What causes fibromyalgia?
Fibromyalgia pathophysiology is underpinned by the development of changes in the central nervous system (CNS)4,5 that alter the processing of afferent sensory input, and can be grouped together under the term ‘central sensitisation’.6 Central sensitisation changes are often triggered by long-standing psychological or physical stress.7 These changes result in the intensity of usually non-painful stimuli being amplified and experienced as painful. Other effects include abnormality in the sleep cycle, where patients are unable to achieve deep, restorative, stage IV non-REM sleep, and disturbances in the hypothalamic-pituitary axis, with altered levels of serum cortisol, decreased 24-hour urinary free cortisol and blunted cortisol responses to dynamic testing.8
Genetic polymorphisms resulting in alteration in CNS serotonergic and catecholaminergic processes continue to be investigated, and appear to increase the risk of developing fibromyalgia.9
Aside from any genetic predisposition, clinical fibromyalgia is frequently triggered. In an internet survey of 2 596 fibromyalgia patients in North America, 79% described potential triggering events at the onset of the their fibromyalgia,10 while 88.7% of patients seen in an Australian public hospital fibromyalgia clinic reported recognisable triggers.11 A physical or psychological stressor in a susceptible individual can result in a chronic, maladaptive stress response, which, in turn, mediates the central changes.12
How is fibromyalgia diagnosed?
Fibromyalgia is diagnosed according to criteria published by the American College of Rheumatology (ACR). The initial classification criteria were published in 1990 and included widespread musculoskeletal pain and tenderness measured by the ‘tender point count’ on physical examination.13 These criteria were useful in defining a standard group for research purposes, however did not recognise the broader spectrum or fluctuating nature of fibromyalgia symptoms.
In 2010 the ACR published diagnostic criteria, taking these aspects into consideration.14 These criteria now account for chronic musculoskeletal pain, as well as fatigue, sleep problems, cognitive disturbance and some more focal symptoms. In publishing these newer criteria, the authors recognised that fibromyalgia symptoms fluctuate significantly over time and they aimed to be able to recognise a spectrum of severity in patients with central sensitisation symptoms – rather than just those with the most severe illness who satisfied the traditional definition of fibromyalgia. The severity scale captured by the new criteria has been termed by some as a degree of ‘fibromyalgianess’ or a ‘polysymptomatic distress scale’.15,16 Recent research focus uses this gauge of central sensitisation symptom severity to investigate the extent of sensitisation syndrome features in patients with fibromyalgia, chronic pain and other associated conditions.16 It is clear, however, that many clinical features of central sensitisation are also found in a large number of other chronic illnesses.
The diagnosis of fibromyalgia is often not initially considered. In a large North American survey, 46% of fibromyalgia patients had consulted 3–6 health care providers regarding their symptoms, prior to their fibromyalgia diagnosis.10
When should fibromyalgia be considered?
Fibromyalgia has multiple, varied and fluctuating symptoms. It should be considered when a patient describes chronic musculoskeletal pain, fatigue and poor sleep. These symptoms are usually accompanied by a number of other problems such as depression or anxiety, sensitivity to chemicals, irritable bowel or restless legs. The symptoms often start or worsen during a period of severe psychosocial or physical stress.
The key symptoms of fibromyalgia are also commonly found in many other illnesses, and a thorough examination and investigation needs to be undertaken in order to ensure there is not another pathological cause for the symptoms – particularly if there are any ‘red flags’ in the patient’s history suggestive of another serious pathology (Table 1).
Table 1. Red flags
- Older age at new symptom onset
- Weight loss
- Night pain
- Focal pain
- Fever or sweats
- Neurological features
- History of malignancy
|
Care also needs to be taken when interpreting results of investigations, particularly radiology. Sometimes abnormalities found on musculoskeletal imaging are attributed to causing symptoms, when the clinical picture is much more global.
Often, screening questions based on the modified 2010 ACR criteria17 (Figure 1) are useful. If patients presenting with widespread chronic pain are also experiencing fatigue, sleep problems, cognitive disturbance, depression, headache and/or abdominal pain, then fibromyalgia should be considered.
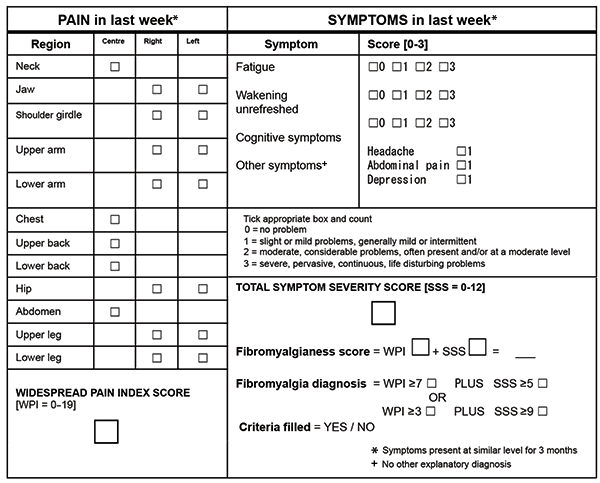
Figure 1. New modified ACR diagnostic criteria for fibromyalgia17
When is fibromyalgia easy to miss?
Fibromyalgia is easy to miss when it coexists with another chronic illness, particularly when it occurs with another condition causing similar symptoms such as arthritis, endocrine disorders, depression or sleep apnoea.
Fibromyalgia coexists in a significant proportion of patients with rheumatoid arthritis. These patients have worse disease activity, joint tenderness and swelling, and psychological distress.18,19 Concomitant fibromyalgia is also reported in patients with systemic lupus erythematosis and osteoarthritis, who have significantly higher proportion of problems associated with central sensitisation, including sleep disturbance and fatigue.20–22 In these conditions, there is an obvious source of nociceptive input to drive central sensitisation processes. In a subgroup of patients with diabetes there is reported coexisting central sensitisation,23 and a significant proportion of patients with hyperthyroidism also have features of fibromyalgia.24 In all of these situations of chronic illness, the possibility of long-standing physical or psychological stress exists, so that even when there is no obvious nociceptive input (such as in thyroid disease), these patients can still develop the changes of central sensitisation. Therefore, if patients have clinical features out of keeping with general disease activity, then it may be necessary to consider whether central sensitisation could be contributing.
Management of fibromyalgia
Team management
Fibromyalgia is a complex disorder, requiring input from many different health care providers, including medical, allied health, and complementary and alternative medicine practitioners. General practitioners are in an ideal position to co-ordinate and monitor these multidisciplinary management strategies.
In this vulnerable patient group, psychosocial issues often arise. General practitioners are uniquely placed to recognise problems such as financial hardship, social isolation, loss of role and secondary depression, and can provide essential structured support and validation for these patients.
Education
Following fibromyalgia diagnosis, an in-depth discussion of the clinical features and pathological mechanisms of fibromyalgia is essential. Patient understanding of the condition and their expectations as to clinical improvement are key to developing a successful management program. Often the validation and reassurance experienced once a diagnosis is made result in improvement.25
The chronic and fluctuating nature of fibromyalgia and the management goals of symptom reduction and optimising function need to be explained. The importance of adherence to treatment plans and realistic expectations regarding progress and outcomes need ongoing reinforcement. Thorough and targeted patient education also results in increased patient engagement and proactive attitude to self management.
Psychology
A number of psychological interventions are helpful in the management of fibromyalgia. Concomitant depression and anxiety often occur in fibromyalgia, and can contribute significantly to reduced patient wellbeing. Addressing these problems, if present, is essential to any improvement in a patient’s overall health.
Stress management techniques are an essential part of any fibromyalgia therapeutic plan and, when combined with the development of other skills such as planning, pacing and coping strategies as part of cognitive behaviour therapy (CBT), then there is demonstrated improvement in pain-related behaviour, self-efficacy and physical function.26 Other psychological strategies such as mindfulness techniques may also be helpful. Mindfulness-based therapies seem to be effective in alleviating symptoms common in fibromyalgia such as pain, depression and a range of other psychological factors as well as improving health-related quality of life, although in studies with active comparator arms, they have in general, not proven superior.27,28 A recent randomised controlled trial of an online mindfulness intervention targeting socioemotional regulation in fibromyalgia patients resulted in significant improvement in social functioning, positive affect and coping efficacy for pain and stress.29
Exercise
Regular exercise improves pain, fatigue and sleep disturbance in patients with fibromyalgia.30 There is no ‘best’ form of exercise and all types may be considered. Aerobic exercise, in particular, reduces fibromyalgia symptoms and improves physical capacity.31 The initiation of any regular exercise program needs to be slow and gradual. Patients who are deconditioned and concerned regarding the possible worsening of pain and fatigue will need reassurance; they may need to start with only a few minutes of gentle exercise several times a week. This can be built up very slowly and gradually as tolerance increases. Often a hydrotherapy pool is a good place to start an exercise regimen, as the warmth of the water and relative weightlessness relieves symptoms while the resistance provides a gentle workout.
Other physical therapies
Other physical therapies can be helpful in the management of fibromyalgia, particularly those that can be self administered. There is evidence to support the use of yoga, qi gong and tai chi in patients with fibromyalgia.32 Studies in which the use of these therapies resulted in improvement in fibromyalgia symptoms and physical functioning were generally small and unblinded, however, given the lack of serious adverse effects and the promotion of self-efficacy, these management modalities are generally useful options.
Medication
There are no pharmaceutical agents currently available on Australia’s Pharmaceutical Benefits Scheme for specific use to treat fibromyalgia.
Analgesics
Simple analgesia is often the first medication patients with fibromyalgia will trial. Guidelines published by the European League Against Rheumatism (EULAR) recommend the use of simple analgesics like paracetamol in the management of fibromyalgia; however, due to insufficient data this is based on expert opinion alone.33 Paracetamol use has not been studied in fibromyalgia patients, other than in combination with tramadol, where the combination resulted in a modest (18%) improvement in pain compared with placebo.34
Other studies have found some benefit with tramadol use for fibromyalgia;5,35 the therapeutic benefit was possibly due to tramadol’s serotonin-noradrenaline reuptake inhibition, rather than µ-opioid activity. Other opioid use in fibromyalgia is not routinely recommended. There is reduced opioid receptor availability in patients with fibromyalgia,36 and a lack of supportive evidence for their efficacy.37
The use of non-steroidal anti-inflammatory agents (NSAIDs) has not been supported with significant research data, however they are often used and a survey of 1042 patients with fibromyalgia, found that 66.1% deemed NSAIDs more effective than paracetamol.38
Antidepressants as pain modulators
Medications that elevate levels of serotonin and noradrenaline in the descending inhibitory nociceptive pathways of the CNS, such as low-dose tricyclic antidepressants (TCAs) and serotonin-noradrenaline reuptake inhibitors (SNRIs), can provide significant benefit in patients with fibromyalgia independent of effects on mood.39 Amitriptyline, duloxetine and milnacipran are the best-studied agents in these categories, and all have substantial evidence for the significant improvement of pain, and other symptoms of fibromyalgia, although some early studies were short term.4 Milnacipran is approved by the Australian Therapeutic Goods Administration for use in fibromyalgia,40 but is not currently available in Australia.
Membrane stabilisers
Pregabalin and gabapentin bind to voltage-dependent calcium channels, reducing calcium influx into sensitised spinal cord neurons in central pain syndromes such as fibromyalgia. In a meta-analysis of randomised, controlled trials in fibromyalgia patients, the use of these agents resulted in reduced pain, improved sleep and better quality of life.41
Key points
- Fibromyalgia is a clinical syndrome resulting from a process of CNS sensitisation.
- It has varied and fluctuating symptoms and can be confused with other illnesses with similar features.
- Fibromyalgia can also coexist with other disorders, and identifying the source of clinical complaints can be difficult.
- The possibility of central sensitisation should be considered in all patients with chronic illness when the one particular aspect (particularly musculoskeletal pain or fatigue) is not responding to seemingly adequate treatment.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.