The causes of hand injuries are varied and include sporting accidents, occupational injuries and bites of various types. This article provides a brief guide to the assessment of hand injuries and outlines the general principles of management for any hand injury followed by more specific detail about common injuries and their management. The aim is not to cover each injury in detail, but to provide a framework so that the general practitioner can confidently assess hand injuries and know which injuries they can manage in their practice and which should be referred to a hand specialist. #
Principles of assessment
History
Mechanism of injury
The mechanism of injury gives important clues about the structures involved and potential complications. It is important to establish what forces were applied to the hand during the injury and the direction of these forces, as well as any special features of the injury. For example, a bite to the hand conveys a high risk of developing infection; a history of a missed tackle (‘grabbing a jumper’) may cause a flexor tendon injury. Blunt trauma causes quite different injuries to penetrating trauma. A history of dislocation and reduction before presentation is important, as this may not be detected on examination.
Previous injuries
A history of any previous hand injury may predispose to further injury and may also mean the ‘normal’ hand for comparison is actually abnormal.
Clinical context
Is this the patient’s dominant hand? What is their occupation, sporting interests, hobbies or other important hand related activities? How crucial is optimal hand function for this person? Occasionally lacerations of the hand can be self inflicted, necessitating psychological assessment and management. Many hand injuries also have legal ramifications if sustained during intrapersonal violence or in the workplace.
Examination
The anatomy of the hand is complex (Figure 1a, b) and an understanding of all its structures is vital. In addition to the general principles common to the assessment of any injury, there are particular issues relevant to examining hand injuries.
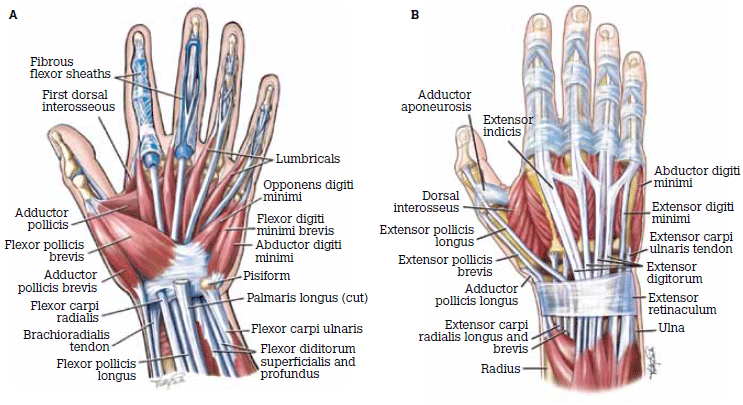
Figure 1. Anatomy of the hand A) Volar aspect; B) Dorsal aspect
Reproduced with permission: Brukner P, Khan K. Clinical Sports Medicine. 3rd edn. Mc-Graw Hill, 2006
Inspection
Observe carefully for bruising, swelling and lacerations. Swelling can be a hallmark of bony injury. Carefully inspect any lacerations, keeping in mind that deeper structures may also be damaged.
Sensation and circulation
Before injecting any local anaesthetic, test for sensation to pain and light touch; check capillary refill and circulation.
Range of motion
Examine the full range of motion of all joints actively and passively comparing with the other hand and the expected range for each joint.
Rotational deformity of hand fractures can only be assessed clinically. All fractures with rotational deformity require surgical evaluation. Assess metacarpal rotation by checking a relaxed fist (Figure 2a, b). Assess rotational deformity of the phalanges by examining the fingers end-on with distal interphalangeal (DIP) joint and proximal interphalageal (PIP) joint flexion.2
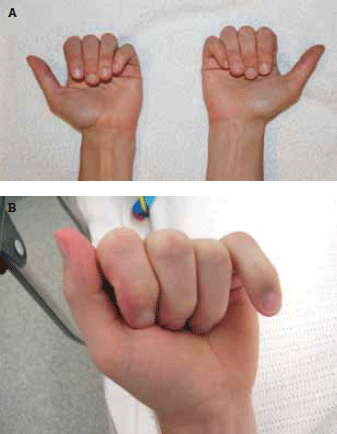
Figure 2. A) Normal hands. The fingers should sit next to each other without overlap, fingernails pointing in the same direction. As a normal variation, the fifth finger can rotate inward and sit under the fourth finger
B) Malrotation of the fifth finger
Resisted movement
The integrity of all tendons needs to be established. Assess flexor digitorum profundus (FDP) (Figure 3a) and flexor digitorum superficialis (FDS) (Figure 3b) separately. If the ability to flex against resistance is absent or reduced, there is tendon damage. Another clue suggesting tendon injury is when resistance cannot be generated due to pain, particularly if the pain is in excess of expected.
Check the integrity of interphalangeal joint ligaments by stressing the joint into ulnar and radial deviation and also in anterioposterior direction. Pain, laxity and loss of the firm-end-feel suggest ligament injury. The PIP joint collateral ligaments should be checked with the joint in 30 degrees flexion and with the metacapophalangeal (MCP) joints flexed to 90 degrees.3
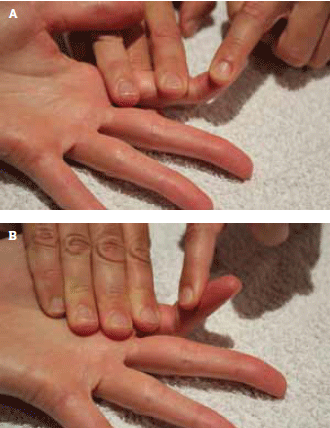
Figure 3A) Digitorum profundus (FDP); B) Digitorum superficialis (FDS)
FDP is assessed by stabilising the PIP joint and testing ability to flex the distal phalanx with and without resistance FDS is assessed by stabilising the MCP joint and testing ability to flex the finger with and without resistance
Investigation
A low threshold for ordering plain X-rays is appropriate, as fractures (particularly avulsion fractures) are difficult to detect clinically. A history of dislocation always requires an X-ray, as associated fractures are common. Grossly displaced fractures are often mistaken for ‘reduced’ dislocations.
Principles of management
Immobilisation
The hand is highly susceptible to permanent loss of joint range with immobilisation. Therefore the duration of full immobilisation is much less than for other fractures, and early movement is promoted through exercise and dynamic splints.4
The position of immobilisation is important. The ‘safe’ position of the hand (Figure 4) is designed to prevent joint contractures by maintaining the MCP joint collateral ligaments on stretch and preventing volar plate contraction (Figure 5). Where possible, minimise the number of joints immobilised.
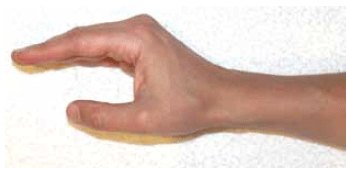
Figure 4. The safe position of the hand for splinting – a minimum of 70 degrees (MCP) joint flexion, minimal (PIP) joint flexion and 30 degrees of wrist dorsiflexion
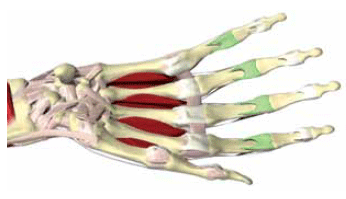
Figure 5. Hand with volar plates at PIP highlighted. The volar plate is a thick fibrocartinolginous structure that reinforces the palmar surface of the interphalangeal joints and prevents hyperextension
Reproduced with permission Primal Pictures. Available at www.primalpictures.com
Hand therapy
Hand therapists are occupational therapists or physiotherapists who specialise in injuries to the upper limb.5 They can tailor a rehabilitation program to individual patient’s needs. Therapy involves the provision of splints, exercises and a range of other specialised treatment techniques to restore function. Hand therapists can be located through the Australian Hand Therapy Association (www.ahta.com.au) and can be found in private practice (often co-located with hand surgeons) and in public hospitals.
Review
Hand fractures are highly prone to displacement (Figure 6a, b) due to the opposing pull of tendons and lack of muscles bellies in the finger. Therefore, most hand fractures require at least one follow up X-ray approximately 1 week after the injury.2,6
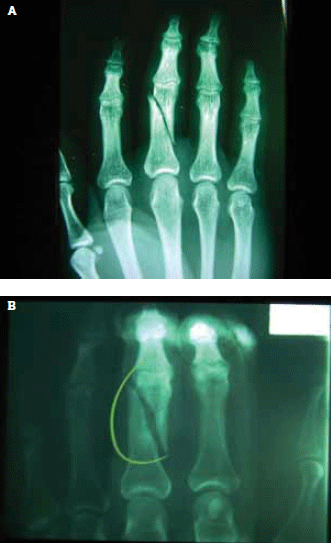
Figure 6. A) Fracture of middle phalanx fracture initially and B) 1 week later showing further displacement
Managing common injuries
Fractures
Details of specific fracture management are summarised in Table 1.
Table 1. Fracture management
| Fracture | Period of full immobilisation | Position of immobilisation | Criteria for referral | Important notes |
|---|
| Proximal phalanx |
Up to 3 weeks |
Safe position |
- Intra-articular surface involvement >30%
- Unstable fractures
– rotation
– excessive angulation*
- Multiple fingers
|
- Review X-ray in 1 week
- Begin active exercise early
|
| Middle phalanx |
Up to 3 weeks |
Interphalangeal joints in extension† |
- Intra-articular surface involvement >30%
- Unstable fractures
– rotation
– excessive angulation*
- Multiple fingers
|
- Review X-ray in 1 week
- Begin active exercise early
|
| Volar plate avulsion fracture |
1 week |
Slight flexion or use an extension blocking splint |
- Large avulsion fragmen
- Fragment within joint space (passive range of motion reduced)
|
- Flexion exercises commence at 1 week with intermittent splint
- Extension exercises commence at 3 weeks
|
| Distal phalanx |
2–3 weeks |
L-shaped splint to protect soft tissue |
- Large loss of soft tissue
- Intra-articular surface involvement >30%
|
- Usually stable fractures
- Often crush injury mechanism
- Treat associated nail injury#
|
| Mallet fracture |
6–8 weeks |
DIP joint in slight hyperextension |
- Avulsion fragment >30% of articular surface
|
- Patient education regarding the wearing of a splint
|
| Metacarpals 2–515,14 |
3–4 weeks |
Safe position MCP at 90 degrees |
- Rotation
- Angulation >10 degrees for metacarpals 2 and 3
- Angulation >20–30 degrees for metacarpals 4 and 5
- Open fracture
- Multiple metacarpals involved
|
- Repeat X-ray at 1 and 2 weeks
- After 3–4 weeks active exercise and intermittent splinting/supportive bandage
- Resume contact sport in 6–8 weeks
|
* Closed reduction of displaced fractures can be attempted, but most require close X-ray monitoring as they have a tendency to displace
† Some authors advocate buddy taping, however, the different levels of PIP joints can create rotary force. Buddy taping can be useful when beginning to mobilise
# Lacerations of the nail bed need to be repaired to avoid future nail deformity. Suspect nail bed laceration if the haematoma is >50% of nail surface or the nail itself has been fractured.9 Haematomas can be drained via piercing the nail with a hot paper clip. However, this converts the fracture to an open fracture, potentially changing management |
Finger fractures
In general, closed and minimally displaced fractures with good alignment can be treated conservatively.4 Phalangeal fractures are fully immobilised for a maximum of 3 weeks2,4,6 followed by reduced immobilisation and active exercise. Unstable fractures require referral.
Volar plate avulsion fracture (Figure 7) occurs after hyperextension injury to the PIP joint, often from a ‘jamming’ injury during ball sports. This type of fracture is common but easily missed2 and, unfortunately, permanent loss of PIP joint function results from mismanagement. Treatment involves several stages of exercise prescription and an extension block splint, ideally under the supervision of a hand therapist.
Transverse fractures require reduction and immobilisation in a thumb spica cast.
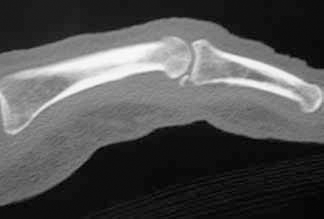
Figure 7. X-ray demonstrating a volar plate avulsion fracture
Joint injury
Proximal interphalageal joint
Dislocation of the PIP joint most commonly occurs dorsally from hyperextension stress. An X-ray should be performed before and after reduction. However, in practice, most of these dislocations are already reduced before presentation. Treat fractures as required. For dislocation to have occurred, the volar plate and collateral ligaments will have been damaged. If after reduction:
- the joint dislocates with active movement, complete rupture of all of these structures is likely and referral for repair is required
- the joint hyperextends, treat as for volar plate avulsion fracture
- there is no hyperextension, splint PIP joint in slight flexion for a few days followed by buddy taping.2
Volar dislocations usually require referral for reduction. If seen after reduction they need to be treated to prevent a boutonnière deformity (Figure 8).
The PIP joint collateral ligaments can also be sprained from a sideways force. Partial tears can be treated with buddy taping for several days followed by early active exercise.
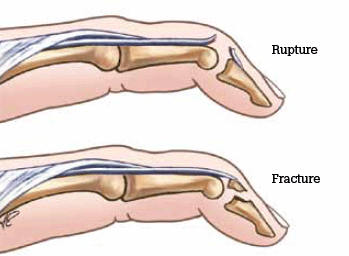
Figure 8. Mallet finger deformity
Reproduced with permission: Brukner P, Khan K. Clinical Sports Medicine. 3rd edn. Mc-Graw Hill, 2006
Distal interphalangeal joint
Injury to the DIP joint often involves extensor tendon damage (See mallet finger deformity). Dislocations are less common and usually occur dorsally.7 After reduction, splint the DIP joint in slight flexion for 2–3 weeks.
Metacapophalangeal joint
The MCP joint of the thumb is commonly injured. Sprain of the ulnar collateral ligament (UCL) – or ‘skier’s’ thumb – though more often seen in ball sports, occurs from forced abduction and hyperextension of the MCP joint. An X-ray is required before assessment of a UCL as any associated fracture is a contraindication to stress testing.
Stress the UCL with the joint at 30 degrees flexion and at full extension. In complete rupture there is loss of end-feel and more than 10–20 degrees of deviation in both positions when compared to the other side. Pinch grip (grasp between thumb and index finger) will be painful and weakened. There may be a painful lump on the ulnar side of the joint due to the ruptured ligament sitting outside the adductor aponeurosis (Stener lesion).8
Complete rupture of the ligament is unstable and requires surgical repair. Partial tears are immobilised with a splint for 6 weeks with the MCP joint in slight flexion. Chronic forms of this injury are also common and are known as ‘gamekeeper’s thumb’.
Injury to the radial collateral ligament of the first MCP can also occur and is treated similarly. Complete rupture does not automatically require surgery, as no Stener lesion forms.
Metacapophalangeal joint dislocations usually require referral for enlocation.
Tendon injuries
In general, acute tendon injuries require surgical evaluation. Exceptions include some of the common extensor tendon injuries detailed below.
Extensor tendon – mallet finger
Injury to the extensor digitorum at its distal insertion occurs when the joint is forced into flexion while being actively extended (eg. a ball hitting the end of an outstretched finger). The patient may not present with a typical ‘mallet finger’ injury deformity (Figure 8). It is therefore important to isolate the DIP joint during resistance testing so that injury is not missed.
An X-ray should be ordered, as mallet finger can occur with an avulsion fracture. Surgery is required when an avulsion fracture involves more than 30% of the articular surface or if there is joint subluxation. Otherwise, mallet finger deformity responds well to conservative management.
Maintain the DIP joint in slight hyperextension via a splint for a minimum of 6 weeks. It is crucial to maintain extension at all times, even when removing the splint for hygiene purposes.9 Patients must be aware that failure to do this will result in permanent joint deformity. While research9 indicates similar outcomes for various splints, premade splints are only available in a small range of sizes, and custom made splinting may be required. After 6 weeks, check for active pain free extension and then begin intermittent splinting and active rehabilitation.
Treatment of mallet finger deformity can be successfully implemented up to 3 months after the initial injury.10,11
Extensor tendon – Boutonnière deformity
Injury to the central slip of extensor digitorum occurs from a direct blow to the PIP joint, or from the same mechanism of injury that causes mallet finger deformity. The patient initially presents with pain but no deformity. The injury is detected by examining active finger extension: the PIP joint will lag behind the DIP joint and full range can be lost.
Point tenderness over the dorsal PIP joint may be present. The lag can be subtle and any suspicion of this injury requires treatment. Failure to detect this injury results in the ‘boutonnière’ (Figure 9) or ‘swan neck’ deformity over time.
Surgery is required if there is associated intra-articular fracture of >30%. Treatment involves splinting the PIP joint in full extension while allowing DIP joint flexion for 6 weeks. Intermittent splinting and active rehabilitation is then required.
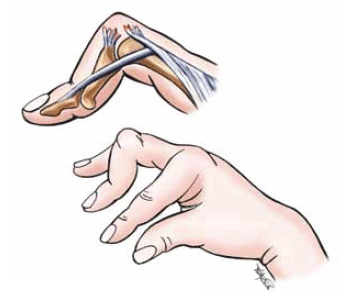
Figure 9. Boutonnière deformity
The rupture of the central slip of extensor digitorum from its insertion allows the lateral bands to migrate in a palmar direction. In turn, the middle phalanx is then pulled into flexion by FDS; the PIP joint herniates through the central slip tear
Reproduced with permission: Brukner P, Khan K. Clinical Sports Medicine. 3rd edn. Mc-Graw Hill, 2006
Flexor tendon injury
Injury to the FDP most commonly occurs at the fourth finger, as it is the weakest. Mechanism of injury is classically a grabbing incident, such as a missed tackle. Often the patient presents with the finger in relative extension to the others, and there is an inability to flex that finger. Order X-rays, as associated avulsion fracture is common. Immediate referral to a hand surgeon is required as these injuries are irreparable after 7–10 days.
Lacerations
Lacerations to the hand require exclusion of damage to underlying structures. Examine movement and sensation before the infiltration of local anaesthetic. Careful wound exploration can then take place. An X-ray should be performed if the mechanism of injury suggests a fracture is possible.
Excessive pain with active and resisted movements is suspicious for tendon injury. If unsure about tendon integrity, re-evaluate in 2–3 days. Surgical referral is required for a compound fracture, tendon or nerve injury.
Simple lacerations should be copiously lavaged and irrigated then sutured loosely to allow ooze. Although normal saline is traditional, there is evidence12 to suggest that drinking-quality tap water is a viable option. Delayed closure is accepted practice in wounds that present after 6 hours of injury. Antibiotics should be prescribed as per antibiotic guidelines13 and tetanus toxoid administered as necessary.
Bites
Bites with fracture require referral for surgical washout and antibiotics. A bite wound should not be primarily closed. Instead lavage copiously, prescribe antibiotics, ensure tetanus cover and review.13,14 For human bites, also consider the patient’s hepatitis B status. If the wound is clean in 3 days, it can be loosely sutured but ongoing review should continue.
Conflict of interest: none declared.
Acknowledgement
I would like to thank Mr Stephen Tham for provision of some of the images and general discussion.
References