Clubfoot is a deformity characterised by structural equinus (pointing down), adductus (turning in), varus (twisting, such that the heel is pointing in or upward) and cavus (high arch). True structural clubfoot differs from postural clubfoot, as it cannot be passively corrected. In unclear cases, review by a paediatric physiotherapist or orthopaedic surgeon is recommended.

Figure 1. Bilateral clubfoot
Diagnosis on ultrasound can be made as early as 12 weeks gestation, although it is more commonly detected at 18–23 weeks.5,6 False positive diagnoses are documented to range from 0.9% to 17%7–9 but can be as high as 40%10 during the third trimester when postural clubfoot cases are present. No significant relationship has been found between prenatal diagnosis and severity of the affected foot/feet.5
Following a prenatal diagnosis, parents may seek information from their general practitioner regarding management and treatment during pregnancy and after birth.
Case study 1
Jenny is 22 weeks pregnant and presents to her GP. Her 20-week ultrasound identified that her baby has left congenital talipes equinovarus. No other abnormalities were identified. Jenny lives in a rural town with limited access to tertiary care and plans to deliver her baby at the local hospital. She has been searching the internet for information and is concerned about what to expect after delivery.
Question 1
What would you tell Jenny about congenital talipes equinovarus and its management?
Question 2
What intervention is required at this time?
Question 3
Where can Jenny source further information?
Answer 1
Prenatal education, reassurance and referral has the potential to ease parental anxiety and facilitate appropriate management for an optimal outcome. It is important to explain to Jenny that clubfoot is a treatable condition with excellent long term outcomes.1 There is no evidence that clubfoot is associated with any adverse affects on pregnancy, labour or birth outcomes.
The most common treatment for clubfoot is the Ponseti technique.11 This involves 4–6 weeks of long leg (toe-to-groin) plaster casts, changed weekly with gentle manipulation of the foot between casts to gradually correct the deformity. In the authors' experience, most babies are not unduly unsettled while wearing plaster casts and during cast changes. Following casting, most cases of clubfoot (80%) require an Achilles tenotomy (cutting of the Achilles tendon) to correct residual equinus deformity.1 This can be done under a local anaesthetic by an orthopaedic surgeon, either in the outpatient clinic or operating theatre, and does not require sutures. Following tenotomy, the lower limb is placed back into a long leg cast, which is left in place for 3 weeks. On removal of the final cast, the child is placed into an abduction brace (Figure 2) which is worn 23 hours a day for 3 months and then 14–16 hours, while asleep, until the child's fourth birthday. Compliance with the abduction brace is a major factor in reducing recurrent deformity12 and avoiding major surgical intervention.13 Long term outcomes following the Ponseti technique are excellent14 (Figure 3) compared to previous practice of major surgical intervention.15–17

Figure 2. Abduction brace (boots and bar)

Figure 3. Corrected bilateral clubfoot at 1 year of age
There is no evidence to suggest this treatment has an adverse effect on gross motor development18 and the authors' experience is that almost all children are able to participate in activity and sport without any problems. The treatment for clubfoot does not need to start on day one; several studies have suggested no correlation between the age at the start of treatment and outcomes.19 Most centres in Australia recommend beginning treatment within the first few weeks of life.
Answer 2
Jenny should be referred to a paediatric physiotherapist for prenatal advice about the diagnosis and management of club foot. Importantly, in some areas, particularly in rural areas where services are scarce, local physiotherapists may not be experienced in treating clubfoot. In these cases, the nearest tertiary hospital physiotherapy department can be contacted to provide further prenatal advice and make a plan to locate a suitable physiotherapist. In some cases, management of clubfoot may be shared between tertiary and local centres.
Answer 3
Jenny can be directed to major children's hospital websites for further information. The website www.aussieclubfootkids.org is run by parents of children with clubfoot and may be helpful. This site includes information, parent forums and contact details of orthopaedic surgeons and therapists around Australia who practise the Ponseti technique.
Case study 2
Megan has just given birth to her first child, Harry, via normal vaginal delivery. He was born at full term, with a breech presentation. His birth weight was 3.9 kg. The neonatal period has been uneventful, however the maternal and child health nurse has noted that Harry has bilateral clubfoot, which was not identified on prenatal ultrasound. Megan and her husband, Gary, present with Harry to their GP for further assessment and management.
Question 1
What assessment would you perform to determine whether Harry has postural or structural clubfoot?
Question 2
If Harry has postural clubfoot, what advice would you give to his parents?
Question 3
If Harry has structural clubfoot, what advice would you give to his parents?
Answer 1
In postural clubfoot the foot is structurally normal and, despite an abnormal resting position, is able to be passively corrected; ie. full passive range of movement of the foot is achieved, despite positional abnormality (Figure 4). It is considered to be a packaging defect, which develops during the third trimester of pregnancy. Most postural cases will present with an almost full range of movement at birth. In particular, one should be able to manipulate the foot into at least 10 degrees of ankle dorsiflexion.
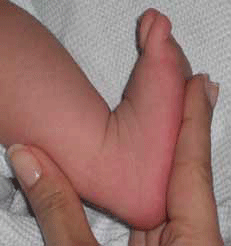
Figure 4. Postural clubfoot with normal passive range of motion
Answer 2
No treatment is required for most cases of postural clubfoot. Resolution often occurs within the first few weeks of life. However, severe cases which do not resolve within 1 month may actually represent mild structural clubfoot and referral to a paediatric physiotherapist is recommended.
Answer 3
In cases of structural clubfoot, education as per prenatal counselling should be given. There is no association between structural clubfoot and breech presentation. Treatment does not need to commence on day one, however immediate referral to a paediatric physiotherapist is required to facilitate coordination of further assessment and treatment plans.
Key points
- Congenital talipes equinovarus is a common paediatric orthopaedic condition.
- The Ponseti technique is the current gold standard treatment for clubfoot. It has led to favourable outcomes compared to previous surgical techniques.
- Prenatal education, reassurance and referral has the potential to ease parental anxiety and facilitate appropriate management for optimal outcomes.
Conflict of interest: none declared.
References