Addressing the AHT injury toll is a core clinical responsibility for primary care providers, who are in the best position within the current Australian health system to provide population-wide pre-injury interventions. This article describes the incidence and aetiology of AHT and hopes to raise awareness of the problem. The most evidence based intervention for AHT prevention is the Period of PURPLE Crying® program,2–4 which provides information to family and carers and web based training and support for providers. Evaluating the cultural appropriateness of this intervention for the rural and remote Australian context is overdue and necessary before its clinical use.
The problem
Abusive head trauma is a common cause of mortality and morbidity in infants.2 The incidence of AHT in Australia is comparable to overseas studies. A recent study into the incidence of AHT in Queensland found 29.6 cases of AHT for which hospital admission was required per 100 000 infants aged 0–24 months and under per year.1 A population based study in the United Kingdom found that the incidence of subdural haemorrhage due to child abuse was 10.1 cases annually per 100 000 children under the age of 2 years,5 and 25–30 cases per 100 000 presentations per year in Edinburgh, Scotland.2 In the United States, between 1200–1400 children may be injured or killed by shaking every year.6 More recent incidence studies in the USA have suggested rates of AHT occurrence are approximately 10 times higher than that of the most common childhood leukaemia.1
The consequences of AHT are significant. In 80% of cases severe morbidity is present, which includes intellectual impairment, behavioural disorders and impaired motor and cognitive skills.7 Enduring cognitive limitations due to AHT include problems with IQ, mental organisation, memory, alternation, inhibition and verbal processing.8 The level of long term impairment seen in children who have experienced AHT in infancy has been demonstrated to be significantly higher than that found in children who have experienced an accidental head injury during infancy.1 The high morbidity and incidence of AHT has financial implications for the healthcare system. Lifetime costs for brain injury have been estimated to be $2.5 million per moderate case and $4.8 million per severe case, with annual treatment costs varying from $8800 to over $280 000.9
Incidence studies in Queensland established that occurrence of AHT was more frequent than that of low speed runovers, drowning and childhood neoplasms in Australian children during age incidence peaks.1 The frequency of infant AHT in Queensland, and the long term sequelae and costs to the healthcare system underline the need to implement and evaluate AHT prevention programs in Queensland settings.
Recognition of the problem
Research has identified numerous factors relating to the infant, family and perpetrator that appear to be associated with an increased risk of AHT.1 Epidemiological research suggests that preventive efforts should engage male carers alongside female carers, as males are reported to be more frequent perpetrators of AHT than females.10 There is a correlation between the peak of infant crying and subsequent incidence of AHT.11 A threecomponent model of AHT aetiology, whereby infant factors, carer factors and situational factors interact and lead to the occurrence of AHT, has been suggested and is outlined in Figure 1.
While AHT injuries carry lifelong disability, diagnosis remains contentious.12 This is due in part to the nonspecific symptoms of head injury; there is wide variability in the clinical presentation, ranging from nonspecific symptoms such as vomiting, to coma or death.13 This suggests a high rate of missed cases. Carers’ attempts to conceal instances of child assault1,14 also increase the risk of misdiagnosis. In a large number of cases, the history provided by the carer is either ‘no’ history or that of a short fall from a bed, couch, counter or other item of household furniture.6 According to Chadwick,15 the probability of receiving a life-threatening head injury as a result from a fall of less than 1.3 m is remote, with the outcome of short falls most commonly benign.15,16 Despite it being possible to differentiate abusive head injury from accidental head injury or disease,16 AHT does not feature in Queensland and Australian national injury prevention strategies for children under 5 years of age.17–19
There is a compelling need to educate and train primary care professionals, including doctors, early childhood educators, health workers, nurses and midwives, in order to decrease the number of preventable cases of AHT. There is also a need for continued monitoring of AHT. Wirtz and Trent14 call for a comprehensive surveillance system to identify high risk areas or groups for intervention and to monitor trends over time.
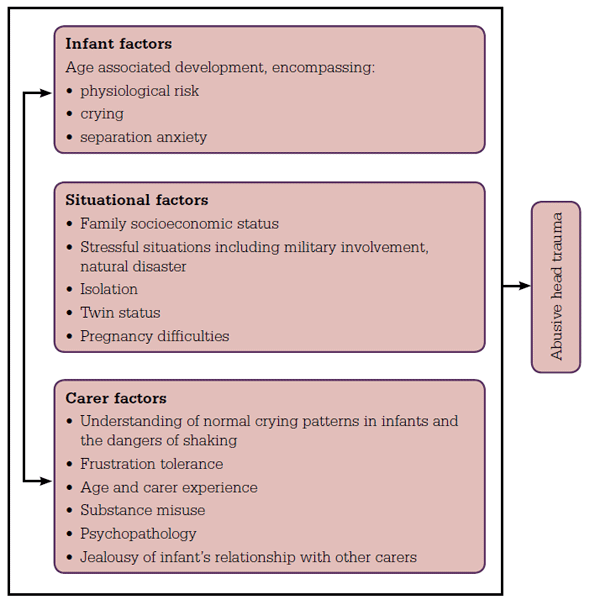
Figure 1. Aetiology of abusive head trauma
Adapted from Kaltner, 20101
Prevention programs
Research suggests that AHT is preventable.2,3 Barr4 asserts that prevention programs delivered to birthing parents have been shown to decrease AHT incidence and increase parental awareness of the dangers of shaking and physically harming their baby. Carer education based prevention programs have shown strong efficacy, with reductions in AHT incidence of up to 50%.4 Barr additionally postulates that programs which increase awareness of crying norms also decrease general childhood physical assault incidence alongside AHT.4
There have been several locally designed, urban based prevention efforts in Australia: at the Westmead Hospital in Sydney, New South Wales; the Royal Women’s and Children’s Hospital in Adelaide, South Australia;20 and in Ipswich in southeast Queensland.1 To date, the evaluations of these local Australian programs have not been published nor implemented within the rural/remote context.
The Period of PURPLE Crying® (Table 1) informs prevention initiatives at the Westmead Children’s Hospital.1 This intervention has been implemented across North America and was referenced in The Royal Australian College of General Practitioners continuing education program for GPs regarding early infant care.21
Table 1. A snapshot of the Period of PURPLE Crying® program
| The Period of PURPLE Crying® program is an evidence based approach to infant AHT prevention. It educates carers and service providers to understand the frustrating features of crying in normal infants, which can lead to shaking or abuse |
| The program includes an 11-page booklet, 10-minute DVD and website resources for parents and care providers of new infants (Figure 2). The materials are presented to parents/carers before leaving the maternity setting (or very early in the infant’s life), by allied health workers, midwives, GPs or maternity physicians. The intervention is supported by internet based training and resources |
| The validated materials are designed to be accessible, available to services at low cost (USD2.00 per package), and intended to be given to every family with every birth. The materials present people from diverse ethnic backgrounds and are presented in plain English and in up to 10 languages |
| Randomised controlled trials in the United States and Canada in 2003–07 with over 4400 parents in a range of medical settings, including hospitals, pre-natal classes and home nurse visits, concluded that the program can significantly alter the knowledge and change the behaviour of carers; evaluation is ongoing |
| The program is implemented in over 800 hospitals and organisations in 49 states of the USA and in Canada, Japan and Australia |
| Source National Centre on Shaken Baby Syndrome, 2011 |

Figure 2. Period of PURPLE Crying® Intervention materials
Reproduced from Barr, 201111
Building the quality of services and evidence base in rural and remote Australia: a strategy for change
There is a paucity in the current literature in Australia, particularly for rural and remote regions, regarding effective interventions to decrease infant AHT. We propose that an initial scoping project to examine the Period of PURPLE Crying® program and its suitability for the rural and remote Australian context is a necessary first step before conducting implementation and clinical trials. A statewide epidemiological data analysis found that children of Aboriginal and Torres Strait Islander descent are over represented in AHT cases in Queensland and are up to three times more likely to experience an incidence of severe AHT compared to infants from the wider Australian community.1 While this might reflect systematic data deficits and reporting bias, this documented occurrence in Aboriginal and Torres Strait Islander populations adds to the imperative for a culturally sensitive intervention program.
In this initial scoping project, primary care and local specialists will be interviewed to evaluate the cultural appropriateness of the intervention in its current form for possible use in a local trial in northern Queensland.
Community and expert engagement is essential to ensure that any AHT prevention interventions are appropriate to the Australian context. A more widespread program is urgently required in Australia to begin to address this issue, to raise awareness, enhance early parenting skills where needed, and to reduce the burden of injury caused by AHT.
Conflict of interest: none declared.