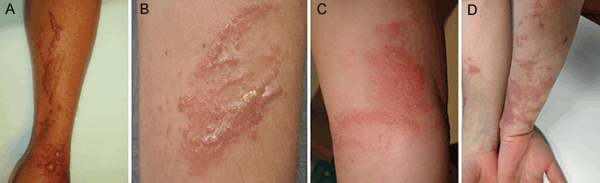
Figure 1. Clinical appearance of the patients
Question 1
What is the most likely diagnosis in these patients?
Question 2
What are the most common culprits for this dermatosis?
Question 3
How can we make the correct diagnosis of this disease?
Question 4
What differential diagnoses would you consider?
Question 5
What therapeutic measures would you recommend?
Answer 1
The diagnosis in all these presentations is phytophotodermatitis (PPD), a common cutaneous phototoxic inflammatory eruption resulting from contact with plant-derived photosensitising compounds, generally furocoumarins (psoralens), followed by exposure to sunlight (especially ultraviolet A 320–380 nm).1,2
Answer 2
PPD is caused by at least four different plant families: Apiaceae (formerly Umbelliferae), Rutaceae, Moraceae and Leguminosae.1–3 The Apiaceae family, the most common plant family implicated, has a distinctive floral umbel that makes them easy to recognise.3 Parsley, parsnips, celery and carrots are examples from this group. The Rutaceae family includes Citrus and Ruta species and is the second most common cause. The fig tree from the Moraceae family and the Psoralea corylifolia from the Leguminosae family are also implicated in PPD.3 In our study, the culprit plants were the parsnips in patients 1 and 2 and lime in patients 3 and 4.
Answer 3
Phytophotodermatitis is a clinical diagnosis. Therefore, a thorough history is essential in making the diagnosis of PPD. The clinician must ask about contact with fruits, plants and medicines or perfumes containing oils from botanical origin. It should be noted, however, that psoralens may also be transferred indirectly through person-to-person contact.4 The patient should also be asked about hobbies, recreational activities, occupation and the use of ‘folk’ remedies.1,2,5 The patient usually complains of a painful or burning sensation rather than pruritus, which is commonly associated with allergic contact dermatitis.2
On physical examination, erythema and oedema with or without blistering can be observed in the acute phase, beginning in the first 24 hours after exposure, maximal at 48–72 hours, and lasting 3–5 days.2 The skin lesions often have a bizarre and linear configuration. The most commonly involved areas include the dorsa of the hands, wrists, forearms and lower legs.1 Hyperpigmentation appears 1–2 weeks after the exposure and may last months to years.1,3 Sometimes the initial inflammatory reaction may be subtle and only the hyperpigmentation is evident.5
Answer 4
Conditions to be considered in the differential diagnosis of PPD are listed in Table 1.1,2,4 A careful history and physical examination are usually enough to differentiate most of the conditions. However, if necessary, laboratory studies such as porphyrin levels (to rule out porphyria cutanea tarda), photopatch tests (to distinguish between photoallergic and phototoxic dermatitis), microbiological analysis of bullae aspirate, biopsy for histologic examination, and further studies may be conducted.2 PPD occurring on a child may be mistaken for child abuse, as children may acquire lesions from contact with other people who have juice on their hands; lesions may have a bruise-like appearance usually in the shape of handprints or fingerprints.1,3,4,6
Table 1. Conditions to consider in the differential diagnosis of phytophotodermatitis1,2,4
| Disease | Clues for diagnosis |
|---|
| Thermal burns |
Contact with hot substances |
| Irritant contact dermatitis |
Contact with strong irritants such as acid, alkali, solvent, and others |
| Drug induced bullous disorders |
Recent exposure to systemic drugs |
| Allergic contact dermatitis |
Contact with topical medications or other suspicious allergens |
| Jellyfish stings, arthropod bites |
History of outdoor and nature-based activities, including in the sea and forest |
| Cutaneous larva migrans |
History of lying or walking barefoot on soil or tropical beaches |
| Cellulitis |
Presence of local inflammatory signs and systemic symptoms |
| Bullous impetigo |
Mainly affects infants and children, especially on the face and extremities; crusted, honey-coloured exudate over erosions can be observed |
| Porphyria cutanea tarda |
Previous history of liver disease, hypersensitivity to the sun and a recurrent rash on the exposed areas, including blisters, erosions, scarring, hyperpigmentation, hypertrichosis and milia. |
Answer 5
Appropriate treatment for this condition includes:1,2
- avoidance of the offending agent
- cool wet compresses during the acute phase
- potent topical glucocorticoids in severe and oedematous lesions
- oral salicylates or indomethacin for pain relief in adult patients
- skin-lightening cream if chronic hyperpigmentation results.
However, prevention is the best treatment for PPD. Known furocoumarin-containing plants should be avoided and not be planted near play areas. It is prudent to advise the use of sunscreens, gloves and protective clothing while in contact with these plants, especially on sunny days. If the contact occurs, prompt washing with soap and water is essential.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.