Case study
Figure 1 demonstrates the use of this technique to repair a helical rim defect following excision of melanoma in situ (Figure 1a) in a man aged 73 years. Stages involved in this procedure were as follows.
- The scar was excised (Figure 1b).
- A retroauricular skin flap was created (Figure 1c).
- The skin flap was doubled up into a roll to simulate the rolled appearance of the helical rim (Figure 1d).
- This roll was sutured into the surgical defect (Figure 1e).
- The ear was pinned back to the retroauricular area to avoid inadvertent pulling of the ear, which can damage the flap.
- The flap was allowed to heal for 2 weeks (Figure 1f) and was then divided.
- As the retroauricular skin was slow to granulate (Figure 1g), an S plasty was performed for a direct closure.
- A satisfactory outcome was noted after 3 months (Figure 1h).
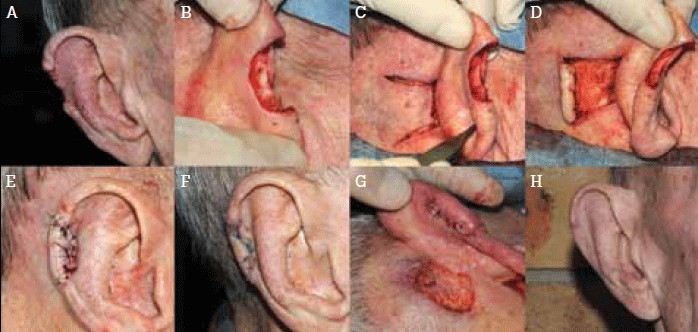
Figure 1. Repair of a full thickness surgical defect of the helical rim using a retroauricular skin flap
Skin cancers are commonly diagnosed and managed in the general practice setting1 and are most prevalent on sun exposed areas such as the ear.2 A cosmetically satisfying result following excision of a skin cancer from this area and reconstruction of the anterior surface and helix of the ear can be difficult to achieve due to limited availability of skin. Some patients may be unconcerned by a postoperative defect or prefer not to undergo further surgery. Others may benefit from surgical options that have the potential to improve the cosmetic outcome.
Various surgical options are available to repair surgical defects of the ear including wedge excision3, local flap surgery (using skin from same anatomical unit) and skin grafting. Cosmetic outcomes with these methods are generally very good; however they can cause the affected ear to look smaller postoperatively. This may be particularly noticeable when the defect is on the helical rim. One option to prevent this complication is to fill the surgical defect with a distant flap using the soft tissue outside the ear such as from the retroauricular area.4–7
Retroauricular cutaneous advancement flap
Retroauricular soft tissue is geographically located close to the ear, thus a skin flap of this region can easily be advanced to fill soft tissue defects. This area is well vascularised6 and its close proximity to the ear enables flap length and movement to be minimised, which reduces the vascular burden of the flap. The flap donor site scar can be easily concealed behind the ear.
One disadvantage of this technique is that a two staged procedure is required with the first stage to create the flap and the second to divide the flap at a later date. Also the donor site wound may require repairing. However, it is a relatively simple procedure of skin advancement flap with numerous advantages: good match of skin colour and texture, better ear profile, and avoidance of miniaturisation of the ear.
Several factors need to be taken into consideration and customised for a retroauricular advancement skin flap to be successful.
Stage 1: Flap creation
Flap length: Correct approximation of flap length is important. In general, the flap will need to be at least 2 mm longer than the surgical defect to be filled. However, when it is intended to be rolled up to reconstruct a helical rim defect, it will need to be approximately 4 mm longer than the anticipated length. Overlengthening of the flap should be avoided as this can cause devascularisation.
Flap thickness: Thick retroauricular soft tissue enables the operator to produce a flap of varying thickness to match the surgical defect of the ear (Figure 2). The flap can be rolled up and thickened to recreate a helical rim or its distal end can be thinned to avoid step deformity. The use of a wide based pedicle will maximise the available blood supply from the richly vascular retroauricular skin.
Flap tension: The tension placed along the flap can be reduced by immobilising the ear to the mastoid process by suture fixation. This prevents inadvertent pulling of the flap.
Haemostasis: Meticulous haemostasis is essential in any surgery but it is particularly important in the ear and the periauricular region as haematoma and delayed haemorrhage can occur, causing significant patient distress.
Postoperative: A compression dressing should be applied and the dressing left intact for 1 week, after which the wound can be showered and cleansed daily.
Stage 2: Dividing the flap and repairing the secondary defect
Timing: It is important to leave the flap for at least 2 weeks before dividing it and detaching it from the retroauricular skin. This allows for adequate collateral revascularisation, which is essential in preventing flap loss.
Secondary defect: The longer you leave the second procedure, the more granulation will have taken place in the secondary defect. Smaller secondary defects (2 cm) close completely in 2 to 4 weeks. A delay between the first and second procedure of greater than 2 weeks is advantageous as the second stage procedure can then be performed relatively quickly and easily. If the secondary defect is large and/or if the wound bed is slow to granulate, this defect should be closed by primary intention.
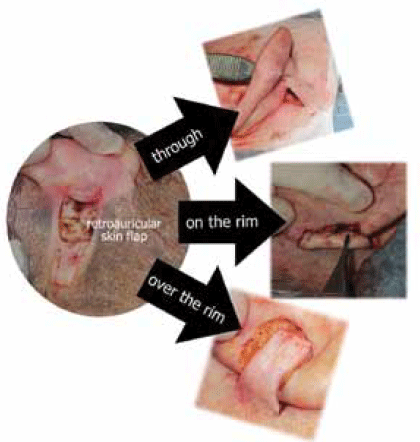
Figure 2. Applications of retroauricular advancement flap to fill the surgical defects of the anterior surface and helix of the ear
Conclusion
A retroauricular cutaneous advancement flap is an option for patients who require cosmetically satisfying reconstruction of the ear post skin cancer excision. The technique can avoid the miniaturisation of the ear that may occur with other techniques.
Conflict of interest: none declared.