and are being treated with a BP or lipid lowering medication are less likely to benefit from their treatment, and harms are more likely to outweigh benefits. The high rate of prescribing of BP and lipid lowering therapy evident in this study is likely to include prescribing to patients at low risk.
We have based our cut-offs for the individual risk factor approaches on previously published guidelines. Clinicians may be basing treatment decisions on the individual risk factor approach but adjusting the cut-off based on other factors. For example, clinicians may be less inclined to treat elderly patients, even though age is a strong predictor of increasing risk. This could increase the extent of undertreatment occurring.
The classification reveals some ambiguities in the absolute risk approach. Absolute risk could be interpreted as:
- treating all patients at high risk with both a BP and lipid lowering medication, regardless of baseline values of BP and/or cholesterol (Figure 2), or
- treating all patients at high risk with either a BP or a lipid lowering medication or both, depending on which risk factors are present and, possibly, patient choice (Figure 3).
The newly released NVDPA guidelines advise that all patients who are assessed as being at high absolute risk should be treated with both a BP and a lipid lowering agent unless contraindicated or clinically inappropriate.14 This approach involves some major shifts in current practice. For example:
- BP lowering therapy would only be used in patients with at least a moderate absolute risk of CVD
- patients with normal BP levels but at high absolute risk may be treated with a BP lowering medication.
There is good evidence that the relative reduction in CVD risk is largely independent of baseline risk or initial BP (including patients with ‘normal’ BP but high risk),15,16 but this approach does involve a significant departure from current practice.
Forty-three percent of the patients at high absolute risk identified in this study had normal levels of serum cholesterol. Currently, one-seventh of the expenditure of the Australian Pharmaceutical Benefits Schedule (PBS) is spent on lipid lowering therapy17 and the clinical effectiveness and cost effectiveness of the various approaches outlined above need to be evaluated.
The guidelines also recommend assessment of additional risk factors, particularly in those with a CVD risk between 10% and 15%. We are unable to estimate how many participants in the AusDiab follow up study would be considered for treatment based on these factors. The evidence base for these factors varies considerably. As an example, obesity is included in this list. While obesity is a risk factor for CVD, its effects are mediated through effects on diabetes, cholesterol and BP, particularly over the 5–10 years used in assessing cardiovascular risk.18 Studies used to establish obesity as a risk factor in recent cohorts are confounded by treatment effects and therefore unreliable unless treatment has been taken into account in the analysis.19 Other risk factors, such as family history of CVD, are also likely to be mediated through the traditional risk factors.
The move to using absolute risk in the prevention of CVD has been a rational and helpful step. However, this new conceptualisation of treatment categories has also created ambiguities that need further clarification.
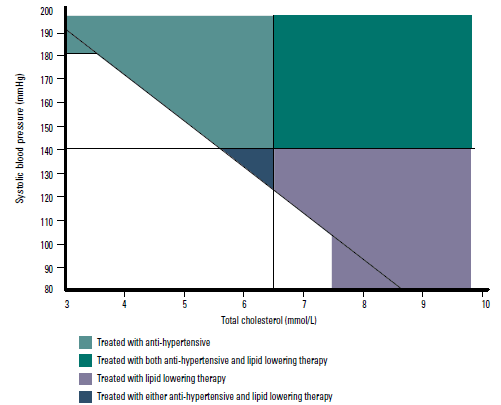
Figure 3. Cross-classification of participants with elevated BP, dyslipidaemia and high absolute risk (n=3627)
Conflict of interest: none declared.
Acknowledgements
Funding for this research was provided by the NHMRC as part of the General Practice Clinical Research Program. We are grateful to the investigators of the AusDiab study for allowing us access to the data used in this analysis, and to the reviewers for helpful comments.