Learning in the community is increasingly seen as an important component of undergraduate medical education in Australia. This has been driven by factors that include increasing medical student numbers,1 high patient acuity in tertiary hospitals2,3 and recognition of the importance of generalism as an attribute of medical practitioners.4–6
Community based medical education in rural settings is now well established in rural and remote centres across Australia, supported by Commonwealth Government funding.7 Rural general practitioners and visiting specialists are key players in the success of the rural clinical schools, which provide medical students with broad clinical training based in rural practices and local hospitals. In urban areas, CBME as an alternative to traditional tertiary hospital teaching is not yet well established or supported by infrastructure funding.
Most urban general practice placements have traditionally focused on introducing students to general practice, rather than the provision of broader clinical training. While urban general practice allows students to understand the epidemiology of illness in the community, by itself, it may not provide the breadth of clinical exposure and training in different disciplines required to meet curriculum objectives. Although many urban GPs have special interests in diverse areas of medicine such as women’s health, skin cancer and sports medicine8 they may be less connected to hospitals and emergency departments than their rural colleagues.
Early evidence from rural clinical schools shows that training location can influence geographical location of future practice.9 Suburban areas of low socioeconomic status,10 while not suffering the tyrannies of distance that rural areas face, are often relatively underserved compared to more affluent areas. Community based medical education in these areas could potentially influence future practice location and help address poor access to health services.
In 2009, Flinders University established a pilot suburban CBME program in a relatively disadvantaged area11 in outer suburban Adelaide (South Australia). The program was designed to take the principles of CBME (continuity of supervision and contact with patients), which have been shown to be effective in the rural setting, and apply these to an urban setting. Because of the differences between urban and rural practice, a new approach was required. A pilot program was designed, which combined a longitudinal placement in general practice with clinical experience in a community hospital and emergency department (ED). This was seen as providing continuity with a set of clinical supervisors (ED and general practice) and the potential for continuity of patient contact across the region’s health services.
The pilot ran for 2 years, providing a yearlong integrated clinical placement. The ED and general practice placements were successful and achieved the aims of the program, but specialist clinicians expressed dissatisfaction with the lack of consistent contact with students. The program was modified and expanded, and the OCEP was formally launched in 2011. This article describes the pilot and the influence of student, GP, specialist and other stakeholder groups in shaping the formal OCEP 2011 program.
The Onkaparinga Clinical Education Program pilot 2009–10
The OCEP pilot was designed initially12 to replicate the Flinders University Parallel Rural Community Curriculum (PRCC)13 experience as much as possible using integrated clinical placements. These have been shown to be as effective at producing academic success as traditional block placements.14
In 2009, eight students undertook their entire third year of the Flinders Graduate Entry Medical Program at the OCEP. Students spent two sessions (half days) each week with the same general practice, and two sessions per week in the ED at Noarlunga Hospital, a community hospital of 111 beds. These placements provided students with the opportunity to develop and practise core skills and clinical reasoning. Specialty placements in hospital and community settings complemented the ED and general practice placements, and regular tutorials were held throughout the year. Figure 1 shows that in an average week students spent their time spread evenly between general practice, ED, formal learning sessions and specialty practice. In 2010, although seven student placements were available, one student was unable to take up their place, thus six students undertook the same program as in 2009.
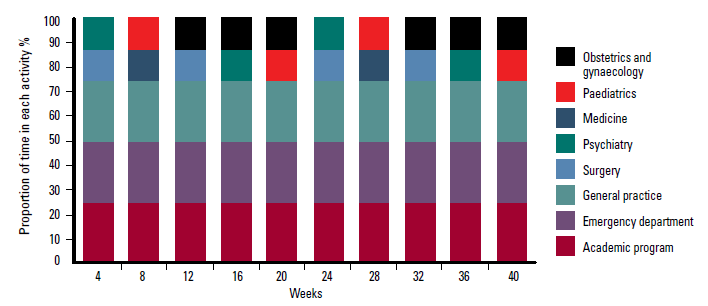
Figure 1. Typical student program in the Onkaparinga Clinical Education Program pilot 2009–10
The program was managed administratively by one full time administrator, and academically by one GP clinical educator (the academic coordinator) with input from visiting specialists.
Stakeholder perspectives on the pilot program
During the first half of 2010, the academic coordinator held face-to-face meetings with as many people who had been involved in 2009 as possible. This included GPs, practice staff, hospital staff, private specialists, university academic and administration staff and students. Evaluation via surveys was also undertaken with clinicians in both hospital and private practice, and with students through routine course evaluation. This provided five key perspectives that informed the OCEP’s further development – those of GPs, students, specialists, ED clinicians and program administration staff.
General practitioners
General practitioners found the longitudinal placements more rewarding than shorter attachments, and the opportunity to watch a student’s progress was highly valued. Placements worked particularly well if several GPs from a practice participated in the teaching role, although this was not an essential requirement. Some GPs, usually those with less support from other practice members, felt that 40 weeks could be too long and made it difficult to take leave during the year.
Parallel consulting, where the student sees a patient on their own in a separate room while the doctor is seeing another patient, has been shown to decrease some of the time pressure on GP preceptors.15 Lack of space to provide parallel consulting opportunities was a common issue, limiting the number of sessions that were made available for clinical training. Comments from GPs included:
‘ I enjoyed having a student last year and watching him develop.’
‘ [The program provides] potential for integrated community/hospital understanding of healthcare.’
‘ Continuity benefits both the practice and student, aids familiarisation.’
‘ [Students have] exposure to ‘normal patients’ rather than hospitalised, chronically ill patients.’
Although three new practices were recruited for 2010, four of the initial eight GPs withdrew at least temporarily from the program, one through ill health, two to take on a general practice registrar, and one through feeling ‘burned out’ by 40 weeks of teaching. Two of these GPs rejoined in the new 2011 program.
Students
The pilot program was well received by students, although they were initially anxious. Preliminary comparison of academic results achieved by OCEP students and the whole of class results (includes Flinders Univeristy students at tertiary hospitals, rural clinical schools and the Northern Territory) when sitting the same end of year examination showed no difference in exam performance. This will be formally evaluated at the end of 2012. Student interest in the program was evident from the high number of students choosing the OCEP as their first preference for their year 3 program in 2011. Students liked being actively involved, rather than just sitting and watching and they commented that the longer placements enabled them to earn the GP’s trust to allow them to be active participants. The ED provided the students with the opportunity to see acute medicine and to see patients at initial presentation. Students found the need to move between several different locations for placements somewhat stressful and transport related issues were common.
Specialists
Specialists who supervised OCEP students in the pilot program, both at Noarlunga Hospital and in private practice, were not as well engaged with the program as the GPs. They found OCEP placements less satisfying than familiar hospital block rotations, and felt that the intermittent and brief nature of the pilot specialty placements did not allow them to develop any meaningful student-teacher relationships.
The lack of funding and infrastructure to support the teaching role was another recurring theme in this group.
Emergency department and hospital staff
Many of the hospital staff enjoyed teaching.
‘ Long term involvement enables us to get to know them, their strengths and weaknesses and to supervise accordingly.’
‘ Extended placement allowed them to integrate into the clinical team and clinicians could observe the development of their practice.’
However, there was concern about the additional workload created by student placements.
‘ Produced stress on ED during busy times.’
Program administration staff
Rostering students across many different activities and ensuring equivalence of clinical exposure, while juggling frequent changes to consulting times and supervisor availability, is a difficult and time consuming task.
Maintaining the OCEP requires liaison with many unique clinical organisations and individuals. It also requires tailoring of each small component of the program to suit the specific situation. While this was possible with eight students, any increase in student numbers required a different approach for the program.
The Onkaparinga Clinical Education Program 2011
The OCEP 2011 was designed to incorporate the positive aspects of the pilot, address some of the issues that had been raised by stakeholders, and accommodate a much larger group of students. The new program, which accommodates 24 students for a full year, consists of a half year longitudinal, community based program combined with a half year program of specialty rotations, which are based in the community as much as possible. The academic program continues to be integrated across the full year, ensuring all OCEP students come together each week for tutorials with GPs and specialists. The program is located in a purpose-built Commonwealth Government funded facility opposite Noarlunga Hospital.
Moving to the hybrid program has allowed the OCEP to offer more flexibility for GPs to be involved, as they can choose to teach for either of two 20 week semesters, or for the full, year. It has also enabled the specialist teaching resources to be used more fully and effectively, with an opportunity for student-teacher relationships to develop. It has allowed improved structure to be brought to the administration of the program, although the task is still very detailed and time consuming. Together these changes have made it possible to increase the program to 24 students.
The major components of the OCEP 2011, as illustrated in Figure 2 are:
- longitudinal general practice, ED and community specialist placements (20 weeks)
- five blocks of specialty rotations of 4 weeks in each of surgery, internal medicine, psychiatry, women’s health and paediatrics (total 20 weeks)
- longitudinal academic program (40 weeks).
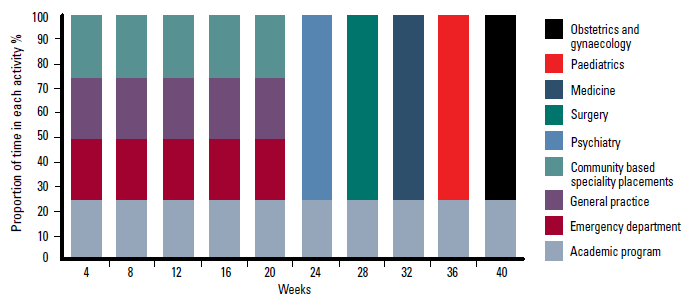
Figure 2. Typical student program – Onkaparinga Clinical Education Program 2011
The community semester consists of general practice, ED and community based specialty placements. For 20 weeks, students spend two or more sessions per week in general practice with a GP preceptor and two sessions per week in ED. Other placements are arranged in specialist areas and in fields such as aged care and Aboriginal health.
In the specialties semester, students undertake five blocks of 4 weeks each. Psychiatry, surgery and medicine are undertaken at Noarlunga Hospital. These rotations include attachments in community and private specialist practice. Students return to Flinders Medical Centre (a tertiary centre) for paediatrics and women’s health rotations.
The academic program runs longitudinally throughout the year and includes problem based and case based tutorials and specific skills training sessions. The students undertake the same assessments as all year 3 Flinders University medical students.
As a member of the Training for Health Equity network,16 Flinders University School of Medicine has a strong focus on social accountability and in keeping with this, the OCEP 2011 required students to participate in a community activity that provided some benefit to the community. Examples in 2011 included health education for high school students and falls prevention community education. The OCEP is located in an area of relative socioeconomic disadvantage, and is in the early stages of developing a long term plan to work with staff and students at the local high school.17
Discussion
The experiences of the OCEP have highlighted some of the issues that need to be addressed to enable further development of the urban CBME model. A cycle of evaluation and reflection has led to modifications that better balance longitudinal placements with experiences in hospital specialties.
General practice
Precepting can provide significant benefits for GPs, including professional enrichment and enjoyment of the positive aspects of the studentteacher relationship.18 Growth of the OCEP in the pilot program model was limited initially by the difficulty of recruiting GPs to undertake a new type of teaching role over an extended time. A commitment to 40 weeks of teaching was sometimes difficult. By decreasing the longitudinal component to 20 weeks, GPs could choose to teach for the full year, or for one semester only. Most GPs teach for the full 40 weeks, but know there is the option for less if they wish.
Lack of infrastructure is a significant obstacle to suburban general practice teaching.19 Ideally, students should have general practice placements of four sessions per week to enable all the benefits of the symbiotic model described by Worley et al.2 Urban CBME would benefit from funding to provide infrastructure for teaching space and parallel consulting as has occurred in the rural CBME model. General practitioner teachers who do not have the opportunity to use parallel consulting consistently report that teaching students costs them time and decreases their consultation rate.20 As the strengths and benefits of the program become apparent, it is hoped that more funding will become available.
Specialties
The introduction of 4 week specialty rotations has enabled OCEP specialists to be more engaged in the program. They have a 4 week intensive block in which to develop their own student-teacher relationships and obtain greater satisfaction from teaching, which was not possible in the earlier model where they had intermittent student contact. Many specialists currently participate in the OCEP altruistically (the Practice Incentive Payment does not apply to specialist practice). As with GPs, it is expected that improved funding and infrastructure would help to strengthen this component of urban CBME and help it to grow.
Evaluation
As discussed, initial evaluation of the pilot resulted in significant restructuring of the program. Formal evaluation of the 2011 program is currently in progress and will look at all aspects of the program and seek input from all stakeholders. In addition, comparison between the pilot and the new program will be made where possible. It is hoped that this will clarify the strengths and weaknesses of the program, and help to inform the future design of urban CBME.
Summary
There is a wealth of clinical learning potentially available for urban CBME programs based in general and private specialist practices, and in community and private hospitals. Flinders University has offered a hybrid urban CBME program in Darwin since 2008,21 The University of Melbourne is currently piloting an urban CMBE program called ‘The Crescent,’22 and the University of Queensland is piloting a program called ‘Urban LinCc’.
The OCEP case study has demonstrated a new approach to CBME that provides medical students with longitudinal clinical experiences grounded in the community setting and with general practice at its core. The program has successfully grown from eight to 24 students between 2009 and 2011, has purpose built teaching accommodation, two full time equivalent (FTE) academic/clinical educators (one full time and six fractional appointments including GPs and specialists) and 2.6 FTE administration staff. There are now 16 general practices involved, ranging from solo GPs to large group practices. Around 35 private specialists and eight community and allied health services offer clinical placements. Noarlunga Hospital staff offer surgical, medical, psychiatric and ED placements. The OCEP provides a viable model for urban CBME, offering an integrated curriculum combining continuity of supervision in general practice and ED with focused placements across the core specialties.
Despite the achievements to date, the program remains vulnerable. Its reliance on goodwill gives it the strength of committed and enthusiastic teachers, as well as the weakness inherent in reliance on goodwill. Its competition with other teaching programs such as general practice registrar training, and general practice based junior doctor training adds to its vulnerability, as does the inflexibility of the Practice Incentive Payment and lack of funding for nonaccredited or non-GP clinical supervisors.
It is hoped that new opportunities and models may be possible in the future through Health Workforce Australia funding.23 Improvements in funding for infrastructure and better financial models to reward clinical teachers in private practice will help to harness this rich resource for education. In return, local communities are likely to benefit from greater retention of doctors in relatively disadvantaged areas, and the local clinical community could benefit from the academic and teaching presence,24,25 as has happened in rural areas.
Key points
- Urban GPs can provide teaching and clinical experience for medical students across much of the curriculum.
- Longer placements allow students to become more actively involved in seeing patients.
- A mix of urban general practice and ED placement exposes students to primary patient presentations across the acuity range.
- Infrastructure to support the parallel consulting model would ameliorate the time cost of student teaching in general practice.
- Precepting can provide significant benefits for GPs, including professional enrichment and enjoyment of the positive aspects of the student-teacher relationship.
References