The condition
Knee osteoarthritis is the most common cause of knee pain in people over 50 years of age. Malalignment of the patella, with abnormal distribution of force on the lateral facet, is thought to contribute to pain in knee osteoarthritis.
The intervention
The application of strong adhesive tape or strapping, aiming to realign the patella and unload painful soft tissue.
Taping is a very effective pain-relieving strategy and can assist participation in other strongly recommended therapies, such as cardiovascular and resistance land-based and aquatic exercises, for knee osteoarthritis.
Preparing to tape
Tape is applied before painful activities, such as exercise; however the tape can be left in place for days to weeks depending on adhesion durability. Before applying tape it may be necessary to shave the skin and this should be done 12 hours before applying tape. Ensure the skin is thoroughly cleaned and dried before applying tape.
Ask the patient to perform a symptom-provoking activity such as a step down before applying the tape so that the level of pain can be re-assessed following tape application. Better results will be obtained if immediate reductions in pain can be obtained with tape.
Apply the tape with the patient either lying or sitting on the edge of a chair with the leg extended and the thigh muscles relaxed.
Several different taping methods can be used. The choice depends on which combination is most effective at reducing the patient’s pain. Prior to placing each piece of rigid tape, place several strips of hypoallergenic tape across the knee region to cover the patella and the medial and lateral knee regions.
A 2–3-step method
The taping method, described below, consists of steps 1 and 2 with or without step 3.
1. Medial tilt and medial glide
Start the tape in the middle of the patella, at the level of the superior aspect of the patella, lift the skin on the medial side of the knee towards the patella and pull the tape medially. Fix the tape to the medial aspect of the knee just short of the hamstring tendons ensuring there is some slight wrinkling of the skin (Figure 1). This tilts the lateral patellar border away from the femur.
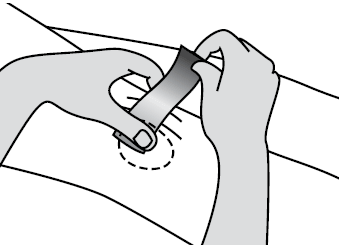
Figure 1. Medial tilt and medial glide
2. Anteroposterior tilt and medial glide
Start the rigid tape on the lateral aspect of the knee at the level of the superior aspect of the patella. Gently lift the skin on the medial side of the knee towards the patella as you pull the tape medially. Fix the tape to the medial aspect of the knee just short of the hamstring tendons ensuring there is some slight wrinkling of the skin (Figure 2).
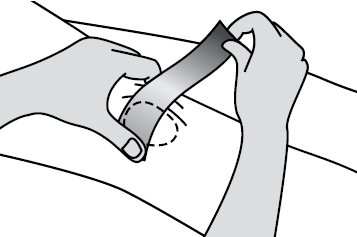
Figure 2. Anteroposterior tilt and medial glide
3. Unloading the infrapatellar fat pad and reducing stretch of inflamed soft tissues
Commence the tape at the tibial tubercle and lift the soft tissue towards the patella, while firmly pulling the tape to the medial joint line. Repeat with a second piece of tape but firmly pull the tape toward the lateral joint line (Figure 3).
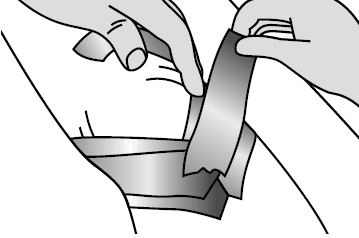
Figure 3. Unloading of the infrapatellar fat pad
What should I consider?
A physiotherapist experienced in assessment and taping techniques should show the patient how to apply the tape as precise placement is needed for maximum benefit.
Taping is not recommended as a sole intervention, and exercise programs and weight loss (for overweight patients) are strongly recommended in conjunction with any other therapy.
Skin care is important. Use hypoallergenic tape to protect the skin from direct contact with rigid strapping tape. The majority of skin damage is done during tape removal, so remove and re-apply tape less frequently in older patients. Ensure that the tape is removed slowly and carefully. Hand cream can be applied to the skin after tape removal. If skin irritation occurs, a skin preparation (spray, roll-on, plastic film or even calamine lotion, which must dry first) can be applied prior to tape application.
Availability
Physiotherapist costs and accessibility vary, but many patients would have out of pocket costs.
Physiotherapists typically use an adhesive, non-stretch (rigid) 38 mm sports tape to restrict undesired motion and improve patella positioning. This is used in combination with a hypoallergenic underlay tape. Both tapes are available over the counter from pharmacies.
Pre-cut tape is available in packages that contain 10–20 applications of pre-cut strong elastic tape that can be used in the pool or shower. This tape is not rigid so initially may not be as effective in reducing pain. Depending on use, a package might last 40–60 days.
Adverse effects
Taping is associated with negligible adverse effects which generally include minor skin irritation.
Evidence
National Health and Medical Research Council (NHMRC) Level I evidence (systematic review of randomised controlled trials) for pain relief.
Anything else?
Patients can be taught to self-tape, enhancing their ability to self manage.
Patients with concurrent hand osteoarthritis may find taping difficult. Pre-cut tape could offer some advantages.
Even tape that does not exert appreciable force on the patella can provide some pain relief. This may be due to a sensory or placebo effect.
Taping has been shown to have immediate and short-term pain reducing effects while the tape is being worn and also provides benefits for some weeks after tape removal.
Key references
- Crossley KM, Marino GP, Macilquham MD, Schache AG, Hinman RS. Can patellar tape reduce the patellar malalignment and pain associated with patellofemoral osteoarthritis? Arthritis Rheum 2009;61:1719–25.
- Hochberg MC, Altman RD, April KT, et al. American College of Rheumatology 2012 recommendations for the use of nonpharmacologic and pharmacologic therapies in osteoarthritis of the hand, hip and knee. Arthritis Care Res 2012;64:465–74.
- Page CJ, Hinman RS, Bennell KL. Physiotherapy management of knee osteoarthritis. Int J Rheum Dis 2011;14:145–51.
- Warden SJ, Hinman RS, Watson MA Jr, Avin KG, Bialocerkowski AE, Crossley KM. Patellar taping and bracing for the treatment of chronic knee pain: a systematic review and meta-analysis. Arthritis Rheum 2008;59:78–83.
Acknowledgements
Handbook of Non Drug Intervention (HANDI) Project Team members include Professor Paul Glasziou, Dr John Bennett, Dr Peter Greenberg, Professor Sally Green, Professor Jane Gunn, Associate Professor Tammy Hoffmann and Associate Professor Marie Pirotta. The HANDI Team is grateful to Professor Kim Bennell for her contribution to the development of this intervention.
Competing interests: None.
HANDI is supported by a grant from the Jack Brockhoff Foundation.
Provenance and peer review: Commissioned; not peer reviewed.